Presentation
A 58-year-old African-American female presented to the Ocular Oncology Service at Wills Eye Institute with intermittent irritation of her left eye for two years. She described the irritation as itching, burning and redness unrelieved with medical therapies. She denied visual acuity changes during this time. She reported that two years ago bilateral redness and purulent drainage (left eye worse than right) was noted. She went to the emergency room at that time and was treated for conjunctivitis. The problem completely resolved in her right eye but her left eye remained "red" since that time. The patient stated that she had tried multiple medications including topical antibiotics, antihistamine drops and lubricating drops with no improvement in the left eye.
Medical History
The patient revealed a past ocular history of a left eye macular hole diagnosed in 2005, which had been followed by a retina specialist. She had a past medical history of sinusitis and borderline hypertension on no treatment at this time. Her medications at the time of presentation included only as-needed medications of fluticasone, diphenhydramine and artificial tears. She had a distant history of tobacco use, quitting 20 years ago. Her review of systems was otherwise negative.
Examination
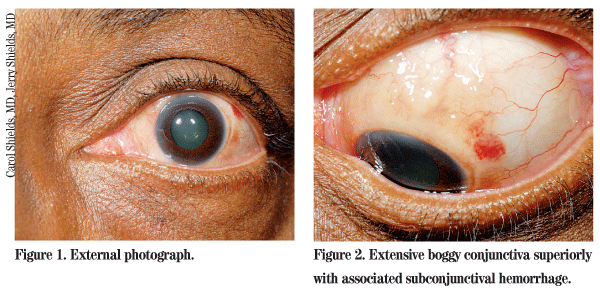
At presentation, best-corrected visual acuity was 20/25+ in the right eye and 20/400 in the left eye. Intraocular pressure was 21 mmHg in the right eye and 18 mmHg in the left eye. Pupils, motility and visual fields were all within normal limits. The anterior exam of the right eye was unremarkable. The left eye demonstrated extensive boggy conjunctiva superiorly and medially, which extended posteriorly from the limbus into the fornix. The area was minimally raised, multinodular and mobile with a rubbery consistency. There was also an area of subconjunctival hemorrhage associated with the lesion. The cornea was clear and the anterior chamber and iris were normal. There was bilateral trace nuclear sclerosis. Fundus exam of the right eye was normal and the left eye demonstrated the aforementioned macular hole.
Diagnosis, Workup and Treatment
This patient presented to the Ocular Oncology Service with a conjunctival redness on her left eye present for at least two years with intermittent symptoms and failed improvement on multiple topical medical therapies. There was no documented progression of the condition photographically but the consistency was thought to be changing, per patient observation.
After thorough slit-lamp examination, an anterior segment optical coherence tomograph was obtained. The OCT images displayed superior conjunctival thickening of the left eye corresponding to the area seen on exam. The lesion was completely isolated to the conjunctiva and no cornea or scleral involvement was seen.
Given the appearance and chronicity of the lesion, the patient was taken to the operating room and the conjunctival mass was removed. At the time of surgery, it was noted that there was extensive, diffuse gelatinous subconjunctival tissue that was cleanly scraped off of the sclera and submitted for pathology.
Discussion
This patient presented with a diffuse gelatinous thickening of the conjunctiva with hemorrhage. There are several concerning diagnoses that should be considered when confronted with this type of lesion. They include lymphoid tumors (from lymphoid hyperplasia to lymphoma); sarcoidosis; Kaposi's sarcoma; amyloidosis; sebaceous gland carcinoma; amelanotic melanoma; and squamous cell carcinoma. Other lesions to consider include papillomas and granulomas. Interestingly, Kaposi's sarcoma and amyloid lesions can present with recurrent conjunctival hemorrhage and should be kept high on the differential if found concurrently, as in this patient. Any suspicious conjunctival lesion should be biopsied or completely excised with tissue review by an experienced pathologist.
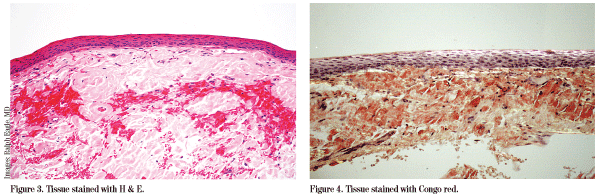
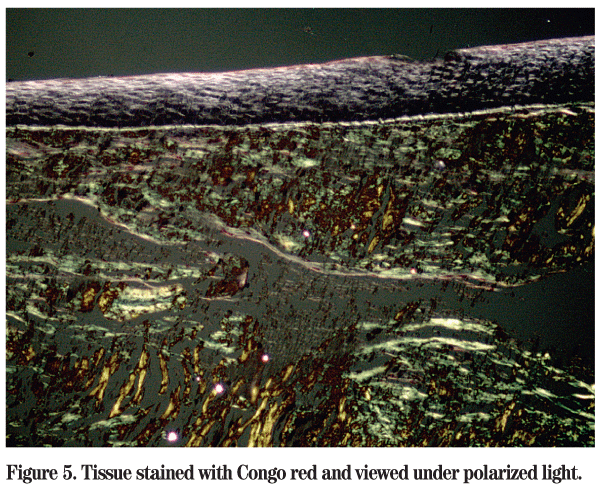
Amyloid is an extracellular protein in abnormal fibrillar form (misfolded) that is deposited in organs and tissues and progressively accumulates. It is diagnosed by microscopic examination of affected tissues. The amyloid deposits are identified histologically by Congo red staining demonstrating the characteristic apple green birefringence when viewed under polarized light. Congo red positivity is the gold standard in the diagnosis of amyloidosis.
There are various forms of amyloidosis that can be described as localized or systemic, primary or secondary and heredofamilial. Amyloid proteins may be derived from many sources including immunoglobulin lambda or kappa light chains, protein AA, protein AP, some proteins of prealbumin origin and transthyretin. In the heredofamilial form, the misfolded protein is typically transthyretin and can result in vitreous amyloidosis.
Localized amyloid lesions usually have little clinical significance, whereas systemic amyloidosis can have catastrophic consequences with widespread organ involvement and dysfunction. Patients with systemic amyloid deposition can develop congestive heart failure, kidney dysfunction, tongue enlargement and neuropathies.
Conjunctival amyloidosis is a very rare condition that is usually seen in middle-aged adults presenting with a yellow-pink nodular thickening of the conjunctiva. In a pathology review by Hans Grossniklaus, MD, and colleagues, only 0.002 percent of conjunctival lesions demonstrated amyloidosis (five out of 2,455 specimens submitted). In a clinical evaluation by Carol Shields, MD, 1,643 patients with conjunctival lesions were evaluated and of the non-neoplastic tumors, 3 percent were found to be amyloid.
Systemic involvement is uncommon, and one study that reviewed 50 cases of conjunctival amyloidosis found systemic involvement only 6 percent of the time. Despite the low rate of systemic amyloidosis, patients must be screened for systemic involvement. These patients should be referred back to their primary-care physicians for a thorough physical exam and baseline studies including a complete blood count, complete metabolic panel, urinalysis, coagulation profile, serum protein electrophoresis (SPEP), urine protein electrophoresis (UPEP), EKG, Bence Jones proteins and a skeletal survey if multiple myeloma is suspected. Systemic diagnosis can be confirmed by bone marrow biopsy, subcutaneous fat aspiration or rectal biopsy (90 to 95 percent sensitivity).
The author would like to thank Carol Shields, MD, and Jerry Shields, MD, of the Wills Eye Institute Oncology Service, and Ralph Eagle, MD, director of the Wills Eye Institute Ocular Pathology Department, for their time and assistance with this case.
1. Hakan D, Shields CL, Eagle RC, Shields JA. Conjunctival Amyloidosis: Report of six cases and review of the literature. Surv Ophthalmol 2006;51:419-33.
2. Mesa-Gutiérrez JC, Huguet TM,
3. Shields JA, Eagle RC, Shields CL, Green M, Singh AD. Systemic amyloidosis presenting as a mass of the conjunctival semilunar fold. Am J Ophthalmol 2000;130:523-525.
4. Duke JR, Paton D. Primary familial amyloidosis: Ocular manifestations with histopathological observations. Tr Am Ophthalmol 1965;63:146-67.
5. Leibovitch I, et al. Periocular and orbital amyloidosis. Ophthalmology 2006:113:1657-64.
6. Fraunfelder, FW. Liquid nitrogen cryotherapy for conjunctival amyloidosis. Arch Ophthalmol 2009;127:645-8.
7. Lee HM, et al. Primary localized conjunctival amyloidosis presenting with recurrent subconjunctival hemorrhage. Am J Ophthalmol 2000;129:244-5.
8. Grossniklaus HE, Green WR, Luckenbach M, et al. Conjunctival lesions in adults. A clinical and histopathologic review. Cornea 1987;6:78-116.
9. Surguchev A, Surguchov A. Conformational diseases: Looking into the eyes. Brain Research Bulletin, doi:10.1016/j.brainresbull.2009.09.
10. Shields CL, Demirci H, Karatza E, Shields JA. Clinical survey of 1,643 melanocytic and nonmelanocytic tumors of the conjunctiva. Ophthalmology 2004;111:1747-54.



