Today, cataract surgery—the most performed surgery in the world—is a very high-tech operation. Because today’s surgeons use some of the most sophisticated tools available in medicine, understanding the technology has become as important as understanding how to perform the surgery itself.
“Phacoemulsification is a very complex, delicate surgery,” notes Nick Mamalis, MD, a professor of ophthalmology, director of ocular pathology and co-director of the Intermountain Ocular Research Center at the Moran Eye Center at the University of Utah in Salt Lake City. “You can get into trouble if you don’t do it properly, or if you don’t have the proper equipment. But all of the phaco machines have gotten much better in recent years. That makes a big difference—especially with novice surgeons.
“My colleague, Randy Olson, MD, has been doing a series of experiments looking at the effectiveness of this new generation of phaco technology,” he continues. “His team has found a way to modify a pig’s eye nucleus to mimic the characteristics of a human nucleus. Then he sees how efficiently the new technologies emulsify little cubes of that nucleus material. Each of these systems has been shown in the lab to efficiently dissect a hard-lens nucleus without using much energy inside the eye. This is a big advance in phaco, across the board.”
Here, surgeons share their experience with three of the most advanced phacoemulsification machines currently available in the United States (in alphabetical order): The Centurion (from Alcon); the Stellaris (from Bausch+Lomb); and the new Veritas (from Johnson & Johnson Vision). Then, they offer some tips for making the most of whichever machine you’re using.
The Centurion
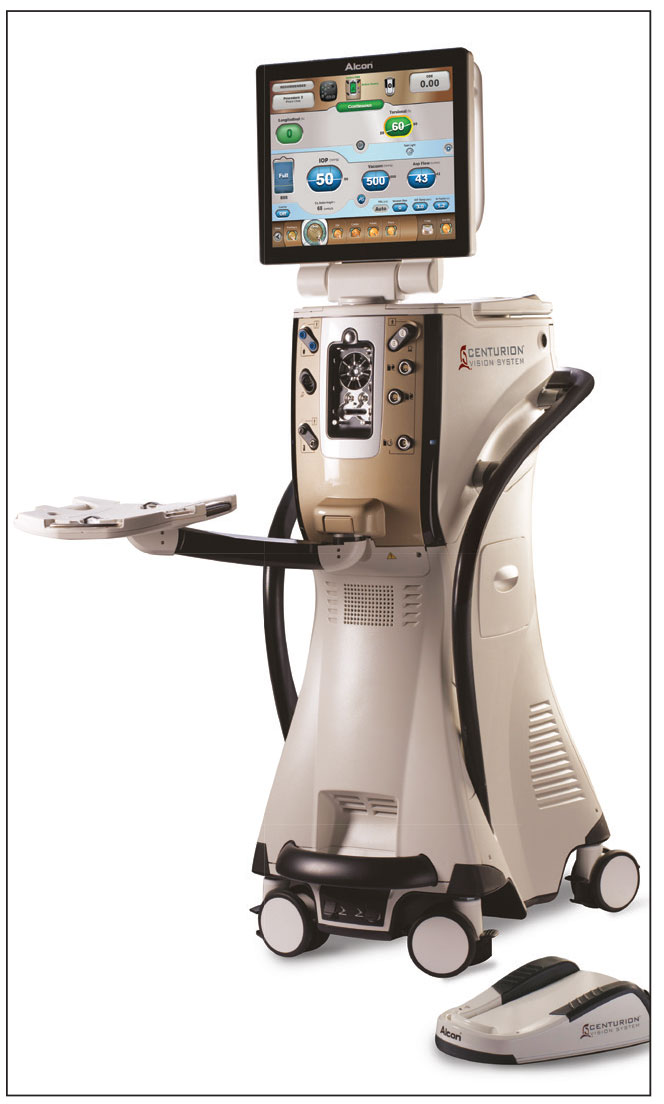 |
| Alcon’s Centurion offers Active Fluidics for anterior chamber stability and Ozil tip movement for enhanced emulsification. |
Alcon’s Centurion features Active Fluidics, a system that compensates for pressure changes in the eye during surgery, thus helping to maintain a surgeon-selected IOP. The company says the combination of Ozil Technology (relating to the phaco tip’s motion), the Intrepid balanced tip and the Centurion’s fluidics allows for enhanced emulsification that requires minimal fluid and produces a reduced temperature rise inside the eye. (The company says the cumulative dissipated energy generated during surgery is 39 percent of that generated by the previous Infiniti Vision System.)
According to Alcon, additional key features of the Centurion include:
- a graphical user interface that displays essential data and allows the surgeon to easily adjust system parameters;
- a wireless remote that allows technicians to control the machine from different areas within the OR;
- an HD monitor with a 19-inch adjustable touch-screen interface that’s easily visible;
- an adjustable instrument tray for ease of working on either eye;
- a task light for illumination wherever it’s needed;
- a foot handle that allows surgeons and techs to move the machine after scrubbing in;
- an ergonomic, easily storable wireless footswitch that allows extended mobility in the OR, with an optional power cord for additional power.
Conquering the Surge
Dr. Mamalis says his phaco experience has largely been using the Centurion. “This machine has been quite an advance,” he says. “When we’re doing phacoemulsification, the ultrasound tip often catches a piece of the nucleus, and as we’re trying to emulsify it, it may break loose, resulting in a post-occlusion surge and shallowing of the anterior chamber. This has long been a potential source of trouble during cataract surgery.
“The Centurion has a system called Active Fluidics that reduces the occlusion-break surge,” he continues. “When you’re preparing for surgery, you set the pressure that you want to maintain inside the eye, and the machine constantly monitors the pressure during surgery. When you get an occlusion break, the system recognizes it immediately and pumps more fluid into the system to counteract the potential surge before the chamber can shallow. I think this has been a real advance in phaco safety. Because I’m at a university, I spend a lot of time teaching residents, and they frequently get occlusion breaks. With the older systems, the anterior chamber would shallow and there’d be an increased risk of a complication such as a posterior capsule tear. That’s no longer an issue.”
Other surgeons agree that the Centurion’s fluidics are a big selling point. Richard Mackool, MD, medical director at The Mackool Eye Institute and Laser Center, and senior attending surgeon at the Mt. Sinai New York Eye and Ear Infirmary and New York University Medical Center, believes the most important aspect of phaco technology is the fluidics. “The pressurized infusion system of the Alcon Centurion—Active Sentry—detects and responds to aspiration pressure changes within the phaco handpiece,” he says.
Elizabeth Yeu, MD, who practices at Virginia Eye Consultants in Norfolk, serves as an assistant professor in the department of ophthalmology at Eastern Virginia Medical School and is medical director of the Virginia Surgery Center, has used both the Centurion and brand new Veritas machines. “The Centurion has extremely stable fluidics and excellent utilization of ultrasound energy,” she says. “It allows me to efficiently disassemble all densities of nuclei and trust that there will be minimal post-occlusion surge.”
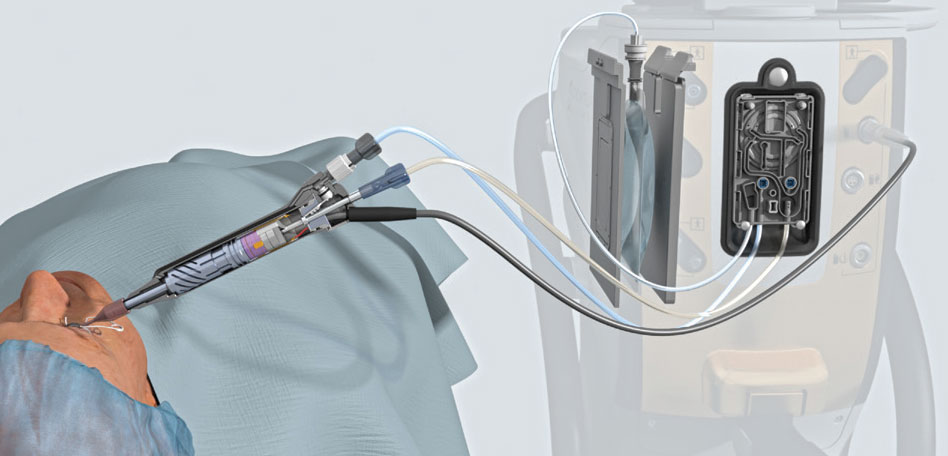 |
| Centurion’s Active Sentry handpiece and Active Fluidics system. |
Other Features
Additional Centurion features noted by surgeons include the Ozil technology, the optional Intrepid Transformer handpiece and its ability to easily break up hard pieces of nucleus.
“With Alcon’s Ozil technology, the phaco tip works with an oscillating, side-to-side motion,” explains Dr. Mamalis. “The old phaco machines moved the needle in and out, almost like a jackhammer. The harder the nucleus was, the more likely it would be repulsed from the tip, leaving hard fragments bouncing around inside the anterior chamber. The Ozil system’s oscillating motion allows us to keep a piece of hard nucleus at the tip, so it can be emulsified without being repulsed.”
Dr. Mamalis notes that the oscillating motion also allows a hard nucleus to be emulsified more efficiently. “That means less cumulative dispersed energy, or CDE,” he says. “That’s important because theoretically, reducing the energy put into the eye reduces the risk of complications. In fact, this is a focus of all of the modern phaco machines: more efficient removal of the cataract without putting so much energy into the eye.”
Sheri Rowen, MD, medical director at NVision Eye Centers in Newport Beach, California, and a clinical assistant professor of ophthalmology at the University of Maryland, has used both the Stellaris and the Centurion. She says she likes the Centurion a lot. “It works well, and it’s very safe,” she notes. “I love the way the Ozil tip works. It’s very efficient. It’s good at breaking up hard lenses and pulling the pieces into the port; it crushes them easily.”
Deepinder K. Dhaliwal, MD, L.Ac, a professor of ophthalmology at the University of Pittsburgh School of Medicine, and the director of refractive surgery and the Cornea Service at the UPMC Eye Center, uses both the Stellaris and Centurion phaco machines when doing surgery at different locations. She sees advantages to both. “The Centurion is a great machine,” she says. “It’s extremely efficient when you’re removing the nucleus—it rapidly emulsifies it. However, it works differently from the Stellaris. It doesn’t have active vacuum. You have to occlude the tip to build vacuum.”
 |
| The Centurion’s Intrepid Transformer handpiece easily converts from coaxial use to bimanual, allowing the surgeon to reach cortex directly beneath the incision. |
Mark Hansen, MD, anterior segment surgeon and partner at Minnesota Eye Consultants, and fellowship director and adjunct faculty member at the University of Minnesota, has used all of the phaco platforms. “One thing that’s nice about the Centurion is that it has an optional irrigation/aspiration handpiece, called the Intrepid Transformer, which can be easily converted from coaxial to bimanual,” he notes. “Oftentimes, the most difficult part of cortex removal is removing the cortex that’s lying right below the incision. The Transformer handpiece makes it very easy to reach that because the aspiration port can be separated, allowing the surgeon to switch to bimanual surgery and use the paracentesis rather than the main incision. You just have to make an extra paracentesis, and then it’s really easy to get to the subincisional cortex.”
The Stellaris
According to Bausch+Lomb, the Stellaris Vision Enhancement System enables micro-incision (less than 2 mm) cataract surgery (MICS) through a flexible, hybrid approach to fluidics and advanced, ultra-efficient cutting dynamics. The company notes that the potential advantages of 1.8-mm-incision MICS include increased wound sealability; a reduction in endothelial cell loss; less surgically-induced astigmatism; and a more rapid visual recovery.
 |
|
The Stellaris includes customizable fluidics control and a Venturi pump, the ability to perform micro-incision cataract surgery and dual-linear foot pedal control. |
The system features:
- StableChamber Fluidics, which can be customized based on either flow or vacuum control, which the company says allows safe, efficient and predictable chamber stability during the procedure;
- the Attune Energy Management System, designed to deliver enhanced followability, reduced heat generation and increased phaco efficiency using minimal energy during cataract removal. It includes a six-crystal handpiece that delivers consistent 28.5-kHz energy with increased stroke length, and software that provides dual-linear control, front or back loading profile and programmable waveform modulation.
The Stellaris also features:
- a Bluetooth foot pedal;
- an 18-inch user interface with a video inlay and overlay; and
- a dual light source with surgeon-selected color filters that can enhance the surgeon’s ability to see ocular tissue better under various conditions.
One feature that particularly appeals to many surgeons is the Stellaris’ Venturi pump. “When you’re performing phacoemulsification, you want safety, control and efficiency,” Dr. Dhaliwal notes. “The Stellaris’ Venturi pump and active vacuum give me a lot of control. I can do more specialized things when I’m using active vacuum. I can finesse things a little more.”
Dr. Hansen agrees. “I like the Venturi pump system,” he says. “I like the machine being reactive, moving quickly and responding to the foot pedal touch immediately, rather than waiting for the pump system to build up.”
Dr. Rowen also says her favorite feature of the Stellaris is the Venturi pump. “I don’t have to occlude my port to pull a piece of nucleus to it,” she explains. “It’s very efficient.”
Additional Features
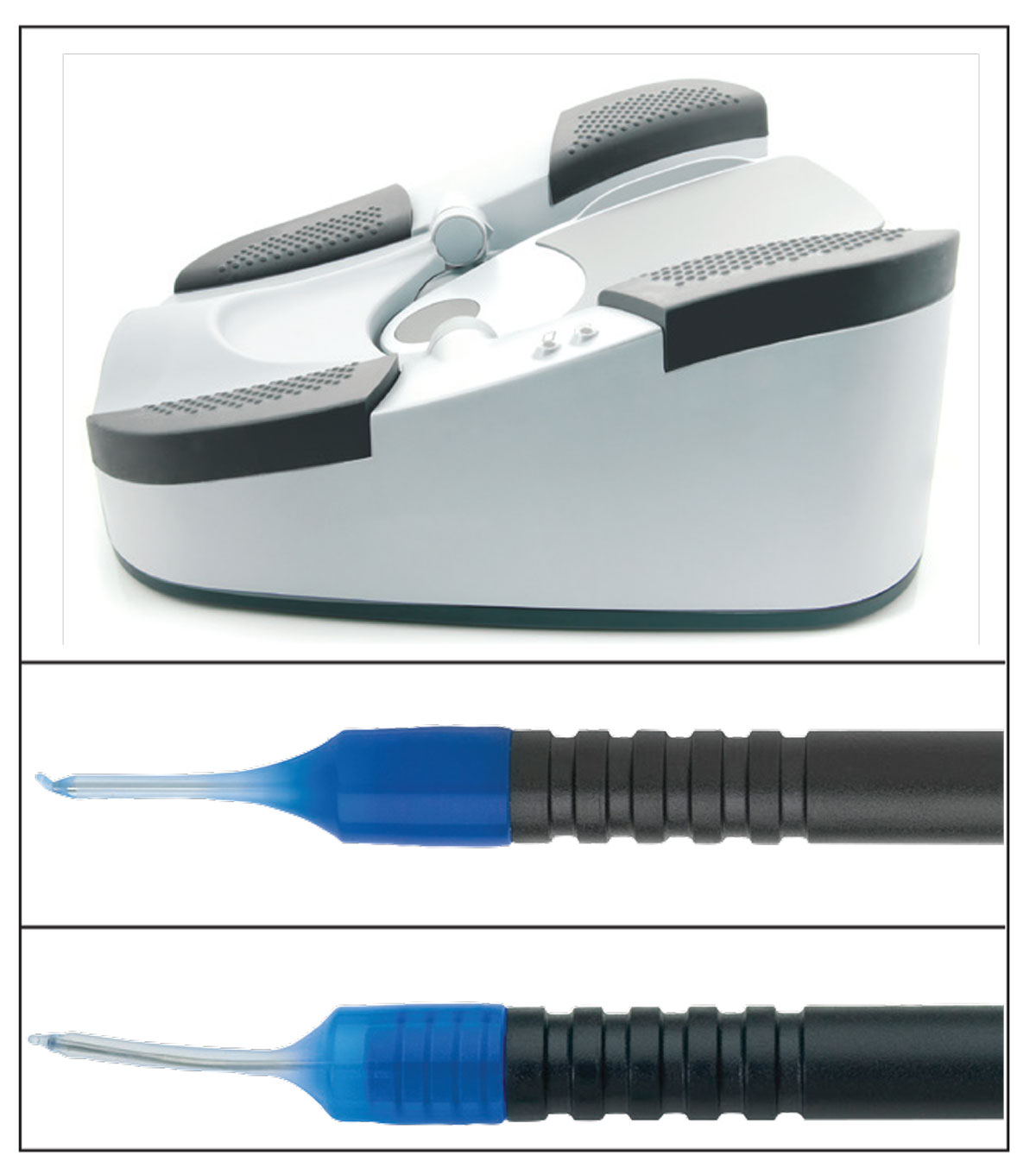 |
| The Stellaris dual-linear foot pedal works well with the Venturi pump, according to surgeons. Surgeons also report that their preferred phaco tip works well regardless of cataract density. |
Other features that have impressed surgeons using the Stellaris include its dual-linear foot pedal, its customizability, not having to change the phaco tip, and its irrigation/aspiration handpiece tip.
“I love the foot pedal, which gives me dual-linear control of different parameters,” Dr. Dhaliwal says. “I can get just a tiny bit of phaco when I want it, especially when I’m doing epinuclear removal. I don’t have to press all the way down on the pedal and build a lot of vacuum, and only then initiate phaco. That’s what happens with a peristaltic machine. With a Venturi machine you can go down as much as you want on the vacuum and then just yaw over with the foot pedal and get a little bit of phaco. And, this is true in all of the different modes. When I’m sculpting, if I want a little more vacuum I can achieve that with a yaw. I feel like I have more control when I’m using the Venturi system and the dual-linear foot pedal.”
Dr. Hansen also appreciates the dual-linear control provided by the foot pedal. “I find this very helpful with complex lens exchanges when a vitrectomy is planned,” he explains. “Being able to toggle between irrigation/aspiration and cut is essential. Because of this ability to control the settings with the foot pedal I use the Stellaris in complex cases such lens exchanges, traumatic cataracts, dislocated lenses, and cases where I know I’m going to be doing an anterior vitrectomy.”
“The Stellaris is totally customizable,” Dr. Dhaliwal adds. “You can program the machine to do what you want it to do. In fact, you really need your company rep to be there when you set it up, to help you understand how the parameters should be set to work with your technique. This is definitely not ‘One size fits all.’ ”
Another factor noted by Stellaris surgeons is not needing to change the phaco tip to manage different types of cataracts. Dr. Dhaliwal says the curved phaco tip on the Stellaris works equally well in multiple situations. “I don’t switch to a different tip, whether the cataract is dense or soft,” she says. “With other systems, I have to change the phaco needle to make sure I get enough cutting.
“The other thing I really like is the I/A handpiece tip, which is called ‘Capsule-guard,’ ”she adds. “It has that name for a reason. The tip is made of a silicone that’s gentle enough that it won’t pop through the capsule, but strong enough that if you need to get rid of a piece of nucleus you missed, you can mash it into the I/A tip using a second instrument. You can use this tip with any phaco machine, although it’s a Bausch + Lomb product.”
Dr. Rowen agrees that the B+L irrigation/aspiration handpiece tip is a big plus. “The tip with the capsule guard is my favorite instrument for this purpose,” she says. “It takes the cortex really nicely, and it’s very safe.”
The Veritas
 |
| The new Veritas Vision System from Johnson & Johnson Vision lets surgeons switch between Venturi and peristaltic pumps, even during a single case. |
As of this past summer, Johnson & Johnson Vision announced the worldwide availability of its new Veritas Vision System. The company states that the Veritas was designed to increase efficiency, patient safety and surgeon comfort during use. According to the company, the Veritas’ innovations include:
- Hybrid Fluidics Technology, designed to minimize post-occlusion surge, using Intelligent Occlusion Sensing Technologies, a system that automatically responds to occlusions.
- A phaco tip that takes advantage of the company’s WhiteStar micropulse technology, featuring elliptical tip movement and using less energy than previous systems.
- Veritas’ Dual Pump System, which gives the surgeon access to both peristaltic and Venturi pumps. The company says the system can transition between the two at any point during surgery, on demand.
- An ergonomically designed, comfortable-to-use foot pedal that gives the surgeon total control.
Sumit (Sam) Garg, MD, vice chair of clinical ophthalmology, medical director and a professor of cataract, corneal and refractive surgery at the Gavin Herbert Eye Institute, University of California, Irvine, has been using the new Veritas system for the past several months. He lists a number of things that he believes make the Veritas exceptional.
“Perhaps most impressive, you can use either a peristaltic or Venturi pump—and you can use both in the same case,” he says. “I typically start off making my chops in peristaltic; then I move to Venturi for nuclear fragment and viscoelastic removal. Venturi tends to be a little more efficient; with peristaltic, you get a little bit better holding of the lens when you’re trying to chop it up. Maybe that flexibility doesn’t make much difference in routine cases, but in complex cases it’s nice to have. Also, if you’re in a center with multiple surgeons who have different operating styles, this is a big advantage.”
Dr. Yeu has also had the opportunity to use the new Veritas, and says her experience has been good. “The fluidics have superior stability,” she notes. “The Veritas offers both peristaltic and Venturi fluidics, and I prefer to use both types. I specifically love that I can have Venturi occlusion-independent rise of vacuum during the removal of cortex, and then thorough removal of viscoelastic device after IOL placement.”
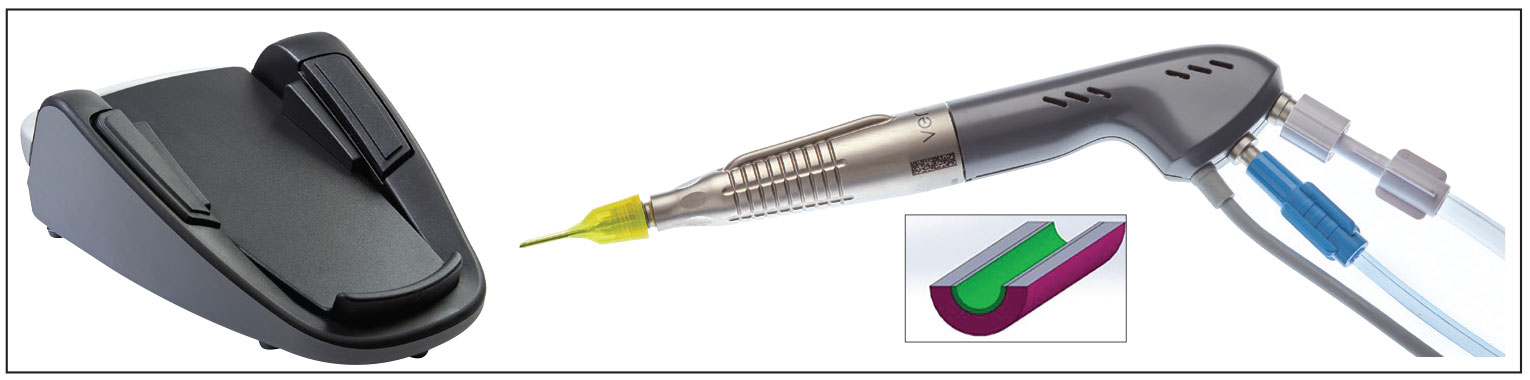 |
| Notable features of the new Veritas machine include the ergonomic foot pedal, the swivel handpiece that reduces drag, the ability to use multiple tips and still have the system’s unique elliptical tip movement, and the two-layered tubing that adds chamber stability. |
Additional Features
“One key thing about the Veritas is that it lets you operate the way you want,” Dr. Garg says. “It allows surgeons to customize the machine to match the way they prefer to operate. You can use a curved tip or a straight tip. You can use a 20-gauge needle or a 19- or 21-gauge needle. You can use a high-infusion sleeve.
“The company has made two changes that add to anterior chamber stability,” he continues. “The system now has pressurized infusion, and a new type of tubing called dual durometer aspiration tubing. Most other tubing is made of the same material all the way through; this tubing is made from two different compounds with different rigidity. There’s a slightly harder tubing on the inside, so there’s less chance the tubing will collapse, and a slightly softer material on the outside, which allows for good flexibility without a lot of drag. This modification, along with the pressurized infusion, contributes to a very stable anterior chamber. In fact, because of the tubing, the anterior chamber stability is now so good that I rarely need to use the pressurized infusion.
“A third factor that’s worth mentioning is that because the system is brand new, all the electronics are current,” he says. “The processing speed is very fast. If you look at the bench testing done by the company, the occurrence of surge is very low and recovery is faster than any other system on the market. That has implications for patient safety.”
Dr. Garg says another very useful feature only available in the Veritas is a swivel handpiece. “When phacoing you often feel a little bit of resistance or drag on the handpiece,” he explains. “That’s either because of the weight of the handpiece or because of the tubing. The Veritas has a swivel handpiece, where the back end of the handpiece stays fixed while the front part swivels independently. This gives you more maneuverability. I don’t feel any resistance when I’m using it.”
In terms of the phaco tip, Dr. Garg notes that the idea of a moving tip was invented by Alcon, currently available in their Ozil format. “The Veritas has a different movement call Ellipse, which is basically an elliptical motion,” he explains. “The nice thing about it is that you can use it with any needle configuration you want, such as curved or straight. My partner uses a straight tip; I like to use a curved, beveled tip, which allows for better power modulation and more efficiency. Other machines only produce their motion with one type of phaco tip.”
Dr. Garg adds that he also finds the new graphical user interface and foot pedal to be very user-friendly. “The GUI is more intuitive than the previous system [the Signature Pro],” he says. “The screen is color-coded in such a way that you can just glance at it and know exactly where you are in the system. Meanwhile, the new foot pedal is very ergonomic. I think it’s an improvement over the previous version, in respect to its weight, travelability and features.”
Dr. Garg says that, overall, he’s found the Veritas to be very efficient. “I haven’t had any issues with soft or hard cataracts, pseudoexfoliation, post-vitrectomy eyes—all of the complex cases we commonly see. So far, the machine has done really well.
“Whenever there’s a new phaco machine, people want to know whether it’s worth looking at, worth trying a demo,” he adds. “In this case, I think it’s worthwhile. It’s a noticeable change from the prior version, the Signature. I didn’t think the change from Signature to Signature Pro was all that dramatic. But this system is a significant advance.”
Maximizing Your Machine
Phaco and Femto Today, some surgeons use a femtosecond laser to break up the nucleus before removal. They note that the most significant phaco machine feature in this situation is the type of vacuum it allows you to use. “There’s an advantage to using a Venturi pump if you’re using a femtosecond laser to break the nucleus up into tiny pieces,” notes Sumit (Sam) Garg, MD, medical director and a professor of cataract, corneal and refractive surgery at the Gavin Herbert Eye Institute, University of California, Irvine. “A peristaltic pump only builds vacuum when the tip is occluded, so a nucleus fragment will only come to the tip if it’s very close. With the Venturi pump, you don’t need occlusion to create vacuum. As a result, you don’t need to chase the chips that are farther from the phaco tip; they come to the tip. That allows surgeons to keep the phaco needle in the center of the eye, away from delicate structures such as the iris or the posterior capsule.” Sheri Rowen, MD, medical director at NVision Eye Centers in Newport Beach, California, and a clinical assistant professor of ophthalmology at the University of Maryland, agrees. “Having a Venturi pump is ideal when you’re using a femtosecond to break up the nucleus,” she says. “The pieces come right up to the phaco tip.” |
Whatever phaco system you’re using, surgeons offer these tips to make the most of the technology:
- Choose a phaco machine that works best with your preferred style of lens removal. Dr. Rowen points out that different phaco machine features may make more sense with a particular lens removal technique. “Some surgeons divide and conquer the lens; some split the lens; some people chop it; some hold it while they’re fracturing it,” she explains. “The different pumps, phaco tips and other features may be more helpful with one method of lens removal than another. Surgeons should try out the different options and pick the machine that works best with their favorite style of lens removal.”
- Understand how your machine works before you use it. “Before you start using any phaco machine, it’s imperative to become well-versed in its features—especially the vacuum pump—and how the machine works,” says Dr. Dhaliwal. “I use both peristaltic and Venturi machines, so I know how different they are. For example, you may have to modify your technique depending on whether you have active vacuum or not. Saying that there was a problem during surgery because you didn’t know how to use the machine isn’t acceptable.”
- If you switch machines, make sure your phaco tip and sleeve match your incision size. Many surgeons use different phaco machines at different ASCs or hospitals. “When switching to a different machine, if you’re using the wrong blade for the wrong tip and the wrong phaco sleeve, you’ll get a lot of leakage around the tip and cause the chamber to collapse frequently,” Dr. Hansen points out.
- Optimize the settings to match your preferred technique for nucleus removal. “There are many ways to remove a cataract,” Dr. Hansen points out. “You may like divide-and-conquer, or horizontal or vertical chop, or just flipping the nucleus into the anterior chamber. However, they all require different phacodynamics, so the settings should be adjusted—especially when you’re starting on a new machine or switching between machines.”
- Use your company reps as a resource. “Anytime you gain access to a new machine, it’s extremely helpful to have the company representative give you a tour of the options, until you’ve fine-tuned your process to match your machine,” notes David R. Hardten, MD, FACS, a founding partner at Minnesota Eye Consultants in Bloomington, Minnesota.
Technique Tips
These suggestions will help ensure that you and your phaco unit produce great outcomes:
- Don’t limit yourself to a single phaco technique. “It’s important to be comfortable with a wide range of techniques, so you can match the lens you’re conquering,” says Dr. Hardten. “Some lenses are easier to manage with a supracapsular approach, some with vertical chop, some with horizontal chop, and some with divide-and-conquer.”
- Remember that different needles, sleeves and incisions require different phaco settings. “It’s important to understand that changing one factor in your phaco setup will probably require a change in your settings,” notes Dr. Garg. “I use different settings for different needles, depending on the density of the lens and what I’m trying to achieve. I’ve seen other surgeons try to use my phaco settings with a different needle, and the machine behaves differently, affecting chamber stability.”
- Make sure the infusion is off before coming out of the eye. “Many surgeons leave the infusion on when they’re coming out of the eye,” notes Dr. Garg. “That leads to a greater chance of iris prolapse. That’s especially problematic in patients who have floppy iris syndrome.”
- If you need to perform a vitrectomy, use a smaller-bore, higher-cut-rate vitrector. “The newer phaco machines have very-high-cut-rate vitrectors, which is great for elective cases, or unplanned situations in which you have to do a vitrectomy,” notes Dr. Garg. “The higher the cut rate, the more efficiently and safely you can remove vitreous, without causing traction. All of the new systems offer this, but many surgeons will stick to a larger-bore, 20-gauge vitrector. Having that much vitreous sucked out at once can be quite jarring to the eye. Using the smaller bore allows for a smoother removal of vitreous, whether planned or unplanned.”
Dr. Garg is a consultant to Johnson and Johnson Vision. Dr. Rowen consults for Alcon and Bausch + Lomb. Dr. Yeu consults for Johnson & Johnson Vision and is on the speaker’s bureau for Alcon. Dr. Mackool is a consultant for Alcon. Drs. Dhaliwal, Hardten, Mammalis and Hansen report no financial ties to any product discussed.