The line between cataract and refractive surgery has become more blurred in recent years as patient demands for impeccable vision have increased and technologies have advanced, particularly in the realm of IOLs. The dawning of the modern-day IOL put tools previously reserved for cataract surgeons into the hands of refractive surgeons for elective procedures. For patients who don’t meet the criteria for corneal refractive surgery, refractive lens exchange has become an appealing alternative to achieve spectacle independence.
However, refractive lens exchange is nuanced. Patients can’t be matched with just any IOL, it’s a careful process of reviewing the benefits and potential trade-offs for each option.
“Just as important as clinical and surgical acumen, is knowing when a patient isn’t a good candidate for a certain procedure,” says Arjan Hura, MD, a cataract, refractive and anterior segment surgeon in practice at the Maloney Shamie Vision Institute in Los Angeles. “Thus, I feel that decision-making about whether to offer refractive lens exchange to a patient, like offering laser vision correction, has to be based on solid ethics, clinical acumen and surgical competency. Much of this is informed by the experience level of the surgeon. Refractive surgeons with the knowledge and skill set for RLE understand the ins and outs, pros and cons, and nuances with patient selection and counseling. The ultimate goal is safely achieving vision correction and helping patients see better and actualize their life. Not everyone is a candidate for RLE.”
Despite the niche criteria for RLE candidates, that hasn’t stopped patients from inquiring about the procedure. “Refractive surgery awareness in the United States is interesting,” says Dr. Hura. “LASIK has such a high level of brand awareness that patients often think of all forms of eye surgery as LASIK. Thus, awareness of other forms of vision correction like RLE may not be as well known. I practice in Los Angeles and operate in Beverly Hills so the awareness of RLE and other specific forms of vision correction is likely higher than average. I often see patients referred to me specifically for refractive lens exchange, or patients who have done their own research or who have friends who have had RLE and are interested in having surgery themselves.”
It’s a trend being noticed in the Midwest as well. “I’m noticing refractive surgery becoming more lens-based,” says William F. Wiley, MD, medical director at the Cleveland Eye Clinic. “We’ve seen younger myopes moving more towards implantable contact lenses, and hyperopes leaning towards lens exchange even at a younger age.”
Presbyopia does play a role in a patient’s candidacy for RLE. “As patients get older, once they get to the presbyopic age, we have to decide: Are they going to be a better candidate for corneal refractive or a lens exchange?” says Dr. Wiley. “There are a few different things that go into that, but when they’re myopic and pre-presbyopic, we’re going to perform either ICL or LASIK/SMILE (corneal refractive). If they’re presbyopic, then we’re going to be considering either LASIK or refractive lens exchange.”
The Nuances of Patient Selection
There are several demographics who are suitable for RLE, Dr. Hura says. “I typically think of RLE as an option on the spectrum of refractive surgery for a patient who’s in their 40s to 60s without signs or symptoms of visually significant cataracts. It’s also a great option for patients who may not be good candidates for laser vision correction, or presbyopes who don’t want monovision. There’s also a subset of younger patients with extreme refractive error who aren’t candidates for laser vision correction or phakic IOLs, or patients with corneal disease who may be good candidates. Patients with very high hyperopia or high levels of astigmatism—these patients tend to be thrilled with the results of RLE,” he says.
Dr. Wiley uses the rule of three to define his home-run multifocal IOL candidate. “A multifocal IOL can, in theory, correct three different vision problems,” he says. “It can correct a cataract if the patient is of that age, it can correct distance vision, and it can also correct presbyopia or near vision. If you’re correcting all three, it’s almost automatically a home run and patients are going to be happy. If you have a cataract patient who’s hyperopic and is already in bifocals, they’re a no-brainer because it’s going to correct the cataract, distance and near, and those are three things they’re already missing in their vision so that’s a home run.”
 |
|
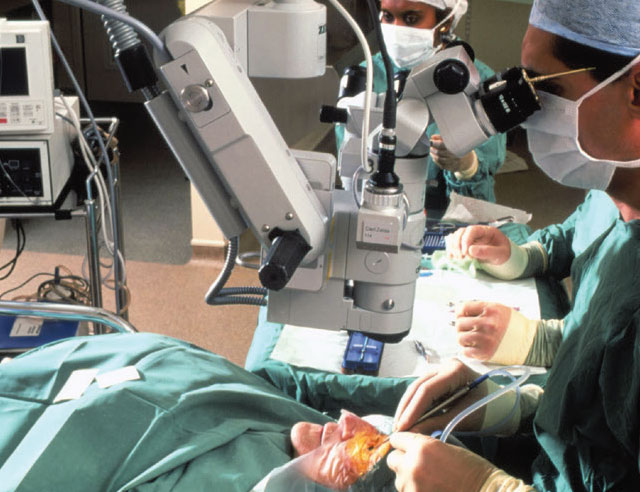
RLE allows patients to take advantage of advancements in IOL technology. Image courtesy of WebMD. |
But it’s a bit different when a cataract isn’t involved. “On the other extreme, the worst patient might be somebody who just turned 40 and is a plano presbyope, and they’re just having a little bit of loss of near vision,” says Dr. Wiley. “In my mind, you’re probably only correcting one issue with the multifocal IOL and those are probably the hardest patients because you’re really not correcting their distance issue. They’re already enjoying great distance vision and they don’t have a cataract yet. They’re just experiencing that loss of near vision and the multifocal lens, although it can treat that patient, I think it’s going to be a harder one to make happen with plano presbyopes.
“More often though, you’ll have patients that are somewhere in between,” Dr. Wiley continues, “such as a 60-year-old who doesn’t have cataracts but is hyperopic or even a higher myope, and so they really can’t see at distance, they really don’t have functional near vision. You’d be correcting two of the three things, and in general if you’re correcting at least two of the three, you’re going to have a relatively happy patient. However, you have to go through some of the expectations that the quality of vision with the artificial lens will be different than what it would be with a natural, clear lens. There are some give and takes. Thankfully, most people over the age of 40 have already started experiencing some dysfunctional lens syndrome symptoms and, although they might not have a full cataract, they have some glare at night or certainly some loss of function, and I think that the new artificial lenses do well for those patients. But again, the more that you’re correcting with their visual problems, I think the higher the chance of patient satisfaction.”
There is one group of patients that should be approached with particular caution, though. “Most of the controversy with refractive lens exchange is related to performing it in high myopes due to the risk of retinal detachment after surgery,” says Dr. Hura. “This is based on data from the 1980s and 1990s and has been followed up every decade with subsequent studies. Although technology and surgery have advanced, the risk of retinal detachment after RLE is related to immutable clinical factors such as pre-existing retinal pathology like lattice degeneration or retinal holes/tears, lack of a posterior vitreous detachment and axial length.”
An extended seven-year follow-up of noncomparative case series evaluated the incidence of complications after clear lens exchange in 52 eyes of 30 patients with myopia greater than -12 D.1 During the seven years, retinal detachment occurred in four of 49 eyes. One patient had bilateral retinal detachments. The overall incidence of posterior vitreous detachment was 16.3 percent.
Another 15-year retrospective study of 437 eyes that underwent refractive lensectomies by a single surgeon revealed a 0.69 percent overall rate of retinal complications, 0.23 percent of which were retinal detachments.2
“In particular if a high myope hasn’t had a posterior vitreous detachment, that risk for retinal detachment goes up because the act of doing the surgery can cause a PVD,” adds Dr. Wiley. “During an examination we’ll check to see whether they’ve had a PVD or not. If they’ve had a PVD, we’re a little more confident with lens exchanges, but if they haven’t had a PVD, we warn them that it could happen and clear lens exchange could exacerbate that at a younger age. We make sure to discuss signs and symptoms of retinal tear detachment.”
Dr. Hura suggests consulting with a retina specialist, or refraining from refractive surgery altogether potentially. “High myopia is typically best treated with a phakic IOL like the EVO ICL,” he says. “If a patient isn’t a good candidate for laser vision correction or EVO ICL, and if RLE is being considered instead for a high myope, I feel that coordination with a retina specialist and thorough informed consent is important. Ultimately, a patient may simply not be a candidate for any form of refractive surgery.”
In addition to evaluating their ocular anatomy, Dr. Hura says every surgical plan must be tailored to the individual and their personality and expectations. “It’s rare that an operating room day goes by where I’m not using lenses from all different manufacturers,” he says. “I view this to some extent as the art of refractive surgery. Getting a patient a great outcome involves more than just safely doing the surgery. Getting to a great outcome involves understanding the patient’s personalities, hobbies and how they use their vision on a day-to-day basis. These are all things I’m assessing: patient personality—are they type A or type B personality? Are they incredibly demanding? Do they have realistic expectations?”
The Right IOL for Each Patient
Modern IOLs give a greater range of vision to patients, but usually come with some caveats. It’s a matter of how much of an impact they’ll make on each patient.
Even easygoing patients need to know about the side-effect profile of multifocal lenses, continues Dr. Hura. “If I have a relatively easygoing patient and they say, ‘Doc, I just want to be out of glasses,’ I’ll usually lean toward the multifocal lenses because we know that they give really good distance, intermediate and near vision. But there’s no free lunch with optics, so the side-effect profile is reduction in contrast sensitivity and increased dysphotopsias at night, which is inherent to the diffractive optics that are used in these types of lenses. I personally tend to overemphasize the side effects of diffractive optics. If after a discussion, the patient says that doesn’t really bother them and they seem pretty laid back, then I know they’re going to do great with a multifocal lens. But if they’re apprehensive about the idea of slightly reduced contrast, halos and glare, then I’ll probably shy away from that lens.
“A patient who’s a good candidate for a multifocal is someone who has a pristine optical system—they don’t have a lot of dry eye, they don’t have Fuchs’ endothelial dystrophy, ERMs, macular degeneration, glaucoma, etc.,” says Dr. Hura.
If they have mild pre-existing ocular disease or they’re averse to the discussed side effects of multifocal lenses, Dr. Hura will discuss an extended-depth-of-focus lens with or without mini-monovision. “I’ll emphasize to patients that there will still be certain situations where they’ll need their reading glasses, such as reading a restaurant menu in dim lighting,” he says.
Dr. Wiley says he uses a variety of lenses, including the trifocal PanOptix (Alcon) and the Tecnis Synergy (Johnson & Johnson). “We’ve been leaning toward PanOptix, but I think they’re both great lenses,” he says. “They have distance, intermediate and near, which is great, but some patients do experience glare and halo so I caution patients that have certain lifestyles—a police officer, truck driver, airline pilot—who might not appreciate the quality of nighttime vision. We’re very aware that there is a trade-off there and some patients are fine with that trade-off and other patients would rather have better clear vision at night without glare and are willing to wear glasses for near.”
Monofocal-plus lenses are a good option for those patients who are concerned about the nighttime symptoms, continues Dr. Wiley. “There are newer lenses marketed as monofocal-plus that give a little bit more intermediate than a traditional monofocal,” he says. “We do have those discussions—if you’re going to take the lens out, should you give the patient the full range with a trifocal, but we also have patients who are fine with a monofocal-plus style lens with really high-quality distance, maybe a little bit of intermediate, but they’ll wear reading glasses and they don’t have the nighttime symptoms that a multifocal would have.”
The Light Adjustable Lens (RxSight) may be a good option for patients who previously had RK, LASIK, PRK or SMILE, some surgeons say. “If they’re post-refractive surgery patients and especially if they’ve enjoyed monovision before, then I tend to opt more for a Light Adjustable Lens,” says Dr. Hura. “This allows the patient to ‘test drive’ their vision after surgery and we can postoperatively refine the refractive error.”
Dr. Wiley agrees. “The LAL does a great job for monovision because it allows you to hit those near and distance targets really nicely,” he says. “Monovision has a little bit higher demand on hitting the visual target so the LAL is going to work great. It allows you to fine tune that intermediate vision or near vision, and the patient can also test drive it before we’ve completely locked it in. This gives them confidence that we’re going to give them the functional near in one eye and distance in the other and they can live with that trade-off before we lock it in.”
Dr. Hura adds, “It’s important to note that in eyes that have had refractive surgery it can often be difficult to achieve the desired refractive outcome after surgery because of the changes that refractive surgery causes in the eye anatomy. Thus, the LAL is a great option in these eyes because, even if the initial refractive target isn’t achieved, the light treatments can get the patient to the finish line.”
Another lens that could put RLE within reach for more patients is the Apthera IC-8 (B + L) and refractive surgeons are excited by the potential.
“The IC-8 lens can certainly be used for refractive lens exchange,” Dr. Hura says. “The small aperture optics of the IC-8 confer extended depth of focus. Typically patients will be aimed plano with a monofocal lens in the dominant eye and then an IC-8 in the non-dominant eye set for about -0.75 D sphere, and that can give quite a broad range of vision as long as the patient understands that they experience a sense of dimming in that eye. The IC-8 can also be used for post-RK eyes, irregular astigmatism or atypical corneas—but this is all off-label.”
Dr. Wiley says he’s still determining the best use for the Apthera. “For someone who’s younger with irregular astigmatism, we found that the small-aperture optic can help neutralize their irregular astigmatism and give some better quality of vision,” he says. “If a patient had previous corneal cross-linking for keratoectasia and I was looking for a visual-quality solution, we can use a small aperture lens to help correct some of the irregular astigmatism and it works almost like a therapeutic clear lens surgery. Not only can it help their lifestyle, but helps treat some of the pathology that’s there. Furthermore, if somebody has been using Vuity eyedrops or pupil modulating eyedrops and really likes the small aperture vision and is used to that but is tired of taking the drops, the IC-8 could be considered. I would do a modified monovision with a monofocal in one eye and a small aperture lens in the other eye.”
Patients may ask what their options are if their eyes continue to change. “I tend to tell them that the main thing that changes over time is the eye’s natural lens as it’s developing a cataract,” says Dr. Wiley. “The fact that we’re removing their natural lens typically removes the main variable that was changing over time. While there’s a chance that you miss the target, that would show itself right away—within the first month or so—but if they’re pretty good within that first month, chances are that the vision is going to maintain over time.”
Dr. Hura considers a few factors in the event of a refractive miss. “If a patient has a virgin cornea—they’ve never had laser refractive surgery—and there’s a refractive miss after RLE, it can be corrected with LASIK, SMILE or PRK,” he says. “But if that refractive miss is significant and noted immediately after surgery, I feel the best way to correct it is to address the issue at the source. This might mean IOL exchange for a different power lens or rotating a toric IOL to the intended axis if postoperative rotation has taken place.”
The Keys to Success
Ultimately, a surgeon’s success with RLE comes down to patient selection and knowledge. “The surgeon really needs to understand the lenses inside and out,” says Dr. Hura. “It’s not enough to know that multifocal lenses give glasses-free vision, you really have to understand the nuances of the optics of all the lens implants because there’s no perfect lens and each one has trade-offs. It also goes without saying, but you have to be a good surgeon and get good surgical results because patients are paying out of pocket for this premium surgery, it’s all elective. You have to be able to deliver the desired outcome.”
Dr. Hura is a consultant and speaker for Alcon, Rayner, Zeiss, Staar and AcuFocus/B + L. Dr. Wiley is a consultant for Alcon, Johnson & Johnson, Staar and Zeiss.
1. Colin J, Robinet A, Cochener B. Retinal detachment after clear lens extraction for high myopia: Seven-year follow-up. Ophthalmology 1999;106:12:2281-4.
2. Stonecipher, Karl et al. Refractive lensectomy outcomes and complications for myopia and hyperopia: A 15-year retrospective study. Medical Research Archives Online 2015;2:5.



