Nasolacrimal Plumbing
The nose and eyes function as complementary sensory organs vital to exploring and understanding our physical world. Though sight and smell are two very different senses, the eye and nose are intimately connected by the nasolacrimal apparatus, the drainage system that carries tears from the ocular surface to the nose and ultimately to the gastrointestinal tract.
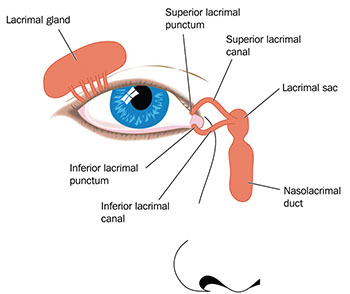 |
| The interconnected nature of the nasolacrimal system. Tears drain through the puncta and canaliculi, and ultimately flow down the throat. |
The lacrimal canaliculi are tube-like structures that run from the eye to the lacrimal sac. The ends of the canaliculi, the superior and inferior puncta, are found on the inside of the eyelids adjoining the medial canthus. In addition to spreading tears, blinking causes a transient opening of the lacrimal sac, creating a negative pressure that draws tears in to drain through the puncta and canaliculi. From the lacrimal sac, tears drain via the inferior turbinate and ultimately down the throat. It’s not uncommon for patients to associate some eye drop medications with a noticeable taste as the diluted drops travel this route.
The funnels of nasolacrimal drainage are the puncta. A number of conditions, including infections, congenital syndromes and the adverse effects of some drugs (such as the anti-neoplastic docetaxel) can cause punctal stenosis, leading to partial or complete occlusion of the drainage pathway.1,2 Punctal plugs are used to the same end for patients with dry-eye syndrome; by occluding drainage, the plugs increase the length of time tears remain on the ocular surface. Plugs have also become a popular vehicle for depot drug delivery, a topic covered in previous installments of Therapeutic Topics.
Deeper Connections
From the canaliculi, tears drain into the lacrimal sac and then the nasolacrimal duct, emptying into the nasal cavity. This explains why the nose runs when one cries or eyes water excessively. The first division of the trigeminal nerve innervates both the ocular surface and nasal mucosa and is responsible for the nasolacrimal reflex—the tearing that occurs upon stimulation of the nasal mucosa. This response likely occurs, at least in part, to provide additional tear flow to wash away allergens or other noxious stimuli from both the eyes and the nose via the nasolacrimal apparatus. It may also represent a relatively unexplored aspect of dry-eye disease: A 2010 study comparing reflex tearing in normal subjects to dry-eye sufferers found a significant delay in response time in the latter group. (Maffei C, et al. IOVS 2010;51:ARVO E-Abstract 3398) This is likely an aspect of the delay seen in the natural compensatory mechanisms in patients with dry eye.3
A recent innovative approach to dry eye currently in development from Oculeve and Allergan takes advantage of the reflex using a nasal reflex stimulator. In an open-label, six-month study of patients with moderate to severe dry eye, use of the stimulator resulted in significant improvement in Schirmer’s scores, corneal fluorescein staining and symptom scores.4 This novel technology is a first in terms of implementing device technology as a patient-driven complement to drugs or tear substitutes as therapies for dry eye.
The movement of fluid between the eyes and nose raises important questions and concerns about topical eye drop absorption and potential systemic exposure. As the nose is a highly vascular tissue, drugs administered intranasally are almost certain to be absorbed into the bloodstream and may exert systemic effects. This is important for physicians prescribing topical eye drops that may have negative systemic side effects, as it has been demonstrated that some drugs are absorbed from the tear fluid by the epithelial lining of the nasolacrimal duct.5 An example of this is the glaucoma drug timolol, which, when absorbed systemically, can cause a number of adverse effects including insomnia, hallucinations and cardiac effects. Similarly, when absorbed through this route, high-dose topical corticosteroids can exert the systemic side effects more commonly seen with oral steroid use.
Pathophysiology
The connection between the eyes, nose and even mouth comes into sharp focus in allergic disease, where the co-morbidity of rhinitis and allergic conjunctivitis is estimated to be 60 to 90 percent.6 Patients often report symptoms in the eyes, nose and mouth (itchy palate is most common), and it’s likely that nasolacrimal drainage of allergens plays at least some part in this.7 Using the conjunctival allergen challenge model, researchers here at Ora Inc. showed that 82 percent of subjects experienced an itchy palate after allergen was applied directly to the ocular surface via eye drops (Schoemmell E, et al. IOVS 2016;57:ARVO E-Abstract 310). This confirms the notion that ocular allergen exposure alone can cause extraocular effects downstream via allergen, histamine and mediator passage through the nasolacrimal apparatus, highlighting the important link between these tissues. Therefore, the nasolacrimal apparatus is of particular importance in the pathophysiology of allergic disease, acting as the interface and conduit between the external and internal milieu that reacts to allergen exposure with rhinitis (runny nose, congestion, post-nasal drip) and conjunctivitis (red, itchy eyes). Therapy follows the same path, as in clinical trials of the ocular antihistamines Bepreve (Bausch + Lomb) or Lastacaft (Allergan), which both reduced symptoms of allergic rhinitis as well as conjunctivitis.8,9 This dual efficacy holds true for other ophthalmic anti-allergics, as well.10 One might even make the argument that ocular antihistamines are the superior mode of therapeutic drug delivery for both the eye and the nose, particularly with respect to relief of acute itching.10
It’s generally thought that retrograde movement of fluid in the nasolacrimal system is negligible or nonexistent. One study examined this question by using a modified Jones Test, wherein drainage from the ocular surface through the nasolacrimal apparatus is assessed by adding fluorescein to the ocular surface and measuring the amount subsequently collected from the nasal cavity. When fluorescein dye was placed on the ocular surface, it was found in the nose within five minutes in every subject tested. Conversely, when fluorescein was administered intranasally via nasal spray, fluorescein was never detected on the ocular surface in any of the subjects tested.11 While this study suggests that there is no significant movement of fluid from the nose to the ocular surface, this is proving to not be the whole story. Nasal allergen challenges can induce ocular symptoms,12 a finding difficult to reconcile with unidirectional movement of fluids through the nasolacrimal apparatus. Interestingly, in a study using Ora’s Allergen Biocube, a controlled environmental exposure unit that provides a controlled allergen concentration in the air, subjects treated with an intranasally delivered drug (Nasapaque; 3E Therapeutics) saw a significant reduction in rhinorrhea, congestion and nasal and ocular itching. (Gomes P, et al. IOVS 2016;57:ARVO E-Abstract 305)
More Than Meets the Eye
These findings are significant for multiple reasons. In general they suggest that both nasal and ocular symptoms of allergic rhinitis or conjunctivitis may be treated with an intranasal or ocular administration of drug, easing disease management for patients. At a more basic level, though, they show that the link between the nose and eye is complex and dynamic. In another study, for example, the researchers suggest that histamine released following nasal allergen exposure could stimulate afferent nasal nerves, which then induce an efferent parasympathetic response, thereby causing a “nasal-ocular” reflex.13 This response is likely also a target for the selective activity of many H1 histamine receptor antagonists. Inhibiting histamine release in the nose blocks this pathway from the start, reducing or eliminating the conjunctivitis that typically results downstream of antigen challenge.
It is likely that not only allergic but also inflammatory reactions are interconnected in the nose and eye through these same channels. The immunopathology of dry-eye disease has been amply studied, with age-related changes in the ocular and nasal immune system teased out on many levels. One area of interest is nasal-associated lymphoid tissue, or NALT, and its near relation, conjunctiva-associated lymphoid tissue, or CALT. Some researchers have suggested that a deterioration of immune responses of aging NALT contributes to the ocular inflammation observed in dry eye.14 Surgical closure of the nasolacrimal duct in a rabbit model of dry eye significantly decreases the inflammatory responses of conjunctiva-derived T cells, suggesting that communication with NALT somehow enhances the inflammatory response of this ocular mucosal immune system.
Another connection between the eye and the nose is through secretory IgA. Though this mucosal defense mechanism is predominantly directed against pathogens, for many years dry-eye researchers have been studying a possible role of secretory IgA derived from lacrimal glands and other ocular sources. Intranasal immunization induces IgA not only in the nose and salivary glands but also on the ocular surface,15,16 indicating that NALT can serve as an inductive site for ocular mucosal IgA responses. The integrated nature of NALT and the ocular mucosal immune system even provides some rationale for intranasal immunotherapeutic targets for inflammatory dry-eye disease.14 Certainly the notion of intranasal local immunotherapy benefiting ocular allergic disease is attractive, as is the elegant notion of using the ocular or nasal allergic response as a marker for response to systemic immunotherapy.
There’s certainly more to learn about the dynamics of ocular-nasal interactions, and future studies are likely to inform and modify future therapeutic development. For example, what role does the local vasculature play in ocular-nasal interactions? How might depot formulations in the eye impact downstream tissues? Understanding this ocular-nasal complex will surely lead to innovation in treatment delivery and multisystem therapies of the future.
Dr. Abelson is a clinical professor of ophthalmology at Harvard Medical School. Dr. Hollander is chief medical officer at Ora, and assistant clinical professor of ophthalmology at the Jules Stein Eye Institute at the University of California, Los Angeles. Dr. Hertsenberg is a medical writer at Ora. Dr. Abelson may be reached at MarkAbelsonMD@gmail.com.
1. Soiberman U, Kakizaki H, Selva D, Leibovitch I. Punctal stenosis: Definition, diagnosis, and treatment. Clin Ophthalmol 2012;6:1011-1018.
2. Esmaeli B, Valero V, Ahmadi MA, Booser D. Canalicular stenosis secondary to docetaxel (taxotere): A newly recognized side effect. Ophthalmology 2001;108:5:994-5.
3. Ousler GW 3rd, Abelson MB, Nally LA, Welch D, Casavant JS. Evaluation of the time to “natural compensation” in normal and dry eye subject populations during exposure to a controlled adverse environment. Adv Exp Med Biol 2002;506(Pt B):1057-63.
4. Friedman NJ, Butron K, Robledo N, Loudin J, Baba SN, Chayet A. A nonrandomized, open-label study to evaluate the effect of nasal stimulation on tear production in subjects with dry eye disease. Clin Ophthalmol 2016;10:795-804.
5. Paulsen FP, Foge M, Thale AB, Tillmann BN, Mentlein R. Animal Model for the absorption of lipohilic substances from tear fluid by the epithelium of the nasolacrimal ducts. IOVS 2002;43:10:3137-43.
6. Gomes PJ. Trends in prevalence and treatment of ocular allergy. Curr Opin Allergy Clin Immunol 2014;14:5:451-6.
7. Bernstein DI, Teper A, Gopalan G. Effects of intranasal mometasone furoate on itchy ear and palate in patients with seasonal allergic rhinitis. Ann Allergy Asthma Immunol 2012;108:359-362.
8. Macejko TT, Bergmann MT, Williams JI, Gow JA, Gomes PJ, McNamara TR, Abelson MB. Multicenter clinical evaluation of bepotastine besilate ophthalmic solutions 1.0% and 1.5% to treat allergic conjunctivitis. Am J Ophthalmol 2010;150:1:122-127.
9. Torkildsen G, Shedden A. The safety and efficacy of alcaftadine 0.25% ophthalmic solution for the prevention of itching associated with allergic conjunctivitis. Curr Med Res Opin 2011;27:3:623-31.
10. Akhavan A, Karimi-Sari H, Khosravi MH, Arefzadeh E, Yavarahmadi M. Comparing the effects of ketotifen fumarate eye drops and ketotifen oral pills on symptom severity and quality of life in patients with allergic rhinitis: A double-blind randomized clinical trial. Int Forum Allergy Rhinol 2015;5:5:386-91.
11. Spangler DL, Abelson MB, Ober A, Gomes PJ. Randomized, double-masked comparison of olopatadine ophthalmic solution, mometasone furoate monohydrate nasal spray, and fexofenadine hydrochloride tablets using the conjunctival and nasal allergen challenge models. Clin Ther 2003;25:8:2245-2267.
12. Baroody FM, Shenaq D, DeTineo M, Wang J, Naclerio RM. Fluticasone furoate nasal spray reduces the nasal-ocular reflex: A mechanism for the efficacy of topical steroids in controlling allergic eye symptoms. J Allergy Clin Immunol 2009;123:6:1342-8.
13. Baroody FM, Foster KA, Markaryan A, deTineo M, Naclerio RM. Nasal ocular reflexes and eye symptoms in patients with allergic rhinitis. Ann Allergy Asthma Immunol 2008;100:3:194-9.
14. Farid M, Agrawal A, Fremgen D, Tao J, Chuyi H, Nesburn AB, BenMohamed L. Age-related defects in ocular and nasal mucosal immune system and the immunopathology of dry eye disease. Ocul Immunol Inflamm 2016;24:3:327-347.
15. Gill RF, Montgomery PC. Enhancement of rat tear IgA antibody responses following intranasal immunization with antigen and CpG ODN. Curr Eye Res 2002;24:228-233.
16. Ridley Lathers DM, Gill RF, Montgomery PC. Inductive pathways leading to rat tear IgA antibody responses. Invest Ophthalmol Vis Sci 1998;39:1005-1011.



