San Bernardino, Calif.
To get a picture of the current state of affairs regarding glaucoma surgery, it's helpful to review the national trends over a significant period of time. One way to do that is by examining reimbursement claims data. Although most third-party payers are unable or unwilling to publish their data sets, the Centers for Medicare & Medicaid Services does make their information public, making it possible to get a good sense of how the utilization of different types of glaucoma surgery has shifted over time. (Because glaucoma is much more common among the elderly, the lack of data for non-Medicare beneficiaries inherent in this approach is unlikely to significantly distort our assessment of the state of affairs.) The analysis in this article is based on numbers of paid claims for Part B services provided to Medicare beneficiaries between 1995 and 2007 (the latter being the most recent numbers currently available) for surgical services that are primarily indicated to treat glaucoma.
Conclusions drawn from this data are, by nature, subject to limitations. For example: Because these numbers represent only patients covered by Medicare Part B, they exclude any data from those insured under Medicare Part C and those insured by other sources; the older average age of this population sample implies that these patients may have more advanced disease and more co-morbidities; there is inherent ambiguity because multiple ways of performing some procedures are covered by a single code; and, the accuracy of these numbers assumes that physicians code procedures correctly. In addition, its likely that several factors influencing surgeons' choices are at work at the same time. Nevertheless, it's possible to draw some interesting and illuminating conclusions, even though we cannot be absolutely certain what caused these trends.
A Tale of Trabeculoplasty
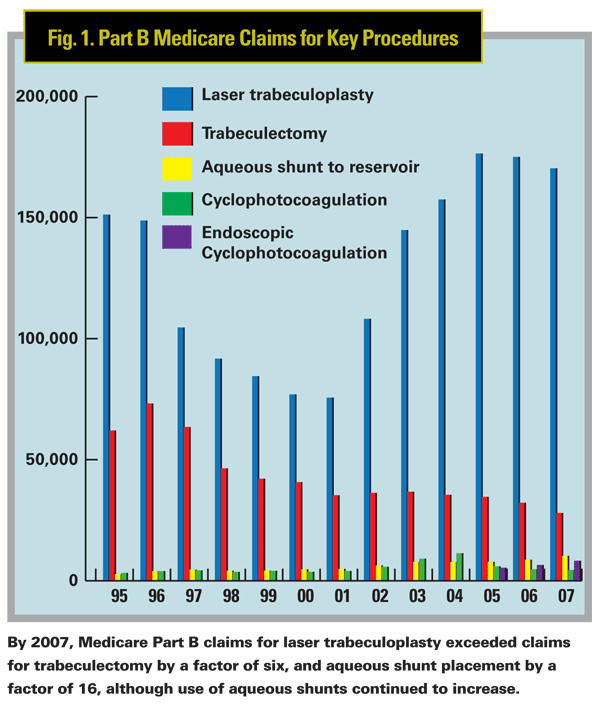
As you can see in Figure 1, laser trabeculoplasty (CPT code 65855) is the dominant surgical procedure in glaucoma, by far—at least in terms of Medicare claims.
However, the number of claims for this category changed dra- matically between 1995 and 2007. In 1995 surgeons submitted about 150,000 procedure claims for laser trabeculoplasty, but the number steadily diminished until 2001; at that point, the number of claims began to increase rapidly, peaking at around 175,000 procedures a year in 2005, where the number has generally remained.
The reason for the decline in laser trabeculoplasty claims is suggested by events at that time; the medical treatment of glaucoma changed dramatically in 1995 with the introduction of latanoprost (followed soon thereafter by apraclonidine and brimonidine).
This advent of new anti-glaucoma medications likely caused a shift in treatment preferences. The development that seems likely to explain the reversal of that downward trend a few years later is the appearance of the Lumenis Q-switched Nd:YAG laser and the selective laser trabeculoplasty procedure in 2001. (It's also conceivable that common problems with anti-glaucoma medications, such as poor compliance and high cost, gradually became more apparent and reduced their attractiveness for some patients, despite the introduction of even more eye-drop options as the years passed.)
It's likely that SLT has become popular because it's an effective, low-cost, low-risk, in-office procedure with few complications and attractive Medicare reimbursement. Significantly, pharmaceutical benefits (Medicare Part D) are not universal among Medicare beneficiaries and provide only limited reimbursement, so there are substantial financial advantages for elderly glaucoma patients who choose a Medicare covered laser procedure over out-of-pocket anti-glaucoma medications. Also, in some parts of the
In 2007, the most recent year for which we have Medicare claims data, laser trabeculoplasty was being performed six times as often as trabeculectomy and 16 times as often as aqueous shunt placement. Since trabeculoplasty is considered a good treatment option in early-stage glaucoma, according to the American Academy of Ophthalmology's Preferred Practice Patterns, advances in technology that permit earlier detection of glaucoma could also be providing a larger pool of candidates for the procedure.
Trabeculectomy, Shunts and ECP
As you can see in Figure 1, paid claims for trabeculectomies steadily diminished during this period. (Codes 66170 and 66172 are combined in this dataset.) This likely reflects a growing understanding that trabeculectomy is a less-than-wonderful approach to treating glaucoma, leading surgeons to shift to other more attractive surgical options as they become available.
Nevertheless, trabeculectomy re- mains an important surgical option, particularly in re-operations. In fact, if we look at the two subcategories of trabeculectomy claims (66170—trabeculectomy ab externo in absence of previous surgery, and 66172—trabeculectomy ab externo w/scarring from previous surgery or trauma), shown separately in Figure 2, it becomes clear that trabeculectomy performed on virgin eyes accounts for all of the decline. That's true despite the fact that this is a much easier surgery than its counterpart, where the surgeon must deal with scar tissue and other impediments.
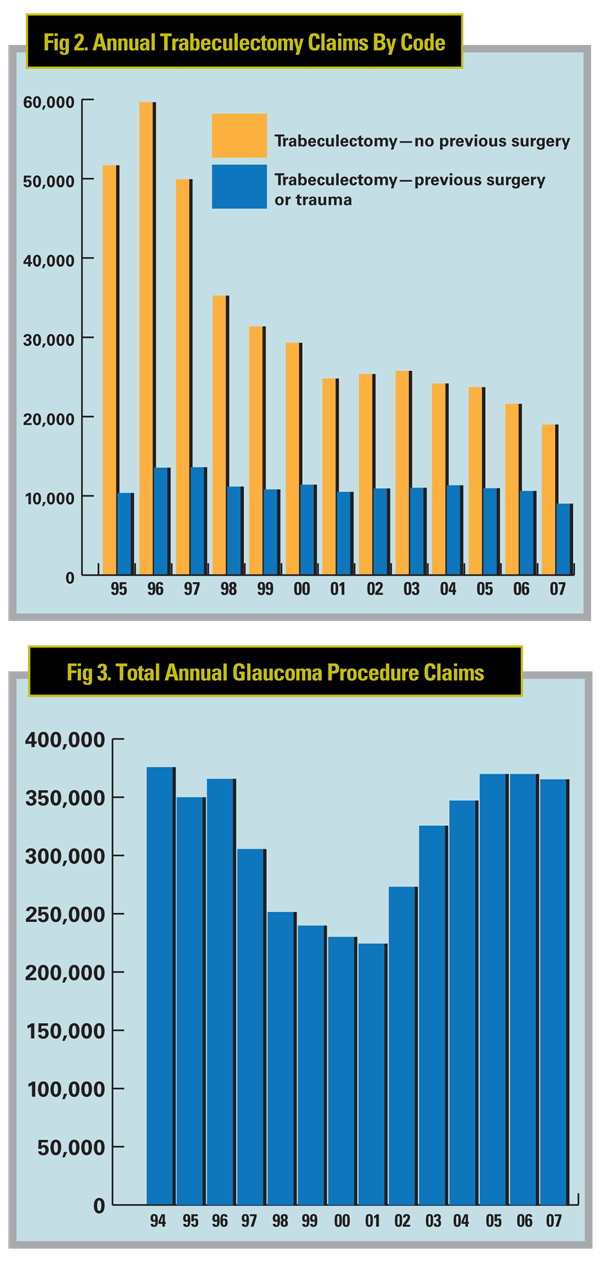
In contrast to trabeculectomies, claims for implantation of aqueous shunts (CPT code 66180) have increased dramatically since 2002. This abrupt increase coincides with the introduction of the Ex-Press shunt in the
In terms of absolute numbers, surgeons are still performing far more laser trabeculoplasties than shunt implantation, but use of aqueous shunts is on the rise. The relative comparison to trabeculectomy is particularly striking: in 1995, trabeculectomy claims outnumbered aqueous shunt claims by a factor of 23 to 1; by 2007, the former only outnumbered the latter by a factor of 3 to 1.
The trends for cyclophotocoagulation (CPT code 66710) are a little difficult to interpret because more than one procedure is subsumed under this category. Even so, much of the gradual increase in the number of claims using this code can be attributed to the growing popularity of endoscopic cyclophotocoagulation as an adjunct to cataract surgery. In 2005, this received its own CPT code (66711), and as the chart shows, once this procedure was separated from the others, claims for the original code dropped, while claims for endoscopic cyclophotocoagulation have only increased. Although the overall number of ECP claims filed was still relatively small in 2007, the number nearly doubled in the three years after it was assigned its own code.
Surgical Options: Present and Future
Figure 3 shows the over- all number of Medicare Part B claims for glaucoma procedures by year. During the first half of the studied period, the total number of glaucoma surgical procedures declined in each year, but the trend line reversed in 2002, increased through 2005 and then flattened thereafter. Given that the Medicare population being treated has steadily increased in size throughout this time period, this data suggests a waxing and waning of clinicians' preference for treating glaucoma with surgery.
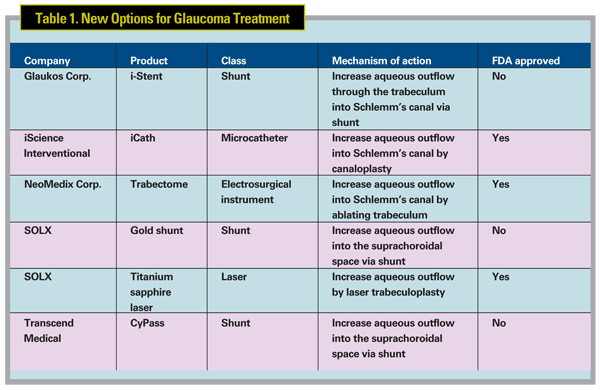
What percentage of glaucomatous eyes are being treated surgically? In a country with an estimated 3 million patients who have glaucoma, comprising 1.5 million identified patients and an equal number of unidentified patients, for a total of about 6 million eyes with glaucoma, there were 365,000 operations for glaucoma in 2007 on Medicare beneficiaries and a guesstimated 70,000 more procedures on non-Medicare patients. That means that only about 7 percent of all glaucomatous eyes received surgical treatment.
So what's likely to happen in the upcoming years? Looking at the newest surgical options (see Table 1, above), some of which are still awaiting FDA approval, glaucoma surgery is on the cusp of a transformation. While it's impossible to know which alternatives will eventually have the most impact on clinicians' treatment choices, it's worth noting that three of these new options are shunts, indicating a great deal of interest and financial investment in this approach to treatment.
Based on that reality, and the growth in use of the Ex-Press shunt, it seems likely that glaucoma surgery will move more and more in this direction, at least in the foreseeable future.
Mr. Corcoran is president of Corcoran Consulting Group. He can be reached at 1-(800)-399-6565, or at kcorcoran@corcoranccg.com.



