Known as the great imitator because of its protean manifestations, syphilis results from infection by the spirochete Treponema pallidum. Although the incidence of infection has decreased dramatically since advent of penicillin in the the mid-20th century,1 syphilis still represents a large global problem, especially in developing countries. The World Health Organization estimated that 12 million new cases of syphilis occurred worldwide in 1999. Despite a program instituted in the 1990s to eliminate syphilis from the United States, the incidence of infection here has risen by more than 75 percent since 2000, when it was at a low of 2.1 per 100,000 people. According to statistics from the 2008 National STD Prevention Conference (
http://www.cdc.gov/stdconference/ 2008/media/ release-12march 2008.htm), 2007 marked the seventh consecutive year that the rate of syphilis rose in the United States—a year when nearly two-thirds of acquired syphilis infections occurred in men who have sex with men, a group in which the rate of HIV co-infection is also high. Although responsible for less than 5 percent of all cases of uveitis,2,3 syphilis should always be considered in the differential diagnosis of ocular inflammation, both because it is often curable and because accurate diagnosis and treatment prevents further spread of the infection.
Systemic Disease
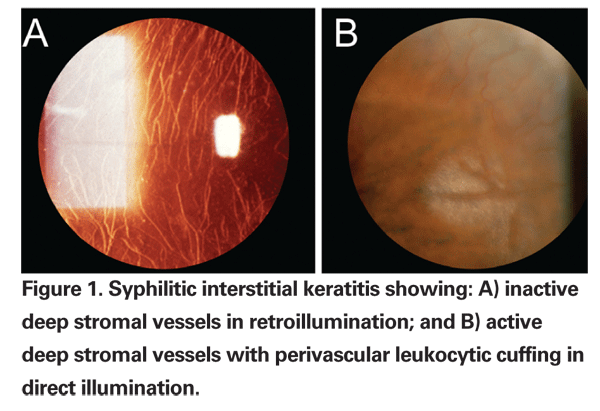
Syphilis can be acquired transplacentally or in the postnatal period. Congenital syphilis can present during childhood with a number of systemic features, including Hutchinson's teeth, saddle nose deformity and deafness, and can also cause ocular complications, most notably interstitial keratitis (See Figure 1) and ectopia lentis.4 Acquired syphilis is divided conventionally into four stages.4 Primary syphilis is characterized by the formation of a painless chancre, which typically appears two to six weeks after infection at the site of inoculation. Secondary syphilis occurs four to 10 weeks following infection and is characterized by non-specific symptoms, such as fever and malaise, as well as the formation of a generalized rash, which often involves the palms and soles.5 Latent syphilis, in which disease is clinically undetectable, can persist for many years. Tertiary syphilis, characterized by neurologic and cardiovascular manifestations, occurs months to years following infection and may produce significant morbidity.
Ocular Manifestations
|
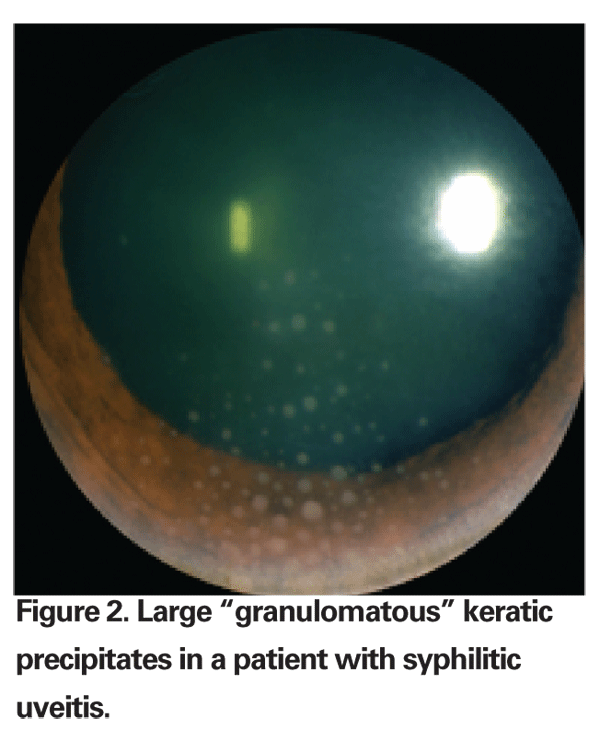
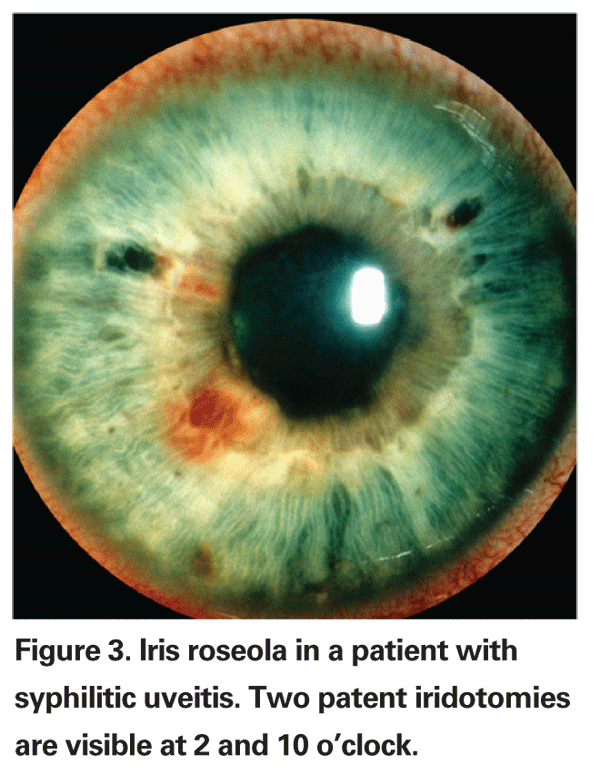
Uveitis, which may be unilateral or bilateral, is one of the most frequent ocular manifestations of syphilis.2,3,9 Granulomatous features, including large keratic precipitates (See Figure 2) and iris nodules, may occur in syphilitic uveitis, but are by no means the norm.10 Dilated iris vessels, known as iris roseolae (See Figure 3), occur rarely, but are relatively specific for syphilis.10 Along with all forms of herpes virus infection, sarcoidosis and toxoplasmosis, syphilis is a common cause of elevated intraocular pressure associated with uveitis, or so-called Inflammatory Ocular Hypertension Syndrome.12
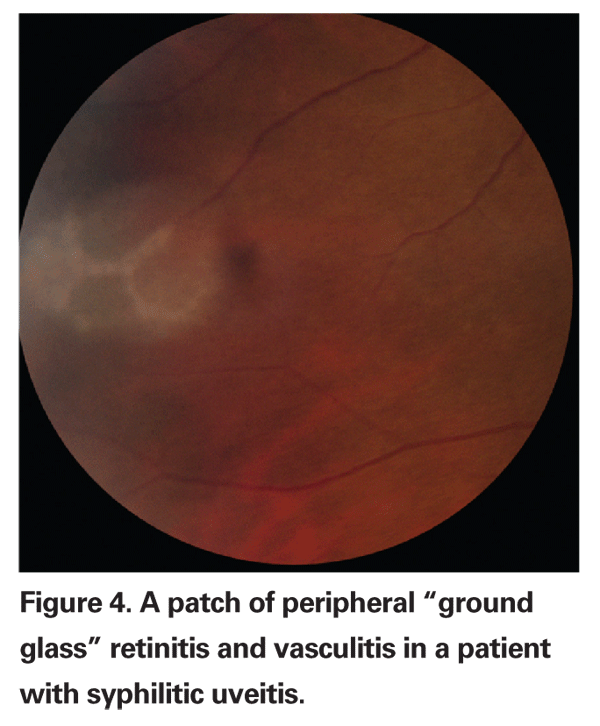
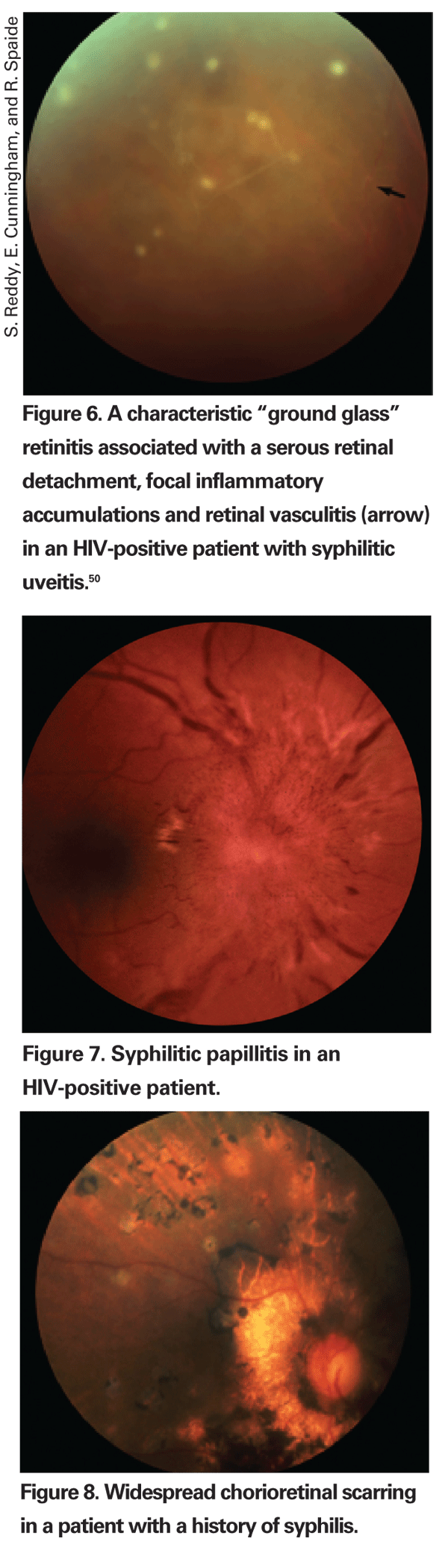
Posterior segment involvement, including chorioretinitis, retinitis, vasculitis, vitritis and panuveitis, can also occur.7,13-15 Chorioretinitis, one of the most frequent manifestations, is typically multifocal and associated with a significant degree of vitreous inflammation.15-17 A "ground glass" retinitis, often associated with retinal vasculitis, is said to be characteristic of syphilis (See Figure 6).18
|
Syphilitic retinitis can be patchy early, becoming more confluent over time.24 Such changes can be difficult to distinguish from acute retinal necrosis (ARN) and toxoplasmic retinochoroiditis, especially when heavy vitritis is present,25 but unlike ARN and toxoplasmosis, syphilitic retinitis responds promptly to penicillin.13,15,22 Syphilitic retinitis can cause serous retinal detachment, which resolves promptly with penicillin treatment (See Figure 6).26 Neuroretinitis, sometimes associated with vasculitis or vitritis, may occur in syphilis as well (See Figure 7).15,27
Isolated retinal vasculitis can affect either arteries or veins and, if occlusive, may cause lasting retinal damage.15,28,29 Although more typical of toxoplasmic retinochoroiditis, nodular arteritis, known as Kyrieleis plaques, can also occur in syphilitic uveitis.30 Syphilitic intermediate uveitis may occur as well, although pars plana exudates are said to be infrequent.7,27 A host of neuro-ophthalmic manifestations, including the Argyll Robertson pupil, optic neuritis and optic neuropathy have also been described.10,31
Diagnosis
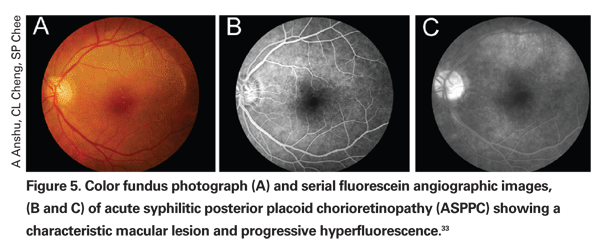
The diagnosis of ocular syphilis depends largely on serologic testing. Despite the stigma of infection and the generally low prevalence of syphilis in the population at large, clinicians should have a low threshold for performing serologic analysis in patients with uveitis.5,32 Strong indications to test include a history of other sexually transmitted diseases or of high-risk sexual behavior, inflammation refractory to treatment with corticosteroids, or the finding of one or more suggestive clinical features described above, such as granulomatous features, iris roseola, ground glass retinitis, focal inflammatory accumulations or findings consistent with ASPPC. A recent case series found non-granulomatous anterior uveitis to be the most common manifestation of syphilitic uveitis, however, suggesting that syphilis testing is indicated even in the absence of suggestive clinical findings.33
Two types of antibody-based serum tests are employed in the diagnosis of syphilis—non-treponemal and treponemal.4 Non-treponemal tests, which include the Rapid Plasma Reagin (RPR) and the Venereal Disease Research Laboratory (VDRL) tests, detect antibodies directed against host antigens, such as cardiolipin, which are released following tissue damage induced by T. pallidum. Non-treponemal tests offer the advantage of quantifiability, reflect both disease activity and response to therapy, and can be used to test for reinfection. RPR and VDRL suffer, however, from limited sensitivity—which has been suggested to be as low as 70 percent.2,34 In contrast, treponemal tests, which include the Fluorescent Treponemal Antibody Absorption (FTA-ABS) and the Microhemagglutination Treponema pallidum (MHA-TP) tests, measure serum antibodies directed specifically against the T. Pallidum, and are highly sensitive. Titers of specific treponemal tests are generally not reliable in gauging response to treatment, however.35 While both treponemal and non-treponemal tests are quite specific, false positive results may occur, for example, in the setting of collagen vascular disease, advanced age and HIV infection. We therefore recommend that both a non-specific and specific test be obtained when considering the diagnosis of ocular syphilis.
Per Centers for Disease Control and Prevention guidelines, analysis of cerebrospinal fluid (CSF) should be performed in all patients with ocular syphilis,15,36,37,38 particularly since the presence of neurologic involvement, which is associated with greater morbidity and mortality, can not be accurately determined clinically. Findings suggestive of neurologic involvement include: greater than five white blood cells per microliter; elevated protein levels; or the presence of either treponemal or non-treponemal antibodies in the CSF. Non-treponemal testing, specifically VDRL or RPR, is performed most commonly on CSF and offers the same advantages and disadvantages relative to specific treponemal testing as described above for serologic testing.39
Direct visualization of treponemes by darkfield microscopy or silver staining aspirated fluids or excised tissues is also possible. Samples can be obtained from a chancre in primary syphilis, from an open pustule or regional lymph node in secondary disease, or from aqueous humor or vitreous in patients with uveitis.40 Polymerase chain reaction-based analysis of intraocular fluids may also be performed, particularly when serologic testing is unreliable, as in patients with collagen vascular disease, advanced age or HIV infection.39 In practice, however, such fluid- and tissue-based tests are rarely done in patients suspected of having ocular syphilis.
 |
Treatment
Penicillin is the treatment of choice for all stages of syphilis. Acquired syphilis with ocular involvement should be treated as neurosyphilis with intravenous penicillin G, 18 to 24 million units (MU) daily for 10 to 14 days, followed by intramuscular procaine penicillin, 2.4 MU weekly for three weeks.36,37 T. pallidum replicates once every 30 hours, so sustained elevated intraocular levels of penicillin are required to achieve a bactericidal effect. Treatment failure may occur in patients treated solely with intramuscular penicillin, which does not achieve adequate, sustained intraocular concentrations.3,14,18,22 The overall failure rate of penicillin treatment in immunocompetent patients is approximately 1 percent,43 although persistent or recurrent disease may, in some cases, be attributed to noncompliance or insufficient therapy.3,18,43,44
In patients with penicillin allergy, several therapeutic alternatives are available, including tetracycline, doxycycline, chloramphenicol, ceftriaxone and the macrolide antibiotics.22,45 No antibiotic other than penicillin, however, has been proven to be effective for the treatment of syphilis. Therefore, penicillin desensitization, in which increasing doses of the penicillin are administered with careful monitoring, is sometimes recommended, particularly in patients with neurologic involvement.13
 |
In assessing the efficacy of therapy, either RPR or VDRL titers should be obtained at six, 12 and 24 months following treatment, and more frequently in patients with HIV.37 If a fourfold decrease in non-treponemal antibody titers is not achieved following six months of treatment in patients with primary or secondary syphilis, or 12 months after treatment in patients with latent or tertiary disease, reanalysis of the CSF, reassessment of HIV status and re-treatment should be considered. In patients with positive CSF abnormalities, lumbar puncture should be performed every six months following treatment until the abnormalities have normalized.37 Retreatment should be considered if the CSF white blood cell count has not decreased by six months after therapy or if CSF abnormalities persist past two years following treatment.
Long-Term Ocular Complications
Common long-term complications of syphilitic uveitis include glaucoma, cataract, epiretinal membrane and macular edema. Choroidal neovascularization, while uncommon, has been described and may resolve following treatment with penicillin.44 The Jarisch-Herxheimer reaction, which results from the release of treponemal antigens from spirochetes killed following initiation of antibiotic therapy, may result in fever, malaise and headache, as well as a worsening of ocular manifestations48 and may be prevented by administration of systemic corticosteroids concurrent with antibiotic treatment. Widespread chorioretinal scarring can occur in some patients.
Syphilis and HIV
A high index of suspicion for ocular syphilis should be maintained in all HIV-infected patients, regardless of CD4 count.22,49 Unusual ocular manifestations, including ASPPC (See Figure 7) and preretinal focal inflammatory accumulations (See Figure 8), have been observed more commonly in HIV-positive patients.50,51 HIV-positive individuals are also more likely to have a severe, atypical clinical course;14,52-54 uveitis is more frequently posterior and bilateral; central nervous system involvement is more common; and serologic testing is less reliable in patients with HIV.22,55 Of note, the sensitivity of treponemal tests (FTA-ABS, MHA-TP) has been reported to be as low as 62 percent in symptomatic HIV-positive patients.10,29,56
Patients with HIV are also at increased risk for serologic treatment failure, with slower normalization of antibody titers or CSF abnormalities.57,58 Cases of actual treatment failure despite high-dose intravenous penicillin treatment have prompted some experts to recommend a prolonged treatment course and possibly maintenance therapy in patients with HIV infection.22,54
Syphilis remains a common infection worldwide. Despite initially successful attempts to lower the incidence of syphilis in the United States in the 1990s, a steady increase in the rate of infection has been noted since 2000, especially among men who have sex with men and in those infected with HIV. Syphilis should be considered in all patients with uveitis, and in particular those who are known to be HIV-positive or who engage in high-risk sexual activities. Serologic testing is required both to confirm the diagnosis and to monitor response to therapy. Patients with ocular syphilis should undergo CSF testing and, regardless of findings, be treated as neurosyphilis with 10 to 14 days of high-dose intravenous followed by three weekly injections of IM penicillin. All patients found to have syphilis should be reported to the local health authority so that sexual partners can be contacted and tested.
Dr. Wender is a resident in ophthalmology at California Pacific Medical Center in San Francisco. Dr. Eliott is a professor of ophthalmology and director of the Retina Service at Doheny Eye Institute, University of Southern California, Los Angeles. Dr. Jumper is the CPMC Retina Service chief and in private practice at the West Coast Retina Medical Group. Dr. Cunningham is director of the Uveitis Service at CPMC, an adjunct clinical professor of ophthalmology at Stanford University School of Medicine, and in private practice at West Coast Retina Medical Group. Contact Dr. Cunningham at West Coast Retina, 185 Berry St, San Francisco, Calif. 94107. Phone: (415) 972 4600; fax: (415) 975 0999; e-mail:
emmett_cunning ham@yahoo.com. This work was supported by the San Francisco Retinal Foundation and the Pacific Vision Foundation.
1. Primary and secondary syphilis--United States, 2003-2004. MMWR Morb Mortal Wkly Rep 2006;55:269-73.
2. Tamesis RR, Foster CS. Ocular syphilis. Ophthalmology 1990;97:1281-7.
3. Barile GR, Flynn TE. Syphilis exposure in patients with uveitis. Ophthalmology 1997;104:1605-9.
4. Fauci AS. Harrison's principles of internal medicine. New York: McGraw-Hill, 2008.
5. Foster CS, Vitale AT. Diagnosis and treatment of uveitis. Philadelphia: W.B. Saunders, 2002:xvi,900.
6. Spektor FE, Eagle RC, Jr., Nichols CW. Granulomatous conjunctivitis secondary to Treponema pallidum. Ophthalmology 1981;88:863-5.
7. Deschenes J, Seamone CD, Baines MG. Acquired ocular syphilis: Diagnosis and treatment. Ann Ophthalmol 1992;24:134-8.
8. Marks R, Thomas-Kaskel AK, Schmidt D, Donauer J. Steroid refractory episcleritis as early manifestation of neurosyphilis. Eur J Med Res 2006;11:309-12.
9. Aldave AJ, King JA, Cunningham ET Jr. Ocular syphilis. Curr Opin Ophthalmol 2001;12:433-41.
10. Margo CE, Hamed LM. Ocular syphilis. Surv Ophthalmol 1992;37:203-20.
11. Rapkin JS, Bogorad DD. Bilateral dislocation of the crystalline lens in a patient with presumed syphilitic uveitis. Henry Ford Hosp Med J 1986;34:207-10.
12. Reddy S, Cubillan LD, Hovakimyan A, Cunningham ET Jr. Inflammatory ocular hypertension syndrome (IOHS) in Patients with Syphilitic Uveitis. Br J Ophthalmol 2007; 91: 1610-2. Epub 2007 May 23.
13. Chao J, Khurana RN, Fawzi AA. Syphilis: Reemergence of an old adversary. Ophthalmology 2006;113:2074-9.
14. Shalaby IA, Dunn JP, Semba RD, Jabs DA. Syphilitic uveitis in human immunodeficiency virus-infected patients. Arch Ophthalmol 1997;115:469-73.
15. Ormerod LD, Puklin JE, Sobel JD. Syphilitic posterior uveitis: Correlative findings and significance. Clin Infect Dis 2001;32:1661-73.
16. Thomas S, Wiselka M, Dhar J, Bibby K. Syphilis presenting as acute multifocal retino-choroiditis. J R Soc Med 2006;99:371-2.
17. de Souza EC, Jalkh AE, Trempe CL. Unusual central chorioretinitis as the first manifestation of early secondary syphilis. Am J Ophthalmol 1988;105:271-6.
18. Browning DJ. Posterior segment manifestations of active ocular syphilis, their response to a neurosyphilis regimen of penicillin therapy, and the influence of human immunodeficiency virus status on response. Ophthalmology 2000;107:2015-23.
19. Gass JD, Braunstein RA, Chenoweth RG. Acute syphilitic posterior placoid chorioretinitis. Ophthalmology 1990;97:1288-97.
20. Baglivo E, Kapetanios A, Safran AB. Fluorescein and indocyanine green angiographic features in acute syphilitic macular placoid chorioretinitis. Can J Ophthalmol 2003;38:401-5.
21. Ouano DP, Brucker AJ, Saran BR. Macular pseudohypopyon from secondary syphilis. Am J Ophthalmol 1995;119:372-4.
22. Tran TH, Cassoux N, Bodaghi B. Syphilitic uveitis in patients infected with human immunodeficiency virus. Graefe's Arch Clin Exp Ophthalmol 2005;243:863-9.
23. Zamani M, Garfinkel RA. Corticosteroid-induced modulation of acute syphilitic posterior placoid chorioretinitis. Am J Ophthalmol 2003;135:891-4.
24. Dodds EM, Lowder CY, Boskovich SA. Simultaneous syphilitic necrotizing retinitis and placoid chorioretinitis in acquired immune deficiency syndrome. Retina 1995;15:354-6.
25. Huang C, Park S, Castellarin AA. Diagnostic and therapeutic challenges. Retina 2007;27:385-90.
26. Jumper JM, Machemer R, Gallemore RP, Jaffe GJ. Exudative retinal detachment and retinitis associated with acquired syphilitic uveitis. Retina 2000;20:190-4.
27. McLeish WM, Pulido JS, Holland S. The ocular manifestations of syphilis in the human immunodeficiency virus type 1-infected host. Ophthalmology 1990;97:196-203.
28. Yokoi M, Kase M. Retinal vasculitis due to secondary syphilis. Jpn J Ophthalmol 2004;48:65-7.
29. Venkatesh P, Verma L, Garg SP, Tewari HK. Rapid seroconversion to Treponema pallidum and HIV positivity in a patient with retinal vasculitis. Clin Experiment Ophthalmol 2002;30:297-9.
30. Krishnamurthy R, Cunningham ET Jr. Atypical presentation of syphilitic uveitis associated with Kyrieleis plaques. Br J Ophthalmol 2008;92:1152-3.
31. Pelfrene E, Michielsen W, Voet D. Neurosyphilis presenting with optic neuropathy. Report of a case and review. Acta Clin Belg 1993;48:324-30.
32. Colletti JE, Giudice EL. Syphilis screening in a high-risk, inner-city adolescent population. Am J Emerg Med 2005;23:225-6.
33. Anshu A, Cheng CL, Chee SP. Syphilitic uveitis: An Asian perspective. Br J Ophthalmol 2008;92:594-7.
34. Backhouse JL, Nesteroff SI. Treponema pallidum western blot: Comparison with the FTA-ABS test as a confirmatory test for syphilis. Diagn Microbiol Infect Dis 2001;39:9-14.
35. Augenbraun M, Rolfs R, Johnson R. Treponemal specific tests for the serodiagnosis of syphilis. Syphilis and HIV Study Group. Sex Transm Dis 1998;25:549-52.
36. Jay CA. Treatment of neurosyphilis. Curr Treat Options Neurol 2006;8:185-92.
37. Workowski KA, Berman SM. Sexually transmitted diseases treatment guidelines, 2006. MMWR Recomm Rep 2006;55:1-94.
38. Hart G. Syphilis tests in diagnostic and therapeutic decision making. Ann Intern Med 1986;104:368-76.
39. Muller M, Ewert I, Hansmann F. Detection of Treponema pallidum in the vitreous by PCR. Br J Ophthalmol 2007;91:592-5.
40. Tabbara KF, al Kaff AS, Fadel T. Ocular manifestations of endemic syphilis (bejel). Ophthalmology 1989;96:1087-91.
41. Villanueva AV, Sahouri MJ, Ormerod LD. Posterior uveitis in patients with positive serology for syphilis. Clin Infect Dis 2000;30:479-85.
42. Kuo IC, Kapusta MA, Rao NA. Vitritis as the primary manifestation of ocular syphilis in patients with HIV infection. Am J Ophthalmol 1998;125:306-11.
43. Poitevin M, Collart P, Bolgert M. Syphilis in 1986. J Clin Neuroophthalmol 1987;7:11-9.
44. Halperin LS, Lewis H, Blumenkranz MS. Choroidal neovascular membrane and other chorioretinal complications of acquired syphilis. Am J Ophthalmol 1989;108:554-62.
45. Savaris RF, Abeche AM. Azithromycin versus penicillin for early syphilis. N Engl J Med 2006;354:203-5; author reply 203-5.
46. Yagasaki T, Akiyama K, Nomura H, Awaya S. Two cases of acquired syphilis with acute central chorioretinitis as initial manifestation. Jpn J Ophthalmol 1992;36:301-9.
47. Orsoni JG, Zavota L, Manzotti F, Gonzales S. Syphilitic interstitial keratitis: Treatment with immunosuppressive drug combination therapy. Cornea 2004;23:530-2.
48. Fathilah J, Choo MM. The Jarisch-Herxheimer reaction in ocular syphilis. Med J Malaysia 2003;58:437-9.
49. Westeneng AC, Rothova A, de Boer JH, de Groot-Mijnes JD. Infectious uveitis in immunocompromised patients and the diagnostic value of polymerase chain reaction and Goldmann-Witmer coefficient in aqueous analysis. Am J Ophthalmol 2007;144:781-5.
50. Reddy S, Cunningham ET Jr., Spaide RF. Syphilitic retinitis with focal inflammatory accumulations. Ophthalmic Surg Lasers Imaging 2006;37:429-31.
51. Moloney G, Branley M, Kotsiou G, Rhodes D. Syphilis presenting as scleritis in an HIV-positive man undergoing immune reconstitution. Clin Experiment Ophthalmol 2004;32:526-8.
52. Diaz-Valle D, Allen DP, Sanchez AA. Simultaneous bilateral exudative retinal detachment and peripheral necrotizing retinitis as presenting manifestations of concurrent HIV and syphilis infection. Ocul Immunol Inflamm 2005;13:459-62.
53. Thami GP, Kaur S, Gupta R. Syphilitic panuveitis and asymptomatic neurosyphilis: A marker of HIV infection. Int J STD AIDS 2001;12:754-6.
54. Becerra LI, Ksiazek SM, Savino PJ. Syphilitic uveitis in human immunodeficiency virus-infected and noninfected patients. Ophthalmology 1989;96:1727-30.
55. Balba GP, Kumar PN, James AN. Ocular syphilis in HIV-positive patients receiving highly active antiretroviral therapy. Am J Med 2006;119:448 e21-5.
56. Haas JS, Bolan G, Larsen SA. Sensitivity of treponemal tests for detecting prior treated syphilis during human immunodeficiency virus infection. J Infect Dis 1990;162:862-6.
57. Rolfs RT, Joesoef MR, Hendershot EF. A randomized trial of enhanced therapy for early syphilis in patients with and without human immunodeficiency virus infection. The Syphilis and HIV Study Group. N Engl J Med 1997;337:307-14.
58. Telzak EE, Greenberg MS, Harrison J. Syphilis treatment response in HIV-infected individuals. Aids 1991;5:591-5.