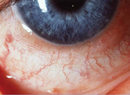
The use of diagnostic dyes represents one of the most efficient, objective, non-invasive, and directly visible means we have of identifying and tracking ocular-surface changes at the cellular level. Though they're particularly useful in dry-eye diagnosis and clinical trials, the utility of these dyes also extends far beyond dry eye to numerous other ocular surface conditions that affect corneal and conjunctival cells.
The three dyes with the highest visibility in the eye-care practitioner's office today are fluorescein, rose bengal and lissamine green. In this month's column, we'll explore each of these three dyes, looking at their merits and drawbacks, with a particular focus on lissamine green, an underappreciated tool.
Fluorescein
This yellow-colored dye was first used on the eye in 1882 when researchers discovered it could reveal corneal epithelial defects.1 Fluorescein is now used in various areas of ophthalmology, especially in retinal vasculature imaging and as a systemic marker in numerous pharmacokinetic studies. From the ocular-surface perspective, the water-soluble dye molecules diffuse into the intercellular spaces between living cells. The intensity of the stain is increased in areas of cellular degeneration or death, where the damage to cells, cell membranes and cell-to-cell junctions allow for the intracellular spaces to be more highly penetrated by the dye. This property makes the dye most useful for observing permeability in corneal epithelial and endothelial cells. However, in conjunctival staining it may become more difficult to make precise observations because of the dye's presence in both cells and intercellular spaces.2
Localization of the dye in this manner allows the practitioner to identify areas of desiccated or injured cells and areas where ocular-surface damage has occurred, such as epithelial defects and corneal abrasions.
Standardized grading of corneal and conjunctival fluorescein staining as well as measurement of tear-film breakup times, which have been made more clearly visible using fluorescein, have given this dye broad applicability as a dry-eye diagnostic test. It is particularly valuable as an assessment tool in clinical studies of dry eye. Research has indicated that fluorescein stains some types of healthy cells in vitro, though this typically is not visible except by using fluorescence microscopy.3
One challenge with the use of fluorescein staining is that the presence of the dye in the tear film may obscure readings of ocular-surface staining.4 A method developed at Ophthalmic Research Associates to circumvent this difficulty is to first assess tear-film related measurements (e.g., TFBUT) immediately upon instillation of micro-quantities of the dye while a portion of the dye is concentrated in the tear film. Once the dye diffuses from the tear film to the ocular surface, ocular-surface related measurements (e.g., corneal and conjunctival staining) can be evaluated. The portion of fluorescein that has penetrated to the ocular surface and localized in areas of cell damage will then become visible. Using controlled micro-quantities of fluorescein has been shown to greatly contribute to the repeatability and precision of such measures.5 The level of standardization achieved using this method has allowed TFBUT, fluorescein staining and, in some cases, fluorophotometry to become standards of evaluation for testing the efficacy of novel dry-eye therapies.
 |
Rose bengal, though useful in some situations, may have too many drawbacks to be the dye of choice in dry-eye diagnosis. Fluorescein is still an effective diagnostic dye for dry-eye management, but could yield to lissamine green in some situations. It may be time to give lissamine green a go, given its excellent safety profile and sensitivity in detecting the signs of dry eye. |
The use of a Wratten #12 yellow filter also enhances the visibility of fluorescein and is recommended when observing TFBUT and staining. In fluorophotometry, the instillation of a calculated amount of fluorescein onto the ocular surface allows measurement of tear volume immediately and over time in order to determine the tear turnover rate, a useful way to diagnose dry eye.
Rose Bengal
The second of these three dyes, rose bengal, is actually a derivative of fluorescein. Both dyes are hydroxyxanthines, though they differ structurally: Eight more halogens, four chlorines and four iodines are present on the rose-bengal molecule. Its instillation in the eye was first documented in 1914 and later popularized by Swedish physician Henrik Sjögren in the 1930s for diagnosing keratoconjunctivitis sicca; he noted a distinctive staining pattern following rose bengal instillation in the eyes of patients having the disorder.6 Since that time it's been used for the evaluation of numerous other ocular pathologies including herpetic corneal epithelial dendrites, superficial punctate keratitis, meibomian gland dysfunction and dysplastic or squamous metaplastic cells of conjunctival squamous neoplasms.3
Researchers have hypothesized that the differences in molecular structure between these two dyes confer the functional differences observed between the two molecules.3 However, our understanding of the functionality of rose bengal has shifted in recent years. Unlike fluorescein and lissamine green, it cannot be termed a "vital" dye. Rose bengal stains not only dead or dying cells as previously thought, but actually stains normal, healthy, living cells.3 How then do we explain its selective staining patterns in dry eye or Sjögren's syndrome?
Research on rose bengal has revealed that it's blocked from staining the ocular surface where molecules such as mucins, albumin or even an artificial tear compound such as carboxymethylcellulose are present. Thus, in areas where there are breaks in tear-film integrity or a dysfunction in the production of tear-film components, rose bengal can penetrate the ocular surface,7 where it stains by localizing primarily in cellular nuclei and, to a lesser degree, in other organelles.3 Tear-film components such as mucin protect the surface of the healthy eye, acting as a barrier against rose bengal, which would stain these cells if they were not effectively shielded from the dye molecule. Though fluorescein has also been observed to stain healthy, living cells as noted above, it does so to a much lesser degree and the functional use of fluorescein remains relatively unaffected by this property.
Rose bengal has also been discovered to have intrinsic cellular toxicity. Studies have shown that rose bengal has a dose-dependent, toxic effect on human corneal epithelial cells in vitro that is further enhanced by light exposure.3,8 This phototoxic effect may also explain rose bengal's toxicity toward bacteria and viruses. Thus, the use of rose bengal may complicate the diagnosis of disease that relies upon obtaining a viral culture from the ocular surface.9 (Chodosh J, et al. IOVS 1992;33:ARVO Abstract 2520)
Lastly, it's widely known that patient discomfort, particularly stinging upon instillation, which can become severe, is often a deterrent from using rose bengal.10,2,4 Rose bengal can be useful in certain circumstances, such as characterizing ocular surface damage that has resulted from lipid tear abnormalities secondary to meibomian gland dysfunction.11 However, don't overlook the other dyes. This is especially true if they offer equivalent, or superior, assessment of ocular-surface conditions while providing better patient comfort and prevention of further ocular-surface damage.
Lissamine Green
In this light, lissamine green may be considered the most underappreciated of the diagnostic dyes. Considering the list of shortcomings evident with the use of rose bengal, it's surprising that more practitioners haven't already turned to lissamine green as a standard diagnostic tool.
Lissamine green B has historically been known by a variety of names: wool green S; food green; acid green S; fast light green; pontacyl green S; cyanol green B; calcoid green S extra and pyronin G.2,12 This dye is a synthetically produced organic molecule containing two aminophenyl groups. It's classified as a phenyl methane dye, unlike both fluorescein and rose bengal, which fall into the category of xanthine dyes. Lissamine green has broad applicability as a dye, and is widely used as a non-ophthalmic drug, cosmetic and food additive.12,13,14 Lissamine green is also available for ophthalmic use as individually packaged, sterile strips.
Lissamine green preferentially stains membrane-damaged or devitalized cells,2 and, like rose bengal, localization of the dye to the cell nucleus has been noted.12 However, lissamine is unique in this group of three in that it has not been shown to stain healthy ocular surface cells. Evaluation of lissamine green staining in both rabbit and human corneal epithelial cells in vitro revealed that it doesn't stain healthy, proliferating cells and has a minimal effect on cell viability.15 (Chodosh J, et al. IOVS 1994;35: ARVO Abstract 1046)
The safety record of lissamine green is spotless to date, having no carcinogenic or cellular toxicity properties.16,17,18 Due to this lack of toxicity, the problem with rose bengal's killing viruses before a culture can be obtained isn't a concern. There is no stinging or discomfort such as that associated with rose bengal.
Visibility of color is one more point of differentiation: These dyes are often used in eyes that may be red. The green coloring of lissamine is visible with greater contrast on a red background, whereas the red/pink hue of rose bengal can be somewhat masked by a red eye.12
The safety and comfort profile of lissamine green clearly set a high standard, and several studies have also looked at its functionality.
In 1973 Dr. M.S. Norn of Denmark published a study on the use of lissamine green as a vital dye. His study examined lissamine in 171 eyes, in some cases instilling a combination of two (lissamine and rose bengal) or three dyes (fluorescein was added). In other eyes he instilled the dyes sequentially, with lissamine followed by rose bengal or vice versa. In his slit-lamp observations of the corneal and conjunctiva staining, Dr. Norn noted that whenever lissamine and rose bengal were instilled, either simultaneously or sequentially, the two dyes stained the same regions. In addition, he noted that for identifying pathological conditions, lissamine performed comparably to rose bengal.12
Subsequent study of the two dyes has shown they have similar sensitivity in detecting the signs of dry eye. In a study of 100 patients diagnosed with dry eye and 100 age- and gender-matched controls, researchers found that 89 percent of the dry-eye subjects exhibited rose bengal staining, and 87 percent exhibited lissamine green staining. No staining was observed for either dye in the control eyes.19
Another study compared the ocular staining properties and patient tolerance of rose bengal and lissamine green. Twenty subjects, 12 having KCS and eight control subjects having no ocular-surface disease, received a drop of one of the two dyes in both eyes at the first visit, and then received the other dye approximately one week later (order was determined randomly). Each subject graded ocular discomfort on a 0-5 scale immediately following dye instillation, and a study investigator graded corneal, nasal and temporal conjunctival staining on standardized 0-4 scales. Subjects also selected a preferred dye. Results showed that every subject preferred lissamine green, and their comfort scores on the standardized scale reflected this, with significantly greater discomfort demonstrated following instillation of rose bengal (KCS subjects: p=0.00006; non-KCS: p=0.01). No significant differences existed between the two dyes in corneal and conjunctival staining scores.10
In clinical trials using Ophthalmic Research Associates' Controlled Adverse Environment study model, researchers observed a greater change in ocular surface staining with lissamine green when compared to rose bengal post-CAE exposure, demonstrating this dye's sensitivity and ability to detect the effect of ambient conditions on the ocular surface. (Krenzer KL, et al. IOVS 2000;41:ARVO Abstract 928) Thus, lissamine green appears to be as effective and as specific as rose bengal.
These three dyes have historically comprised the diagnostic staining toolkit of the eye-care practitioner. It may not be time to eliminate any of them, but the current research clearly warrants an evaluation of how frequently and in which cases we reach for each dye. The two vital dyes, fluorescein and lissamine green, complement each other, with fluorescein staining between cells and achieving clearer staining of the cornea, and lissamine green staining the cells themselves and appearing particularly clearly on the conjunctiva. It's time, however, to rethink the necessity of using the potentially cytotoxic rose bengal when lissamine green could achieve equivalent staining with a lesser degree of patient discomfort. Though there may be situations in which use of rose bengal is warranted, simply reaching for rose bengal out of habit may not be best. So, the next time you need an ocular surface stain, stop and carefully consider your options.
Dr. Abelson, an associate clinical professor of ophthalmology at Harvard Medical School and senior clinical scientist at Schepens Eye Research Institute, consults in ophthalmic pharmaceuticals. Dr. Ingerman is an ophthalmologist with Johnson & Johnson Visioncare, where he is responsible for ophthalmic clinical research.
1. Pflüger. Zur Ernährung der cornea. Klin Monatsbl Augenheilkd 1882;20:69-81.
2. Kim J. The use of vital dyes in corneal disease. Current Opinion in Ophthalmology 2000;11:241-247.
3. Feenstra RPG, Tseng SCG. Comparison of fluorescein and Rose Bengal staining. Ophthalmology 1992;99:4:605-617.
4. Bron AJ, Evans VE, Smith JA. Grading of corneal and conjunctival staining in the context of other dry eye tests. Cornea 2003:22:7:604-650.
5. Abelson MB, Ousler GW, Nally LA, Emory TB. Dry Eye Syndromes: Diagnosis, clinical trials, and pharmaceutical treatment –'improving clinical trials.' Lacrimal Gland, Tear Film, and Dry Eye Syndromes 3. Ed. D. Sullivan et al., Kluwer Academic/Plenum Publishers 2002:1079-1086.
6. Sjögren H. Zur kenntnis der keratoconjunctivitis sicca. Acta Ophthalmol Suppl 1933:2.
7. Khan-Lim D, Berry M. Still confused about Rose Bengal? Current Eye Research 2004;29:4-5:31-317.
8. Feenstra RPG, Tseng SCG. What is actually stained by rose bengal. Acta Ophthalmologica 1992;110:7:984-93.
9. Roat MI, Romanoswki E, Araullo-Cruz T, Gordon J. The antiviral effects of Rose Bengal and fluorescein. Arch Ophthalmol 1987;105:1415-17.
10. Manning FJ, Wehrly SR, Foulks GN. Patient tolerance and ocular surface staining characteristics of lissamine green versus Rose Bengal. Ophthalmology 1995;102:12:1953-1957.
11. Lee S, Tseng SGC. Rose Bengal staining and cytologic characteristics associated with lipid tear deficiency. American Journal of Ophthalmology 1997;124:736-750.
12. Norn MS. Lissamine Green: vital staining of cornea and conjunctiva. ACTA Ophthalmologica 1973;51:483-491.
13. Randolph WF. FD&C Green No.3. Fed Register 1982;47:52140-52145.
14. Novitch M. D&C No.5: listing as a color additive in drugs and cosmetics; termination of stay and confirmation of effective date. Fed Regist 1982;47:49628-49632.
15. Kim J, Foulks GN. Evaluation of the effect of lissamine green and rose Bengal on human corneal epithelial cells. Cornea 1999;18:3:328-332.
16. Clode SA: Teratogenicity and empryotoxicity study of Green S in rats. Food Chem Toxicol 1987;25:995-997.
17. Moorhouse SR, Creasy DM, Gaunt IF. Three generation toxicity study of rats ingesting Green S in the diet. Food Chem Toxicol 1987;25:985-993.
18. Brantom PG, Creasy DM, Gaunt IF: Long-term toxicity study of Green S in mice. Food Chem Toxicol 1987;25:977-983.
19. Khurana AK, Chaudhary R, Ahluwalia BK, Gupta S. Tear film profile in dry eye. Acta Ophthalmol (Copenh) 1991;691:79-86.