Presentation
An 80-year-old Caucasian female with a six-week history of gradual-onset blurred vision in her right eye presented to the Wills Emergency Room for evaluation. The patient reported that over a six-week period she had noticed progressive, painless loss of the entire visual field in her right eye.
Medical History
Her past ocular history included cataract surgeries in 2000 and 2006 and a YAG capsulotomy in the right eye in 2012. Her past medical and surgical history was remarkable for type 2 diabetes, hypertension and a right total knee replacement. Her social history was significant for social alcohol consumption. Current medications included: simvastatin; metformin; pioglitazone; losartan; and liraglutide.
Examination
Ocular examination demonstrated best-corrected visual acuities of 20/40 OD and 20/25 OS. Pupils and confrontation visual fields were normal. Intraocular pressures were 14 and 13 mmHg OD and OS, respectively. Extraocular motility was full bilaterally. The anterior segment examination revealed posterior chamber intraocular lenses bilaterally with an open posterior capsule in the right eye and early posterior capsular opacification in the left eye.
Dilated fundus examination of the right eye demonstrated trace vitreous cell, disc edema with a chalky white appearance, surrounding retinal whitening, peripapillary edema and streak peripapillary retinal hemorrhages (Figure 1). The macula, vessels and periphery appeared normal. The left eye had a normal optic disc, macula, vessels and periphery.
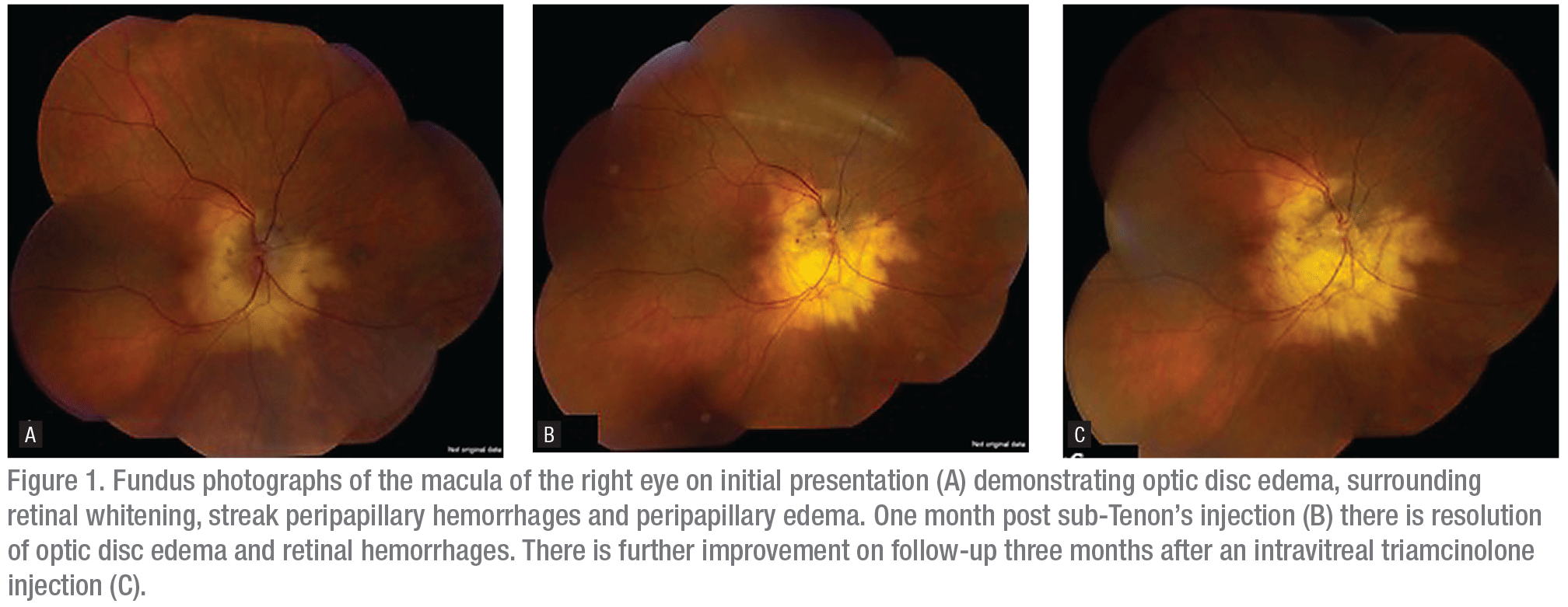 |
What is your diagnosis? What further workup would you pursue?
Please click this link for diagnosis, workup, treatment and discussion.



