Ophthalmologists and professional athletes have more in common that you might think. Both need to maintain a level of physical ability, and stay on top of their nutrition, in order to be at their best. And, sometimes, both end up sacrificing their bodies for their professions. However, this doesn’t have to be the case for the modern ophthalmologist. In this article, we’ll take a look at how to optimize the ergonomics of a practice so that ophthalmologists can continue to perform surgery and diagnose patients without pain.
Preventative Measures
In a paper published in August of 2017, Santosh Honavar, MD, takes a thorough look at what he terms “modifiable risk factors” and some of the main physical struggles an ophthalmologist faces. According to Dr. Honavar, physical strains directly associated with the ophthalmic profession include stress on the shoulders, neck, back, arms and hands resulting from poor posture during examination and surgery. He also identified repetitive actions common to the surgical profession as some of these modifiable risk factors.1
One of the potential solutions to these problems is the ergonomic redesigning of workplaces.
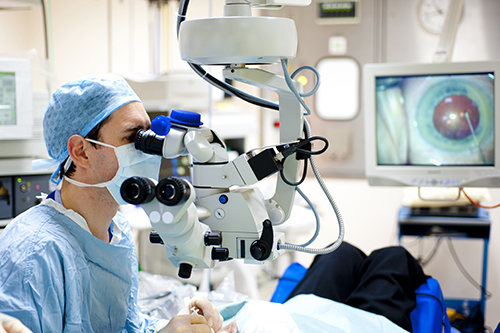 |
| The surgeon’s typical posture during cataract surgery can wreak havoc with his neck and back over time, say physicians. |
Surgeons say there are many measures you can take both in the exam lane and in the operating room to ensure that you’re not putting yourself at risk for years of pain and unnecessary stress. According to Dr. Honavar’s research, a survey of U.S. ophthalmologists revealed that 52 percent of the 697 respondents reported neck, upper body or lower back pain, with 15 percent having to set aside their work as a result.1
John Jarstad, MD, director of
“Now, thankfully, there are several things that can be done to prevent neck and back injuries,” he says. “Those include positioning the microscope at a comfortable angle for yourself in the OR. Another tip is to raise the patient up to eye level where you as a surgeon are comfortable so you don’t have to hunch over.”
Larry Patterson, MD, medical director of Eye Centers of Tennessee, offers similar advice. “One thing that’s really important is
“When I’m doing cataract surgery, I tilt the patient’s head about 30 degrees towards me and we tape it in place there,” Dr. Patterson continues. “I have my microscope tilted back a bit as well, so I can sit there relaxed, leaning back a bit, and I can remain comfortable during the procedure.”
Sandra Woolley,
Aside from making good, healthy lifestyle choices outside of the office, ophthalmologists also have the opportunity to be more comfortable in their own offices and ORs by adjusting their equipment and office layout. “Make sure the computer monitor is sitting at eye level; hands are on the keyboard at elbow height or slightly lower; and feet are flat on the floor,” Dr. Woolley says “For surgery, raise the bed so the patient comes up and you don’t have to lean forward; bring the scope up so your head is in a neutral position and there’s no backward extension. These may sound like silly little things, but they do add up.”
Dr. Patterson also provides some insight into the ergonomics of his practice. “I think it’s personal preference,” he says. “Just go with what you’re most comfortable with. Personally, I don’t like those chairs that have back supports. They’ve just never really worked for me. When you’re seeing patients and sitting at the slit lamp one person after another, get a chair and lamp that are comfortable for you.”
Dr. Jarstad offers his
Personal Routines
Aside from the ergonomics of an office, there are plenty of ways for ophthalmologists to stay in shape based on lifestyle choices.
“Like a number of us ocular professionals, growing up, I wasn’t a jock,” Dr. Patterson says. “We’re academics. We’re not all football or basketball stars, but I’ve since realized that I need to take care of myself as if I were an athlete. In med school, I started having back problems. And I would guess that ophthalmologists, by the nature of our work, have a high rate of back and neck problems. I started being more careful, but it wasn’t until later in life that I started going to the gym regularly and thinking about nutrition.
“I have a personal trainer now,” Dr. Patterson continues. “I get up each morning around 5:40 and meet him at the gym. We work out pretty hard for about an hour. I do that four times a week. I’ve been a relatively healthy eater, but now I’m trying to take that to another level. I’m 58 years old and I’m probably in better shape than I was when I was 20. It’s not just your practice—it’s you getting older.
“We as ophthalmologists deal with more older people than most other specialties,” he continues. “We see both ends of the spectrum. We see the guy who’s 65, smokes cigarettes, is overweight and has diabetes. On the other hand, we’ll see a patient who’s 80, never smoked, has remained active and was always careful about what he put in his body, and he’s in terrific shape. They kind of give you hope looking forward. If anyone can see the effects of how you treat your body, it ought to be us. When you go to the grocery store at 80, you want to be able to walk around instead of being propelled. I have virtually no back issues right now because of these habits.”
Dr. Jarstad also weighs in, describing some of the routines he uses to stay on top of his health outside of the clinic. “I’d say, get an ab trainer or sit-up bench,” he says. “They can range anywhere from $100 to $2,000. I was doing 400 sit-ups per day, but I’ve fallen back to 50 to 100 recently. It’s important to strengthen your core because that really affects your posture. As you strengthen the opposing muscle group, the back muscles also get into shape. I also recommend walking, cycling, rollerblading, skiing and water activities—anything that lets you be active and doesn’t feel like a chore. You can enjoy it.”
However, if you missed the boat and are already suffering from some sort of
Ergonomics vs. Outcomes
As to whether or not efficient ergonomics is related to good outcomes, Dr. Patterson says that ergonomics surely matters during surgery. “I used to have a tendency, when things got tense in surgery, to tighten up my shoulders, causing them to lift up a bit,” he says. “It would put a
“I’ve seen people hunched over their microscopes, and it just looks awkward and uncomfortable,” Dr. Patterson adds. “That’ll come back to bite them. They’re going to have pain eventually if they have a high-volume surgical center. You should be as comfortable as you would be at home reading a book. You need to get yourself into that mindset. Just because its surgery doesn’t mean everything has to be stressful.”
Dr. Jarstad agrees that poor ergonomics will likely result in poorer results for your practice. “Remember, as an ophthalmologist, you’re like a major league baseball or football player,” he says. “Those teams provide nutritionists, physical therapists, sports psychologists, masseuses and many other perks to keep those athletes in top form day after day. Shouldn’t you do the same?” REVIEW
1. Heads up, heels down, posture perfect: Ergonomics for an ophthalmologist. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5598171/ accessed 13 February 2018.





