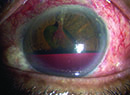
Researchers from the Bascom Palmer Eye Institute and Duke University say that the use of nylon wicks with fenestrations in nonvalved aqueous shunt surgery can help reduce intraocular pressure and glaucoma medication usage in the immediate postoperative period compared with the use of fenestrations alone.
In the retrospective study, the physicians analyzed all nonvalved aqueous shunt insertions completed by one surgeon. Patients had undergone either Baerveldt or ClearPath 350 mm2 aqueous shunt insertion with fenestrations only (n=37) or fenestrations with two nylon wicks (n=92). The surgeon ligated all devices with a 7-0 Vicryl (polyglactin) suture, and either four fenestrations or two fenestrations, and two 9-0 nylon wicks were placed anterior to the ligature.
The investigators collected data on visual acuity, IOP, number of glaucoma medications, and complications from the preoperative visit just before surgery, postoperative day one, week three, week five, and month two. This data was used as the primary outcome of the study.
The researchers found no difference in logMAR visual acuity between the two groups at any time point. At postoperative week three, intraocular pressure was significantly lower in the wick group (14.6 ±7.7 vs. 18.1 ±8.7 mm Hg, p=0.03). The number of glaucoma medications used was significantly reduced in the wick group at three weeks postop (0.5 ±0.9 vs. 1.0 ±1.2, p=0.02) and two months after surgery (0.7 ±1.0 vs. 1.4±1.3, p=0.02). There was no significant increase in the overall rate of complications in the wick group, but there was a higher rate of transient hyphema (28 percent vs. 8 percent, p=0.02).
The researchers say that, as the surgeon waits for the ligature suture to dissolve after nonvalved aqueous shunt device implantation, the use of two nylon wicks with fenestrations can significantly lower intraocular pressure and medication burden.
J Glaucoma 2021;30:32-36.
Swaminathan S, Quist M, Dawson L, et al.
Low-concentration Atropine for Myopia Progression
Researchers from the Chinese University of Hong Kong and Hong Kong’s Tung Wah Eastern Hospital evaluated the effect of age at treatment and other factors on the treatment response to atropine in the Low-concentration Atropine for Myopia Progression (LAMP) study, as part of a secondary analysis from a randomized trial.
Participants included 350 children, ages 4 to 12 years old (randomization was stratified by age and gender) originally assigned to receive 0.05%, 0.025%, 0.01% atropine or placebo once daily in both eyes, who completed two years of the LAMP study. In year two, the placebo group was switched to 0.05% atropine.
The change in spherical equivalent and axial length over two years were evaluated by generalized estimating equations in each treatment group.
Other factors evaluated included age at treatment, gender, baseline refraction, parental myopia, time outdoors, diopter hours of near work and treatment compliance.
Here are some of the findings:
- In the 0.05%, 0.025%, and 0.01% atropine treatment groups, younger age of the patient was the only factor associated with spherical equivalent progression (coefficient=0.14, 0.15 and 0.20, respectively) and axial length elongation (coefficient=-0.10, -0.11 and -0.12, respectively) over two years; the younger the subject age, the poorer the response.
- At each year of age from four to 12 across the treatment groups, researchers found that the higher-concentration atropine showed a better treatment response, following a concentration-dependent effect (p<0.05).
- The mean SE progression in 6-year-old children using 0.05% atropine (-0.90 D; CI, -0.99 to -0.82) was similar to that of 8-year-old children using 0.025% atropine (-0.89 D; CI, -0.94 to -0.83), and 10-year-old children using 0.01% atropine (-0.92 D; CI, -0.99 to -0.85).
The researchers report that all of the atropine concentrations were well-tolerated at all of the patient age groups.
The investigators found that younger age was associated with poor treatment outcomes with low-concentration atropine 0.05%, 0.025% and 0.01%. They added that, among atropine concentrations studied, younger children required the highest concentration, 0.05%, to achieve a reduction in myopic progression similar to older children on lower concentrations. τ
Ophthalmology 2021;Jan 21 (epub ahead of print).
Li F, Zhang Y, Zhang X, et al.