Diagnosing a patient withunexplained ocular pain can be time-consuming and difficult. Taking an anatomic approach and excluding causes along the way can aid in the diagnosis.
"Patients with pain are underserved. Eye pain is always diagnosable, but you have to think anatomically," says Kathleen Digre, MD, a neuro-ophthalmologist in practice at the
Kimberly Cockerham, MD, agrees. She notes that there are not enough neuro-ophthalmologists to treat the number of patients with unexplained ocular pain. "A lot of general ophthalmologists are having to take on the diagnosis and treatment of these patients because it is difficult to refer," says Dr. Cockerham, adjunct associate clinical professor at
The Surface of the Eye
When a patient presents with ocular pain and few or no other symptoms, the first step in diagnosis is getting a history and examining the surface of the eye and the patient's face for clues. "The anterior surface of the cornea has some of the densest nerves in the whole body," says Daniel Durrie, MD, owner of Durrie Vision in Overland Park, Kan.
"Anything that happens on the cornea that disrupts the epithelium or stimulates those nerves can cause significant pain, so the first thing you have to do is get a history of what they were doing when they first noticed pain. Were they sweeping, working on metal or riding on a motorcycle when the pain started? The history is extremely critical for diagnosing a foreign body or conditions that occur after being struck in the eye."
The history is also important for diagnosing recurrent erosion syndrome, which is most painful when a patient wakes up and then improves throughout the day. "This can be diagnosed almost from the history alone, because the patient reports that the eye waters and he or she feels like something is in the eye in the morning, and both symptoms get better as the day goes on," Dr. Durrie says.
Patients with shingles who have had lesions around their lids and corneas can experience eye pain even years after the acute inflammation has resolved. "History can diagnose this condition, too. Sometimes, in an early episode of shingles, the only symptom is pain that seems to be out of proportion to what you see," Dr. Durrie adds.
Dr. Cockerham, who is in private practice in
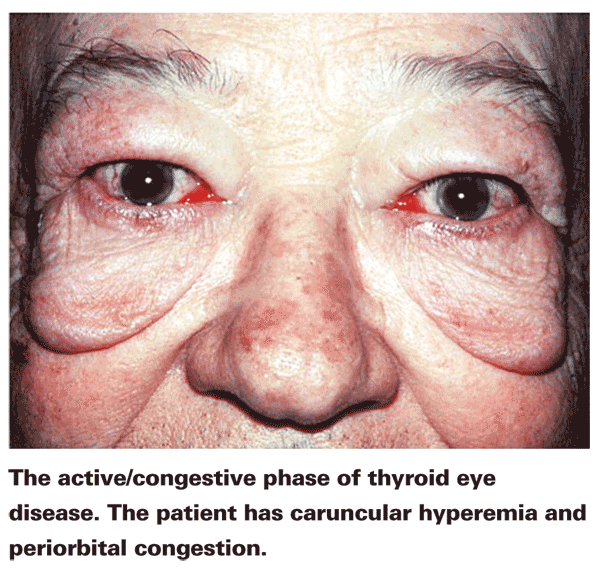
Examining the appearance of the vessels in the eye can also aid in the diagnosis. Patients with a carotid-cavernous fistula can present with pain and bulging of the eye due to dilatation of the veins draining the eye. "Inflamed vessels, particularly over the muscles, could be associated with a myositis or thyroid eye disease," adds Dr. Cockerham.
According to Mark Packer, MD, the most common ocular finding accompanying pain is dry eye. "These patients may have a poor or partial blink, and they may have eyelid abnormalities," says Dr. Packer, who is a clinical associate professor of ophthalmology at Oregon Health and
Dr. Cockerham notes that dry eye is a bilaterally symmetric process. If a patient's Schirmer test measurement is 2 in one eye and 10 or 20 in the other, it could be indicative of a tumor of the lacrimal gland or in the brain that is affecting the complex neural innervations pathway of the lacrimal gland.
Bacterial, viral and fungal keratitis can also cause pain; however, these patients typically have accompanying symptoms. "Acanthamoeba keratitis can be very painful and is often misdiagnosed as a bacterial or viral keratitis," Dr. Packer says. "If it is mistreated with steroids, it can be made worse. This condition is typically seen in contact lens wearers who have used tap water to rinse their contacts, and confocal microscopy is needed to diagnose Acanthamoeba infection."
Intraocular Causes
If a diagnosis cannot be made after taking the history and examining the face and surface of the eye, intraocular causes, such as glaucoma, should be considered. "Then, there are conditions that cause intermittent pain, where the eye exam is actually normal but only at the time you are examining the patient," says Andrew Lee, MD, chair of ophthalmology at the Methodist Hospital and professor of ophthalmology at Weill Cornell College of Medicine in Houston. These conditions include uveitis and intermittent angle-closure glaucoma."
Another intraocular cause of pain is Posner-Schlossman syndrome. "Out of the blue, these people de-velop a high pressure in the eye that is due to inflammation of the trabecular meshwork. When you look at them, the eye looks quiet, and there is no redness, but the pressure is really high. They respond to steroids immediately," Dr. Packer explains.
Another inflammatory condition that can cause eye pain is giant cell arteritis, which is most commonly found in elderly patients. "To look for inflammation, we can do a sedimentation rate and a C-reactive protein," says Dr. Lee. Treatment for giant cell arteritis includes oral steroids. If left untreated, these patients could experience visual loss or, rarely, cardiac events or a stroke.
Another condition to consider is pituitary adenoma. According to Dr. Cockerham, if a patient has a tumor on his pituitary gland and hits his head or takes a large dose of aspirin or other blood thinners, the tumor can start to bleed into itself (pituitary apoplexy). "These patients may present with pain initially without the other classic symptoms of double vision and bitemporal visual field defect," she explains.
Headache Syndromes
Headache syndromes, while not an eye condition, are a significant source of eye pain. "Many headache syndromes can be diagnosed just by history, and criteria for diagnosis were developed at a consensus conference of the International Headache Society, Dr. Lee explains. "This society defines the criteria for conditions that can cause eye pain but are really headache syndromes. The three most common are migraine, tension and cluster. They can be associated with eye pain because the pain itself is in the eye, even though the pain is not from the eye."
According to Dr. Digre, migraine is the most common disorder, affecting 20 percent of women and 10 percent of men. Migraines can cause pain in the eye or orbit, and they can occur with or without aura. "These patients are light sensitive, may be sound sensitive, may have throbbing pain, and may have some nausea. Then, they have a totally normal eye exam," she says.
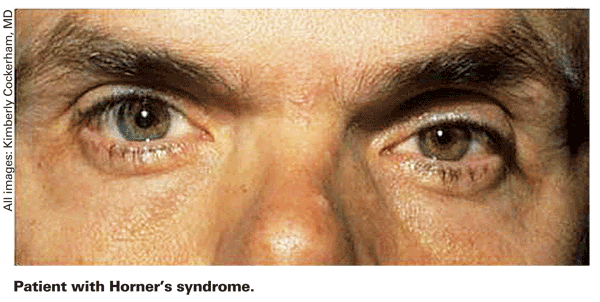
Cluster headache can occur directly over the eye and is more common in men. "You may see an associated Horner's syndrome during the attack and sometimes even in between attacks. These patients present with excruciating eye pain, tearing, lacrimation, rhinorrhea, stuffiness of the nose, possibly swelling around the lid, and maybe some conjunctival redness," she adds.
Another headache disorder, hemicrania and paroxysmal hemicrania, is most often seen in middle-aged women. Attacks typically occur five to 40 times per day, and each attack lasts between two and 45 minutes. Hemicrania continua and chronic paroxysmal hemicrania can cause continuous pain around the face and eye. Fortunately, these disorders can be effectively treated with indomethacin.
Another, less common headache disorder is short-lasting, unilateral, neuralgiform headache attacks with conjunctival injection and tearing (SUNCT). "This rare condition is seen mostly in men, but can occur in women. It lasts seconds and goes away, and it can occur 100 or 150 times in a day. You can even have it without the conjunctival injection and tearing, and that's called SUNA," Dr. Digre explains.
During the initial exam, Dr. Cockerham asks patients to point to the location of the pain. "Sometimes, with unexplained pain, they will point right at their trochlea. Trochleitis is a condition where the trochlea becomes inflamed," she says. Trochleitis is characterized by localized swelling, tenderness and severe pain superomedially. It has been associated with triggering or worsening migraine headaches in patients with pre-existing migraines.1
"Then, there are other patients who don't meet the criteria for a specific headache diagnosis according to IHS criteria, who have normal eye examinations and don't have any other evidence for an intraocular cause. Those patients sometimes have an intraorbital cause, such as myositis or orbital inflammatory pseudotumor. These patients typically have severe pain that is made worse with eye movement," Dr. Lee explains. In addition, some patients with optic neuritis can present with the eye pain before the typical vision loss.
Imaging studies, such as a CT scan, MRI, or ultrasound can confirm the presence of inflammation. According to Dr. Lee, treatment includes nonsteroidals or a short course of steroids.
Other Neurologic Causes
The trigeminal nerve provides sensation to the eye, face, and most of the head. "Some patients who have trigeminal pain or neuropathic pain feel it in their eyes. The greater occipital nerve can also be involved and radiate pain to the eye," Dr. Lee explains.
Dr. Digre adds, "The trigeminal system, whether it is trigeminal neuralgia or trigeminal activation from migraine, can cause a lot of problems with pain in the eye, and there won't be any ophthalmic findings. Everything will look completely normal. I see a lot of eye pain from trigeminal nerve disorders; it's pretty common. You have to think about it every time you see a patient."
Dr. Digre explains that the eyes are innervated by the first division of the trigeminal system, and this same division is also responsible for all of the pain in the cranial cavity, including the dural vessels and the meninges that cover the brain. "People can have something going on in their heads that manifests itself as pain in the eye, she says. "This system is very complex because it has other nuclei that even go down into the cervical system—C1 and C2. If there is a problem even in C1 or C2, I've seen people present with eye pain when they actually had a problem at the cervical cranial junction. One woman had pannus of her odontoid that was compressing her C1-2 region, and she presented with eye pain."

A 2009 report by Perry Rosenthal, MD, and colleagues described patients who have corneal pain suggestive of dry eye, with no clinical signs.2 The authors suggest that this is a disease in its own right. "It's a trigeminal disorder. It isn't just dry eye because when you do dry eye testing, these patients don't have the results that go along with it. I think this condition is really underdiagnosed. The nerve endings are extra sensitive, and things like zoster and diabetes can cause it. Dr. Rosenthal has even diagnosed this condition in refractive surgery patients," Dr. Digre says.
Researchers in
"It seems to be related to abnormal nerve re-growth, but I've done more than 20,000 LASIK procedures, and I have never seen it," Dr. Durrie says.
Although isolated ocular pain can be difficult to diagnose, it is often not serious and is easily treated. "If you have a normal eye exam, your history doesn't suggest any defined headache syndrome, and there is no other finding, the chance of it being something bad is extremely low," Dr. Lee says. "It is extremely unlikely that someone who has an isolated eye pain would have something serious, except elderly people who might have giant cell arteritis or patients who have neuropathic pain. Those are the things that ophthalmologists need to worry about."
1. Yanguela J, Pareja JA, Lopez N, et al. Trochleitis and migraine headache. Neurology 2002;58:802-805.
2. Rosenthal P, Baran I, Jacobs DS. Corneal pain without stain: Is it real? Ocul Surf 2009;7(1):28-40.
3. Tuisku IS, Lindbohm N,



