Ischemic optic neuropathy is a major cause of blindness or significantly impaired vision, and there are few definitive answers regarding its cause, clinical features and treatment.
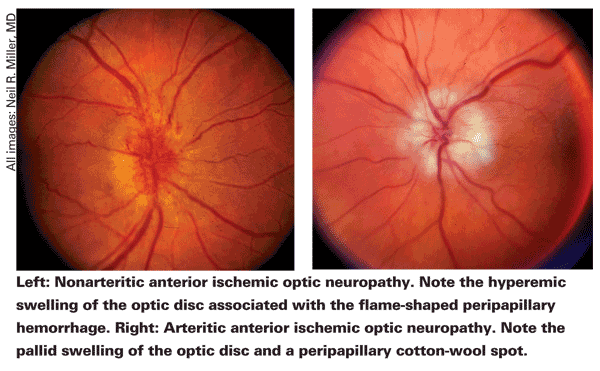
There are two types of ION: anterior (which is characterized by swelling of the optic nerve head) and posterior (in which there is no swelling).
Additionally, each type has several subtypes. Anterior ION is the most common form, while posterior ION is rare. Both can be divided into three subtypes: arteritic (usually due to giant cell arteritis); nonarteritic (due to non-inflammatory causes); and perioperative.
Patients with both anterior and posterior ischemic optic neuropathy present with acute vision loss in one or both eyes that is not associated with pain. "On examination, they have signs that the optic nerve is not functioning normally," says Victoria S. Pelak, MD, an associate professor of neurology and ophthalmology at the University of Colorado-Denver School of Medicine. "These signs include a loss of visual acuity or visual field, an afferent pupillary defect and an abnormal-appearing optic nerve when the ION is anterior."
Arteritic ION
Arteritic anterior and posterior ION are less common than nonarteritic anterior and posterior ION, but they are ocular emergencies that require early diagnosis and immediate treatment. To establish a diagnosis of arteritic ION, patients are asked about the signs and symptoms of temporal arteritis, which include headache, pain in the jaw and pain in the scalp. "Then, we look for that same inflammation of the arteries in the back of the eye, which suggests that it is arteritis (arteritic anterior ION, posterior ION, or retinal arterial occlusion). An erythrocyte sedimentation rate and C-reactive protein are blood tests performed to look for inflammation in the blood," says Andrew G. Lee, MD, chair of the department of ophthalmology at
 Arteritic ION must be treated immediately with systemic high-dose steroids to prevent further vision loss. "The most important role of treatment is to prevent vision loss in the fellow eye, because approximately 50 percent of patients will go blind in the other eye within five to 10 days without treatment," according to Neil R. Miller, MD, professor of ophthalmology, neurology and neurosurgery at Johns Hopkins University School of Medicine in Baltimore. "In addition, some studies have shown that treatment with high-dose steroids will occasionally reverse vision loss in the affected eye."
Arteritic ION must be treated immediately with systemic high-dose steroids to prevent further vision loss. "The most important role of treatment is to prevent vision loss in the fellow eye, because approximately 50 percent of patients will go blind in the other eye within five to 10 days without treatment," according to Neil R. Miller, MD, professor of ophthalmology, neurology and neurosurgery at Johns Hopkins University School of Medicine in Baltimore. "In addition, some studies have shown that treatment with high-dose steroids will occasionally reverse vision loss in the affected eye."
One such study was conducted by Mark J. Kupersmith, MD, director of neuro-ophthalmology at
Nonarteritic ION
Most patients who develop nonarteritic anterior or posterior ION have underlying vascular disease, such as hypertension, diabetes or hypercholesterolemia. However, these conditions may be undiagnosed. "These patients have an increased risk of stroke, heart attack and death by vascular causes," Dr. Miller says. "For these patients, it is important to realize that it is not just about the vision. It is about the general health of the patient. Nonarteritic ION almost never occurs in isolation."
A recent study evaluated the role of cardiovascular risk factors in the development of nonarteritic anterior ION.2 This study included 85 patients who were newly diagnosed with nonarteritic anterior ION and 107 age- and gender-matched healthy patients. The study found that elevated plasma homocysteine and lipoprotein(a) levels, as well as low vitamin B6 levels, may increase the risk of developing nonarteritic anterior ION. The authors suggest that screening for these markers could aid in diagnosis.
Additionally, obstructive sleep apnea has been associated with nonarteritic anterior ION.3,4 "Up to 80 percent of patients who have nonarteritic anterior or posterior ION have obstructive sleep apnea, so the ophthalmologist should ask about symptoms like insomnia, snoring and chronic fatigue," Dr. Miller says. "If there is a positive answer, the ophthalmologist should suggest to the patient or the patient's physician that the patient undergo sleep studies."
 Some medications have also been linked to nonarteritic ION. "In particular, there have been implications that erectile dysfunction medications might predispose people who otherwise might get this disease to go ahead and develop ischemic optic neuropathy," says Kenneth Shindler, MD, PhD, from the department of ophthalmology at the University of Pennsylvania's Scheie Eye Institute in Philadelphia. "One theory is that these drugs cause dilation of blood vessels in other parts of the body, perhaps drawing blood away from the eye."
Some medications have also been linked to nonarteritic ION. "In particular, there have been implications that erectile dysfunction medications might predispose people who otherwise might get this disease to go ahead and develop ischemic optic neuropathy," says Kenneth Shindler, MD, PhD, from the department of ophthalmology at the University of Pennsylvania's Scheie Eye Institute in Philadelphia. "One theory is that these drugs cause dilation of blood vessels in other parts of the body, perhaps drawing blood away from the eye."
However, a study conducted at the
According to Dr. Miller, amiodarone has also been associated with nonarteritic ION. A retrospective case review of 22 patients who developed optic neuropathy while taking amiodarone found that a diagnosis of amiodarone-induced optic neuropathy seemed probable in 14 patients. The association between amiodarone and optic neuropathy was indeterminate in five patients and coincidental in three patients.6
"Ischemic optic neuropathy caused by medication use is very rare, but that doesn't mean it can't occur," Dr. Miller adds. "When the ophthalmologist sees a patient with nonarteritic ION, he or she should ask about medication use."
Dr. Kupersmith notes that the vast majority of cases of acute nonarteritic ION are unilateral. "Be suspicious if it is bilateral at presentation. Then, you are really looking for systemic disease or medication as a cause," he notes.
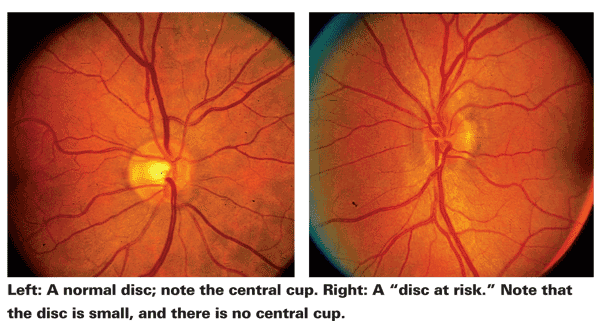
Dr. Lee adds that when a patient is first diagnosed, he examines the other eye to see if it has a "disc at risk," which is a small cup-to-disc ratio. "A small and crowded optic nerve is a predisposing risk factor for the development of the nonarteritic form of anterior ION, and a big cup-to-disc ratio in the fellow eye should make one think about arteritic anterior ION in the affected eye," he says.
A study conducted at the
Unfortunately, there is no widely accepted treatment for acute nonarteritic anterior ION. Fortunately, 40 percent of patients experience spontaneous improvement in visual acuity without treatment.
"For the nonarteritic form of ION, we just work up their vasculopathic risk factors and check their blood pressure, blood sugar and cholesterol," Dr. Lee notes. "We encourage them to eat a good diet, do a moderate amount of exercise and not to smoke. We ask about sleep apnea. They can also take an aspirin a day if there is no contraindication. This is for their general vasculopathic risk factors and not for the anterior ION per se."
If patients with nonarteritic ION are taking blood pressure medication, Dr. Shindler recommends that they take the medication in the morning. "Many people's blood pressure naturally drops at night, and we don't want it to drop too low," he explains.
"Any treatment for nonarteritic anterior ION is controversial," Dr. Miller says. "Most people would say there is no treatment. However, some ophthalmologists have used steroids, intravitreal triamcinolone acetonide injection or erythropoietin to treat nonarteritic ION, although they have not been definitively proven effective. There are a number of things in the pipeline that might help, but at present, the only mainstream treatments are nothing at all or oral steroids."
Researchers at the
Intravitreal triamcinolone acetonide injection has also shown promising results in a small number of patients. Recently, it was used to treat a patient with nonarteritic anterior ION in Korea.9 Fundus examination and measurements of the 65-year-old patient's best-corrected visual acuity and visual field were performed before the injection and after the injection at two weeks, and at one, three and six months. BCVA was 0.05 before the injection, 0.16 at two weeks, 0.3 at one month, and 0.4 at three months after the injection.
Large randomized controlled trials are needed to further assess the efficacy of these treatments. According to Dr. Pelak, it is difficult to study treatments for this condition because some people improve spontaneously. "Anecdotally, I have seen good results with intravitreal bevacizumab injection, but I have also seen two people who may have done worse after injection," she says. "However, that may have been the course that their condition was going to take without treatment. It would be impossible to know without a study."
Perioperative ION
Both anterior and posterior ION that occur after surgical procedures have been associated with low blood pressure, anemia, fluid balance, type of surgery (spine and cardiac), and the positioning of the patient in cases of prone-position spine surgery. "Although there have been a number of hypotheses, we still really don't know what causes perioperative ION, and it is unpredictable, unforeseeable and, unfortunately, not treatable," Dr. Lee says. "Many authors recommend normalizing their blood pressure, staging procedures if possible, and transfusing them if they are anemic, but basically there is no proven effective treatment."
Dr. Miller agrees: "For perioperative anterior ION, which is most common after cardiac surgery, there is no definitive treatment. Some people use steroids, and if it occurs after cardiac surgery, all you can do is make sure that any anemia is corrected as soon as possible and make sure that their blood pressure is good. The same issues hold true for the posterior perioperative ION that occurs after back surgery."
ION is the most common cause of perioperative vision loss. In a recent study of 126,666 surgical procedures, 17 patients experienced perioperative ION, an incidence rate of 0.013 percent.10 Unfortunately, the authors found that no hemodynamic variables differed significantly between the ION patients and the matched control patients.
A study conducted in
"It is a very frustrating situation, and that is why our laboratory and several others are continuing to study this condition," Dr. Miller says. "Our laboratory has developed animal models of nonarteritic anterior ION in rats, mice and monkeys. It is reproducible, and we are in the process of testing a variety of agents that might be of help in reversing visual loss and stabilizing vision in anterior ION."
1. Kupersmith MJ, Langer R, Mitnick H, et al. Visual performance in giant cell arteritis (temporal arteritis) after 1 year of therapy. Br J Ophthalmol 1999;83(7):796-801.
2. Giambene B, Sodi A, Sofi F, et al. Evaluation of traditional and emerging cardiovascular risk factors in patients with non-arteritic anterior ischemic optic neuropathy: A case-control study. Graefe's Arch Clin Exp Ophthalmol 2009;247(5):693-697.
3. Waller EA, Bendel RE, Kaplan J. Sleep disorders and the eye. Mayo Clin Proc 2008;83(11):1251-1261.
4. Nieto Enriquez J, Torres Blanch J, Badal Lafulla J. Ocular disease in sleep apnea. Med Clin (Barc) 2009;133(1):594-598.
5. Laties AM. Vision disorders and phosphodiesterase type 5 inhibitors: A review of the evidence to date. Drug Saf 2009;32(1):1-18.
6. Purvin V,
7. Hayreh SS,
8. Hayreh SS,
9. Sohn BJ, Chun BV, Kwon JY. The effect of an intravitreal triamcinolone acetonide injection for acute nonarteritic anterior ischemic optic neuropathy. Korean J Ophthalmol 2009;23(1):59-61.
10. Holy SE, Tsai JH, McAllister RK, Smith KH. Perioperative ischemic optic neuropathy: A case control analysis of 126,666 surgical procedures at a single institution. Anesthesiology 2009;110(2):246-253.
11. Shen Y, Drum M, Roth S. The prevalence of perioperative visual loss in the



