Presentation
A 62-year-old man had been seen by an outside eye-care provider for lid swelling for one year. The referral letter noted he had a normal dilated funduscopic exam one month ago and needed an oculoplastic evaluation.
He was initially seen in the primary eye-care clinic and stated that he wanted surgery to correct his puffy eyelids. His lid swelling had worsened over the last month especially below his right eye. He denied any changes in vision or eye pain.
Medical History
The patient had a history of hypertension and borderline high cholesterol. He was taking valsartan and controlling his high cholesterol with diet. He had no allergies. The patient's social history was significant for tobacco use. He had recently emigrated from
Examination
Ocular examination showed Snellen visual acuity of 20/20 in each eye. His pupils were normally reactive with no relative afferent pupillary defect. Visual fields were full to confrontation. His intraocular pressures were within normal limits and extraocular movements were full. Slit-lamp examination was normal, except for mildly congested palpebral conjunctival vessels.
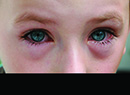
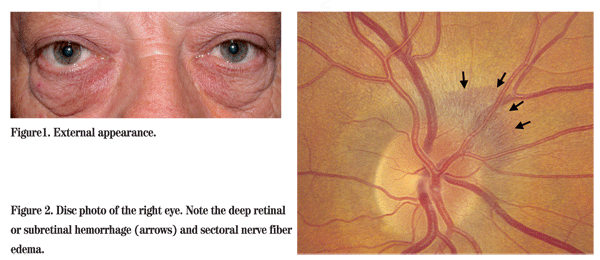
On external examination, he had festooning of the lower lid skin, right worse than left (See Figure 1). No periorbital nodules were palpated. Dilated funduscopic exam showed 2 clock hours of sectoral nerve fiber swelling and a resolving peripapillary flame-shaped hemorrhage or a peripapillary subretinal bleed of the right eye (See Figure 2). The left eye appeared normal.
Diagnosis, Workup and Treatment
The differential diagnosis for a 62-year-old man with normal vision, history of hypertension and smoking and a peripapillary hemorrhage associated with sectoral disc swelling includes pre-ischemic papillopathy, non-arteritic ischemic optic neuropathy, a peripapillary choroidal neovascular membrane, buried optic nerve head drusen and a compressive lesion of the orbit. Giant cell arteritis is less likely.
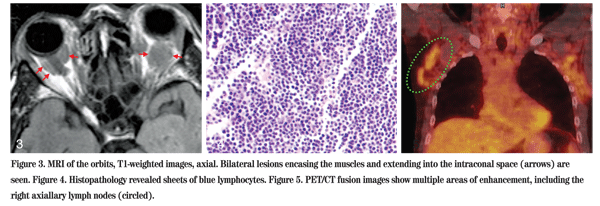
A complete blood count was within normal limits. A Westergren erythrocyte sedimentation rate was 6 mm per hour. The c-reactive protein level was normal. Serum cholesterol was elevated at 251. A hemoglobin A1C was 5.4. Carotid dopplers were within normal limits. An orbital doppler showed a large retroorbital hypoechoic mass on the right. MRI with gadolinium enhancement showed multiple retroorbital masses on both sides encasing the optic nerves and extraocular muscles (See Figure 3).
Given the abnormal imaging studies, the differential diagnosis narrowed to pathologic processes that can affect both orbits. In an adult, such lesions are typically neoplastic or inflammatory, and would include lymphoproliferative disease (lymphoma and lymphoid hyperplasia), sarcoidosis, Wegener's granulomatosis, myelodysplastic or leukemic infiltrate, metastatic disease (such as prostate cancer), orbital xanthogranulomatosis with or without adult-onset asthma, neurofibroma, sclerosing orbital pseudotumor and amyloidosis.
Other lab studies, including angiotensin converting enzyme, prostate-specific antigen, serum protein electrophoresis and anti-neutrophil cyctoplasmic antibody were normal. Chest x-ray was normal. A diagnostic orbital biopsy was performed (See Figure 4). Histopathology showed a diffuse infiltrate of small, well-differentiated B lymphocytes. Immunohistochemical staining was positive for CD20 and negative for CD5 and CD10, consistent with a mucosa-associated lymphoid tissue (MALT) lymphoma. A full body PET/CT showed multiple areas of active uptake in the lymph nodes, indicating active systemic disease (See Figure 5). The patient was referred to an oncologist for systemic chemotherapy.
Discussion
Orbital lymphoproliferative lesions are the most common orbital tumor in adults and orbital lymphoma is the most common of these lesions. There are five main types of orbital lymphoma; MALT lymphoma or MALToma comprises 52 percent of the total. The remaining lesions are comprised of follicular lymphoma (23 percent), diffuse large B-cell lymphoma (8 percent), mantle cell lymphoma (5 percent) and chronic lymphocytic leukemia (4 percent).1
Since lymphoma often masquerades as other conditions, this diagnosis should be considered with any atypical adnexal presentation. In a case series of 69 patients, almost half of patients had a prior diagnosis other than lymphoma upon referral. Typically, lymphoma is considered a painless condition, but in this case series, 19 percent of patients did have pain. Five patients had a presumed diagnosis of orbital inflammation and had undergone steroid treatment for up to 55 months before referral.2
One case series of 160 orbital lymphoproliferative tumors reported the most common presenting symptoms to be eyelid swelling (33 percent), palpable eyelid mass (26 percent), double or blurred vision (13 percent) and proptosis (13 percent).4 Lymphoma typically develops indolently and molds to adjacent tissue planes, usually without bony destruction on imaging studies; not all cases follow these classic patterns.
In the past, location of ocular involvement at time of presentation was considered to be a significant prognostic factor for the development of systemic lymphoma at five years. Patients with initial eyelid involvement had a 67 percent chance for systemic involvement; those with orbital lesions a 35-percent incidence, and those with conjunctival lesions a 20-percent incidence.5
Bilateral orbital involvement also increases the likelihood of concurrent or eventual systemic involvement, as seen in our patient. A recent study estimates that a patient with bilateral involvement on presentation has a 72-percent chance of systemic involvement within 10 years; a patient with unilateral involvement on presentation only has an 11-percent chance of systemic disease.4
Orbital MALT lymphoma is also known as extranodal marginal zone B-cell lymphoma. It can primarily arise in the ocular adnexa or secondarily spread to the orbit as an extranodal process. It is comprised morphologically of heterogenous small B-cells including marginal zone cells, cells resembling monocytoid cells, small lymphocytes and scattered immunoblast and centroblast-like cells. There may also be plasma cell differentiation. These extranodal marginal zone B-cell lymphomas grow in the marginal zone of the reactive B-cell follicles and extend into the interfollicular region.3
Management usually involves either unimodal or combination therapy with radiation, antimetabolites, corticosteroids and biologics. It is important to distinguish MALToma from more aggressive lymphomas. MALToma is typically an indolent, incurable disease that may be considered a chronic condition. In an elderly patient presenting with MALToma, conservative, episodic treatment may be all that is necessary; the toxicity of chemotherapy in such a patient population may be worse than the disease process.
The author acknowledges the assistance of Jurij R. Bilyk, MD, of the Oculoplastic and Orbital Surgery Service, and Ralph C. Eagle, MD, of the Pathology Service at Wills Eye Institute.
1. Ferry JA, Fung CY, Zukerberg L, Lucarelli MJ, et al. Lymphoma of the ocular adnexa: A study of 353 cases. Am J Surg Pathol 2007; 31:170-84.
2. Sullivan TJ, Whitehead K, Williamson R, Dickie G et al. Lymphoproliferative disease of the ocular adnexa: A clinical and pathologic study with statistical analysis of 69 patients. Ophthal Plast Reconstr Surg 2005;21:177-88.
3. Isaacson PG, Muller-Hermenlink HK, Piris MA, Harris NL, et al. Extranodal marginal zone B-cell lymphoma of mucoas-associated lymphoid tissue (MALT lymphoma). World Health Organization Classification of Tumors.
4. Demirci H, Shields CL, Karatza EC, Shields JA. Orbital lymphoproliferative tumors: Analysis of clinical features and systemic involvement in 160 cases. Ophthalmology 2008;115:1626-31, 1631.e1-3. Epub 2008 Apr 28.
5. Knowles DM, Jakobiec FA, McNally L, Burke JS. Lymphoid hyperplasia and malignant lymphoma occuring in the ocular adnexa: A prospective analysis of 108 cases. Hum Pathol 1990;21:959-73.