In the ongoing struggle to compensate for the visual deficits caused by presbyopia, multifocal intraocular lenses have become a popular option. Their solution to a lack of accommodation, however—casting multiple images on the retina simultaneously—has opened a proverbial can of worms. By altering the characteristics of the images striking the retina and simultaneously exposing the brain to an unfamiliar visual experience, multifocal IOLs have created new challenges for both patients and ophthalmologists.
"Neuroadaptation is an issue we've always had to deal with," observes Robert M. Kershner, MD, MS, FACS, a refractive surgeon practicing in
"Some surgeons simply dismiss multifocal patient complaints—or don't see enough patients postop to notice the complaints," he says. "And many patients who are happy with their surgical outcome won't mention that they're having problems adapting to their new vision unless the surgeon specifically asks pointed questions, such as whether they're experiencing visual degradation at night. It's easy to overlook or dismiss such issues. But addressing them can make a world of difference to your patients—and your practice."
The Neuroadaptation Process
One of the things highlighted by the adaptation problems associated with multifocal lenses is the reality that our visual system has two distinct components: the optical system that alters light before it reaches the retina, and the neurological system (including both the retina and brain) that processes the information. Many ophthalmologists haven't had to devote too much time to worrying about the neurological half of the visual system—until now.
"Adaptation can happen quickly, as when we adapt to light or dark, but some types of adaptation happen very slowly over weeks or months," notes Martin A. Mainster, MD, PhD, FRCOphth, professor of ophthalmology at the University of Kansas School of Medicine. "Slow adaptation probably results from neural plasticity, which is long-term alteration in anatomic connections or synaptic properties due to neuronal activity or injury. Axons and dendrites can grow and retract in the retina and the brain; synapses can be lost or gained.
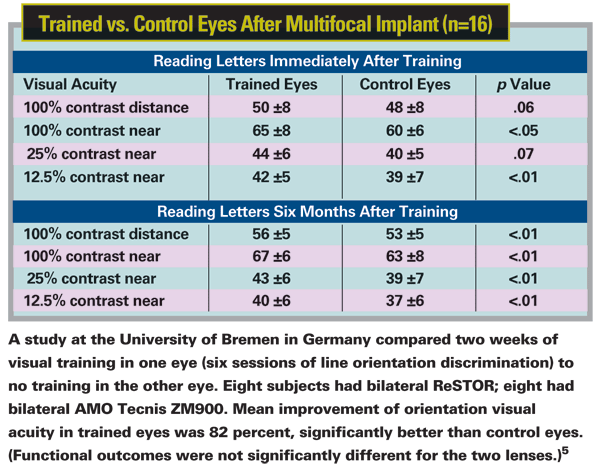
"In fact, the visual system exhibits remarkable plasticity at both retinal and cortical levels," he continues. "For example, adaptation causes people to see better with their own higher-order aberrations than with equivalent optical defocus. In multifocal IOL pseudophakes, neural plasticity probably explains several things: the commonly observed improvement in contrast sensitivity at six months postop; better contrast sensitivity in bilateral multifocal IOL pseudophakes compared to unilateral multifocal pseudophakes; and perceptual learning after surgery, when experience produces reasonably permanent changes in perception. The latter category would include programs that aim to deliberately improve certain types of functioning, such as exercises using Gabor patches or orientation discrimination.
"Vision has been shown to improve in multifocal IOL patients who engage in perceptual learning with these kinds of visual tasks," Dr. Mainster notes.1,2 "This makes sense, because the contrast sensitivity of the overall visual system is equal to the transfer of optical contrast through the cornea and lens, (the modulation transfer function) multiplied by the contrast sensitivity of the retina and brain (the neural transfer function).3 That's why any improvement in neural adaptation in the retina and brain after multifocal IOL surgery produces a corresponding improvement in overall contrast sensitivity function—i.e., an improvement in functional vision."
Multifocal images on the retina are not only unfamiliar to the visual system when first encountered—they also affect the quality of the signal going to the brain. "Imagine looking at a dark line on a piece of white paper," says James E. McDonald II, MD, assistant professor of ophthalmology at the University of Arkansas Medical Center in Little Rock, Ark., and founder of McDonald Eye Associates in Fayetteville, Ark. "The darker the line and the more the contrast at its edge, the stronger the electrical signal your retina sends to the brain.
"When we look through a multifocal lens, we see two images superimposed, one of which is out of focus," he continues. "That undercuts the contrast of the overall image and reduces the strength of the signal being sent to the brain. That's why it's so important to reach emmetropia and eliminate astigmatism when we implant a multifocal IOL. Any extra defocus diminishes the signal to the brain even further." (Dr. McDonald believes monovision is actually a better option for most patients, because both eyes receive a full-spatial-frequency image, so the brain simply has to pay attention to one eye at a time.)
"We know the brain can learn to filter out unwanted information," he points out. "My nephew has hunted all his life; he can spot things in the wild that I can't see at all. His visual cortex has learned to filter out visual information that's not relevant. That's the premise behind using Gabor patches to trigger perceptual learning. The patches help train your visual system to pick out details from a mesh of irrelevant information—exactly the skill the brain needs when seeing through multifocal lenses."
Is Vision Training a Scam?
"The idea that neuroadaptive training is unnecessary or ineffective is absolute hogwash," says Dr. Kershner. "You don't have to take it on faith that training the brain, at any age, can have a substantial impact on a patient's successful rehabilitation following surgery. Just look at what's being done with occupational therapy and stroke patients, or cognitive therapy training and Alzheimer's patients. The neurophysiology literature is loaded with clinical studies that demonstrate overwhelming success with these training processes. It's disingenuous to think that ophthalmology would be any different.
"We know that the brain is not a static organism that stops changing at adulthood," he continues. "The brain is incredibly plastic and is constantly changing and redirecting neural networks throughout life. If a patient has a stroke and has lost a portion of his brain to ischemic injury, every indication is that the brain will correct the deficit as best as it can by redirecting interconnections from surviving neurons so they assume the role that the damaged area used to manage. And when it comes to training the brain, every study has shown that if you provide additional input to the brain during this repair process, the sprouting of new dendrites and new pathways is greatly enhanced. Therapy drives it. I'm always astonished when someone insists that visual neuroadaptation doesn't occur; or that if it occurs you can't influence it; or that you can influence it but a given approach couldn't possibly work. Our profession is stubbornly resistant to new ideas."
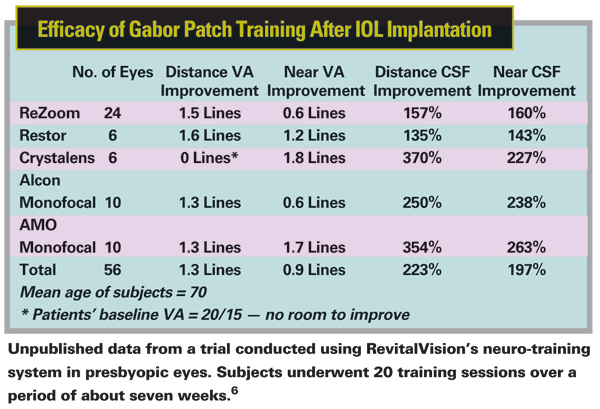
One available system designed to enhance adaptation following implantation of multifocal IOLs is an Internet-based program offered by RevitalVision (using technology pioneered by its predecessor, NeuroVision), based in Lawrence, Kan. "Our training system is designed to enhance neuroadaptation by making the visual system analyze information presented using Gabor patches," explains Brendan Sheil, CCO of RevitalVision. "After every session, we analyze the results and build a revised program for the patient to download the next time he logs on. The revised program provides more of whatever specific stimuli led to improved vision and better responses. We have modules designed to facilitate different goals, such as enhanced contrast sensitivity or enhanced near visual acuity. We've found, for example, that Crystalens patients don't need to work as much with contrast sensitivity; they do better using the post-refractive and visual acuity modules.
"Most doctors still associate this type of program with gimmickry and eye exercises," he notes. "We have to sit there and say, 'We don't do any of that.' This isn't prism therapy, it isn't Bates method therapy. We're stimulating neural interactions, and we monitor the patient's responses; if a particular type of stimuli doesn't generate improved vision, we alter the program until we see the patient's vision improving. Thousands of clinical trial participants and customers have reported significant improvement in their vision performance—an average of two lines of visual acuity, and a 100-percent increase in contrast sensitivity." (A detailed summary of those trials and their results can be found on the Web at revitalvision.com.) So far, the data indicate that once the improvement has occurred, it doesn't fade or require ongoing training to maintain.
Mr. Sheil says this type of neuroadaptive training has also been shown to improve near vision in presbyopic patients. "A growing number of individuals have paid for refractive surgery and now are frustrated because presbyopia is setting in," he notes. "If they're not in need of cataract surgery and they're reluctant to opt for clear lens exchange, this gives the physician something concrete to offer them." Mr. Sheil adds that RevitalVision's policy is to treat staff members with any of their existing programs for free. "When a staff member has experienced dramatic visual improvement from one of our training programs, patients can really see the value of it, and that benefits everyone," he says.
Mr. Sheil says the company is currently conducting a clinical trial making a direct comparison between binocular presbyopic lens patients who receive neuroadaptive training and those who don't. "Our experience has been that we can improve contrast sensitivity and minimize the impact of glare and halo in most multifocal eyes," he says.
"We're including the Crystalens in the study because many Crystalens patients want more near vision; our experience indicates that training can help with that as well."
Richard L. Lindstrom, MD, managing partner at Minnesota Eye Consultants and an attending surgeon at the Phillips Eye Institute and Minnesota Eye Laser and
Dr. Lindstrom notes that while many surgeons are still skeptical, in his experience they're open to the concept, and many are enthusiastic. "We now know the brain is plastic and can 'learn,' even in the elderly," he says. "I believe premium IOLs are an important indication for this technology, as are post-corneal refractive surgery patients with a small residual refractive error and patients with low levels of naturally occurring ametropia and early presbyopia. The treatment also works for amblyopia, and appears to be able to enhance sports performance where vision plays a major role, as in batting in baseball, playing tennis, skeet shooting and the like." He adds that at $250 per patient, the cost is low and allows for a reasonable practice mark-up. "Cost is always an issue for patients, but less so in patient-pay categories such as premium IOLs or LASIK," he says.
But … Is Training Necessary?
Even if it's possible to enhance the neuroadaptive process, do we really need to? "Some vision-related adaptations already occur without surgeon intervention, given enough time—as when a newly implanted IOL lets in a broader range of wavelengths than the crystalline lens was allowing in," observes Dr. Kershner. "Patients who at first notice a color shift after surgery usually report that it's disappeared when asked about it again a few weeks or months later. In that case, the adaptation didn't need to be coaxed at all. But that's not true when you're dealing with optical challenges such as the simultaneous perception of multiple focal points. We're asking the brain to adapt to visual distortions it's never encountered before."
Dr. McDonald says he has great hope that neural training will increase the quality of vision for multifocal patients. "Like patients who have astigmatism or a less-than-perfect LASIK outcome, patients who receive multifocal lenses may eventually adapt on their own," he says. "But with training they may adapt faster—and maybe further—than they would have on their own. If you had a knee or hip replaced, you could probably skip rehab and do okay, but doctors know that a physical therapy program can make a significant difference in helping you adapt to the new joint.
"I believe that using perceptual learning to improve patient neuroadaptation is the next step to improving patient outcomes," he adds. "We may see incremental improvements in the lenses themselves, but the frontier is understanding and taking advantage of neuroadaptation."

Of course, it's not clear that the best way to enhance neuroadaptation has been discovered yet—or that a single approach will work for everyone. "There's no question that training works for most people," says Dr. Kershner. "The question, is, what's the best way of facilitating the neuroadaptive process? That hasn't yet been resolved. We've tried some different approaches, and we're attempting to compile data to see which one may be most effective. The problem is that different techniques seem to work differently for different patients.
"In the long run, when we have enough data, we may be more confident about what works best, but it's going to take plenty of study and time," he adds. "Nevertheless, there's no question in my mind that the data will show that multifocal patients do adapt better visually, and recover more quickly from the change in their optical system with neuroadaptive visual training exercises."
Identifying Poor Candidates
Dr. Kershner believes that the ability of a patient to adapt to multifocal vision is predicated upon his age, the plasticity of his brain, his level of intelligence, how well his sensory apparatus is working, his motivation to make the visual symptoms go away, and any additional training the surgeon provides. "The more input you provide—such as a series of visual training exercises—the better the brain distinguishes the optical characteristics of what the patient is now seeing, and the faster most patients achieve a comfort level," he says. "I've seen this in my own patients."
However, Dr. Kershner notes that some patients will never adapt, no matter what you do. "Having a sure-fire method for identifying these patients ahead of time would be ideal, but I don't know if that will be possible," he says. "We're just beginning to unravel the brain's complexities.
"Clinical experience, however, has exposed some warning signs that seem to correlate with difficulty in neuroadaptation," he says. "Studies have found that addictive behavior is tied to many of the same areas of the brain that we use when we neuroadapt to new visual stimuli; it's possible that a deficit in those regions could lead to both addictive, dependent behavior and difficulty in adapting to new visual stimuli. My experience has supported this idea; patients who clearly have addictive personalities do seem to have more trouble adapting to multifocal vision. As a result I almost categorically avoid implanting multifocal lenses in these patients.
"Also, many surgeons are wary of operating on people in visually de-manding professions such as engineering," Dr. Kershner notes. "An engineer is trained to use precise acuity; if you alter their visual apparatus in any way, they'll be miserable—and they'll let you know! I've had patients come in with a T-square and a drawing pad and draw what they're seeing. And I've had similar reactions from computer programmers.
They've been some of my most difficult refractive surgery patients. Certain professions tend to attract certain types of brains, and that may make them better or worse candidates for interpreting visual cues following surgery.
"Of course, you could argue that this is more an issue of personality than of the brain's ability to adapt, but I suspect that difficulty adapting tends to lead to more rigid, compulsive individuals," he adds. "People who have difficulty dealing with change try to create a world in which they're in control. When you alter their world, you undermine their control. Furthermore, when you implant a multifocal lens the change they have to adapt to is partly negative; you're degrading their image perception in exchange for multifocality."
In the interests of finding ways to predict which patients might adapt to multifocal visuals more successfully, Dr. McDonald is working with several other doctors to develop a method for quantifying visual dominance. "We suspect that being able to quantify how dominant one eye is relative to the other—i.e., neural competitiveness—may help us to predict better how patients will do with both monovision and multifocality," he says. "We've developed a new way to quantify this by measuring the magnitude of interocular suppression, and we recently published results from the first study of our new approach.4 We suspect that those who turn out to be more ambidextrous, in terms of which eye they're using, will have an easier time neuroadapting to multifocals or monovision. Of course, being able to identify the patients who will have a harder time neuroadapting would be a huge advantage for surgeons who offer multifocals to their patients."
A Work in Progress
Dr. Kershner notes that patients who do neuroadaptive training are not necessarily his happiest or most successful patients. "Some patients do the surgery and are thrilled without any further input from me," he says. "But I can tell you this: If you look at the population of people who are not screened or trained, you'll have a certain percentage of failures no matter what. Very unhappy patients. And the more patients you treat, the greater that number will become. That being the case, I like to err on the side of conservativism and optimize success.
"Our clinical experience has convinced us that neuroadaptive training can be very effective as a screening tool, helps people succeed postop who otherwise might not, and cuts 30 or 40 percent off of the adaptation time," he concludes. "There's no question in my experience that it works. Does it work with everybody? No. Can I tell who will gain the most from it? No. Do I know exactly how much it will improve the outcome? No. Do I know what the best way to do it is? Not yet. But does it help? Yes. If you train as many patients as possible both beforehand and afterwards, my experience suggests that you'll have a much lower number of failures and much greater number of successful outcomes."
Drs. McDonald and Lindstrom both have a financial interest in RevitalVision.
1. Kaymak H, Fahle M, Ott G, Mester U. Intraindividual comparison of the effect of training on visual performance with MFIOLs. J Refract Surg 2008; 24:287-93.
2. Lim KL, Fam HB. NeuroVision treatment for low myopia following LASIK regression. J Refract Surg 2006;22:406-8.
3. Mainster MA, Turner PL. Multifocal IOLs and Maculopathy—How Much is Too Much? In: Chang DF, ed. Mastering Refractive IOLs: The Art and Science. Slack, 2008: 389-94.
4. Yang E, Blake R, McDonald JE 2nd. A new interocular suppression technique for measuring sensory eye dominance. Invest Ophthalmol Vis Sci 2010;51:1:588-93.
5. Kaymak H, Fahle M, Ott G, Mester U. Intraindividual Comparison of the Effect of Training on Visual Performance With ReSTOR and Tecnis Diffractive Multifocal IOLs. J Refract Surg. 2008;24:287-293.
6. Hunkeler J, Lindstrom D. Unpublished data, 2009.



