Refined techniques and instruments, both large and small, have made cataract surgery as safe and effective as it’s ever been. But cases complicated by brunescent lenses, pseudoexfoliation, cloudy corneas or inflammation can still occur.
“The only way to avoid the complications of cataract surgery is to not do surgery,” says Alan S. Crandall, MD, senior vice-chair, Department of Ophthalmology & Visual Sciences, Moran Eye Center, University of Utah. “The more surgery you do, the more significantly complications decrease. But they never go down to zero. If you tell me you’re experiencing no surgical complications, then you either have no idea what’s truly going on, or you’re not telling the truth.”
Highly experienced cataract surgeons say, fortunately, time-tested preventive measures and intraoperative solutions can help you avoid or get out of just about every jam.
In this report, these experts explain how to succeed when managing a multitude of challenging cataract cases.
Dense Cataracts
Most surgeons have come to expect an occasional brunescent lens that seems to defy all attempts at simple extraction.
“When you have a patient with a dense cataract, you often also have a small, wobbly lens, miotic pupil and weak zonules as well,” says Kevin M. Miller, MD, Kolokotrones Chair in Ophthalmology at the University of California, Los Angeles. “Such patients are usually very elderly, with deep-set orbits, small pupils and narrow lid fissures. The density of the nucleus makes it hard enough. But you also have to contend with these other factors.”
In some cases, Dr. Miller resorts to an extracapsular cataract extraction. “But I believe we should approach every patient as a phaco candidate,” he says. “In most cases, I proceed with phaco, knowing that I can always switch to a small-incision procedure, if necessary, after I start.” Dr. Miller uses a mydriatic agent to expand the patient’s pupil. “If that doesn’t work, a ring can be inserted to expand the pupil from 3 or 3.5 mm to 6.25 or 7 mm,” he says. “A ring is less traumatic than hooks. If the zonules are really loose, I can put in as many as five capsule retractors around the eye to stabilize the lens.”
 |
Dr. Miller reduces the duty cycle of his phaco unit by as much as 50 percent to reduce the odds of thermal injury, using 100-Hz, on-and-off power switching to create a pulse train that helps break up the lens without disrupting the fragile internal architecture of the patient’s eye.
“We can usually make progress on the lens, but it takes time,” he notes.
Kathryn M. Hatch, MD, Refractive Surgery Service Site Director at
Massachusetts Eye and Ear in Waltham, Massachusetts, says she likes to use the femtosecond laser to soften the cataract. “I can get to the leathery plate of the cataract and it makes the surgery for dense cataracts seem more routine,” she notes.
Dr. Hatch says the MiLoop can also be a useful technology for breaking up dense cataracts because it can “cheesewire” through the lens, segmenting it. “One possible severe complication with the MiLoop can develop when the instrument isn’t brought under the anterior capsule,” she says. “You don’t want to MiLoop the capsule. Let the instrument guide you around to the back of the lens where you can achieve a good hydrodissection, encircle the dense nucleus in the sagittal plane and safely fragment the lens.”
Dr. Crandall urges surgeons to use the MiLoop if they have any doubts about achieving a good outcome with phaco.
“The MiLoop might be your best choice for a black lens that’s as hard as a rock,” he says. “Other factors to consider are how close the lens is to the cornea, and whether the lens is cloudy, not just dense. You might have a lens with very loose zonules that’s floating around. A careful evaluation will tell you what to do. You may be pushed into doing an ECCE or a small-incision procedure, if you’ve been trained to do it.”
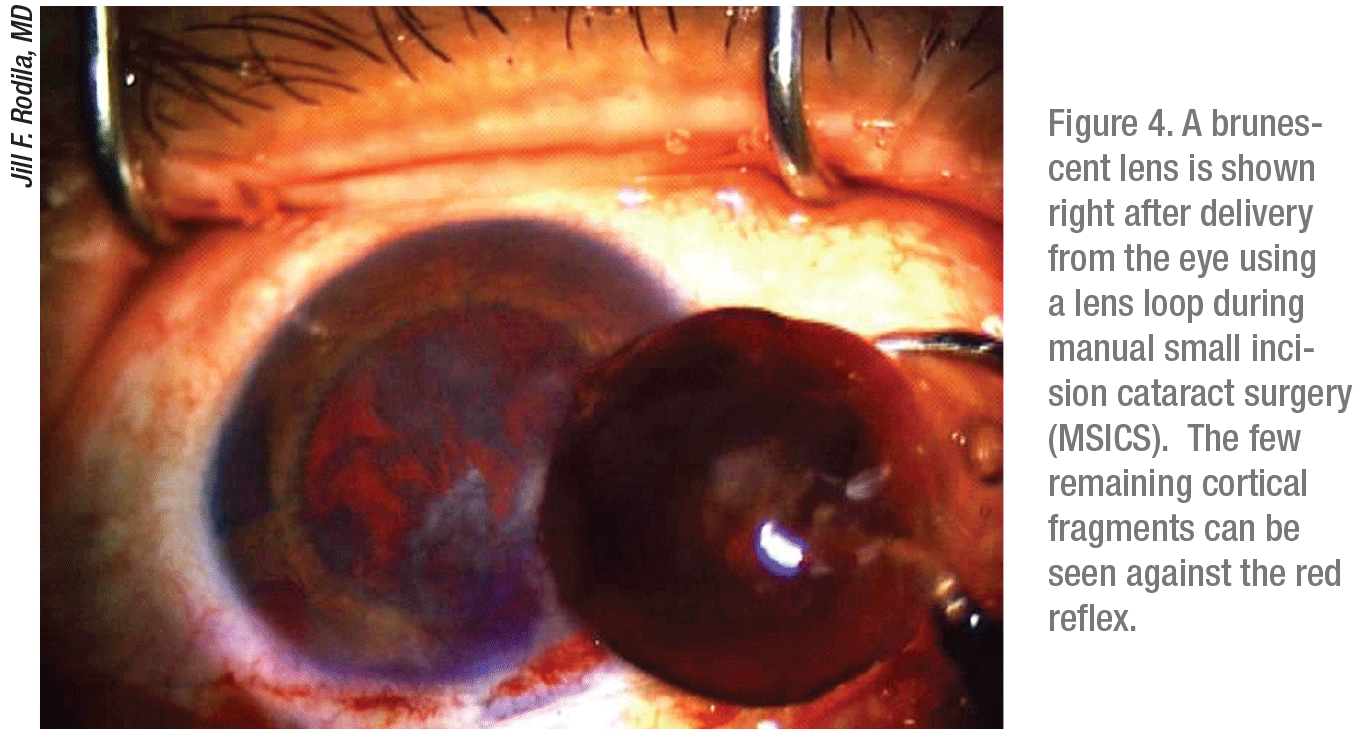
Before even starting her surgeries, Jill Rodila, MD, a surgeon at Aker Kasten Eye Center in Boca Raton, Florida, peers through her slit lamp and grades the appearance of all lenses. “If I see a cataract with a high degree of brunescence, I prepare to use more phaco power,” she says. “I use extra viscoelastic, and I prefer EndoCoat for protecting the corneal endothelium if there’s a densely brunescent lens or a low endothelial cell count.” For extremely dense lenses, Dr. Rodila turns to sutureless extracapsular cataract surgery (manual small incision cataract surgery or MSICS). “I can get the lens out without being harsh on the cornea,” she notes. “It can be difficult to crack a very hard lens all the way when you’re using phaco.”
 |
One of her biggest concerns arises when a leathery posterior cortex seems impossible to break through or mobilize. “It’s very important to get a deep enough groove in the lens right from the start,” she says. “I want to split the lens completely in half, if possible. In situations like this, you might need an additional chopping instrument that’s smooth enough to avoid breaking the posterior capsule but also has a sharp edge that you can safely slice through the lens with.
“Here’s another important point,” Dr. Rodila adds. “At the end of a case, you may see a remaining piece of dense nuclear material that takes a lot of phaco power to remove. Sometimes, you may be dealing with a fragile cornea, and you have to keep the tip more posterior. When doing so, remember that the posterior capsule can be right behind the phaco tip. The rush of fluid into the phaco tip can cause the capsule to rush to the tip as well. It’s wise to use a second instrument posterior to the phaco tip to protect the capsule in case it wants to bounce up into the tip.”
Managing Surgical Risks
Experts say the best weapon to use against a dense lens or many other challenges that may await you inside an eye is proactive preparation.
“Look for signs and symptoms that the cataract is likely to be difficult,” says Dr. Crandall. “Look for issues such as pseudoexfoliation on the capsule or a history of trauma, whether the patient remembers it or not. Look carefully for asymmetry in the depth of the chamber. Look at the patient’s IOP. If it’s low, that could be because of serious retinal problems, including a detachment. You may need to turn this case over to a retina specialist to avoid massive problems if the patient has a retinal detachment.”
Dr. Miller says it’s critical to assess the whole patient preop.
“It’s all about the comorbidities of the patient,” he says. “They have a cataract and they typically have all sorts of other problems. We had a deaf and blind patient recently who required the use of general anesthesia. We had to tape the forehead of a patient with chronic obstructive pulmonary disease to the gurney so that his persistent coughing would not disrupt surgery. We operate on patients with diabetes first thing in the morning so they don’t have to fast all day, risking hypoglycemia. We use lots of pillows and towels to maintain comfort and proper surgical position for patients with bad backs or other orthopedic issues. Some patients have conditions—such as juvenile rheumatoid arthritis, a history of vitritis, extensive uveitis and cystoid macular edema—that tell us they will experience intense inflammation after surgery. So we have to plan for that.”
Pupil, Iris and Zonule Issues
Dr. Hatch says one of her biggest challenges is often a small pupil. “You can pretreat patients with cyclopentolate 1% or atropine for a few days before the surgery,” she notes. “During surgery, you can add phenylephrine and ketorolac intraocular solution 1%/ 0.3% (Omidria, Omeros), if it’s not contraindicated.”
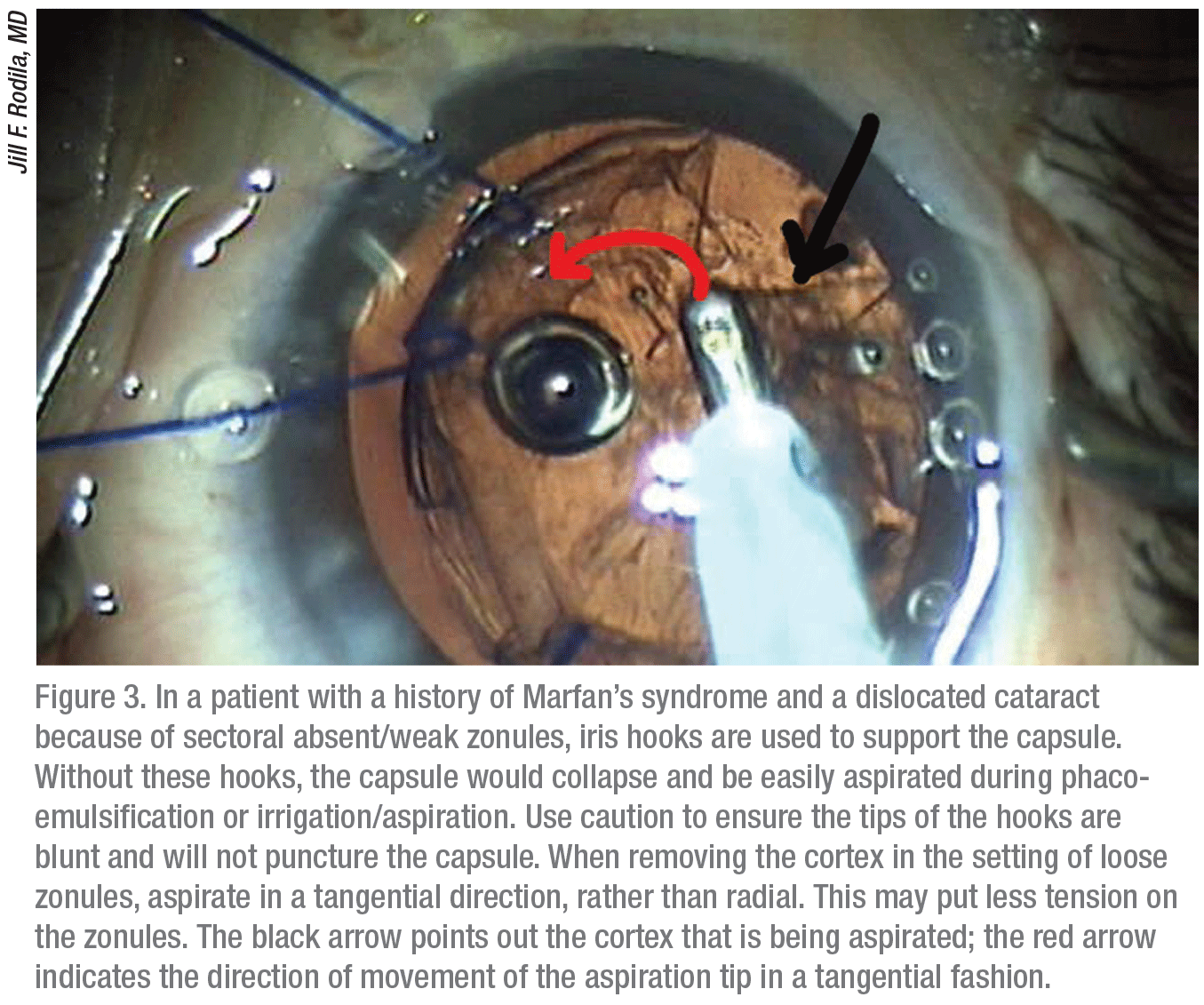
Dr. Rodila watches for pseudoexfoliation and history of trauma that may be associated with a case of loose zonules in a particular patient. “You can tap the slit lamp to see if the lens moves a little,” she says. “If the lens is loose when you examine it, you know there will be a risk. Look also for dislocation of the lens.”
Dr. Rodila confirms loose zonules when doing an anterior capsulotomy she typically encounters less tension when piercing the anterior capsule. When she makes her anterior capsulorhexis, she may discover striae in the capsule. “You know then that you’re definitely dealing with loose zonules,” she notes. “I proceed with the case very gently. And I try to get a good hydrodissection.”
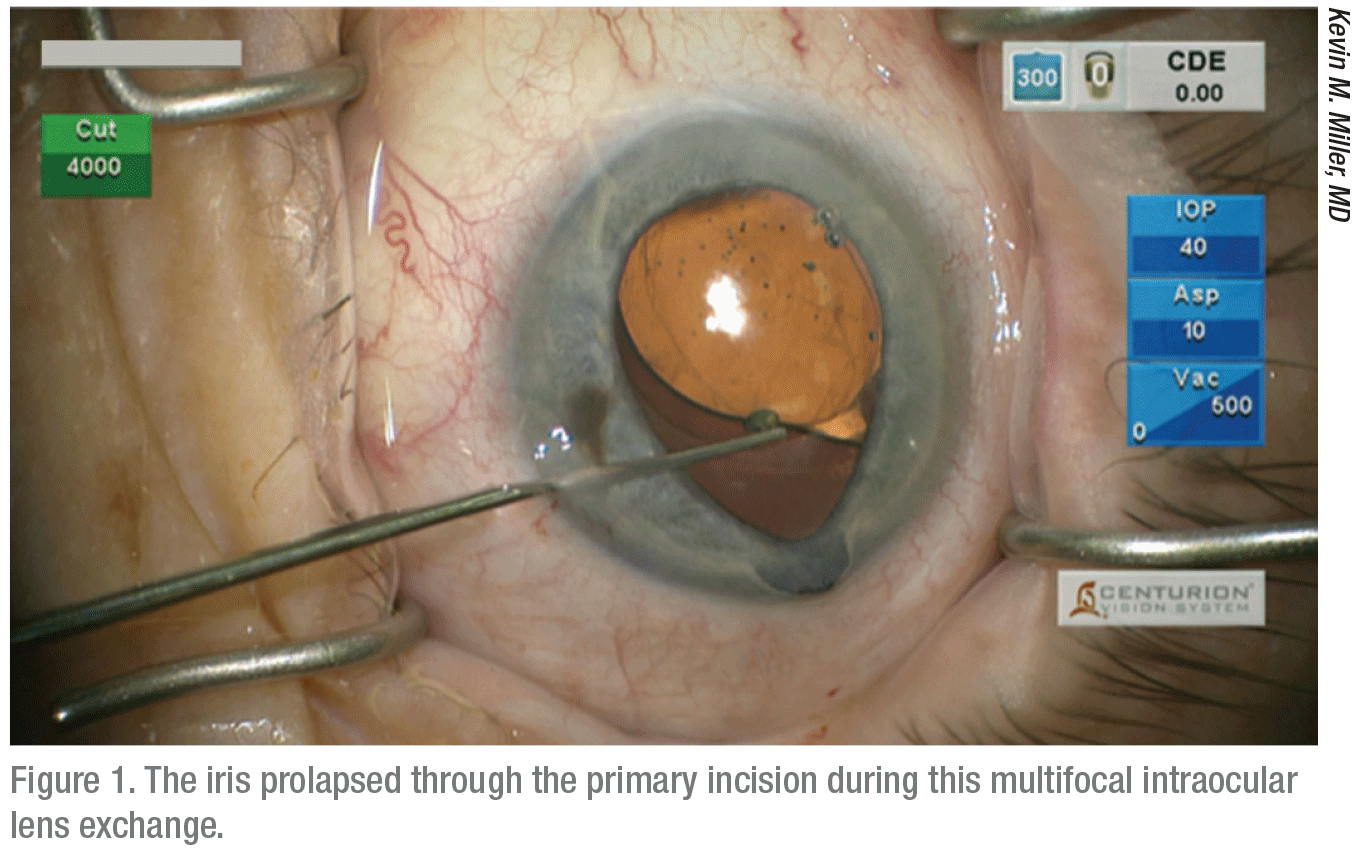
Dr. Miller says seemingly minor techniques can have disastrous effects. “One of the worst complications is damaging a prolapsed iris,” he explains. “It’s pretty easy to do, yet damaged irises are unforgiving.” The damage can occur after the pupil gets stretched from the use of hooks to keep it open, or when the pupil sphincter is torn by any means. “The prolapse can develop during hydrodissection,” he says. “[When this problem occurs], most often, it occurs when the phaco incision is made 1 mm long instead of 1.75 or 2 mm, and an excessive amount of viscoelastic is injected. The pressure of the visco will cause the iris to knuckle up and prolapse through the incision.
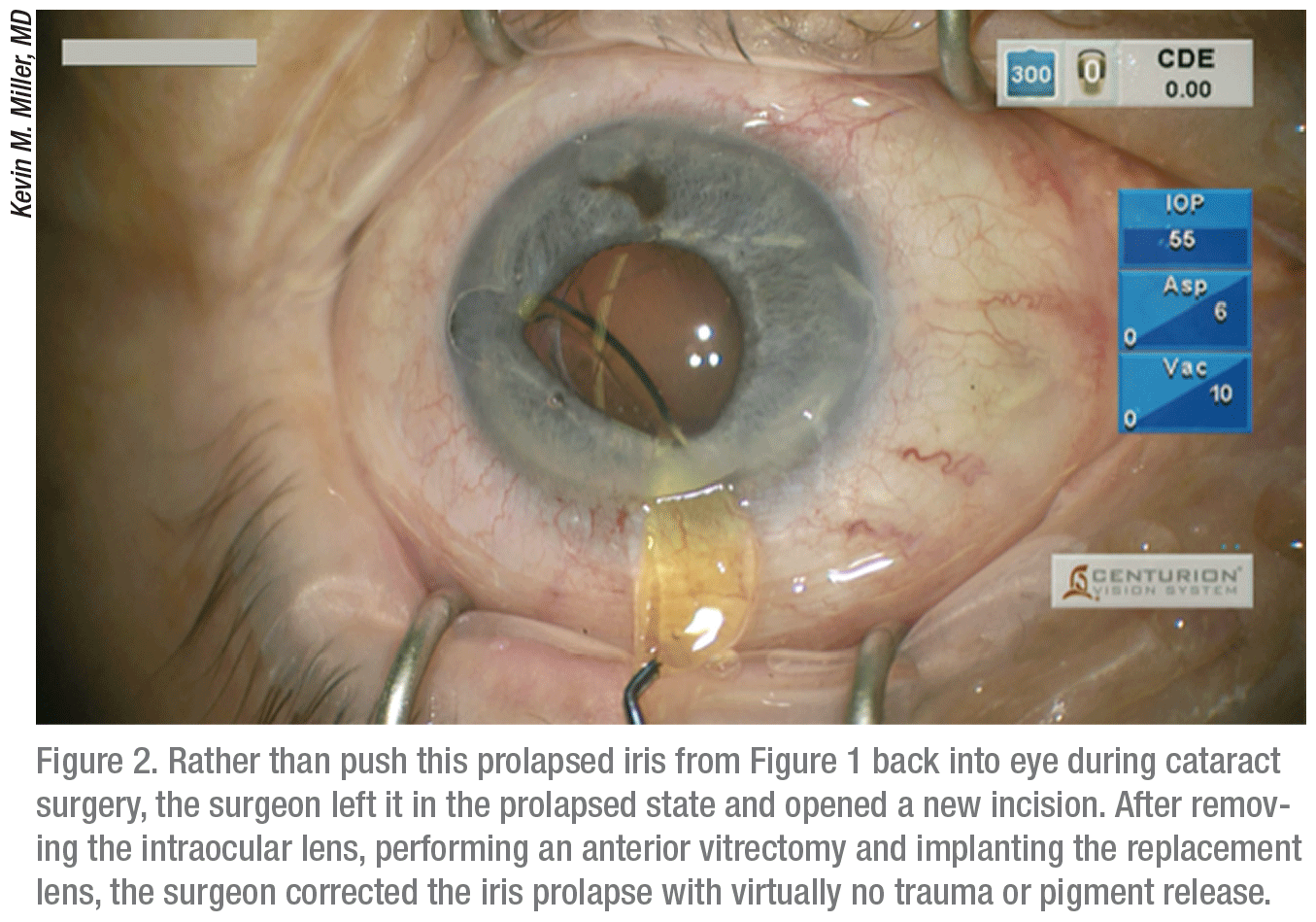
“Once the iris is outside of the eye, you have a small knuckle of visco trapped inside of it, so it’s hard to get it back in,” he says. “You’ll shred the iris if you try to poke it back inside the eye, causing significant cosmetic and functional damage that will affect appearance in light-colored eyes and vision postoperatively. In such a case, you need to evacuate the viscoelastic beneath the iris and the iris will go back in. You can continue the hydrodissection after it’s inside. If it doesn’t go in, just leave the iris outside of the eye until you’ve completed surgery through a separate incision. You can reduce the prolapse by lowering IOP later on and injecting a miotic.”
To avoid this problem? “Make sure your incision is long enough so the iris doesn’t jump out,” Dr. Miller says.
Surgeons also recommend that you avoid making your incision too posterior, which can incise the conjunctiva, causing it to billow and possibly hinder visualization of the case.
Maintaining Visualization
Vision of the inside of the eye during surgery is often taken for granted—until you start to lose it.
“We may encounter this if the cornea becomes hydrated or cloudy during surgery,” Dr. Miller says. “We can stain the capsule with some trypan blue solution to help with this situation. Keeping the cornea clear is always critical.”
Positioning of the patient is also critical. “We had one patient who suffered a neck fracture, and his chin was stuck down,” he recalls. “We had to prop him up just about 90 degrees, almost hanging him by his feet, so that we could get the correct view, using a lid speculum to maximize exposure.”
Sometimes, Dr. Miller adds, he will get a patient with deep-set eyes that will pool up with fluid. “We do our best to dry out the eye with wicks, but to some extent, you find yourself operating underwater.”
Corneal Scars and Abrasions
Scars on the cornea can also create a problem. “When we see a scar,” says Dr. Miller, “we’ll roll the eye around to see where it’s clear, and then move the eye to that area so that we can do the surgery through a relatively clear window.”
Dr. Rodila says there are no easy answers when confronting this issue. “I rely on past experience in the presence of a cloudy or scarred cornea,” she explains. “You have to stay calm and confident when working under scarred areas. You need to trust your sense of feel, knowing where your hands are, trusting your proprioception.” She recommends using trypan blue solution to stain the anterior capsule to get the best visualization possible, especially if you can’t get a good red reflex.
Dr. Hatch, a corneal specialist, says she’s grown accustomed to scars and corneal opacities that can challenge you during surgery. “These include a variety of problems, ranging from corneal dystrophy opacities to scars resulting from prior refractive procedures, such as LASIK or RK,” she says.
“If I find corneal issues, specifically anterior basement membrane dystrophy, within the central 4 mm area and these issues are affecting biometry measurements, I may conclude that a superficial keratectomy is warranted,” she continues. “Afterward, patients heal for four to six weeks, and repeat biometry measurements are taken prior to cataract surgery.”
Abrasions can also be caused by draping the eye too tightly before surgery, when the plastic drape abrades the cornea.
“You may need to re-drape, making sure the cut ends of the drape are away from the limbus and cornea,” says Dr. Miller. “Another common cause of abrasions during surgery is when a surgeon pokes around to find the paracentesis.”
The preventive measure? “Put in a dye when making the paracentesis so that you can see it,” says Dr. Miller. “Some people will enter the cornea through a peripheral blood vessel to mark the incision site with a minor bleed.”
 |
 |
Dealing with Inflammation
Dr. Hatch notes that she would never perform cataract surgery in the presence of inflammation. “If the patient has chronic uveitis and needs cataract surgery, I wait until the patient’s eye isn’t actively inflamed,” she says. “Such a patient will have synechiae and small pupils.
“I give a subconjunctival dexamethasone injection or may rely on the dissolvable implant, Ozurdex (Allergan),” she adds. “Some surgeons will do intracameral injections in conjunction with a steroid and subcameral antibiotic injections along with a steroid and nonsteroidal drop. Taper over four weeks.”
Wound Burns
Dr. Crandall says wound burns are rare but very serious. “One should be aware that different viscoelastics can increase the risk for wound burns,” he says. “It is critical to understand dispersive versus cohesive viscoelastics and to clear space so that there is flow in and flow out of the eye. The tip should not be clogged, because the temperature will immediately cause a burn.”
“Phaco burns are very bad,” adds Dr. Miller. “The cornea coagulates quickly and becomes like hard plastic. You end up needing five to seven sutures to close a 2.2-to-3-mm opening.”
Dr. Miller says phaco burns frequently happen in tight incisions. “Besides developing when the tip has been occluded, a burn can occur when a tight incision crimps the sleeve of the phaco tip and that squeezes against the tip, cutting off fluid flow and causing frictional heat to generate,” he says. “The phaco tip continues to vibrate, generating extreme heat.”
Surgeons can easily avoid this problem, however. “The bottom line is that phaco burns occur in tight incisions,” says Dr. Miller. “The most important thing you can do is ensure that you’re not making incisions that are too tight. Make the incision wide enough to avoid this problem.”
Meeting Expectations
Recognizing that a variety of different challenges can arise during cataract surgery, these surgeons recommend keeping all of the strategies they discussed in mind.
“Above all other things, I would say it’s important to know what you’re getting into and to communicate this honestly to your patient,” says Dr. Crandall. “When it’s not going to be easy, tell the patient it is not going to be easy. You need to be practical—not only in meeting surgical challenges, but also in making sure the patient knows what both of you are up against.” REVIEW



