Narrow-angle glaucoma is a frequently missed diagnosis because patients don’t experience acute pain or vision loss. “Chronic angle-closure glaucoma is one of the most frequently missed glaucoma diagnoses I see in glaucoma referral because the angle anatomy wasn’t appreciated or wasn’t being treated,” says Louis B. Cantor, MD, professor at the Indiana University Department of Ophthalmology. “The referral may say the patient has primary open-angle glaucoma, when in fact he or she has slowly progressive chronic angle closure and he or she just wasn’t diagnosed properly initially. Chronic angle closure often clinically behaves like primary open-angle glaucoma.”
In this article, glaucoma experts share their tips for catching this unique variety of the disease.
The Importance of Technicians
The first line of defense in catching narrow-angle glaucoma is the ophthalmic technician. “Technicians are the first people in the practice to see patients, so I think it’s very important for technicians in the offices of comprehensive ophthalmologists, anterior segment surgeons and retinal specialists to be able to recognize what a narrow angle looks like,” says Valerie Trubnik, MD, who is in practice in Mineola, New York. “All too often, it’s missed. Patients are often dilated by the technician at the beginning of their visit, and I’ve seen a couple of patients who have returned post-dilation from other offices in acute angle closure. It doesn’t happen very often, but it can. So, it’s very important to educate the technical staff about what a narrow angle looks like at the slit lamp via the Van Herick technique. If there is any question, the physician can do a gonioscopy before the dilation.”
She also recommends that technicians look at the patient’s refraction when considering her risk. “If someone is hyperopic or phakic, there is the possibility of narrow angles,” Dr. Trubnik says. “If someone is pseudophakic, then they probably don’t have narrow angles.”
Michael Stiles, MD, from Overland Park, Kansas, agrees and says that all of his technicians are trained to screen for narrow-angle closure, particularly in patients who are hyperopic. “If a patient is more than +3 D hyperopic, our technicians will ask me to perform gonioscopy before we consider dilating the patient,” he says. “I’ll certainly check with the pen light from the side to try to gauge the gross depth of the chamber before considering dilation, and then do gonioscopy if it looks suspicious.”
Gonioscopy
Gonioscopy remains the gold standard for assessing narrow angles and angle closure, whether acute or chronic, and glaucoma experts agree that all patients should undergo it. “The best tip for not missing [narrow-angle glaucoma] is gonioscopy, gonioscopy, gonioscopy,” Dr. Cantor says. “It’s quick, and it’s worth the time for every new patient to have gonioscopy and have the angle assessed. If there are any questions about what is seen on gonioscopy, that can be supplemented with imaging to help clinch that diagnosis or try to determine how at-risk a patient may be.”
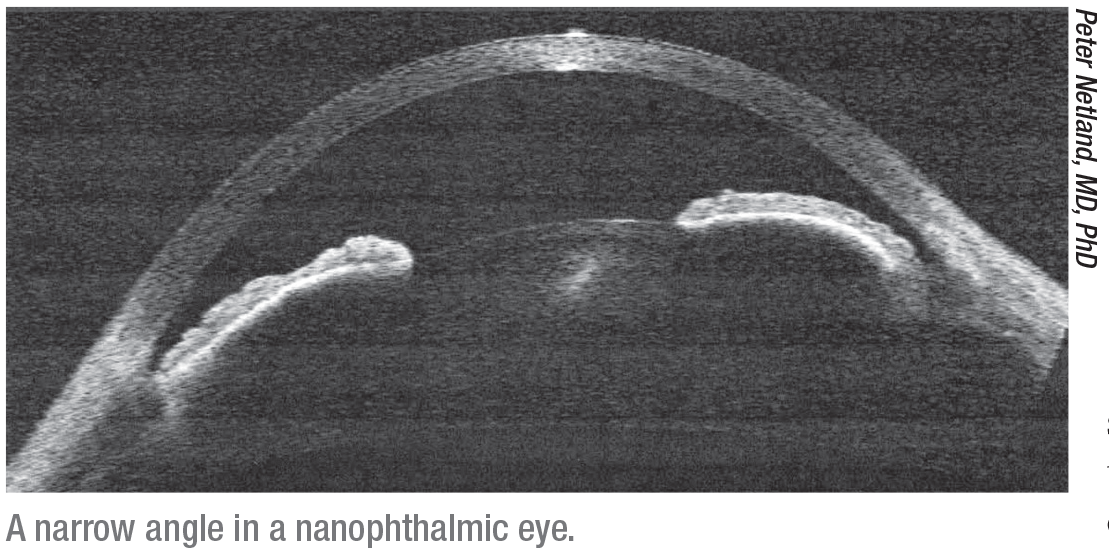 |
Physicians say it’s critical to have a high index of suspicion and look at the angle in all new patients, particularly new glaucoma patients. “I’ve seen cases of narrow and potentially critical angles in myopes, so I think every new patient should undergo gonioscopy, whether or not they’re at risk for angle closure,” Dr. Stiles says. “But, certainly concentrate on the patients most at risk: hyperopes; women; the elderly; and patients with a family history of glaucoma, particularly angle-closure glaucoma.”
Dr. Stiles adds that it’s important to assess both eyes. “Unilateral narrow angles could potentially be a sign of some other type of posterior segment pathology. It’s particularly important to perform gonioscopy on the contralateral eye in a patient who has angle closure or a steamy cornea and high intraocular pressure. These patients could have neovascular glaucoma or something else,” he says.
According to Nathaniel Radcliffe, MD, who is in practice in New York City, it’s important to understand that some people will have open angles in bright light conditions and closed angles in the dark. “So, when you assess the angles in your office, it’s of critical importance to do a pitch black gonioscopy with all lights in the room off, including all computer monitors and phones,” Dr. Radcliffe says. “This is called dark-room gonioscopy. Of course, a dark room setting can be used with our other two angle-detection techniques, which are anterior-segment OCT and ultrasound biomicroscopy. I use all three of those in my patients with glaucoma.”
Dr. Radcliffe also recommends performing gonioscopy at more than one visit. “Repeating gonioscopy on a different day yields slightly different results with surprising frequency,” he says. “I have patients who looked open one year and were closed the next. I don’t think that they changed in one year; I think they fluctuate from visit to visit. Gonioscopy is incredibly valuable, so, repeat it. Do it often. I do it at least annually in patients with glaucoma. And if there’s a question in my mind, I repeat it. It’s not an expensive test, so we should do as much as we need to make sure we never miss angle closure.”
Dr. Cantor also sees value in periodic gonioscopy exams. “We tend to think once we’ve done it, we never need to do it again,” Dr. Cantor says. “Gonioscopy and looking at the angle are very underutilized. Studies have shown that many patients in a Medicare database who are undergoing glaucoma surgery have never been billed for gonioscopy. It’s surprising that so many patients undergoing glaucoma surgery haven’t had their angle examined.”
Dr. Stiles notes that some ophthalmologists use prone testing and dilation as provocative tests. “Some people use prone testing, where patients sit in a dark room in the prone position, as a provocative test to induce elevated pressure if they’re angle-closure suspects,” he says. “I don’t find that very practical, and I don’t know if the sensitivity is strong enough to justify that in a busy clinical practice. Additionally, I don’t dilate patients as a provocative test. Many times, they’ll develop elevated pressures hours later, not immediately. Diagnosis really comes down to gonioscopy.”
Anterior-segment OCT
While a comprehensive clinical exam and gonioscopy are good first steps when examining a patient’s iridocorneal angle, a few supplemental technologies are now available to help ophthalmologists better understand the angle anatomy.
Probably the most commonly used adjunct to supplement gonioscopy is anterior segment optical coherence tomography. “Anterior-segment OCT is limited in that you can’t see anything posterior to the iris plane because of shadowing and loss of signal,” explains Dr. Cantor. “But one of the advantages of an anterior-segment OCT over an ultrasound, which can look posterior to the iris, is that OCT is generally a non-contact exam. Additionally, the patient can be imaged in the seated position with OCT, so that you can see what happens with the lens and you can look at multiple quadrants all at once. This is difficult to do with ultrasound biomicroscopy, where the patient often has to be in the supine position, and you can only image certain areas of the angle at a time. And, of course, when a patient is lying down, the lens may displace posteriorly and change the angle anatomy.”
Dr. Radcliffe says you can multi-task when doing an OCT exam, since most modern OCT machines allow the capacity for anterior-segment OCT, as well as posterior-segment imaging. “If you are managing glaucoma, you should definitely invest in anterior-segment OCT capability,” he says. “Many ophthalmologists have anterior-segment OCT capability, but they don’t use it. The reimbursement hasn’t been perfect, and you can’t bill for an anterior-segment OCT done at the same visit at which you bill for an optic nerve OCT. However, it’s important to focus on the care you want to provide and not on reimbursement. So, every time I have a patient in my office and we’re scanning the optic nerve, I ask the technician to scan the angles as well—and you get surprises now and again. The key, though, is that it only takes your tech a few moments to scan the angles when he or she is already scanning either the macula or the nerve.”
Dr. Trubnik says she’s using anterior-segment OCT more often. “It depends on how the imaging is done,” she explains. “For example, it depends on how much light is in the room during imaging. Even if the angle looks open on anterior-segment OCT but appears closed to me on exam, I will, of course, still recommend a laser peripheral iridotomy.
“I also find anterior-segment OCT very useful when I’m talking to patients,” she adds. “So, for instance, if I’m consenting someone for a laser iridotomy, just doing a gonioscopy isn’t sufficient evidence for patients. Even though they trust me, it really helps if they see the anterior-segment OCT in order to visualize what I’m talking about.”
Patients may not believe that they have narrow-angle glaucoma because they have no pain and no visual symptoms. “It’s a silent condition that they’re unaware of,” Dr. Trubnik says. “So, it can be helpful to actually show them an image of a normal anterior- segment OCT and then their narrow-angle image.”
Dr. Trubnik also uses imaging to follow glaucoma progression. “In some patients, I’ll do it every six months to show them how things are changing,” she explains. “However, I don’t by any means use it as a substitute for my exam. Just looking at the anterior segment OCT can’t diagnose someone with narrow angles or rule it out. It’s just something I use as confirmation.”
Dr. Stiles also uses imaging to follow progression. “This is particularly true if I have a patient who is at risk, but he or she isn’t convinced. “I’ll follow that patient for serial analysis. The other instance would be following a patient who has a fairly narrow angle even after iridotomy.”
Ultrasound Biomicroscopy
Less often, Dr. Trubnik will perform ultrasound. “I find that it’s more helpful in patients in whom I’m suspecting plateau iris,” she says. “It shows me the ciliary body. I don’t use it on a regular basis with just a standard narrow-angle patient.”
Dr. Radcliffe agrees. “For the most part, ophthalmologists and glaucoma specialists can get along fine without using ultrasound biomicroscopy,” he avers. “There are lots of platforms available, so it’s possible to have one in your office. But you don’t need to test every day, and it is a little bit more nuanced, so, it’s nice if you have a colleague you can refer to for the occasions you need it. Everyone doesn’t need UBM in their practice. Having said that, if you do have UBM, it’s very useful. It’s particularly useful for looking at the ciliary body and detecting plateau iris, which occurs in patients who’ve had an iridotomy but still have a narrow angle after the iridotomy has been performed. UBM is also useful for some of the oddball cases of angle closure that don’t make sense and don’t seem to be following the normal patterns.
“If you are performing UBM, performing it in the dark will provide the best yield in terms of detecting people with closed angles, because the pupil dilates in the dark,” Dr. Radcliffe continues. “Of course, we spend one-third of our lives with our eyes closed and our pupils dilated in sleep, so there are many glaucoma patients who look like they have open angles during the day in a lit room, but in the dark with their eyes closed is when the trabecular meshwork is getting damaged and the pressure is probably high.”
The Future
According to Dr. Cantor, the major advantage of anterior-segment OCT is that you can get quantitative assessment. “Gonioscopy is very subjective,” he notes. “With OCT, we can begin to put numbers to things and quantify the angle anatomy in ways that we couldn’t previously. In the future, I think we’ll have Fourier-Domain OCT to get more three-dimensional imaging. This may allow us to better predict those patients who are at risk for angle closure than perhaps we are able to do today. And I think the use of it will grow, but it still won’t replace gonioscopy. Rather, it will supplement our gonioscopy findings to help us better understand the angle anatomy and which patients may be at risk for developing angle-closure glaucoma.” REVIEW
Dr. Cantor is a consultant for Zeiss. Dr. Radcliffe is a consultant for Zeiss and Reichert. Drs. Trubnik and Stiles have no financial interests to disclose.



