One key source of potential tear-film trouble is the meibomian glands. If the glands malfunction, the lipid layer may be reduced, allowing rapid evaporation of the tear complex. Furthermore, if the glands' secretions become trapped inside the glands, inflammation and bacteria can follow, worsening the problem.
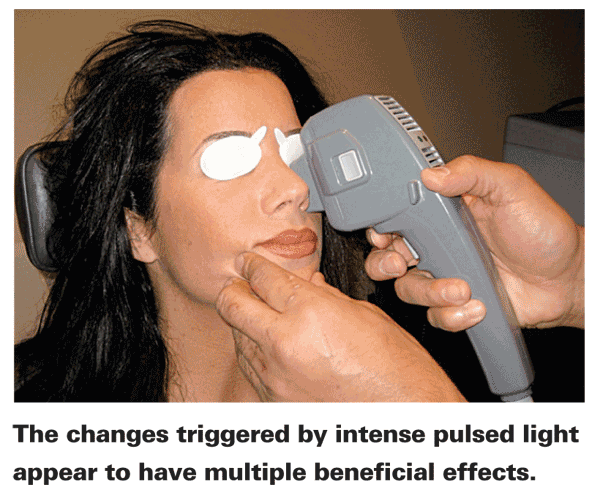
For the past eight years, Rolando Toyos, MD, medical director and founder of Toyos Clinic in Memphis, has been refining a new approach to treating this problem, using intense pulsed light, or IPL, originally developed for use in dermatology. Brief, powerful bursts of light at specific wavelengths (in this case, between 500 and 800 nm) cause changes in blood vessels near the surface of the skin, raise skin temperature and eliminate problematic flora on the skin and eyes,1-5 all of which may have a beneficial effect on meibomian gland dysfunction.
Making the Discovery
Dr. Toyos says he discovered this potential use of intense pulsed light by accident after opening an aesthetics clinic in his practice in 2002. "IPL is FDA-approved for patients with rosacea and acne," he explains. "The light that's emitted from the flashlamp is absorbed by the oxyhemoglobin in the blood vessels on the skin's surface; the absorption generates heat that coagulates the cells, leading to thrombosis of the blood vessels.1-4 This minimizes redness and improves the look of the skin. My rosacea patients who had the IPL treatment would return with their skin looking much better—but some also mentioned that their eyes felt better. On examination, their eyes really were better, even though the IPL treatment wasn't done directly on the glands.
 "So, we began investigating this using different IPL instruments, none of which were designed to treat meibomian gland dysfunction," he says. "We got mixed results. Then in 2003 we received an ASCRS grant to pursue this, and we conducted a small study in which patients with MGD were treated with IPL on one side and nothing on the other side. We found that during some of the time points following treatment, their MGD was better; the lids looked clearer, there was less erythema, fewer blood vessels, thinner secretions, and most important, reduced symptoms."
"So, we began investigating this using different IPL instruments, none of which were designed to treat meibomian gland dysfunction," he says. "We got mixed results. Then in 2003 we received an ASCRS grant to pursue this, and we conducted a small study in which patients with MGD were treated with IPL on one side and nothing on the other side. We found that during some of the time points following treatment, their MGD was better; the lids looked clearer, there was less erythema, fewer blood vessels, thinner secretions, and most important, reduced symptoms."
However, the existing technology was inconsistent, and the bulb's intensity would diminish over time. Dr. Toyos worked with one of the companies, Dermamed, to solvethese problems. "Now, we have an instrument that's safe, with reproducible results," he says. (Dr. Toyos emphasizes that doctors should not attempt this using just any IPL equipment.)
Dr. Toyos says one immediate effect of IPL is that it acts like the "world's best warm compress." "When the light is absorbed by the blood vessels, it generates heat in the dermal layer that melts the secretions and opens the glands," he explains. "So, immediately after treatment we express the glands. We can get out all of the secretions that were stagnating, so patients get some relief right away."
Research in the field of dermatology has uncovered several other relevant effects of IPL treatment. "For one thing, by closing off the blood vessels near the surface of the skin it decreases the inflammatory cytokines6 that contribute to meibomian gland dysfunction," he says. "In addition, IPL decreases the bacterial load on the skin, which is one of the reasons it helps with acne. There's also some evidence that IPL decreases parasites on the eyelash margin that can cause meibomian gland problems."5
Performing the Procedure
"When the patient comes in, we determine the skin type and how severe the meibomian gland dysfunction is," Dr. Toyos explains. "This treatment should only be used for patients whose skin is Fitzgerald type four or below, to avoid causing lightening of the skin color. We then give the treatment from ear to ear; if we just treat the lid, the blood vessels grow back much sooner, requiring more maintenance treatments. Next, after putting an eye shield over the eyes we treat the lower lid."
Dr. Toyos notes that he doesn't directly treat the upper glands. "First of all, when you hit the side of the lid, you close off blood vessels that feed into the upper glands," he explains. "Also, once you get the lower glands working better, the lids appose each other better; as a result, the pumping mechanism that accompanies blinking is more effective in the upper glands. Third, some of the heat is transferred from the side treatment and the lower lids, so you get the warm compress effect on the upper gland indirectly. We've found that the upper glands also open up, allowing us to express them.
"After treatment and expression of the glands we give the patient a drop of Durezol," he continues. "Postopera-tively, we have the patient use Durezol for three days, and Xibrom once a day until they see us again, for inflammation. Then we have the patient use AzaSite at night for 10 days before the next treatment."
Asked whether the results could be attributed largely to the medications, Dr. Toyos says he doubts it. "My initial studies were done without any medications, but patients reported improvement and I saw objective improvement," he notes.
"Also, many patients have come to me after using all of these medications without getting relief. Finally, some of our patients have not used the drops due to cost or allergy, and they still show positive results. But the medications do help to prolong the time between needed retreatments."
Dr. Toyos notes that it usually takes three to four treatments over the course of four months to get the secretions thin and working correctly. "After the gland is normalized we do maintenance treatments every six months to a year," he says. "Younger patients need fewer treatments."
Other surgeons are getting positive results as well. David R. Hardten, MD, director of refractive surgery for Minnesota Eye Consultants and
Getting Started
Dr. Toyos says eight centers in the
"The equipment costs about $50,000," adds Dr. Toyos. "However, there's no click fee, and you get 5,000 shots out of one bulb; then it's about $600 to replace the bulb. It's a solid-state light—not a laser—so it doesn't need maintenance. Plus, this is not covered by insurance, so the technology can pay for itself within a few months. And the instrument we've developed with Dermamed is portable so you can bring it to satellite clinics, etc." With more doctors and clinics now adopting the procedure, Dr. Toyos hopes to begin a large multicenter trial soon.
Dr. Toyos is a consultant to Dermamed, but has no financial interest in the instruments or procedure described. Dr. Hardten has no financial interest in Dermamed or the IPL procedure.
1. Papageorgiou P, Clayton W, et al. Treatment of rosacea with intense pulsed light: Significant improvement and long-lasting results. Br J Dermatol 2008:159;3;628-632.
2. Mark, KA, Sparacio, RM, Voigt, A, Marenus, K, Sarnoff, DS. Objective and quantitative improvement of rosacea-associated erythema after intense pulsed light treatment. Dermatol Surgery 2003;29:6:600-604.
3.
4. Tan SR, Tope WD. Pulsed dye laser treatment of rosacea improves erythema, symptomatology, and quality of life. J Am Acad Dermatol 2004;51:4:592-9.
5. Elmnasser N, et al. Bacterial inactivation using pulsed light. Acta Alimentaria 2007;36:3:401-408.
6. Byun JY, et al. Expression of IL-10, TGF-beta(1) and TNF-alpha in cultured keratinocytes (HaCaT cells) after IPL treatment or ALA-IPL photodynamic treatment. Ann Dermatol 2009;21:1:12-7.



