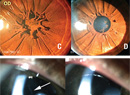
Definition & Characteristics
Cortical visual impairment is defined as bilateral visual impairment, involving acuity and/or higher visual functions, such as visual motor planning, due to posterior visual pathway disease. It is one component of a global neurologic process.
Patients with cortical visual impairment often display characteristic behaviors that may improve or resolve as the child improves. These characteristics include: light gazing; photophobia; poor visual attention; preferences for certain colors; visual field abnormalities; difficulty with visual complexity; problems with viewing distance; eccentric viewing; atypical visual reflex behaviors; and variability with contrast.2 These characteristics may resolve as a patient improves. A detailed history may reveal previously present characteristics.
Causes
|
These patients may have co-morbidities and associated deficits that make the identification, evaluation, treatment and rehabilitation of the patient more difficult. R. Michael Siatkowski, MD, and colleagues have shown that premature infants are particularly vulnerable to anterior and posterior visual pathway disease, which may complicate the identification of the cause of vision loss.5
Pathophysiology
Melvyn A. Goodale, PhD, and A. David Milner, PhD, described the two-stream hypothesis of neural processing in 1999. Information concerning recognition of objects travels from the occipital cortex to the inferior temporal cortex (ventral stream). Information concerning the location of objects and control of movements to locate objects in space travels from the occipital lobe to the parietal lobe (dorsal stream).6 Pathophysiology affecting the ventral stream may cause difficulty with object and facial recognition. Pathophysiology of the dorsal stream may cause difficulty locating objects and visual motor planning (visual guidance of movements).
Originally, it was thought that these two systems were separate entities; however, more recent research indicates that processing of complex visual information requires connections between the ventral and dorsal streams.7
Classroom learning is largely vision-based. Both ventral and dorsal stream pathology may hinder educational progress, unless accommodations and interventions are made. Activities of daily living are also highly dependent on vision. A child’s independence in routine activities may also be affected and require deficit- based compensation.
|
Classification and Prognosis
Christine Roman-Lantzy, PhD, has described a spectrum of phases that correlate with the severity of visual characteristics displayed by a patient with cortical visual impairment. Phase I is the lowest level of function, where a patient displays minimal visual responses. Phase II is a higher level where visual performance is linked to improved function. Phase III is the highest level of performance, where some typical characteristics may become extinct.8 Patients may progress from one phase to another with improvement in function. This type of classification provides a common language for families and the multidisciplinary team caring for a child. It is also the basis for providing interventions and accommodations that may be used to assist a patient with cortical visual impairment in the educational setting and with activities of daily living.
In the past, cortical visual impairment was called cortical “blindness,” with a perceived poor prognosis. Although some patients may not have any improvement, studies have shown that the majority of patients have at least some improvement in vision.9 It is important to communicate this fact to families when the diagnosis of cortical visual impairment is made.
It is important to educate families as well as other health-care providers who may treat children with cortical visual impairment in order to prevent inaccurately poor prognostic predictions. Baseline visual acuity at diagnosis cannot be used to predict final visual performance. The degree of damage demonstrated on brain imaging studies cannot be used to predict final visual performance either.
The Ophthalmologist’s Role
The ophthalmologist is an important member of the multidisciplinary team that cares for a child with cortical visual impairment.
During the history taking, it is important to solicit observations of visual performance from the family and other members of the child’s care team. A child’s performance in a limited examination time, in an unfamiliar place when he may be tired and hungry, may not be representative of true function. It is often the occupational or physical therapist who first notes a visual field defect in a patient.
|
It is vital for the ophthalmologist to make and document the diagnosis of cortical visual impairment, as well as reduced visual acuity, if present. Patients may qualify for services based on the level of visual impairment, especially if a patient has a chronic visual condition that will impair educational progress. Further assistance for interventions or accommodations that may help a patient reach his or her full potential depends on the diagnosis made by the ophthalmologist.
When appropriate, a referral for an evaluation for vision services from the appropriate agency should be made. The referral for infants and children prior to the third birthday can be made through their early intervention program or appropriate state agency, depending upon the patient’s state of residence. The referral for children age 3 and older is made through the school district or appropriate state agency.
The findings of the eye examination and diagnosis should be discussed with the family. Educational and resource materials should be provided. It is important to provide a list of websites with accurate information appropriate for the patient’s diagnosis, since many families primarily use the Internet for medical information. It is also helpful to have pre-printed information ready to give families whose child has a common diagnosis.
Specific recommendations for treatment, interventions and accommodations should be discussed with families, documented and given to families in writing as part of the discharge instructions.
Recommendations for interventions and accommodations should be based on the patient’s level of function and characteristics of impairment present. Suggestions for a low-functioning, 6-month-old, former preemie with periventricular leukomalacia and hypotonia in Phase I may include:
1. High-contrast, lighted and moving visual stimuli;
2. Avoid overstimulation;
3. Provide support for body when performing visual tasks;
4. Allow extra time for response to visual stimuli; and
5. Use auditory and tactile cues to attract and sustain visual attention.
Suggestions for a higher-functioning, school-age child with cerebral palsy in Phase III may include:
1. Allow extra time for response to visual stimuli because of processing and expressive delay;
2. Limit complexity and increase as tolerated;
3. Avoid graphite pencil on recycled paper;
4. Use black marker on white paper for written activities; and
5. Exploit auditory learning skills.
Children with a disability that interferes with educational progress who attend school accepting federal funds may qualify for an individualized educational plan, or IEP, under the Individuals with Disabilities Education Act (See idea.ed.gov.) It is important to document these needs and communicate appropriately with the family and other members of the child’s multidisciplinary team.
It is imperative for the ophthalmologist to be an active and involved member of the team caring for a child with cortical visual impairment. The ophthalmologist should provide diagnoses, referrals for services, treatment of ocular co-morbidities, education and advocacy for the patient. Interventions and accommodations allow the child with cortical visual impairment to attain his or her fullest educational potential and maximize independence in activities of daily living. REVIEW
Dr. Lehman is the chief of ophthalmology at Nemours/AI duPont Hospital for Children, Wilmington, and a clinical professor of ophthalmology and pediatrics at Jefferson Medical College/Wills Eye Institute, Philadelphia.
1. Good WV, Jan JE, de Sa L, Barkovich AJ, Groenveld M, Hoyt CS. Cortical visual impairment in children. Surv Ophthalmol 1999;38:351-364.
2. Roman C, Baker-Nobles L, Dutton GN, et al. Statement on cortical visual impairment. JVIB 2010;104:69-72.
3. Khetpal V, Donahue SP. Cortical visual impairment: Etiology, associated findings, and prognosis in a tertiary care setting. J AAPOS 2007;11(3):235-239.
4. Soul J, Matsuba C. Visual Impairment in Children Due to Damage to the Brain. In: Dutton GN, Bax M, eds. Causes of damage to the visual brain. London, England: Mac Keith Press; 2010:20-26.
5. Siatkowski R, Good W, Summers C, Quinn G, Tung B. Clinical characteristics of children with severe visual impairment but favorable retinal structural outcomes from the Early Treatment for Retinopathy of Prematurity (ETROP) study. J AAPOS 2013; 17(2): 129-134.
6. Goodale MA, Milner AD. Separate visual pathways for perception and action. Trends Neurosci 1992 Jan;15(1):20-5.
7. Wang J, Zhou T, Qiu M, Du A, et al. Relationship between Ventral Stream for Object Vision and Dorsal Stream for Spatial Vision: An fMRI+ERP Study. Human Brain Mapping 1999;8(4):170-181.
8. Roman-Lantzy C. Cortical visual impairment: An approach to assessment and intervention. New York: AFB Press; 2007.
9. Huo, Richard, Susan K. Burden, Creig S. Hoyt, and William V. Good. Chronic cortical visual impairment in children: Aetiology, prognosis, and associated neurological deficits. Brit J Ophthalmol 1999;83:670-675.