In the 1990s, many nearsighted patients who were eager to minimize their dependence on glasses turned to radial keratotomy for relief. Satisfied, they went back to their daily lives, and RK was gradually phased out as more versatile, reproducible surgeries such as PRK and LASIK came on the scene. Now, however, these RK patients are starting to reappear in surgeons' offices, desiring further refractive surgery or needing to have cataracts removed. Since their corneas can have as many as 32 incisions, these subsequent surgeries can be more challenging to perform. In this article, refractive and cataract surgeons share their advice on how to approach these particular patients in order to get the best possible outcomes.
The Refractive Patient
Here are the various issues that can arise when post-RK patients desire further refractive surgery, and how surgeons can address them:
• Determine the refractive target. Surgeons say that, more often than not, RK patients who present for refractive surgery are usually slightly hyperopic due to the hyperopic drift that occurred after some RKs. They may also be presbyopic. "They're usually between +1.5 and +3 D," says
Chicago
"The problem is that, over time, the progressive hyperopic shift may continue, and we have to counsel patients that, no matter what we do today, these incisions could continue to change, as will their vision. If they don't understand this, you could have a very unhappy patient."
In addition to the hyperopic drift, RK eyes' refractions may also fluctuate throughout the day, making the intended refractive goal a moving target.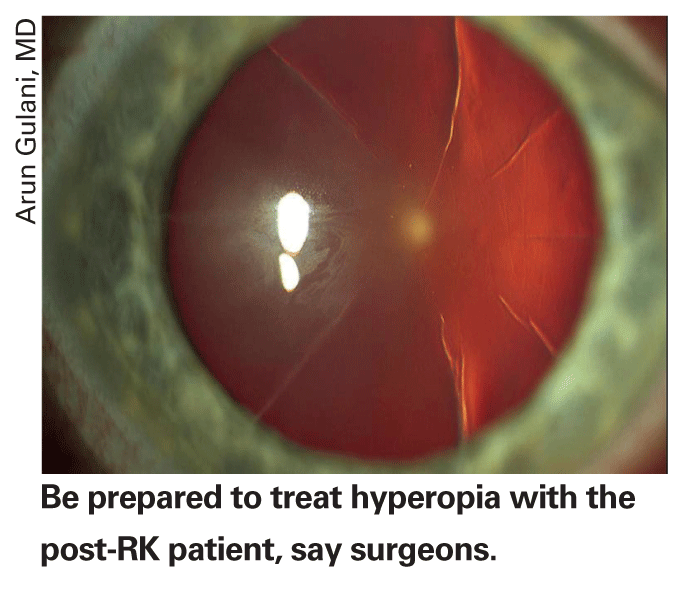
"Within a given day the RK incisions can swell or the cornea can flatten, meaning they need different pairs of glasses for different times," says Dr. Majmudar. "If you have someone who's really fluctuating a lot from morning to evening—I've heard about them though I haven't seen many—I'd lean toward treating a little more hyperopia. This is because most of these patients aren't very young, they're already in their 40s, and leaving them a little myopic will avoid them getting more hyperopic, so you're covered there. It will also give them some near vision." Even for non-fluctuating patients in their mid 40s to 50s, Dr. Majmudar thinks they probably would appreciate a little myopia. "So, you might really want to push them toward a little myopic correction postop," he says.
Dr. McDonald recommends not touching such a patient until he's been stable for a while. "They have to be stable for at least a year, with no change in sphere or cylinder of more than 0.5 D," she says. "You really have to make sure you're not shooting at a moving target. Almost all of these patients have mild diurnal fluctuations, but if they're extreme, I'd wait. I've never seen anyone with diurnal fluctuations that never go away; they might go on for five or 10 years, but I haven't seen them persist for decades.
"However, if someone with significant fluctuations [a diopter or more] comes to me for refractive surgery, saying that his job is on the line and he needs good vision 'or else,' I'd ask him what time of the day he needs good vision, then refract him at that time and base the procedure on that." She adds that if someone has mild fluctuations that he doesn't complain about or isn't even aware of, then you have a pretty good chance of making him happy. For a patient with minor fluctuations, Dr. McDonald takes a series of wavefront maps in the morning and a series in the afternoon, then goes for the value that seems the closest average of the measurements from the two periods.
Jacksonville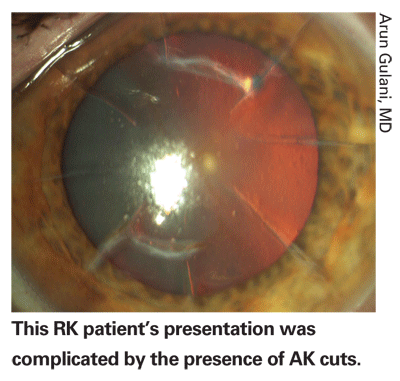
• Choose the procedure. Surgeons agree that surface ablation is the way to go with these patients. "I think LASIK was fairly popular for treating post-RK patients 10 years ago, because you can make a flap in the cornea and it's generally pretty successful in allowing you to perform the ablation," says Dr. Majmudar. "But there are a couple of things to be concerned about: There's always the chance the incisions will splay open during the actual microkeratome pass or during the manipulation of the flap. If that happens, you then have a 'flap salad' with bits of the flap everywhere that you have to gather and put back together to avoid irregular astigmatism that can only be treated with a hard contact lens. Also to consider: What if you need an enhancement of the LASIK over the RK? Do you lift up the flap and risk tearing the incisions?
"Now, since the advent of PRK and, frankly, mitomycin, most surgeons would do PRK for the post-RK patient," he says. "Without the use of mitomycin, there was a higher chance of getting subepithelial fibrosis with PRK after RK. But with the use of mitomycin, you don't get dense scarring along the incisions and don't get that much regression." He says it works best for myopic PRK after RK, but that he's also been fairly successful with hyperopic PRK after RK, as well.
• Space out the procedures. Because the RK cornea can take more time to stabilize after PRK than a virgin cornea, surgeons usually recommend that patients not get bilateral simultaneous surgery because it would be too debilitating. "These patients have a tougher recovery, so you do one eye at a time," says Dr. McDonald. "However, the person who has a unique circumstance, such as a school teacher who's home for the summer, may be able to have both eyes done and then sit at home for a couple of days having other people do things for him until his vision stabilizes. I much prefer spacing the surgeries out, usually by three to four weeks but sometimes longer, no matter how much they swear to me that they don't mind having to have someone drive them around for a couple of weeks. Ultimately, most people don't like that type of situation."
• Use a careful epithelial debridement. The presence of the RK incisions makes for a more risky debridement if you're doing it manually. "You have to scrape the cornea very gently," says Dr. McDonald. "Move toward the center; don't go back and forth against the incisions because they can snap open easily without much pressure. It may take longer than normal—it can take 10 minutes to get it all off."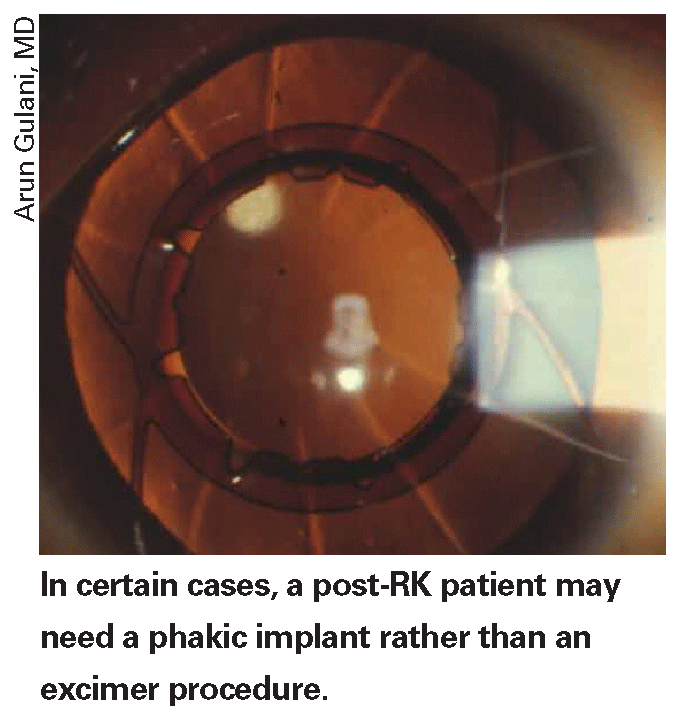
• Modulate the mitomycin. Dr. Majmudar says that, since you're going to be using the antifibrotic agent in these patients, you may want to compensate for its effect on the postop refraction. "For a myopic treatment, since there's not going to be that much compensatory regression, you may want to back off a little on your treatment, because if they end up a little hyperopic, they may stay that way," he explains. "For a hyperopic treatment, I'd cut back a little to get the right adjustment. Though everyone has his own nomogram, if you haven't done a lot of mitomycin-assisted PRK, I'd say a good starting point is to back off about 10 percent on the sphere."
• Dealing with purse-string sutures. Back in the 1990s,
The Cataract Patient
The post-RK cataract case poses some of the same challenges as the post-RK refractive patient, such as working around the incisions, but it also poses some new ones. Here are several surgeons' tried-and-true approaches to getting good results:
• Getting the right central corneal power.
"But with RK, the front and back of the cornea change in unison, so the relationship between them is the same, so your normal lens calculation process works, for the most part. You don't have to make as much of a change in your calculations with RK as you do with a post-LASIK patient, in general, especially if the RK has a larger optical zone and fewer cuts."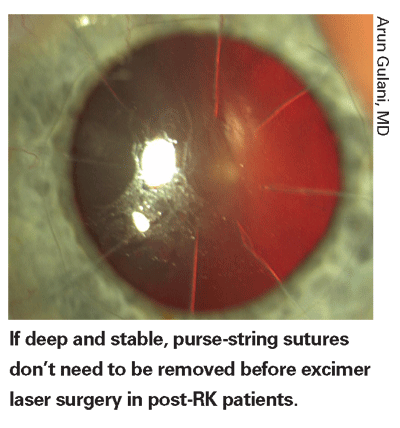
Many topographers and anterior segment analyzers do a good job at getting the central corneal power, say surgeons. "I use two different topographers, the Humphrey Atlas and the EyeSys," says
"The next thing I do is plug those values into the Holladay 2 formula, checking 'yes' when asked by the software if the patient is a previous RK. That means the machine will use a corneal power of around 43.8 D for that portion of the IOL calculation formula that calculates the effective lens position."
Eugene
If you don't have access to one of these devices, Dr. Waltz notes that you can do the contact lens over-refraction method for the tough cases. "You can refract them as they sit, then put a hard contact lens on and refract them again to get a pretty good idea of what their true corneal power is by subtracting one refraction from the other."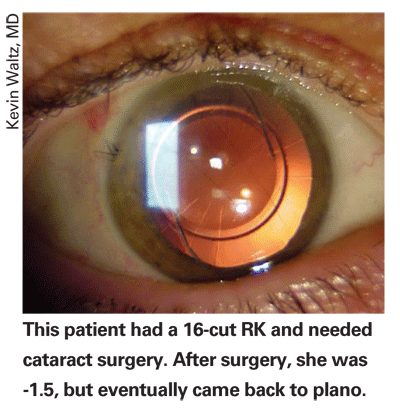
Dr. Koch says you can also give yourself some room for error postop by the refractive target you set. "The third element of my approach is to aim for about -1 D postop," he says. "This is for two reasons: If the calculations are inaccurate, you'll have some leeway one way or the other, and the patient will have some useful vision somewhere. Second, RK patients often have an ongoing hyperopic shift, and if you leave them -1 it will give them many years in which they can, we hope, see well without correction before they'll need some kind of excimer laser procedure."
• Choosing a lens. Surgeons say that an aspheric or toric lens can be useful in these patients, and some will even implant a multifocal.
"I've had some success using toric lenses in post-RK patients," says Dr. Packer. "I use the appearance of the central 3 mm on the topographic map in my planning. By lining that up with the toric IOL, using lenses by either Staar or Alcon, I've had good luck in getting the patients corrected."
Dr. Koch usually goes with an aspheric lens as his first choice. "I prefer using an aspheric whenever possible," he says, "unless they have 2 D or more of astigmatism that's evident on the various calculations, at which point I'd switch to a toric lens."
Doctors disagree, however, on the merits of multifocal lenses in these patients. "These people had their RK so they wouldn't have to wear glasses," says Dr. Packer. "But I've stayed away from using multifocal implants in patients with more than four RK cuts. They have aberrations as it is, and I think the multifocal implant diminishes contrast and gives more unwanted side effects. But, I tend to use the Crystalens if they want some presbyopic correction, because it doesn't add anything to their aberrations."
"I wouldn't get near a multifocal IOL in these patients," says Dr. Koch. "I think that's a disaster in the making. These multifocal lens patients' vision drops if their eyes get a little dry, let alone have an irregular cornea. I think you could consider something like the Crystalens if you wanted to give them some accommodation, but the drawback is it doesn't have the asphericity you look for, nor can it correct astigmatism. But if they have relatively little astigmatism and they're really motivated to have a little more depth of field, the Crystalens could work very well."
Dr. Waltz will use a multifocal IOL in certain patients. "RK eyes have multifocal corneas," he says. "The kind of multifocal cornea they have is a center that's relatively flat for distance and a periphery that's relatively steep for near vision. That multifocal cornea makes it very difficult to get a full effect from a multifocal IOL, so putting in a multifocal IOL is generally not that beneficial, especially in someone with a smaller optical zone and more cuts from their RK. If you have a 4 or 5 mm optical zone, putting in a multifocal IOL will work fine. But it's clearly contraindicated in someone with a smaller optical zone and more cuts. I've done it a couple of times in the latter [small-zone] patient, and in every case I've taken out the IOL."
• Surgical considerations. Once your preop calculations are set, surgeons say the incised RK cornea can still throw some hurdles in your way. The first involves working around the incisions themselves. "If there's enough space, I'll put my cataract incision between the RK incisions," says Dr. Koch. "This is almost always possible with an eight-incision RK. But with a 16-incision RK, for instance, I invariably have to go back into the sclera. I'll just make a little conjunctival peritomy, make a little groove and then dissect forward. Typically, you don't have to suture the scleral incision, but you do have to suture the conjunctiva back in place, or I'd like to, usually." Dr. Gulani recommends not getting too anxious about having to work on a post-RK eye. "Just maintain your technique, keeping it a little lower-flow to keep the pressure in the eye down as you work," he says. He uses the Alcon Infinity with low-flow phaco, Aqualase or phaco chop for this. "But also remember that these patients were once myopic in refraction and still have the myope's ocular anatomy, so all the risks of cataract surgery in myopia [namely retinal issues] still apply."
"The RK incisions can confuse you as you make your capsulorhexis," adds Dr. Packer. "So using capsular stain to highlight the capsule can help you avoid mistaking what you're grabbing when you make your rhexis."
Dr. Majmudar also says it's wise to watch the RK incisions—and the zonules—carefully during the procedure. "The incisions can sometimes open during the procedure, causing micro- or macroperforations, so you have to be prepared to close them with sutures if you see it happening," he says. "I also remember I. Howard Fine stating that these patients may have had a microperforation during their initial RK procedure, which you wouldn't be aware of now. So, be prepared for some zonular laxity due to past shallowing of the chamber during their RK. It might be helpful to have some capsular tension rings nearby in case there's a problem."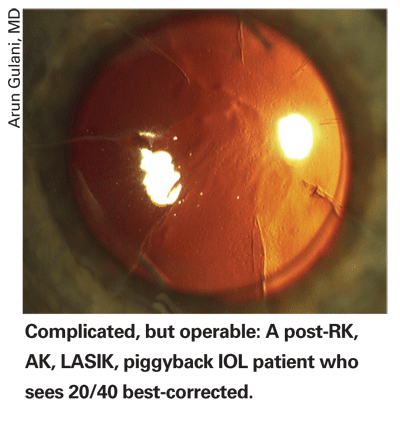
To catch any microperforations that occur during surgery, Dr. Waltz recommends putting a little fluorescein in the eye at the end of the case after the eye's pressurized. "They don't happen often, but it's worth looking for to make sure," he says.
• Be patient postop. One of the key oddities about performing cataract surgery in the post-RK eye, say surgeons, is the effect the incisions have on the cornea postop. "With post-LASIK patients, the flap incision doesn't change much after you do intraocular surgery, so you get a stable effect soon afterward," says Dr. Waltz. "With a post-RK eye, the incisions will soften, and the cornea will flatten somewhat after cataract surgery. For instance, a 42-D cornea may flatten to 41 or 40 D for a while after the cataract surgery; then, as the incisions gradually tighten again, the cornea will go back to what it was, after a few weeks to a few months. This is a big deal, because if you're aiming for
In light of this gradual change, Dr. Packer says it might be a nice courtesy to work a deal with your optical shop for these patients. "It takes a while for these patients to get their best vision, but we don't know when that will be, so make sure to explain that they may need spectacles temporarily and that the correction they need may change, as well. Pre-arranging something with your optical shop to help the patient get some lens changes at no additional cost, or at cost, is nice because he most likely will be dependent on glasses, and you don't want him to have to buy three separate pairs of glasses over two months."
Ultimately, the surgeons say it pays to remember that these post-RK patients can have good outcomes with either refractive or cataract surgery, but will always be the demanding jet-setters who jumped at the chance to have RK back in the 1990s.
"One woman was referred to me after seeing a number of surgeons," recalls Dr. Gulani. "She'd had



