—Walter Bethke, Editor in Chief
A Tough Road
In 1995, the National Eye Institute hosted an industry workshop called Clinical Trials in Dry Eye. Looking back at the meeting report,1 it’s remarkable that so little emphasis was placed on symptoms of the disease: There was only a brief mention of a dry-eye questionnaire for symptom assessment.2 Despite this, the report did recognize the lack of correlation between diagnostic measures and symptomatic assessments, and promoted a general rubric where both signs and symptoms were part of clinical assessment of new therapies.
In hindsight, this might be considered a case of one step up, two steps back: Recognition of the importance of the disconnect between signs and symptoms is a key to understanding dry eye, but many of the studies that followed were based upon a near-impossible hurdle of co-primary endpoints. In addition, the measurement of symptoms turns out to be much more nuanced than was appreciated at the time, and an evaluation of the McMonnies symptom questionnaire showed that the design of the test failed a Rasch analysis of univariate assessments.3 This analysis tests the statistical validity of using summated scores of a specific series of questions as a reliable metric of a condition or variable. Symptom questionnaires have been refined since then, with an emphasis on a few select questions focusing on subjects reporting symptoms as they occurred instead of retrospectively.
In the decade that followed, a host of compounds were tested as potential dry-eye therapies,4-7 but only one treatment was approved, the cyclosporine ophthalmic emulsion Restasis (Allergan). In this case, the approval used a narrow indication, improvement of tear production, as the clinical endpoint rather than the co-primary endpoints of other trials. It’s for this reason that the Restasis label indication is for increasing tear production in patients whose tear production is presumed to be suppressed due to ocular inflammation associated with keratoconjunctivitis sicca.
Progress is Made
Drug developers trying to devise treatments for dry eye were stymied by the unusually large degree of patient heterogeneity that is characteristic of the condition. Some patients have severe symptoms but few or none of the physical manifestations of disease, such as increased corneal staining, reduced Schirmer’s scores or altered tear-film breakup times. In addition, significant variability from environmental factors such as air quality and humidity, and lifestyle factors such as computer use and medications, means that day to day, dry eye can be severe, mild or totally absent.
This kind of variability can be problematic in the setting of a clinical trial, even with large patient populations.
We can get a clue to the ways this problem has been addressed by comparing clinical trial protocols from 2004 to those in 2016. For a 2004 study,4 the inclusion criteria were “non-Sjögren’s dry eye with symptoms for more than six months, and intermittent or regular artificial tear use for three months.” The exclusion criteria were equally brief—patients could not have undergone LASIK, punctal occlusion or cauterization. Despite this, most patients in early studies were the most severe dry-eye sufferers, and tended to be those less responsive to any treatment. In contrast, the most recent trials have focused on either a sign or a symptom as a primary endpoint, and they include inclusion criteria of a minimal level of current disease severity (such as corneal fluorescein staining score of ≥ 2) to establish a sufficient level of disease for therapeutic assessment. In addition, tools such as the controlled adverse environment, or CAE, have provided an additional inclusion tool by identifying those dry-eye patients most likely to experience an exacerbation of their disease under conditions of environmental stress.8,9
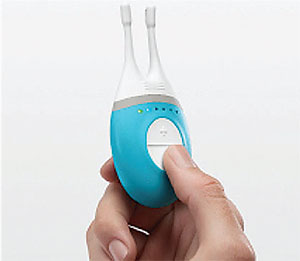 |
| The intranasal tear neuro-stimulator from Allergan is showing potential in trials. |
Another approach to minimizing variation in dry-eye trials is the use of adverse environments such as the CAE. The adverse environmental conditions mimic those that exacerbate dry eye and provide enhanced efficacy measures by comparing patient responses to CAE stress before and after a treatment regimen. Because dry eye is a result of a combination of physiological factors and the environmental milieu, disease variability can be reduced if parameters such as temperature and humidity are controlled. Other types of visual stress, such as computer work and reading,11 have been incorporated into experimental clinical trial designs, and these show promise as a means of establishing clinically significant therapeutic benefits of an intervention.
Recent trial results show how these new approaches can impact clinical success. One recent Phase II study used CAE-based inclusion criteria to enrich the population with patients who had measurable, reproducible signs and symptoms of dry eye. The study demonstrated significant, dose-dependent improvements in corneal staining and in the visual function subset of the ocular surface disease index,12 and thus confirmed the benefit of CAE-based inclusion criteria. A subsequent Phase III trial replicated the staining results from Phase II. Collectively, these studies demonstrated a remarkable degree of reproducibility, a key result that was particularly encouraging for an indication such as dry eye, which is infamous for its variable nature.
Peering into the Pipeline
One drug is rarely the best drug for everyone, especially with a heterogeneous condition such as dry eye. Fortunately, several other compounds are now poised to bring their therapeutic benefits to the market. Many of these treatments are based upon distinct mechanisms of action, promising a future where ophthalmologists may be able to provide their patients with an individualized selection of suitable treatments. Different MOAs for a selection of agents also provide the potential of a future combination therapy for patients with severe dry eye. As in other diseases, it’s clear that dry eye has many phenotypical subsets that have yet to be teased out, and widening the choices for treatment is the best way to successfully treat the most patients.
Some new therapies are devices, not topical medications. The intranasal tear neuro-stimulator system (OD-01 Intranasal Device, Allergan) is a device that increases tear production with a mild nasal electrical stimulus. The stimulator has demonstrated increased Schirmer’s scores and reductions in corneal staining in open-label trials,13 and is currently awaiting FDA review.
Milder forms of dry eye are typically treated with artificial tears, and several programs are exploring improvements in these formulations that may provide relief comparable to anti-inflammatories. Many of these compounds include chemically modified versions of hyaluronic acid,14 with the primary goal of providing a longer lasting symptomatic relief that reduces the need for frequent dosing.
One of the new potential dry-eye therapeutics, SkQ1 (Mitotech, Luxembourg), has a mechanism quite different from other therapeutics: It’s a free-radical scavenger that acts by reducing oxidative stress, including the oxidative stress associated with inflammation. A recently published Phase II study15 focused on therapeutic effects before and after CAE exposure, and showed that the drug provided significant improvements in both corneal staining and in multiple measures of ocular discomfort.
A second therapeutic that has completed Phase II is RGN-259 (ReGenTree; Princeton, N.J.), an ophthalmic solution containing 0.1% thymosin β4, an endogenous, pleiotropic peptide that acts to resolve inflammatory events both by acting on cell migration and on cytokine signaling. The trial used a CAE challenge to screen and enroll an enriched patient population and measure a patient’s ability to withstand an acute adverse environmental challenge to the ocular surface.16 Results from the study included significant improvement in discomfort and central corneal staining. A Phase III study for RGN-259 is in progress.
Another new potential treatment that has reached the Phase III development stage is Tavilermide (Mimetogen Pharmaceuticals, Montreal), a TrkA receptor agonist that can mimic or augment the effects of nerve growth factor. NGF is a major positive regulator of goblet cell growth, conjunctival and goblet cell mucin expression, and mucin secretion. In Phase II trials, Tavilermide significantly improved total corneal fluorescein staining when assessed as the change from pre- to post-exposure in the CAE chamber.10 Tavilermide also showed significant improvements in diary-reported ocular dryness, and ocular discomfort was significantly improved in the high-dose treatment group (p=0.014). These results were encouraging, and despite missing the primary endpoints, the drug is now in Phase III development.
A handful of other compounds under development include CyclASol (Novaliq, Germany), a cyclosporine that employs a proprietary formulation designed to optimize drug delivery; BRM 421 (Brim Biotechnology, Taiwan), a neurotrophic peptide that stimulates wound healing and corneal repair; TOP1630 (Topivert, UK), a kinase inhibitor that blocks inflammatory signaling; and KPI-121 (Kala Pharmaceuticals; Waltham, Mass.) a novel formulation of loteprednol etabonate.
These examples of potential dry-eye therapies demonstrate that there is an assortment of molecular targets that may provide a pathway to dry-eye relief. Perhaps one of the most encouraging aspects of the near future of dry-eye treatments is that, with a refined roadmap to clinical success and a growing number of candidate therapies, each with a unique approach to dry eye, the odds increase that all of our patients will be able to find a treatment best-suited to them. REVIEW
Dr. Abelson is a clinical professor of ophthalmology at Harvard Medical School. Mr. Ousler is vice president for dry eye at the research and consulting firm Ora Inc. Dr. McLaughlin is a medical writer at Ora. Dr. Hollander is chief medical officer at Ora, and assistant clinical professor of ophthalmology at the Jules Stein Eye Institute at the University of California, Los Angeles.
1. Lemp MA. Report of the National Eye Institute Industry workshop on Clinical Trials in Dry Eyes. CLAO J 1995;21:4:221.
2. McMonnies CW, Ho A. Patient history in screening for dry eye conditions. J Amer Optom Assoc1987;58:296-301.
3. Gothwal VK, Pesudovs K, Wright TA, McMonnies CW. McMonnies questionnaire: Enhancing screening for dry eye syndromes with Rasch analysis. Invest Ophthalmol Vis Sci 2010;51:3:1401-7.
4. ClinicalTrials.gov Identifier: NCT00037661 “INS365 Ophthalmic Solution in a Controlled AE in Patients with non-Sjogren’s Dry Eye” Sponsor: Merck Sharp & Dohme Corp. First received: May 18, 2002. Last updated: October 1, 2015.
5. Sall K, Stevenson OD, Mundorf TK, Reis BL. Two multicenter, randomized studies of the efficacy and safety of cyclosporine ophthalmic emulsion in moderate to severe dry eye disease. CsA Phase 3 Study Group. Ophthalmology 2000;107:4:631-9.
6. ClinicalTrials.gov Identifier: NCT00198536 “Efficacy and Safety Study for Ecabet Ophthalmic Solution for Treating Dry Eye Syndrome,” Sponsor: Bausch & Lomb Incorporated. First received: September 13, 2005. Last updated: March 13, 2013.
7. ClinicalTrials.gov Identifier: NCT00201981 “Study of Rebamipide Eye Drops to Treat Dry Eye,” Sponsor: Otsuka Pharmaceutical Development & Commercialization, Inc. First received: September 12, 2005. Last updated: January 4, 2008.
8. Abelson R, Lane KJ, Rodriguez J, Johnston P, Angjeli E, Ousler G, Montgomery D. A single-center study evaluating the effect of the controlled adverse environment (CAE) model on tear film stability. Clin Ophthalmol 2012;6:1865-72.
9. González-García MJ, González-Sáiz A, de la Fuente B, et al. Exposure to a controlled adverse environment impairs the ocular surface of subjects with minimally symptomatic dry eye. Invest Ophthalmol Vis Sci 2007;48:9:4026-32.
10. Meerovitch K, Torkildsen G, Lonsdale J, Goldfarb H, Lama T, Cumberlidge G, Ousler GW 3rd. Safety and efficacy of MIM-D3 ophthalmic solutions in a randomized, placebo-controlled Phase 2 clinical trial in patients with dry eye. Clin Ophthalmol 2013;7:1275-85.
11. Ousler GW 3rd, Rodriguez JD, Smith LM, Lane KJ, Heckley C, Angjeli E, Abelson MB. Optimizing Reading Tests for Dry Eye Disease. Cornea 2015;34:8:917-21.
12. Semba CP, Torkildsen GL, Lonsdale JD, et al. A Phase II randomized, double-masked, placebo-controlled study of a novel integrin antagonist (SAR 1118) for the treatment of dry eye. Am J Ophthalmol 2012;153:1050-1060.
13. Friedman NJ, Butron K, Robledo N, et al. A nonrandomized, open-label study to evaluate the effect of nasal stimulation on tear production in subjects with dry eye disease. Clin Ophthalmol 2016;4:10:795-804.
14. ClinicalTrials.gov Identifier: NCT02205840 “A Clinical Study Evaluating the Safety and Efficacy of SI-614 Ophthalmic Solution in Patients With Dry Eye,” Sponsor: Seikagaku Corporation. First received: July 30, 2014. Last updated: January 19, 2015.
15. Petrov A, Perekhvatova N, Skulachev M, et al. SkQ1 ophthalmic solution for dry eye treatment: Results of a Phase II safety and efficacy clinical study in the environment and during challenge in the CAE model. Adv Ther 2016;33:1:96-115.
16. Sosne G, Ousler GW. Thymosin beta 4 ophthalmic solution for dry eye: A randomized, placebo-controlled, Phase II clinical trial conducted using the controlled adverse environment (CAE) model. Clin Ophthalmol 2015;20:9:877-84.



