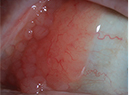
A 59-year-old Caucasian male was referred to the Wills Neuro-ophthalmology Service for a six-month history of intermittent bilateral visual disturbances and two-week history of painless vision loss in the left eye. He described his visual disturbances as yellow and blue pulsating bubbles in the peripheral vision of both eyes. Approximately one month prior to presentation, the patient reported that his vision was measured to be 20/25 in each eye by his optometrist. He denied any headache, fevers/chills, weight loss, jaw claudication, diplopia or other neurologic symptoms.
Medical History
The patient’s past ocular history was significant for mild cataracts in both eyes. His past medical history was significant for coronary artery disease status post quadruple bypass, hypertension, hyperlipidemia, osteoarthritis and hepatitis C. His medications included simvastatin, lisinopril, carvedilol and ibuprofen. He denied any recent travel and had no pets at home. Social history was negative for high-risk sexual activity and illicit drug use. He endorsed a 45 pack-year smoking history and a history of heavy alcohol use until eight months ago.
Examination
The patient’s corrected visual acuity was 20/40 in the right eye and 20/400 in the left without improvement on pinhole. Color plates were full in the right eye and significantly decreased in the left. Amsler grid testing revealed a paracentral inferior scotoma in the left eye. Pupils were normal with no afferent pupillary defect. Motility was full in both eyes. He denied diplopia in all directions of gaze. Intraocular pressure was within normal range and equal in both eyes. There was no proptosis. Nuclear sclerotic lens changes were present. His fundoscopic exam revealed mild hypertensive changes in both eyes and retinal pigment epithelium changes in the left macula. Neurologic exam was unremarkable without weakness, paresthesias, loss of reflexes or ataxia.
What is your differential diagnosis? What further workup would you pursue?
Please click this link for diagnosis, workup, treatment and discussion.