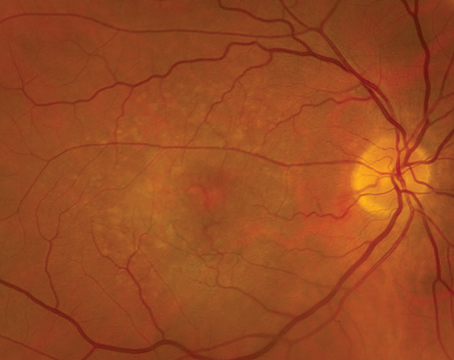
Diabetic retinopathy and diabetic macular edema are leading causes of blindness in the working-age population of most developed countries.1 Intravitreal anti-vascular endothelial growth factor agents have become first-line therapy in DME patients, as several recent clinical trials suggest that these therapies are more effective than laser photocoagulation for diabetic macular edema.2-6 These medications bind vascular endothelial growth factor, thereby decreasing angiogenesis and vascular permeability, and causing regression of diabetic neovascularization and reduction in DME, respectively.
An area of great interest is the role for these agents to limit, and even reverse, the progression of DR, as ranibizumab has recently been approved by the Food and Drug Administration for the treatment of DR. Panretinal laser photocoagulation, the current standard treatment for proliferative diabetic retinopathy, is destructive and causes constriction of visual fields, nyctalopia and decreased contrast sensitivity. Instead of waiting for nonproliferative diabetic retinopathy to progress into PDR before performing destructive PRP, treating DR earlier with anti-VEGF therapy to prevent the development of PDR is more desirable. Furthermore, limiting progression of DR may also prevent the development of DME. Consequently, the treatment of DR will likely undergo radical transformation, similar to the treatment of DME over the past several years. This article will review anti-VEGF agents for the treatment of DR.
The Role of Anti-VEGF Agents
VEGF plays a key role not only in vascular permeability, but also in angiogenesis. There are at least nine different VEGF isoforms due to the alternative splicing and include VEGF-A, PlGF (placental growth factor), VEGF-B, VEGF-C, VEGF-D and VEGF-E.7 The actions of VEGF family members are mediated by the activation of tyrosine kinase receptors.7 The VEGF receptors have seven immunoglobulin-like loops in their extracellular domain and a kinase insert region in the intracellular domain. VEGF receptors can signal via the mitogen-activating protein kinase (MAPK) signaling pathway or through elevation in intracellular calcium concentration in endothelial cells forming the vessel walls. VEGF-A is a critical regulator of ocular angiogenesis and vascular permeability. VEGF-A acts at VEGF receptors (VEGFR) 1 and 2. VEGFR1 (fms-like tyrosine kinase-1) has both positive and negative angiogenic effects; VEGFR2 (fetal liver kinase-1 and kinase insert domain-containing receptor) is the primary mediator of the mitogenic, angiogenic and vascular permeability effects of VEGF-A.8 VEGF mediates angiogenesis by promoting endothelial cell migration, proliferation and survival. Inhibition of VEGF represents a key strategy in the treatment of both DR and DME.
Ranibizumab in DR
Ranibizumab is an antibody fragment without the Fc portion and affinity-matured to more strongly bind VEGF-A. In 2012, ranibizumab was approved by the FDA for DME, based on data from Genentech’s Phase III trials, RIDE and RISE.9,10 These two identically-designed, parallel, double-masked, three-year clinical trials were sham-treatment controlled for 24 months. A total of 759 patients were randomized into three groups to receive monthly treatment with 0.3-mg ranibizumab (n=250), 0.5-mg ranibizumab (n=252) or sham injection (control group, n=257). Beginning at three months, macular laser rescue treatment was made available to all patients, if needed, based on pre-specified criteria. Panretinal laser photocoagulation treatment was available to all patients as clinically indicated. After month 24, patients in the sham injection group were eligible to receive monthly injections of 0.5 mg ranibizumab and all patients were followed and dosed monthly for a total of 36 months.
Compared to controls, a significantly greater percentage of ranibizumab-treated eyes gained at least three additional lines (15 letters) of visual acuity at 24 months: RIDE: 34 percent in the 0.3-mg group versus 12 percent in the control group; RISE: 45 percent in the 0.3-mg group versus 18 percent in the control (primary endpoint). A preplanned subgroup analysis indicated the improvements were generally similar for patients with well-controlled glucose (baseline HbA1c ≤8) and poorly controlled glucose (baseline HbA1c >8). Additionally, in both studies, significantly more eyes that received ranibizumab compared with sham injections achieved vision greater than or equal to 20/40, experienced decreased central foveal thickness on OCT, and reported greater improvements in their ability to perform vision-related daily activities such as reading and driving, compared to the sham group, based on composite responses to the National Eye Institute Visual Functioning Questionnaire-25.
Moreover, in the RIDE and RISE trials, eyes that received ranibizumab were less likely to progress to more advanced (proliferative) diabetic retinopathy.11 In these trials, study eyes had a baseline ETDRS diabetic retinopathy severity scale ranging from 10 to 75. At month 24, an exploratory analysis demonstrated a higher proportion of eyes treated with ranibizumab had a three-step or more improvement of their disease as determined by color fundus photography when compared to sham. In the third year of the studies, as noted above, patients in the control group had the option to cross over to receive monthly treatment with 0.5-mg ranibizumab, whereas patients originally randomized to 0.3-mg or 0.5-mg ranibizumab continued to receive their assigned dose and were followed for 12 additional months. The benefits of ranibizumab treatment achieved at month 24 were maintained through month 36.
One recent report further assessing this issue in RIDE and RISE showed that ranibizumab slows progression of retinal nonperfusion in patients with diabetic macular edema.12 The percentage of eyes that showed an increase in posterior retinal nonperfusion from baseline increased over time at a statistically significant faster rate in the sham group compared to the ranibizumab-treated group. The authors concluded that monthly injections of ranibizumab can slow, but not completely prevent, retinal capillary closure in patients with DME. Nevertheless, it appears that ranibizumab can modify the pathophysiology of DR. On February 6, 2015, the Food and Drug Administration approved ranibizumab for the treatment of diabetic retinopathy in patients with DME.
Aflibercept in DR
In 2014, aflibercept was approved for the treatment of DME. Aflibercept is a fusion protein that inhibits both VEGF-A and placental growth factor (PLGF), another growth factor involved in angiogenesis. Regeneron’s Phase III VISTA-DME and VIVID-DME studies of 862 patients compared aflibercept 2 mg given monthly, aflibercept 2 mg given every two months (after five initial monthly injections), or macular laser photocoagulation (at baseline and then as needed).13 The corresponding proportions of eyes gaining at least three lines (15 letters) of visual acuity were 41.6 percent and 31.1 percent versus 7.8 percent (p<0.0001) in VISTA, and 32.4 percent and 33.3 percent versus 9.1 percent (p<0.0001) in VIVID. Additionally, in both studies, there was a statically significantly improvement in mean visual acuity in the aflibercept-treated patients, as well as decreased central foveal thickness on OCT. The FDA-approved dosing for aflibercept for the treatment of DME is 2 mg every two months following five initial monthly injections. It also may be dosed once per month, but additional benefit was not seen with this dosing plan.
With regard to DR, the VIVID-DME and VISTA-DME trials included a pre-specified secondary endpoint evaluating diabetic retinopathy based on the ETDRS DR severity scale. In these trials, a larger proportion of the aflibercept-treated patients achieved a two-step or greater improvement on the ETDRS diabetic retinopathy severity scale at two years. In the VIVID-DME trial, 29 percent of evaluable eyes in the 2q4 group (monthly) and 33 percent of evaluable eyes in the 2q8 group (every two months, after five initial monthly injections) treated with aflibercept experienced at least a two-step improvement, compared to 8 percent of eyes in the laser control group (p<0.001). In the VISTA-DME, 40 percent of evaluable eyes in both the 2q4 and 2q8 groups treated with aflibercept experienced at least a two-step improvement, compared to 17 percent of eyes in the laser control group (p<0.0001). On December 1, 2014, the FDA accepted for priority review the supplemental Biologics License Application for aflibercept for this indication.
The Future Landscape for DR
The approval of ranibizumab for the treatment of DR signals the beginning of a paradigm shift in the management of DR. It should be noted that the RIDE and RISE trials, as well as the VIVID and VISTA trials, showed efficacy of anti-VEGF therapy for DR based on a population of patients with DME, not a population presenting with DR in the absence of DME. However, it is expected that these results are translatable to a population of DR patients without DME, and it is quite likely that registration trials assessing anti-VEGF agents in this setting will commence soon.
The treatment of DR with anti-VEGF agents will also be studied by the National Institutes of Health-sponsored Diabetic Retinopathy Clinical Research Network Protocol S, designed as a randomized Phase III trial, which will compare prompt PRP to ranibizumab with deferred PRP for patients with PDR. As noted above, PRP is destructive and can cause constriction of visual fields, nyctalopia and decreased contrast sensitivity. Treating DR with an anti-VEGF agent prior to the development of PDR has the potential, therefore, to be far less destructive. Furthermore, limiting progression of DR may also prevent the development of DME in the first place.
The future for DR treatment may look quite similar to the current DME treatment landscape. Unless DRCR Protocol S shows a dramatic difference in efficacy between PRP and ranibizumab, physicians will likely select from a variety of treatments, including PRP, ranibizumab, aflibercept and off-label bevacibumab, depending on patient presentation and insurance coverage. Bevacizumab, a monoclonal antibody that binds VEGF, is used off-label for the treatment of DME and DR, but there is limited randomized prospective data assessing its efficacy in limiting DR progression. In addition, it is currently unknown which anti-VEGF agent will provide the best response in DR, as comparative treatments for DME are now just yielding results. For example, aflibercept was compared to ranibizumab and bevacibumab for the treatment of DME in DRCR Protocol T.14 In this study, 660 patients were randomized to receive either aflibercept 2 mg, bevacizumab 1.25 mg or ranibizumab 0.3 mg, dosed according to a protocol-specified algorithm. Patients were treated with focal/grid laser at or after the 24-week visit based on OCT and visual acuity parameters. In the study, aflibercept demonstrated a significantly greater improvement in mean change in BCVA from baseline at 52 weeks compared to both bevacizumab and ranibizumab injection in the subgroup of patients with worse baseline visual acuity (20/50 or worse), but there was no difference in visual outcomes in those patients with better baseline visual acuity (20/32 to 20/40).
The proper dosing regimens for anti-VEGF agents in DR are also unknown. It is unclear if the best dosing regimens involve fixed-interval-dosing or treat-as-needed or treat-and-extend, regimens that are more familiar in the treatment of exudative age-related macular degeneration. PRP might be preferred in those patients who have limited access to care or those patients who are unable to return frequently for assessment and intermittent injection. Furthermore, combination therapy of PRP and anti-VEGF agents may be used for severe cases.
Although many questions remain unanswered, the adoption of anti-VEGF therapies for DR treatment will dramatically alter the delivery of care to these patients, just as the adoption of anti-VEGF agents has changed the landscape for DME treatment. The ophthalmic community eagerly awaits additional controlled data to guide treatment of DR. REVIEW
Dr. Ciulla is on the Retina Service at Midwest Eye Institute, 200 W. 103rd St. Indianapolis, IN 46290. Contact him at (317) 817-1822 or email thomasciulla@gmail.com.
1. Ciulla T, Amador A, Zinman B. Diabetic retinopathy and diabetic macular edema: Pathophysiology, screening, and novel therapies. Diabetes Care 2003;26(9):2653-64.
2. Diabetic Retinopathy Clinical Research Network, Elman M, Aiello L, Beck R, Bressler N, Bressler S, Sun J. Randomized trial evaluating ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema. Ophthalmology 2010;117:1064-1077 e35.
3. Diabetic Retinopathy Clinical Research Network, Elman M, Qin H, Aiello L, Beck R, Bressler N, Melia M. Intravitreal ranibizumab for diabetic macular edema with prompt versus deferred laser treatment: Three-year randomized trial results. Ophthalmology 2012;119:2312-8.
4. Do DV, Nguyen QD, Khwaja AA, Channa R, Sepah YJ, Sophie R, Hafiz G, Campochiaro PA; READ-2 Study Group. Ranibizumab for edema of the macula in diabetes study: 3-year outcomes and the need for prolonged frequent treatment. JAMA Ophthalmol 2013;131:139-45.
5. Elman MJ, Ayala A, Bressler N, Browning D, et al. Intravitreal Ranibizumab for Diabetic Macular Edema with Prompt versus Deferred Laser Treatment: 5-Year Randomized Trial Results. Ophthalmology 2015;122:375-81. doi: 10.1016/j.ophtha.2014.08.047. Epub 2014 Oct 28.
6. Nguyen QD, Shah SM, Khwaja AA, Channa R, et al. Two-year outcomes of the ranibizumab for edema of the mAcula in diabetes (READ-2) study. Ophthalmology 2010;117:2146-51.
7. Takahashi H, Shibuya M. The vascular endothelial growth factor (VEGF)/VEGF receptor system and its role under physiological and pathological conditions. Clin Sci (Lond) 2005;109(3):227-41.
8. Ferrara N, Gerber H, LeCouter J. The biology of VEGF and its receptors. Nat Med 2003;9(6):669-76.
9. Brown D, Nguyen Q, Marcus D, Boyer D, et al. Long-term outcomes of ranibizumab therapy for diabetic macular edema: The 36-month results from two phase III trials: RISE and RIDE. Ophthalmology 2013;120:2013-22.
10. Nguyen Q, Brown DM, Marcus DM, Boyer DS, et al. Ranibizumab for diabetic macular edema: Results from 2 phase III randomized trials: RISE and RIDE. Ophthalmology 2012;119:789-801.
11. Ip M, Domalpally A, Hopkins J, Wong P, Ehrlich J. Long-term effects of ranibizumab on diabetic retinopathy severity and progression. Arch Ophthalmol 2012;130:1145-52.
12. Campochiaro P, Wykoff C, Shapiro H, Rubio R, Ehrlich J. Neutralization of vascular endothelial growth factor slows progression of retinal nonperfusion in patients with diabetic macular edema. Ophthalmology 2014;121:1783-9.
13. Korobelnik J, Do D, Schmidt-Erfurth U, Boyer D, et al. Intravitreal aflibercept for diabetic macular edema. Ophthalmology 2014;121:2247-54.
14. The Diabetic Retinopathy Clinical Research Network, Wells JA, Glassman AR, Ayala AR, Jampol LM, et al. Aflibercept, Bevacizumab, or Ranibizumab for Diabetic Macular Edema. N Engl J Med 2015 Mar 26;372(13):1193-203. doi: 10.1056/NEJMoa1414264. Epub 2015 Feb 18.