Presentation
A 23-year-old male presented to the Wills Eye Hospital Oculoplastics clinic with a chief complaint of eye pain and pressure, as well as limitation in upgaze. The patient was referred from an outside provider for a second opinion regarding potential treatment and management.
Medical History
The patient’s medical history was notable for daily headaches, depression, hypertension and sciatica. He had jaw surgery to correct midface hypoplasia. Medications included amlodipine, escitalopram, dronabinol and a myriad of homeopathic therapies. He was a former smoker who had quit two months prior to presentation. His family history was significant for Graves’ disease.
Examination
Ocular examination revealed a visual acuity of 20/20 in the right eye and 20/30 in the left. Pupils and confrontation visual fields were normal in both eyes. Intraocular pressures were 33 mmHg and 28 mmHg, in the right and left eyes respectively. Extraocular motility was notable for a significant limitation in upgaze (Figure 1). Ishihara color plates were full in both eyes. There was no proptosis as measured by Hertel exophthalmometry, and there was no resistance to retropulsion. Anterior segment examination revealed mild chemosis in both eyes but was otherwise unremarkable. Dilated fundus examination was normal in both eyes.
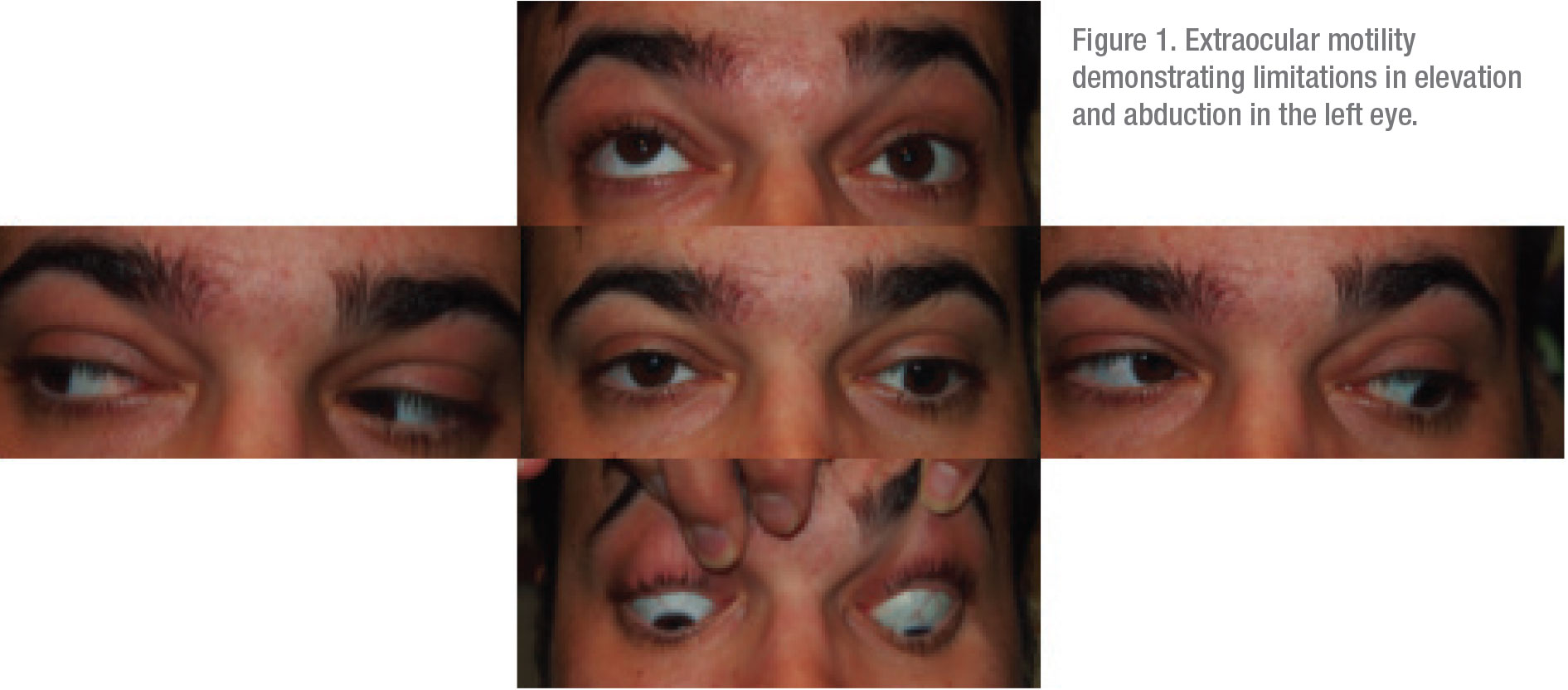 |
What is your diagnosis? What further workup would you pursue? Please click this link for diagnosis, workup, treatment and discussion.



