The long-term medical manage-ment of open-angle glaucoma usually requires one or more medications. These are most commonly selected from five major groups of drugs that lower intraocular pressure: parasympathomimetics; sympathomimetics; carbonic anhydrase inhibitors; beta-adrenergic receptor blockers; and prostaglandin analogs. Unfortunately, all of these categories have potential ocular and/or systemic side effects, some more serious and likely to occur than others. In particular, early recognition of systemic effects is essential, both to prevent serious complications and to maximize patient compliance.
To help minimize toxicity, it's essential that we understand two things about each drug. First, we need to understand the drug's mechanism of action—its pharmacodynamics. This describes what the drug does when it reaches its site of action and how it ultimately achieves its desired effect. In the case of glaucoma drugs, this means how it affects aqueous humor production within the eye, and/or how it affects aqueous humor outflow from the eye.
Second, we need to understand the way the body reacts to the drug—i.e., absorption, distribution, biotransformation, excretion and so forth—its pharmacokinetics. These physiologic processes determine the amount of drug that must be delivered to the site of action, which in large part determines the concentration of the dispensed drug and the drug's dosing schedule.
The following is a brief summary of the pharmacodynamics and pharmacokinetics of the drugs in each of the five categories, including a discussion of how a clinician can prevent or minimize systemic side effects—and failing that, recognize problems early in their appearance in order to minimize any damaging impact. (The drug groups are considered in the order in which they were first used in the treatment of glaucoma.) I'll also offer some general strategies for maximizing effectiveness and minimizing complications when using medications to treat glaucoma.
Parasympathomimetics
This class of drugs, which includes pilocarpine, carbachol, physostigmine, demecarium, echothiophate and isoflurophosphate (isoflurophate), lowers IOP by increasing outflow through the trabecular meshwork. These drugs can be divided into two sub-categories: direct-acting and indirect-acting. The direct-acting members substitute their molecules for endogenous acetylcholine; the latter group act by interfering with the enzymatic metabolism of endogenous acetylcholine, which causes an increase in the amount of acetylcholine at receptor sites. (The latter drugs are often referred to as cholinesterase inhibitors.) Of the six drugs in this group, pilocarpine is direct-acting; the others are indirect-acting, except for carbachol, which acts in both ways and so can be considered to be both direct- and indirect-acting.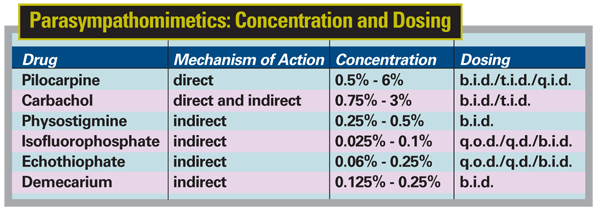
Parasympathomimetics can produce serious systemic effects in some patients; generally, the more beneficial the effect they are having, the more their toxicity also increases. The nature and extent of their side effects is partly a function of whether the specific drug in question acts directly or indirectly. It's helpful to think of them as covering a gradual scale from less effective and less toxic to more effective but potentially more toxic:
• Pilocarpine is less likely than the others to produce unwanted side effects because it's direct-acting; it's considered a safe drug.
• Carbachol and physostigmine have been studied less; they are more effective than pilocarpine, but also have a greater likelihood of toxicity.
• Isoflurophate and echothiophate are indirect-acting, irreversible cholinesterase inhibitors. They are most potent in terms of effect, but also have the greatest potential for systemic toxicity.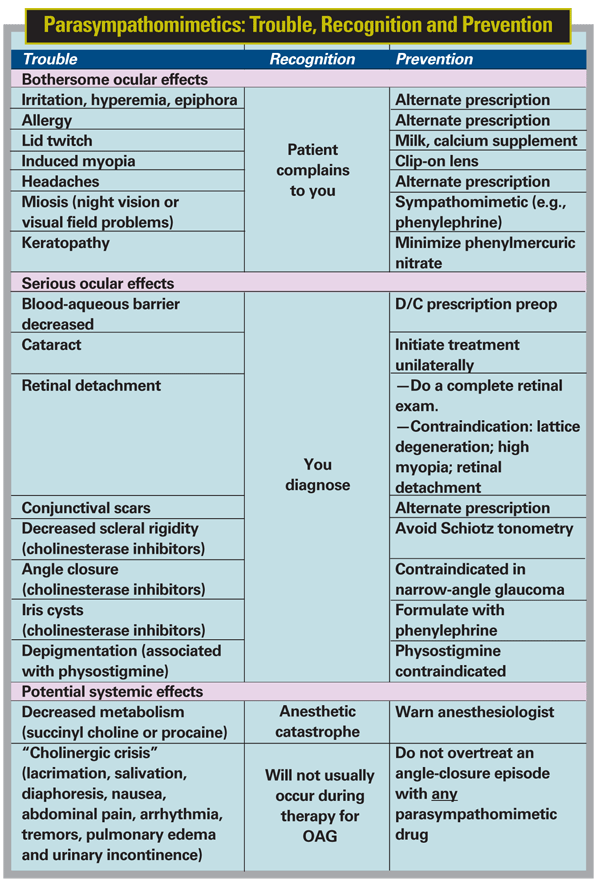
In general, parasympathomimetics should be avoided before surgery, as well as in patients with narrow-angle glaucoma or cataracts, or in those who are at risk for retinal detachment (i.e., patients with high myopia, lattice degeneration or a history of retinal detachment).
Sympathomimetics
This class of drugs increases outflow of aqueous humor from the eye and/or decreases inflow. Drugs in this class include epinephrine, dipivefrin HCl (DPE, Propine), apraclonidine (Iopidine) and brimonidine (Alphagan). The first two increase outflow by affecting beta receptors, and may decrease inflow (alpha receptor) after chronic treatment. The latter two decrease inflow by acting more specifically as alpha-2 receptor agonists. However, they share alpha-1 receptor activity to some extent, as is demonstrated by eyelid retraction, pupil mydriasis and conjunctival vasoconstriction.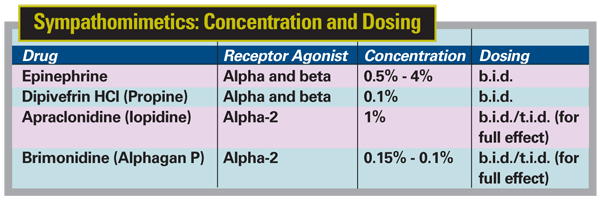
Although epinephrine is considered relatively safe, its beta-receptor activity predisposes it to causing systemic cardiovascular effects. The prodrug dipivefrin (an epinephrine molecule esterified) is considered safer for sensitive patients because of its decreased concentration. These sensitive patients include those with hypertension, cardiac arrhythmias, diabetes and hyperthyroidism, as well as patients taking systemic monoamine oxidase inhibitors and tricyclic antidepressants.
Apraclonidine and brimonidine are the most recent additions to this group of drugs. Common side effects associated with these drugs include dryness in the mouth and occasional insomnia or drowsiness. The most common bothersome reaction to them—which requires cessation of therapy—is the development of a local allergy or other toxic response. (Both apraclonidine and brimonidine are contraindicated in infants because they can cause severe respiratory depression.) Systemically, these drugs tend to raise blood pressure.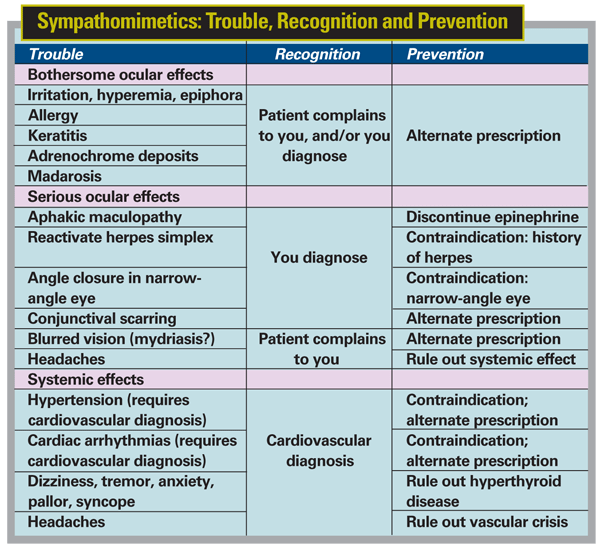
In general, this class of glaucoma medications should be used with caution in patients with a history of hypertension, advanced arteriosclerosis, aneurysms, cardiac disease, hyperthyroidism, diabetes or narrow-angle glaucoma.
Carbonic Anhydrase Inhibitors
This category is the only one that includes drugs that can be taken systemically; all of these are sulfonamide derivatives. Topical drugs in this category include dorzolamide (Trusopt) and brinzolamide (Azopt); systemic drugs include acetazolamide (Diamox), methazolamide (Neptazane), dichlorphenamide (Daranide) and ethoxzolamide (Cardrase).
The list of possible systemic side effects sometimes associated with CAIs is quite long (see chart, below). Some are unavoidable but transient; those include paresthesias, urinary frequency and nocturia. CAIs may also cause gastrointestinal tract problems such as nausea, anorexia, dyspepsia, cramps, diarrhea or constipation (as well as a metallic taste). If the patient reports these symptoms, you can try decreasing the dosage, or change the way the patient is taking it—such as having the patient take it with meals to mitigate problematic effects.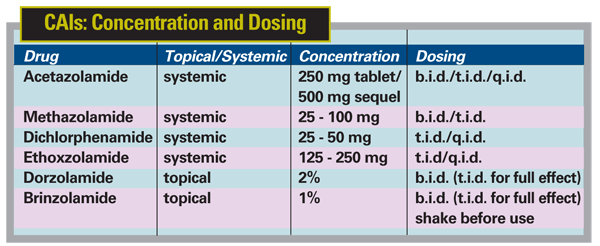
Generally, the systemic drugs in this category are considered more likely to cause side effects than the topically applied agents in the group. Of the systemics, acetazolamide has been most widely used, but some evidence suggests that methazolamide may be equally effective and somewhat less toxic in some patients. Dichlorphenamide and ethoxzolamide are prescribed less often.
Note: Although topical dorzolamide and brinzolamide are safer than the systemic CAIs, the trade-off is that they're also less effective.
In general this class of drugs should be avoided if the patient:
• has a history of reacting to sulfonamides;
• has a history of renal stones or blood problems;
• is pregnant (be on the lookout for early pregnancy in a patient, which may not be obvious);
• has a history of severe skin problems;
• has kidney or liver disease;
• is under long-term treatment for angle-closure glaucoma; or
• has borderline acid/base status (for example, diabetics, alcoholics and dehydrated patients).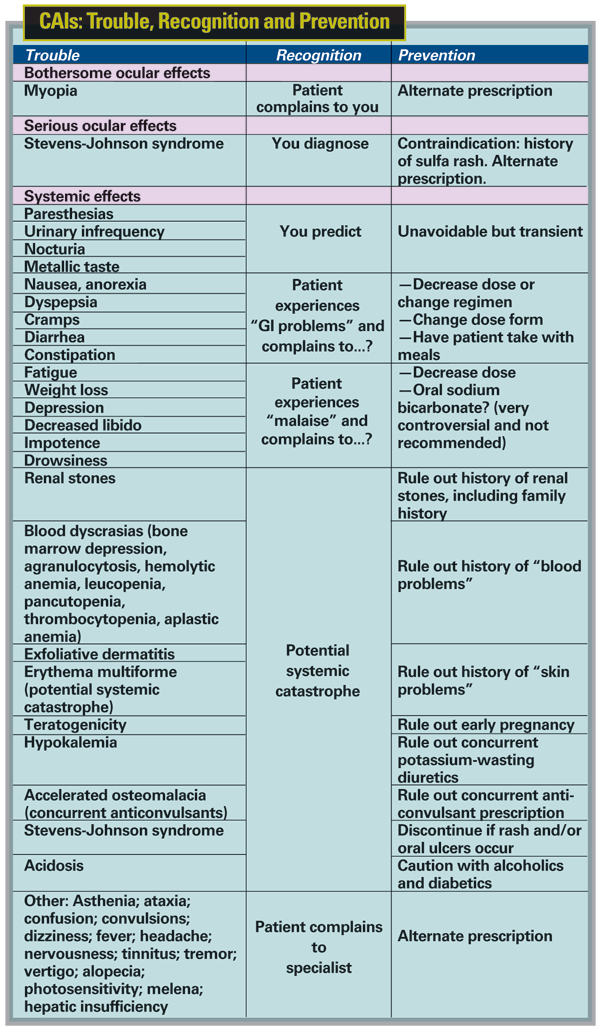
It's also important to avoid drug interactions, particularly with thiazides and anticonvulsants.
Sympatholytics (Beta-Blockers)
These drugs act by decreasing aqueous humor production. Drugs in this group include timolol, levobunolol, metipranolol, carteolol, and betaxolol.
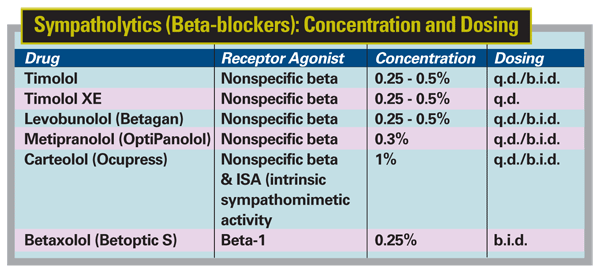
When they first appeared, it was reported that beta-blockers had few systemic side effects. However, long-term use has revealed many potential adverse reactions, including ocular problems and potentially serious pulmonary and cardiac problems. (See chart, below.) Of the six members of this group, betaxolol is least likely to cause pulmonary and cardiac problems due to its relatively specific beta-1 activity. However, betaxolol is also less effective than the nonspecific beta-blockers.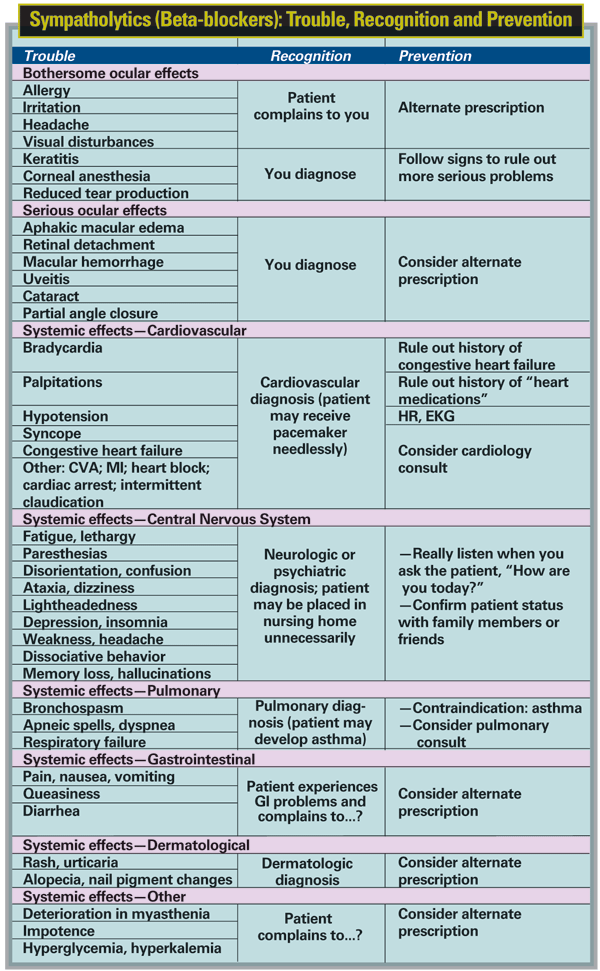
Note that this class of drugs should be avoided in patients with asthma. These drugs can also trigger serious drug interactions with other drugs, notably MAOIs.
Prostaglandin Analogs
This category of drugs, the newest group of glaucoma treatment options, includes latanoprost (Xalatan), bimatoprost (Lumigan), unoprostone isopropyl (Rescula) and travoprost (Travatan). This category of drugs works by increasing uveoscleral and conventional outflow of aqueous humor. These tend to have few systemic side effects, although they can trigger or aggravate migraine headaches.
Strategies for Avoiding Trouble
A quick look at the lists of side effects makes it clear that the most recently introduced IOP-lowering glaucoma medications have, in general, less systemic toxicity than the older agents. Nevertheless, the older drugs are less expensive and continue to be very effective as a means to lower IOP. Furthermore, they can be used safely if the noted precautions are followed.
The following strategies are also very helpful for minimizing side-effect problems—especially systemic side effects:
• Close eyes for five minutes after eye drop instillation. Instruct your patients to close their eyes for five minutes after instilling any drops. Simply doing this (or using punctal occlusion for five minutes) increases ocular absorption by 70 percent and decreases systemic absorption by 70 percent. This provides the most favorable therapeutic index for the patient. In fact, you should make this part of the instructions on the bottle. For example, "One drop in each eye once a day, followed by five minutes of eyelid closure."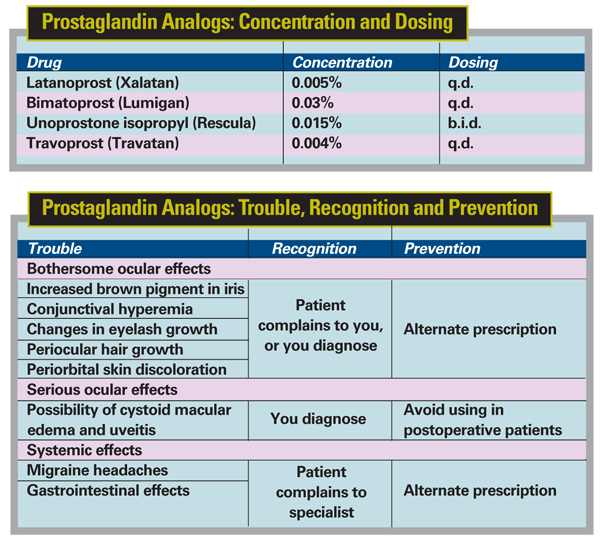
• Don't use systemic options if topical therapy is effective. Clearly, starting treatment with a topical option is key to reducing the likelihood of systemic side effects.
• Keep "defective" products in your possession. Have your patients bring in their medicine bottles. If the patient has a product that looks contaminated, or the solution is discolored, or the bottle appears to have been tampered with, confiscate the bottle and keep it in your possession; give the patient a prescription to replace it. This is a good strategy for medico-legal reasons; if a lawsuit should occur later, you'll have the relevant evidence in your own hands.
• Don't hesitate to use consultants. If a patient has cardiovascular or gastrointestinal problems, or if you're going to start a beta blocker, don't be afraid to ask for a cardiology or gastrointestinal consult first. In fact, if you're having problems achieving your goals with any glaucoma patient, referring to a colleague who specializes in glaucoma isn't a bad idea.
• Be familiar with the information in drug package inserts. However, don't limit your knowledge to that one source.
• Don't allow "refill alterations" on your prescriptions. Don't get in the habit of modifying your prescriptions after the fact. You don't ever want to be in a court of law and have someone say, "Dr. Jones is always changing his prescription after he writes it." You want to be able to say, "When I write a prescription, I write it exactly the way it's supposed to be."
• Arrange frequent follow-up appointments. If you don't, patients may get the impression that you're not interested in them—and you can miss developments such as unforeseen drug complications. It only takes a moment to look at an eye, check a pressure and check for toxicity. I often don't even bill patients for a quick follow-up visit; I just make sure they come in.
• Communicate with the patient. Explain why the patient is using the drug, how it's helping his eyes and how to use it. And don't forget to include "five minutes of eyelid closure after drop instillation" in your instructions.
• Provide careful and complete documentation regarding all medications in the chart. This is important because many medications interact. If the patient has an untoward or poor response to your prescription, it's a tremendous advantage to have a complete grasp of all of his medications. This should be part of every chart.
Dr. Flach is professor of ophthalmology and director of the Evening Ophthalmology Outpatient Unit at the
This article is based upon the popular course taught by Dr. Flach at the annual meeting of the




