While current research on ocular allergy is revealing new possibilities on the causes and mechanisms of the condition, clinical applications of this research in the general ophthalmologist's practice may take some time. "The understanding of the immunology is a lot more advanced than the clinical treatments for allergy, which may come along in the future," explains Stephen C. Pflugfelder, MD, director of the Ocular Surface Center, Baylor College of Medicine in Houston.
However, Dr. Pflugfelder notes that recent discoveries are revealing a new complexity to allergy. "One of the most exciting things in allergy has been the discovery of the pathways leading to exactly how allergy is induced, such as which mediators are involved in the process," he says. These include mast cells, which have been known for years, and also the T-lymphocytes.
"Allergy is a lot more complicated than it was in the past when it was [thought to be] just allergens binding to mast cells," Dr Pflugfelder notes.
Neal P. Barney, MD, an associate professor in the Department of Ophthalmology and Visual Sciences, University of Wisconsin, Madison, notes that it is an exciting time in ocular allergy research. "Allergy research in general is increasingly focusing on the union of the innate and adaptive immune systems in the pathogenesis of the disease," Dr. Barney says. "The ocular surface has been shown to have pathogen-recognition receptors, a key element in recognition of microbial products that we are all exposed to.
We are witnessing research into the effect that microbial product recognition has in the ocular surface undergoing an allergic reaction. Additionally, regulatory T-cell contribution to the initiation of and continuation of control over the allergic inflammation of the ocular surface is a valuable area of investigation."
Immune Responses
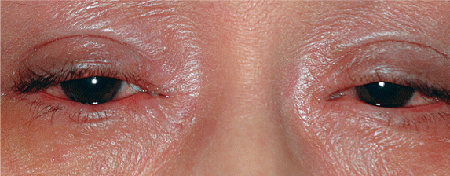
Researchers are continuing to uncover the mechanisms behind allergic eye disease, an abnormal immune hypersensitivity response to allergens. Allergic eye disease is characterized by IgE-mediated and/or T-lymphocyte-mediated immune hypersensitivity reactions that lead to an immune response, resulting in the clinical manifestation of ocular allergy.1
|
"Our studies show that some environmental factors, such as certain microbial components that are produced by bacteria or fungi or viruses, would stimulate the corneal epithelial cells to produce levels of this cytokine called TSLP," says Dr. Pflugfelder, an author of the study. "We found out that TSLP regulates the immune response toward an allergy type of response, which is called T-helper 2 or TH2 response.
Therefore, it shows that for a long time, there has been a link between environmental factors and induction of allergy."
Mite exposure is one example; there is even some evidence that a low-grade infection with staph bacteria may stimulate allergy or eczema in particular. "There are receptors on cells called toll-like receptors, and there are 10 of those in human cells that have been identified," says Dr. Pflugfelder. "They bind to these different microbial components and this stimulates a stress signaling response by the cell. So that is where we found that these microbial factors stimulated production of TSLP through the toll-like receptors," he explains.
The implications for human allergy would be that potentially this could be blocked. For example if a low-grade chronic staph infection were driving allergy, there could be several modes of therapy: The patient could be treated with an antibiotic to kill the staph infection; these toll-like receptors could be blocked so even if there is staph around, the cells won't respond to it; or the cytokine TSLP could be blocked.
Dr. Pflugfelder points out that this cytokine has been very important in asthma and eczema. "This is the first time that we have shown that the eye surface cells produce it and it could be stimulated by environmental factors. It might be as simple as blocking the receptors. It provides new evidence that there are new targets for treatment of allergy," he explains.
In another recent study, serum allergen specific immunoglobulin E (IgE) levels were evaluated in patients with various types of allergic conjunctivitis, including 25 patients with seasonal allergic conjunctivitis; 17 patients with perennial allergic conjunctivitis; and 10 patients with vernal conjunctivitis.3 The researchers concluded that an allergic reaction against house dust mites and pollens was common in VC, whereas specific IgE against grass pollens was remarkable in SAC.
Allergy researchers are also looking at TNF-alpha stimulation. Previous studies demonstrated that mast cell-derived TNF-alpha stimulation is critical to the upregulation of intercellular adhesion molecule (ICAM-1) on human conjunctival epithelial cells (HCECs), which is an important feature of ocular allergic inflammation. Shedding of TNFR1 by TNF-alpha-converting enzyme (TACE) is a primary mechanism for the regulation of TNF-alpha-mediated events.
One group examined the regulation of TNFR1 expression and shedding by TACE on primary HCECs and the IOBA-NHC conjunctival epithelial cell line and found that TACE promotes TNFR1 shedding in HCECs and that TNFR1 expression may be a more significant target than TNF-alpha for intervention in ocular inflammation.4
|
The response was in the form of increased expression of ICAM-1. "Often times, a strategy to downregulate a reaction such as TNF-induced ICAM-1 on the epithelial cells is to block the receptor or to reduce the number of receptors available to interact with TNF. This article suggests that reduced receptor [volume] could be a target for intervention in ocular allergy treatment," he says.
This type of research will most likely lead to novel drug therapies for ocular allergies in years to come. According to Dr. Pflugfelder, pharmaceutical companies are pursuing these new targets, and they are designing strategies to inhibit them or block them so there will probably be more effective allergy treatments in the future for some of these mediators.
Continued Research
Unraveling the mysterious connections of ocular allergies and treatment is stretching beyond ophthalmology (See sidebar). "We are learning from other disciplines and researchers who are conducting research. For example, we got interested in [TLSP] research through a researcher who works in cancer and allergy, and he discovered this molecule about five years ago," explains Dr. Pflugfelder. He notes that it made sense that TLSP might be related to ocular allergy.
"I think there will be greater interaction between different specialties and disciplines for continuing allergy research," he says.
1. Chigbu DI, The pathophysiology of ocular allergy: A review. Cont Lens Anterior Eye. 2009 Feb;32(1):3-15.
2. Ma P, Bian F, Wang Z, Zheng X, Chotikavanich S, Pflugfelder SC, Li DQ. Human Corneal Epithelium-Derived Thymic Stromal Lymphopoietin - A Potential Link between the Innate and Adaptive Immune Responses via Toll-Like Receptors and Th2 Cytokines. Invest Ophthalmol Vis Sci 2009 Jan 17. [Epub ahead of print]
3. Kocabeyoglu S, Bozkurt B, Bilen O, Irkec M, Orhan M. Serum allergen specific immunoglobulin E levels in patients with allergic conjunctivitis. Eur J Ophthalmol 2008 Sep-Oct;18(5):675-9.
4. Cook EB, Stahl JL, Graziano FM, Barney NP. Regulation of the receptor for TNFalpha, TNFR1, in human conjunctival epithelial cells. Invest Ophthalmol Vis Sci 2008 Sep;49(9):3992-8. Epub 2008 May 16.