Presentation
A 72-year-old woman presented with a three-day history of blurred central vision, floaters consisting of “sprinkling lights” and a blue light in the superotemporal visual field of her right eye. She didn’t have any pain. Her left eye was asymptomatic.
Medical History
Her past ocular history was notable only for myopia. Past medical history was remarkable for a right bundle branch block, lumpectomy for fibrocystic breast disease (right 2009, left 2006), hysterectomy (2008) and Bell’s palsy (2005, laterality unspecified). Social history was significant for occasional alcohol consumption, but she denied any history of tobacco or drug use. Family history was notable for breast cancer in her mother and thromboangiitis obliterans and Raynaud’s disease in her grandfather.
Her medications included low-dose aspirin, atorvastatin, risedronate, estradiol, mometasone nasal spray and fexofenadine. There had been no recent changes to her medications.
Examination
Her exam demonstrated best-corrected visual acuities of 20/40 OD and 20/20 OS. Pupils, intraocular pressures and motility were normal. Color vision was 11/11 OU but slower OD. Confrontation visual fields demonstrated superotemporal constriction OD. She reported metamorphopsia on Amsler grid testing, OD only. Anterior segment examination was notable for 2+ nuclear sclerosis in both eyes. Dilated fundus examination revealed bilateral posterior vitreous detachment and peripapillary myopic degeneration; the macula was normal OU (Figure 1 A, B).
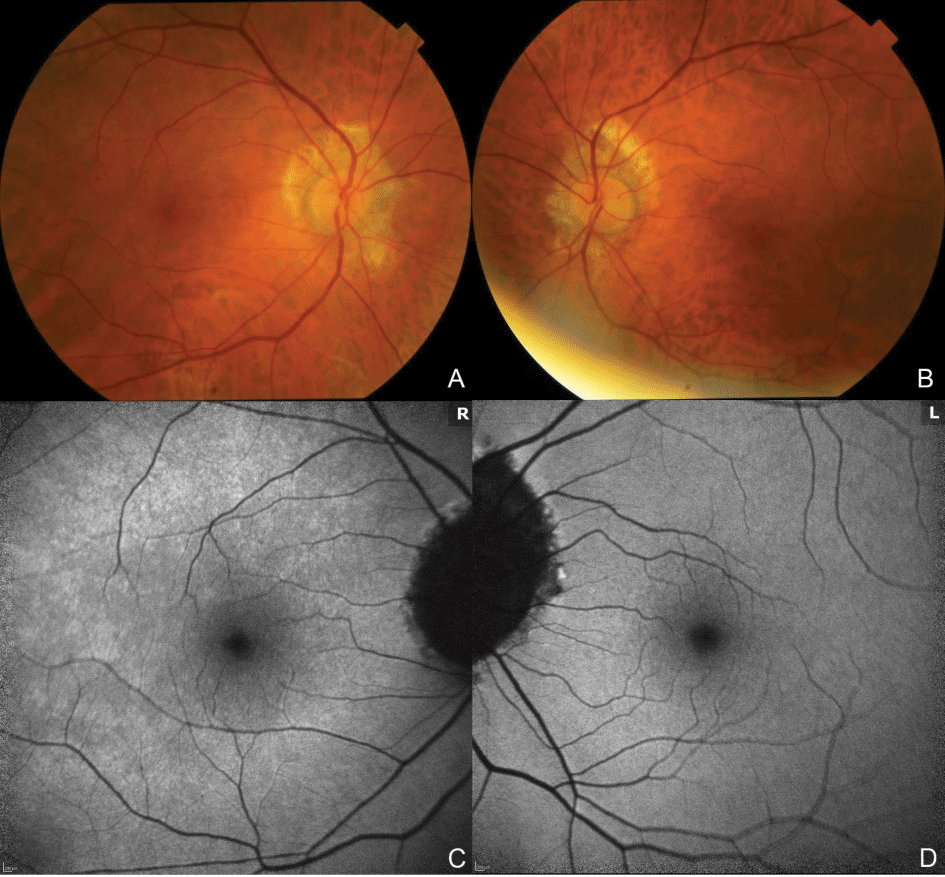 |
|
|
What is your diagnosis? What further workup would you pursue?
Please click this link for diagnosis, workup, treatment and discussion.



