
Presentation
A 58-year-old man with a past ocular history significant for LASIK performed on both eyes in 2000 with multiple subsequent enhancements (last in 2002) presented to his local ophthalmologist with a chief complaint of pain and redness of the left eye for approximately one week. The patient was treated with topical tobramycin/dexamethasone four times daily OS, giving modest improvement in his symptoms. Upon discontinuation of the drop, his symptoms returned with a higher degree of severity. Topical moxifloxacin was then initiated in the left eye, and the patient was referred to the Wills Eye Cornea service for consultation. The patient denied contact lens wear.
Medical History
The patient had a past medical history of osteoarthritis. Additional past ocular history included ocular rosacea. He denied use of systemic medications. His family and social history and review of systems were noncontributory.
Examination
On examination at the Wills Eye Cornea Service, the uncorrected visual acuity was 20/25+ OD and hand motion OS. His pupils were round, equal, briskly reactive and without a relative afferent pupillary defect. Extraocular motility and confrontational visual fields were full OU. Intraocular pressures were 11 mmHg OU. Examination of the lids revealed mild blepharitis OU. LASIK scars were visible OU. The patient's right cornea was clear centrally but was found to have multiple nests of epithelial ingrowth at the interface. Examination of the left cornea revealed stromal edema with a 2.5 x 3.0 mm paracentral infiltrate and an overlying 6.0 x 7.0 mm epithelial defect. An area of interface haze at 1 o'clock was additionally noted. Exam of the anterior chamber showed a hypopyon OS (See Figure 1). Fundus exam was within normal limits OU, though somewhat limited OS secondary to the corneal process.
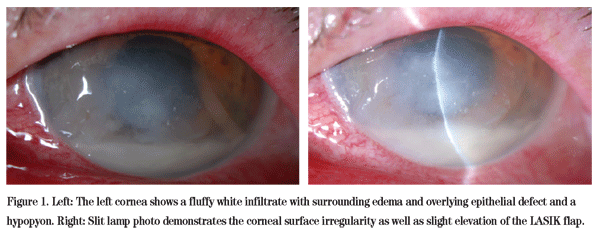
Diagnosis and Workup and Treatment
Based on the clinical exam, the patient was thought to have an infectious ulcer located in the LASIK flap/cornea interface. The flap was lifted, scraped and irrigated with gatifloxacin in the clinic. Bacterial, fungal and acid fast bacilli cultures were obtained, and the patient was admitted to the hospital for close observation and hourly topical antibiotic administration. He was started on topical fortified cefazolin, fortified tobramycin, gatifloxacin, atropine and oral moxifloxacin. After one day of hospitalization the patient appeared to worsen clinically. The LASIK flap of the left cornea showed significant keratolysis and was surgically amputated to debride infected tissue and allow better penetration of antibiotics. Bacterial cultures were positive for the gram negative rod Serratia marcescens. After susceptibilities were obtained, the patient's antibiotic regimen was changed to fortified amikacin, fortified tobramycin, ciprofloxacin ointment, and oral ciprofloxacin.
The patient began to show improvement on the new antibiotics (See Figure 2a) and was discharged from the hospital on day five after admission. Approximately two weeks after initial presentation, the antibiotics were tapered and a topical steroid was added. The patient's vision was 20/200, pinhole to 20/50+1, at his last follow-up visit seven weeks after his initial presentation, and he was fitted with a gas permeable contact lens. Best corrected visual acuity with the lens was 20/30. A slow taper of loteprednol was continued to try to minimize corneal stromal scar formation (See Figure 2b).
Discussion
Serratia marcescens is a motile, facultatively anaerobic gram-negative rod of the Enterobacteriaceae family, which also includes Escherichia coli and Salmonella. Serratia is well known for its production of a reddish-orange pigment called prodigiosin. This organism's virulence in the cornea stems in part from its production of proteases and bacterial endotoxins that cause liquefactive necrosis in rabbit corneas by destruction of proteoglycan ground substances. In addition, these factors increase vascular permeability resulting in corneal edema. Serratia is capable of causing lacrimal duct infections, keratitis, conjunctivitis and endophthalmitis. Ocular infections are often associated with contact lens wear, especially rigid gas permeable lenses, use of contaminated topical medications, and previous ocular surgery. Systemic conditions associated with Serratia infection include diabetes, rheumatoid arthritis, renal failure and alcoholism. This patient did not have any known risk factors except for history of LASIK with multiple revisions, the last of which was several years before presentation.
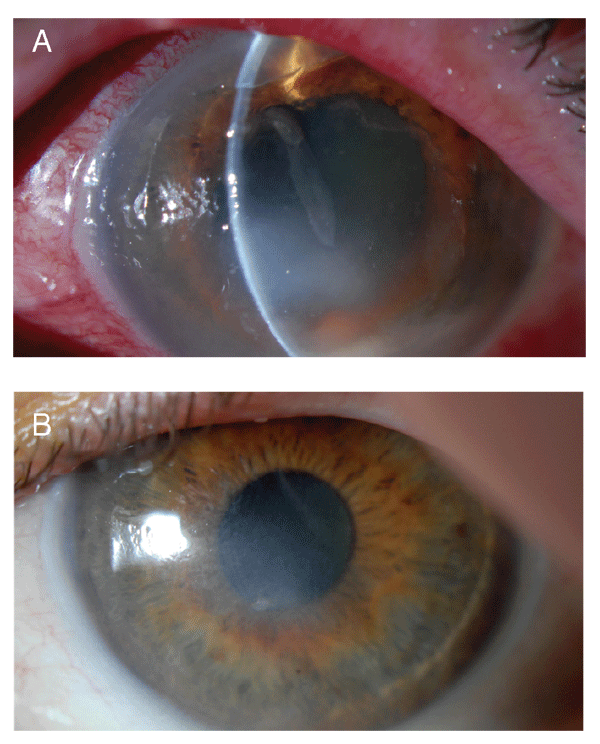
Figure 2. The left cornea (a) shows decreased size of the infiltrate and resolving hypopyon after appropriate antibiotic therapy. Note the "step-off" of the slit beam at the top of the photo representing the anterior defect after LASIK flap amputation. (B) Loteprednol was continued to try to minimize corneal stromal scar formation.
There are very few cases in the literature describing LASIK flap infections caused by Serratia, and in these cases, the infection manifested itself within the first 24 hours after the procedure. Therefore our case was unusual in that the infection occurred so many years after the procedure. In general, bacterial keratitis following LASIK is a serious complication and is considered to have a relatively low incidence, ranging from 0.02 percent to 1.5 percent. Interface infections can be difficult to treat as antimicrobials may not penetrate effectively through the flap, similar to corneal abscesses. The most common causative organisms include gram-positive cocci such as Staphylococcus aureus, Streptococcus pneumoniae, and Streptococcus viridans. Cases involving Nocardia asteroides, fungus and atypical mycobacteria have also been described. In two reported cases (three eyes) post-LASIK bacterial keratitis caused by Serratia, the patients presented with a purulent keratoconjunctivitis without deep stromal infiltrates. The infections quickly progressed to flap ulceration and detachment despite treatment. In contrast to gram-positive bacterial keratitis which often cause severe scarring, those patients infected with Serratia were left with only trace to mild subepithelial corneal haze one year after the infection with a best corrected visual acuity ranging from 20/40 to 20/22 with irregular astigmatism.
Serratia is often multi-drug resistant, which can make treatment quite challenging. Aminoglycosides and amikacin have both shown consistent efficacy in vitro. Fluoroquinolones, third-generation cephalosporins, trimethoprim/sulfamethoxazole, tetracycline and synthetic penicillins show variable activity. Effective treatment of Serratia and other gram-negative protease-producing organisms should ideally aim to eliminate bacteria as well as neutralize pathogenic factors such as proteases and endotoxins. Experimental modalities of treatment described include chicken egg-white ovomacroglobulin, which is a broad-spectrum protease inhibitor. Also, active and passive immunization with purified protease preparations from Serratia could potentially prevent infections prior to exposure to live bacteria.
Dr. Ohsie would like to thank Brandon Ayres, MD, of the Cornea Service at Wills Eye Institute for his assistance with this case.
1. Chang MA, Jain S, Azar DT. Infections following laser in situ keratomileusis: an integration of the published literature. Survey of Ophthalmology 2004;49:269-280.
2. Karp CL, Tuli SS, Yoo SH, Vroman DT, et al. Infectious keratitis after LASIK. Ophthalmology 2003; 110:503-510.
3. Levartovsky S, Rosenwasser G, Goodman D. Bacterial keratitis after laser in situ keratomileusis. Ophthalmology 2001; 108:321-325.
4. Liu J, Kwon YH. Seton Infection: Serratia Marcescens: 57 y.o. WF with 1 day history of redness, swelling, and pain in her right eye. EyeRounds.org. 5 March 2005. http://webeye.ophth.uiowa. edu/eyeforum/cases/case34-setoninfection.htm. Accessed Oct. 16, 2007.
5. Muñoz G, Alió JL, Pérez-Santoja JJ, Artola A, Abad JL. Ulcerative keratitis caused by Serratia marcescens after laser in situ keratomileusis. J Cataract Refract Surg 2004;30:507-512.



