Presentation
A 70-year-old Caucasian man presented to the Wills Eye emergency room accompanied by two nurse aides. He had a right upper eyelid growth that had produced bloody discharge onto his pillowcase for several days. He had been seen by an ophthalmologist for this lesion three years prior but had refused biopsy at that time. Though the mass progressively enlarged, he refused further medical evaluation until he was brought to the emergency room under a legal hold.
Medical History
The patient had a history of paranoid schizophrenia for which he took sertraline (Zoloft) and risperidone (Risperdal). His history also included an episode of rheumatic fever in 1952, but was otherwise negative. Family and social histories were noncontributory.
Examination
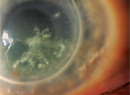
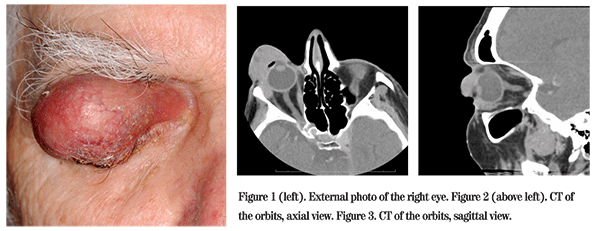
On examination in the Wills Eye Emergency Room, his visual acuity was light perception in the right eye and 20/25 in the left eye. The right upper eyelid was noted to have a firm painless mass measuring 5 cm x 3.5 cm overhanging the entire palpebral fissure. The lid margin was ulcerated and crusted with temporal madarosis (See Figure 1). Elevation of the upper lid revealed the inferior and nasal portions of the globe. The conjunctiva was thickened and erythematous with a fleshy appearance. The cornea was vascularized and opacified with a paracentral pigmented corneal nodule measuring 4 mm x 3 mm x 3 mm. He had no adenopathy in the preauricular, submandibular and submental regions. Computed tomography of the orbits was obtained, revealing a preseptal soft tissue mass with extension into the lateral orbit (See Figures 2 and 3).
Diagnosis, Workup and Treatment
The differential diagnosis of an enlarging eyelid mass includes benign entities such as chalazia, epidermal inclusion cysts and sebaceous cysts. Given the relentless growth, madarosis and bleeding, malignancies such as basal cell carcinoma, squamous cell carcinoma, sebaceous gland carcinoma, amelanotic melanoma or lymphoma were considered.
The patient followed up in the Wills Eye Institute Ocular Oncology Service four days after presenting to the emergency room, and a punch biopsy of the right upper eyelid was performed. Microscopic examination of the specimen disclosed soft tissue infiltrated by nests and lobules of malignant neoplasm. Cells were found containing vacuolated cytoplasm and a focus of comedo-carcinoma differentiation was seen, confirming the diagnosis of sebaceous gland carcinoma (See Figures 4 and 5). The patient and his family were counseled that exenteration was indicated. The patient has refused treatment at the present time and is being followed.
Discussion
Sebaceous carcinomas account for 3.2 percent of malignant eyelid lesions. They most commonly occur in the elderly, especially women, and are also associated with a history of radiation to the face. Lesions occur almost exclusively in the ocular adnexa, arising from meibomian glands, glands of Zeis and sebaceous glands of the caruncle. They classically occur along the upper eyelid margin but may be multifocal. Eyelid sebaceous carcinoma notoriously may be mistaken for refractory blepharitis or recurrent chalazia, potentially delaying treatment. Metastatic disease has been reported to appear in 8 percent of cases after 41 months of follow-up and most commonly occurs in the regional lymph nodes, with later spread to the lungs, brain, liver and bone. 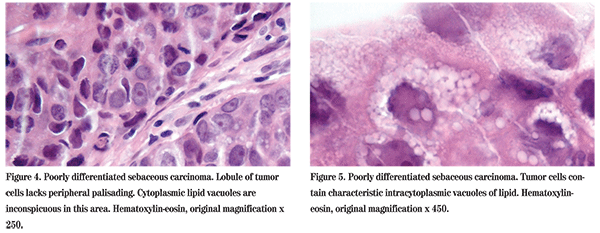
Recommended treatment of sebaceous carcinoma is wide excision of the lesion, alone or in combination with cryotherapy, and topical chemotherapy. Map biopsies are preferred in order to ensure complete excision despite the presence of skip lesions. Sentinel lymph node biopsy can be performed using perilesional injection of Tc 99m. Exenteration is indicated when there is orbital invasion, involvement of upper and lower eyelids or pagetoid spread to the conjunctiva. The response to radiation is poor. Mortality can range from 6 to 22 percent, though this may be decreasing with increased surveillance and earlier treatment.
Dr. Neuwelt would like to thank Carol Shields, MD, and Carlos Gustavo, MD, of the Wills Eye Institute Ocular Oncology Service and Ralph Eagle, MD, of the Pathology Service for their assistance with this case.
Chao AN, Shields CL, Krema H. Outcome of patients with periocular sebaceous gland carcinoma with and without conjunctival intraepithelial invasion. Ophthalmology 2001;108:1877-83.
Margo CE, Lessner A, Stern GA. Intraepithelial sebaceous carcinoma of the conjunctiva and skin of the eyelid. Ophthalmology 1992;99:227-31.
Nijhawan N, Ross MI, Diba R. Experience with sentinel lymph node biopsy for eyelid and conjunctival malignancies at a cancer center. Ophthal Plast Reconstr Surg 2004;20:291-5.
Zurcher M, Hintschich CR, Garner A. Sebaceous carcinoma of the eyelid: A clinicopathological study. Br J Ophthalmol 1998;82:1049-55.
Shields JA, Demirci H, Marr BP, Eagle RC Jr, Shields CL. Sebaceous carcinoma of the eyelids: Personal experience with 60 cases. Ophthalmology 2004;111:2151-2157.
Shields JA, Demirci H, Marr BP, Eagle R, Jr., Stefanyszyn M, Shields CL. Conjunctival Epithelial Involvement by Eyelid Sebaceous Carcinoma. The 2003 J. Howard Stokes Lecture. Ophthal Plast Reconst Surg 2005;21:92-96