“I always tell students, techs and practices that products are consumed; services are experienced,” says Palm Coast, Florida’s Sharon Alamalhodaei, COMT, OSC. “We’re providing an experience to our patients. If they don’t have a phenomenal experience with you, they’re not going to be your patients for very long.” Thoughts on the elements of a great patient experience follow, along with measures you might consider to show your patients how much you value them.
Superstar Staffing
In the age of online reviews, a rude or dismissive front-desk or clinical staff will eventually garner unwanted attention. There’s evidence that the elements of the Press Ganey patient-satisfaction survey most associated with high scores from ophthalmology patients are the amount of time the provider spends with the patient and the ease of scheduling appointments.1 Another study compared mean Press Ganey survey scores of physicians with and without negative online reviews, and found no difference between the two groups’ mean satisfaction scores on physician-specific questions. The physicians with lower online reviews did, however, have lower mean satisfaction scores on questions about non-physician-specific parameters.2
While your staff doesn’t control how much time you spend with each patient, they can increase satisfaction with many other aspects of the patient/physician encounter. A few key ways your staff can make patients want to return to your office include: managing the patient flow; helping patients manage wait times; and making a powerful first impression.
• Direct the traffic. Connecting patients with needed services quickly sets the tone, says Scott Neilson, COE, CPA, CGMA, executive director of Pacific Eye Associates in San Francisco. His high-volume office created a greeter position shortly before he joined the practice several years ago. “Since we have about 13 doctors at our practice, we can easily see between 200 and 250 patients per day,” he explains. “We noticed that especially at the beginning of our clinic shifts, we had many doctors all getting started at the same time, bringing in roughly 10 to 15 patients within about five minutes for the first of the morning or afternoon appointments. Additionally, people would often come into our optical shop around lunchtime or first thing in the morning to pick up glasses or contacts. Sometimes, patients just needed to be routed to the correct person or department instead of standing in a line five or eight deep just waiting to check in or to have a basic question answered.”
They tried a stationary greeter standing at a kiosk, but eventually decided to give the greeter a mobile device and allow him or her to meet people as they came through the door. “We found that the line to check in or check out dramatically dropped as new arrivals could access different parts of the health-care transaction without having to wait in line to do it,” says Mr. Neilson. “It’s definitely an expense to the practice, but the payoff comes in the form of higher patient-satisfaction scores. We frequently get good comments about the helpfulness of our greeter.”
He says the practice schedules one greeter per shift, but the director of communications has cross-trained front-office staff as greeters, check-in or telephone receptionist. “We have to be nimble,” Mr. Neilson says. The greeter isn’t a strictly dedicated position; by being flexible we have an extra person in the organization that can go where we need them to help keep our lines as short as possible.”
• Manage the wait. Ms. Alamalhodaei, who founded Eye Tech Training (EyeTechTraining.com), a company specializing in ophthalmic technician training and education as well as onsite assessment and training, says a customer-focused staff helps your patients take waiting in stride. “You have to manage their perception of the passage of time,” she explains. “By way of example, I ask my students to imagine the Cheesecake Factory at 6 p.m. on a Friday night. When you’re seated, the server may come by your table and say, ‘I’ll be with you in just a moment.’ That action resets the clock we have in our heads. We all have an amount of time that we’re willing to wait happily and comfortably. For me, it’s about 15 minutes in a doctor’s office. Between 15 and 30 minutes, I’m still fine, but I’m noticing the wait. But at 45 minutes, I’m thinking about going up to the front desk. I tell my students that by the time a patient approaches you and asks how much longer the wait is going to be, they’ve been stewing about it for a while. Most people don’t just stand up and ask that question spontaneously.
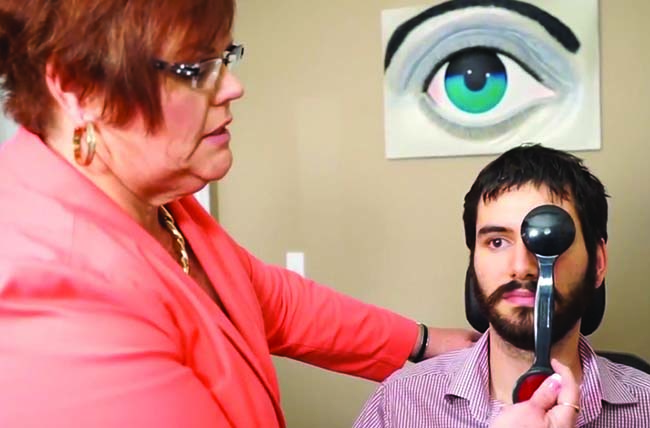 |
| Sharon Alamalhodaei, COMT, OSC (using occluder), emphasizes that members of the eye-care team must focus on serving patients whenever they are visible or within earshot. |
“When someone comes and tells me that it will only be a moment, it resets that clock in my head to zero,” she continues. “I’ve had a contact; they’ve acknowledged my presence, so I know that I’m not going to be forgotten. My timer’s back at zero. Suppose a doctor is running behind with one patient, and there’s another patient waiting in the room next door. Just sticking your head in and saying, ‘Mrs. Smith, I want to let you know that you’re next to see the doctor. He or she’s been with this other patient for a little while, but you’re the very next patient.’ That resets the clock.”
Ms. Alamalhodaei adds that it’s better to give patients a finite wait time rather than an unknown, “infinite” wait. “To apply this principle in the clinic, if the doctor is running behind, you should tell your patient, ‘Mrs. Smith, I want to let you know that the doctor’s running about a half-hour behind schedule.’ The patient will tolerate the wait better.” Ms. Alamalhodaei emphasizes that this also empowers patients to manage their time: If they know they’re facing a 45-minute wait, a heads-up gives them the option to quickly run a nearby errand instead of sitting idle.
“It just shows respect for the patient to let them know that,” she stresses.
• Make an impression. “Our opportunities to make a lasting impression are when patients first call on the phone and when they come into our office,” says Ms. Alamalhodaei. Whether your staff is answering the first or the hundredth call of the day, callers should always sense engagement and a willingness to help. “They should never perceive that it’s the hundredth call, even if it is,” she says.
As a practice administrator, Ms. Alamalhodaei would employ a powerful, no-cost strategy to make new patients feel cared for. “I instructed my front desk staff to let me know when new patients came in,” she explains. “I would seek out that new patient and shake their hand, make eye contact, smile, welcome them, introduce myself and give them my card. I would say, ‘I’m Sharon, and I’m the practice administrator here. I want to welcome you to our practice. Here’s my card: If you ever have any questions or problems, I want you to feel free to contact me.’
“I sure wouldn’t give my card to a patient if we had crappy service, poor billing procedures or nasty staff,” Ms. Alamalhodaei continues. “It was a way of holding myself accountable for providing a wonderful experience. It didn’t cost a penny, but it made a lasting impression.”
When Mr. Neilson noted negative online reviews regarding Pacific Eye’s front desk and check-in process, he implemented three mandatory aspects of customer service: smile, greet, and use the patient’s name.
“Before you say one word to a patient, you need to be smiling at them,” he says. “Before you get down to business, greet them. You have to say, ‘Hello.’ ‘Good morning.’ ‘Good afternoon.’ Our staff speaks a lot of different languages: At our front desk alone, we have five languages represented. We encourage our staff to learn greetings in languages other than their own. Even if a patient needs language-support services from one of our interpreters, at least they’ve heard a greeting in their native language,” he says.
“And sometime during that exchange with the patient, you have to use their name at least once,” Mr. Neilson continues. “Our name is so important to us that when we hear it, it activates certain pleasure centers in the brain. And using a patient’s name makes them an individual—not an account number, not ‘next in line.’ Forming that connection through the use of a name is very important. So every new hire, and anyone who’s been here for 20 years, needs to smile, needs to greet and needs to use the patient’s name at least one time during the initial interaction. Although [patient] volume is still important, so is being more focused on making sure we connect with our patients through basic customer-service skills.”
Ms. Alamalhodaei likens being wherever patients can see you or hear you to being onstage. “Being onstage is not being phony,” she says. “It means that you have your professional demeanor on, and that your talk and actions are all patient-centered. You’re not talking about the shoe sale at the mall, for example. Your focus is on your patient and on serving them.”
She adds that it’s also important that your talk be positive. “Instead of ‘Oh, our office doesn’t do that,’ you can say, ‘This is how our office handles that situation,’ ” she explains. “You’re saying the same thing, but you’re sending the message in a completely different way that will most likely be received in a very different way.”
Consider a Physician Extender
Lee Schelonka, MD, a retina specialist in practice at the Department of Ophthalmology, Kaiser Permanente Lone Tree Medical Offices in Lone Tree, Colorado, says via email that the addition of physician assistant Chad LaRoche, PA-C, to his office has increased the efficiency of intravitreal injections and won rave reviews from patients, without compromising safety. “By performing the majority of the injection procedures, he’s improved access for evaluation appointments with our ophthalmologists,” he says. “Chad has great communication skills for patient education, and makes personal connections with them. He also helps our patients navigate the patient-assistance programs that help with their copays. Our surveys show that he has even better patient-satisfaction scores than our MD’s.”
Dr. Schelonka says that Kaiser Permanente explored the idea of adding a physician extender several years ago, after another retina surgeon wondered if his nurse could do injections. “In Great Britain and Denmark, most intravitreal injections are done by nurses,” he explains. “But in the United States, nurses have certain regulatory restrictions on their practices that could potentially limit a role in doing injections. On the other hand, in Colorado, the scope of practice of physician assistants is limited only by the supervising physician’s scope of practice, and the physician’s decision that it would be prudent and safe to delegate procedures to the PA. One other Kaiser Permanente retina specialist in Hayward, California, had a PA doing intravitreal injections under his supervision; he and his PA were very positive about the quality and patient satisfaction. As we researched further, we found a few other practices also using PAs for eye injections. We reviewed our plans with our quality and legal teams and hired Chad, our first physician assistant. Since April 2017, he has done more than 4,000 injections. Our patients love the care he gives, and his quality is great, as we reported at AAO 2018.” Dr. Schelonka presented a poster at the meeting assessing safety and patient satisfaction of the practice’s first 2,000 PA-administered injections.
One specific boon to patient happiness that Dr. Schelonka notes is decreased patient wait times. He cautions, however, that the laws governing the scope of practice and supervision of PAs vary by state, so adding a physician assistant may not be uniformly feasible. “Our PA was a great fit into our intravitreal-injection and oculoplastic practice,” he reports. “He does procedures which are beyond the scope of practice of optometrists, without encroaching on our optometrists’ refractive and primary eye-care practices.”
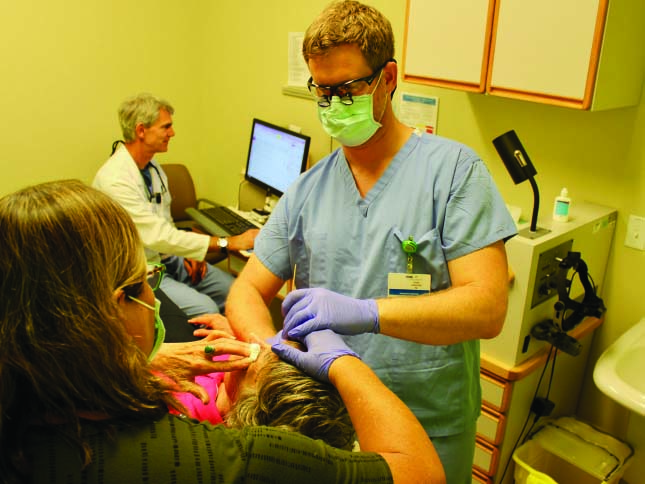 |
| Lee Schelonka, MD, (background) says adding physician assistant Chad LaRoche, PA-C, to his retina practice has increased efficiency and patient satisfaction. |
Tech and Surveys
Mr. Neilson says that surveys like those conducted in Dr. Schelonka’s practice are important. He tries to keep his office’s surveys to a maximum of four or five questions, each carefully phrased to preserve statistical integrity by avoiding overlap. Some practices have long touted the convenience of online check-in and the ability to access personal medical records through a web portal. Mr. Neilson says, however, that Pacific Eye’s satisfaction surveys haven’t indicated that these are high priorities for their patients. “We have those features,” he says. “But we have separate EHR and practice-management systems, so giving someone the ability to access an appointment goes through one program; giving them the ability to look at their records goes through a different program. We’re currently exploring some options to possibly tie them together, instead of having the patient register for two different portals with two different logins and passwords. We’ve also found a number of our patients tend to be borderline-technophobic in some respects. Many of our patients are either non-English speakers or second-language English speakers, so that has created an additional hurdle to encouraging everybody to go online to access their medical records. Many patients have either indicated that they don’t want or don’t find a lot of value in that service. So far, at least statistically, we haven’t seen a huge indication that our patients strongly desire electronic access. Some do, but not very many.
“One of the things we’ve wanted to be careful about was going more tech-centric within the practice at the expense of the human side of the equation,” Mr. Neilson continues. “We’d like to wait until we have a little more clarity on it. I think better electronic access might be somewhat important, but we currently get very few responses indicating that that’s a mission-critical aspect of our patients’ health care.”
For Surgeons
Patient satisfaction is the surgeon’s job too, regardless of how good your front office and technicians are at providing it, according to Ms. Alamalhodaei. “The tail doesn’t wag the dog,” she notes.
Mr. Neilson adds, “Being competent in your profession is no longer sufficient. Twenty or 30 years ago, you could get by with that. In the current consumer-driven world of health care, just being a good clinician, physician or surgeon isn’t enough. You really have to convey the warmth of why you’re in this profession as well as your competency.”
He says that smiling is an important part of the physician’s therapeutic armamentarium. “We always encourage our physicians to smile,” he says. “We encourage them to greet patients when they walk into the room, whether it’s, ‘Welcome to the practice!” or, ‘Glad to see you back again!’ It has to be somewhat enthusiastic, but not over the top. The other skill we try to teach them is a dual one: to listen and sympathize. Patients come to our practice because something’s wrong and it’s affecting their vision—and that’s really scary for a lot of people. We encourage doctors to listen to what the patient has to say. It’s important to listen and repeat back what you just heard in order to show sympathy. For example, you could say, ‘I’m so sorry that you’re going through that. I know that must be scary.’ It really does have an impact when patients know that you’re not just a good doctor, but that you also care about them.”
When you and your staff share the pursuit of patient satisfaction, they can alert you to potential challenges. “Empower and listen to your staff,” said Vance M. Thompson, MD, of Thompson Vision in Sioux Falls, South Dakota, during a presentation on managing unhappy refractive patients at October’s 2018 American Academy of Ophthalmology meeting in Chicago. “They spend the most time with the patient.” He said that alert and empowered staff could tip surgeons off to cues in a patient’s attitude or demeanor that would suggest a satisfactory outcome is improbable. “I won’t operate on a patient that I don’t feel a bond with,” said Dr. Thompson. “Whatever else is going on, we need to connect.”
Although his talk at the AAO meeting was specifically geared toward addressing unhappy refractive patients, much of Dr. Thompson’s advice was applicable to surgeons from other subspecialties seeking to increase patient satisfaction. “Perception is reality,” he said of the patient’s experience of health care. “Think every step of the way how you’d feel,” he urged. Dr. Thompson also advised his audience not to skimp on patient education. “Fifty to eighty percent of information is forgotten; of the information that is remembered, 50 percent is remembered correctly.” He suggested writing your personal contact information onto a business card as a way of communicating personal care to patients.
Whether the encounter is a routine screening or a consultation for a sight-threatening condition, your patient wants to know that you and your staff are caring as well as skillful. “You should cultivate a culture in your practice where there’s an unspoken and subtle peer pressure, so that everyone knows that providing high-quality service is what’s expected,” says Ms. Alamalhodaei. “It’s about reaching a sort of critical mass, so that both newcomers to your practice and established employees who don’t toe the line and embrace the culture will clearly stand out to everyone as falling outside of the standard.” REVIEW
Ms. Alamalhodaei is the author of two books: “How to Be the Tech Your Doctor Can’t Live Without,” and “10 Steps to a Phenomenal Patient Experience: Customer Service Secrets for the Eye Care Team.” Mr. Neilson reports no relevant disclosures. Dr. Schelonka reports no relevant disclosures. Dr. Thompson reports no relevant disclosures.
1. Long C, Tsay EL, Jacob SA. Factors associated with patient Press Ganey satisfaction scores for ophthalmology patients. Ophthalmol 2016;123:2:242-7.
2. Widmer RJ, Maurer MJ, Nayar VR, et al. Online physician reviews do not reflect patient satisfaction survey responses. Mayo Clin Proc 2018; 93:4:453-7.



