Cataract predicted increased mortality in patients 49 years and older, and age-related macular degeneration predicted mortality in those aged 49 to 74 years, according to researchers in
At baseline, 3,654 persons 49 years and older were examined in the Blue Mountains Eye Study (1992-1994). Researchers used standardized photographic grading to assess AMD and cataract. Mortality and causes of death occurring between baseline and December 31, 2003, were obtained via data linkage with the Australian National Death Index. Age-standardized mortality rates were calculated. Hazard ratios (HRs) and 95 percent confidence intervals (CIs) were assessed using Cox models.
Cumulative follow-up of the study cohort was 11 years (median: 10.7 years; minimum: <1 year; maximum: 12 years). Data on mortality or cause of death were missing for 21 participants (0.6 percent). The remaining 3,633 participants were considered to be at risk. During an average 11-year period, 1,051 participants (28.9 percent) died of any cause and 483 (13.3 percent) died of vascular causes.
Researchers detected visual impairment in 132 participants (3.6 percent), including 24 participants who were younger than 75 years and 108 who were 75 years and older at baseline. Cumulative 11-year mortality was higher in participants with vs. without visual impairment (75 vs. 26.9 percent), with age-standardized mortality of 54 percent and 34 percent in participants with and without visual impairment, respectively. Among persons younger than 75 years, visual impairment predicted higher all-cause mortality, that is, mortality from any cause (HR, 2.9; 95 percent CI, 1.6 to 5.5). A similar association between visual impairment and vascular mortality was observed in persons younger than 75 years after age and sex adjustment, but the association became nonsignificant after adjusting for other factors (HR, 1.1; 95 percent CI, 0.2 to 8.4).
Of 3,553 participants with data available to assess the mortality risk associated with AMD, the disease was found in 6.9 percent of participants at baseline (n=244), including 4.8 percent with early AMD (n=172) and 2 percent with late AMD (n=72). Of those with late AMD, 12 were younger than 75 years at baseline. Cumulative 11-year mortality was higher in participants with vs. without AMD (55.8 vs. 25.9 percent), with age-standardized mortality of 45.8 percent and 33.7 percent in persons with and without AMD, respectively. There was no significant difference in all-cause mortality risk between persons with vs. without any AMD (HR: 1; 95 percent CI, 0.8 to 1.3). In participants younger than 75 years, any AMD predicted higher all-cause mortality (HR: 1.7; 95 percent CI, 1.2 to 2.4) and increased vascular mortality risk (HR, 2.1; 95 percent CI, 1.2 to 3.8). After further adjusting for visual impairment and any cataract at baseline, this association remained significant (HR: 1.8; 95 percent CI, 1.2 to 2.6).
Any cataract was seen in 1,204 (33 percent) participants. Cumulative 11-year mortality was higher in participants with vs. without any cataract (43.3. vs. 17.4 percent). Age-standardized all-cause mortality was 39.2 and 29.5 percent for persons with and without cataract, respectively. Any cataract (HR, 1.3; 95 percent CI, 1 to 1.5) and cortical (HR, 1.2; 95 percent CI, 0.97 to 1.4), nuclear (HR, 1.2; 95 percent CI, 0.98 to 1.5) and posterior subcapsular (HR, 1.3; 95 percent CI, 1 to 1.7) cataract were also associated with higher all-cause mortality.
The researchers admit to a number of limitations with the study; they include the likelihood that some important confounding factors may not have been controlled for, and the possibility of chance findings cannot be completely excluded.
(Arch Ophthalmol 2007;125(7):917-924)
Cugati S, Cumming RG, Smith W, Burlutsky G, Mitchell P, Wang JJ.
A New Clinical Challenge
Researchers in
In this retrospective observational case series, surgeons reviewed the medical and photographic records of six patients examined and observed from July 1984 to January 2006. The patients were noted to have clinical features that challenged conventional diagnoses. Clinical follow-up ranged from 13 to 245 months (mean: 68). Main outcome measures were best-corrected visual acuity and angiographic findings.
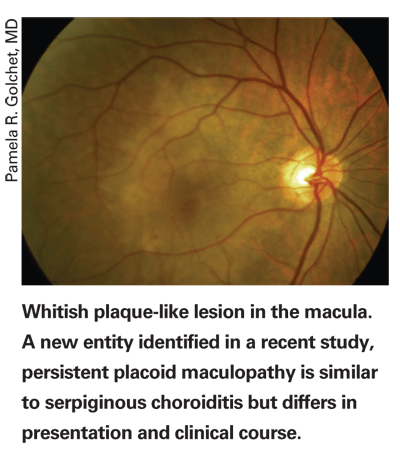
There were five men and one woman, with ages ranging from 50 to 68 years old. None of them had consistent systemic medical problems. They had well-delineated whitish plaque-like lesions involving the macula and sparing the peripapillary areas of both eyes. In contrast to serpiginous choroiditis, acuity remained good despite early involvement of the fovea until complications related to choroidal neovascularization or pigmentary mottling developed. Angiographic characteristics and the clinical course were also atypical. Fluorescein angiography revealed well-defined early hypofluorescent areas that partially filled in the late phase. Indocyanine green showed the hypofluorescence to be persistent. Unlike serpiginous choroiditis, the white macular lesions faded over a period of months to years, whereas the characteristic angiographic findings often persisted. CNV developed in 11 of 12 eyes, with subsequent conversion to disciform macular scars in nine of 12 eyes. Unlike serpiginous choroiditis, none of the eyes showed chorioretinal scar formation unless related to CNV.
(Ophthalmology 2007;114:1530-1540)
Golchet PR, Jampol LM, Wilson D, Yannuzzi LA, Ober M, Stroh E.
Adjustable IOL in Cataract Surgery
According to researchers in
In the prototype of the lens used in the study implantations, a haptic containing an adjustment element is connected to the optic. This is formed by an interruption of the haptic consisting of a cylinder 1 mm high attached to the optic, which contains a piston attached to the outer part of the haptic. The cylinder and the piston can be moved relative to each other. This element allows the optical part of the PC/IOL to move along the optical axis. During continual follow-up, eyes were monitored for appearance of the anterior and posterior segment of the eye. Refraction, visual acuity and intraocular pressure were measured. Amsler grid testing was also used.
After implantation, adjustment surgery was carried out through two 1-mm corneal paracenteses. An IOL optic manipulator with a T- or L-shaped spike was used to press down onto the piston, while a second was placed against the connection of the optic and the cylinder from the opposite side. The first instrument either pushed the piston while the second supported the cylinder from the posterior side or vice versa.
None of the eyes with an adjustable IOL developed any signs of inflammation, corneal decompensation, iris atrophy, pupil distortion or spontaneous capsular tear either during surgery or the entire observation period. Centration of the adjustable PC/IOL was maintained in all eyes. Comparison of eyes with the adjustable PC/IOL and eyes with the conventional PC/IOL in bilaterally pseudophakic patients showed no significant difference in central visual acuity, refractive stability or intraocular pressure. Results of Amsler grid testing were normal in all eyes containing the adjustable PC/IOL. Eighteen eyes developed posterior capsule opacification, but this was treated with Nd:YAG laser capsulotomy and central visual acuity was restored in all of the 18 eyes.
The study adds more evidence to the idea that an adjustable PC/IOL is a safe long-term option.
(Arch Ophthalmol 2007;125(7):936-939)
Jahn CE, Schöpfer DC.




