In the clinical setting, neovascular age-related macular degeneration is commonly treated with an intravitreal syringe and a vial of anti-VEGF drug. However, it's also possible to treat the disease with a subretinal pic, forceps and a micropipette.1 In a recent study, a majority of wet AMD patients receiving autologous retinal pigment epithelium transplants gained two or more lines of visual acuity postoperatively.2 Although RPE transplantation is performed infrequently today, stem cell technology may have the potential to make the procedure more common. Here's a look at how stem cells might enhance RPE transplants.
RPE and Photoreceptors
Cleanliness can be important to health in general, and retinal health in particular. In the eye the tips of photoreceptor outer segments (OS) are discarded and replaced in a continuous cycle that repeats about every nine days.3 The cycle of photoreceptor OS death and rebirth is propelled, in part, by the RPE, which phagocytoses the OS and recycles retinoids and membrane lipids. The RPE's role as a garbage collector and recycler may seem humble, but it's essential to photoreceptor survival.3
Some retinal pathologies are related to the ingestion or digestion of photoreceptor
If the RPE is incapable of doing its job because of retinal pathology, some researchers theorize that perhaps replacing dysfunctional RPE with functional RPE can reduce photoreceptor loss. That's the theory behind RPE transplantation.
Autologous and Allogenic Transplantation
The success of RPE transplantation depends largely on the origin of introduced RPE cells. Autologous transplants taken from the patient's own eye and allogenic transplants using foreign cells have dramatically different patient outcomes.
One method of autologous RPE transplantation for cases of wet AMD involves a pars plana vitrectomy and two retinotomies.1 In the first retinotomy, the surgeon dissects and removes the damaged subfoveal membrane with forceps. In the second retinotomy, the surgeon gently removes RPE cells in a different region of the retina with a blunt instrument and aspirates them out of the eye with a micropipette. The surgeon then deposits the suspension of harvested RPE cells into the subretinal space that was created by the first retinotomy.
Using this RPE transplantation method, Susanne Binder, MD, a surgeon at the Rudolph Foundation clinic in
Allografts have been less effective in these transplants. In 1990, a group of researchers treated AMD patients with RPE allografts using patch or suspension techniques. After three months, all five wet AMD patients showed signs of graft rejection, and after 20 months most (five out of nine) grafts in dry AMD patients appeared to have been rejected.7
The words "transplantation" and "risk of rejection" are often spoken in the same breath. For ophthalmic transplants, the risk of rejection can be low, however. In 1948, researchers discovered homologous skin tissue grafts in the anterior chamber of the eye were not rejected.8 This immune privilege has been seen in other regions of the eye, including the RPE. Neonatal RPE sheets seem to retain an inherent immune privilege when they are transplanted in heterotopic sites such as the anterior chamber and the underside of the mouse kidney.9 Since the RPE forms the outer layer of the blood retinal barrier, RPE disruption by CNV pathogenesis or surgery may compromise ocular immune privilege, leading to graft rejection.7,10
Both allogenic and autologous transplants have disadvantages. Allogenic transplants may be rejected,7 and autologous RPE may already be impaired by existing disease. Also, patients with large central retinal atrophy may not have enough functional RPE to donate to themselves. In 2006, Raymond Lund, PhD, professor at the
hES RPE
Pluripotentiality is part of the promise and the problem of hES transplantation. How can a specific type of cell needed for transplantation be created from a cell that has not decided which part of the body it will become?
The RPE is originally descended from ectodermal cells that are destined to develop along a neuronal path. The question, "What controls fate?" is not entirely philosophical in embryology, and in 1924 a group of German scientists found a biological answer to this question.11 Human embryos contain a region called Spemann's organizer, which appears to direct the ectoderm to form a neurologic epithelium.12 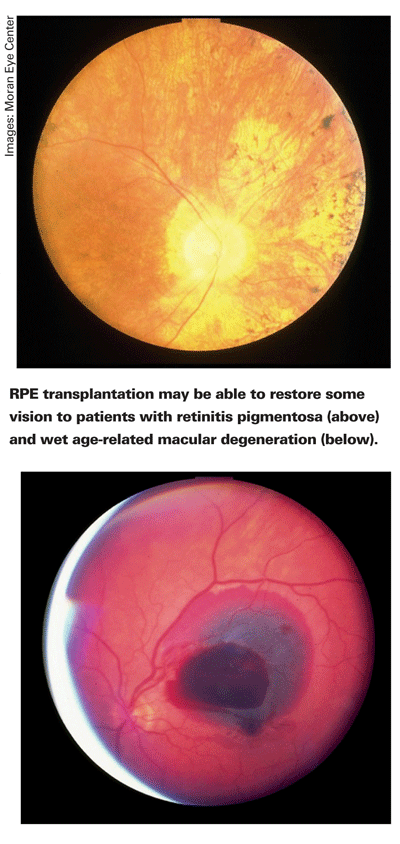
But the question then becomes: How exactly does Spemann's organizer direct neural induction? Initially, researchers studying the process believed molecules secreted by the organizer, such as noggin, follistatin and chordin, were solely responsible for neural induction.13 According to a new theory, ectodermal cells will automatically adopt a neural development fate as a result of the inhibition of the bone morphogenic protein signaling pathway.13
Researchers demonstrated this theory of neural induction with plates and serum free-cultures in 2006.14 Because of the default path of neural induction, the investigators reported, hES cells will spontaneously differentiate into RPE cells after six to eight weeks.14
In a well-publicized study in the fall of 2006, Dr. Lund and his colleagues pushed the stem cell debate closer to the realm of clinical ophthalmology.15 Dr. Lund's study, which measured the effect of subretinal injections of cultured hES-RPE cells, was done using the RCS rat model of retinal dystrophy.
To create transplantable RPE cells, the scientists moved the hES cells from medium to medium and from culture to culture. The most crucial step in cell development didn't require any intervention, however. The hES cells spontaneously differentiated into RPE cells using a default path of neural induction.
After subretinally injecting hES-derived RPE cells into the eyes of RCS rats, Dr. Lund's group reported visual improvement in some of the animals.15 After injection, the responses on an electroretinogram were significantly better for hES-RPE-treated rats (p<0.05), compared to sham for both the a-wave (31 ±27 vs. 6 ±17 µV) and the b-wave (108 ±46 vs. 36 ±33 µV). Optomotor acuity showed hES-treated rats were approximately 50 to 100 percent better (p<0.05) at tracking a moving stimulus with their eyes, compared to sham and untreated controls, respectively.
Stem cells are full of the theoretical power of possibility. Some of stem cells' possibilities are more practical than others, however. For example, homotypic stem cell transplants meant to replace photoreceptors have failed to integrate with host tissue in one published study.16 To improve visual function, photoreceptor graft synapses would have to connect to host synapses, thus completing the neural circuitry. Since the RPE is not part of the neural retina, there are no complicated neural connectivity problems involved with hES-RPE transplantation.
In short, human epithelial stem cell-derived RPE transplantation may be more feasible than other applications of hES technology. Although hES-RPE transplantation hasn't been performed in humans yet, autologous transplant successes by Dr. Binder and others have validated the concept of RPE transplants. RPE transplantation therapies, in other words, are already here, and they may be about to get better.
Dr. Abelson, an associate clinical professor of ophthalmology at
1. Binder S, Stolba U, et al. Transplantation of autologous retinal pigment epithelium in eyes with foveal neovascularization resulting from age-related macular degeneration: A pilot study. Am J Ophthalmol 2002;133:2:215-25.
2. Binder, S, Krebs I, et al. Outcome of transplantation of autologous retinal pigment epithelium in age-related macular degeneration: A prospective trial. Invest Ophthalmol Vis Sci 2004;45:11:4151-60.
3. D"Cruz PM, Yasumura D, et al. Mutation of the receptor tyrosine kinase gene Mertk in the retinal dystrophic RCS rat. Hum Mol Genet 2000;9:4:645-51.
4. Young, RW. Pathophysiology of age-related macular degeneration. Surv Ophthalmol 1987;31:5:291-306.
5. Gal A, Li Y, et al. Mutations in MERTK, the human orthologue of the RCS rat retinal dystrophy gene, cause retinitis pigmentosa. Nat Genet 2000;26;3:270-1.
6. Ryan SJ,
7. Algvere, PV, Gouras P, et al. Long-term outcome of RPE allografts in non-immunosuppressed patients with AMD. Eur J Ophthalmol 1999;9:3:217-30.
8. Medawar P. Immunity to homologous grafted skin. Br J Exp Pathol 1948;29:58-69.
9. Wenkel, H Streilein JW. Evidence that retinal pigment epithelium functions as an immune-privileged tissue. Invest Ophthalmol Vis Sci 2000;41:11:3467-73.
10. Thurmann G, Hoffman S, Hinton DR. Cell Biology of the Retinal Pigment Epithelium. In:
11. Spemann H, Mangold H. Uber Induktion von Embryonanlagen durch Implantation artfremder Organisatoren. Wilholm Roux Arch Entw Mech Organ 1924;100:599-638.
12. Kintner C, Lumsden A. Neural Induction and Pattern Formation. In: Zigmond MJ, Bloom FE,
13. Munoz-Sanjuan I, Brivanlou AH. Neural induction, the default model and embryonic stem cells. Nat Rev Neurosci 2002;3:4:271-80.
14. Klimanskaya I. Retinal pigment epithelium. Methods Enzymol 2006;418:169-94.
15. Lund RD, Wang S, et al. Human embryonic stem cell-derived cells rescue visual function in dystrophic RCS rats. Cloning Stem Cells 2006;8:3:189-99.
16. Gullapalli VK, Khodair MA, Want H, et al. Retinal pigment epithelium and photoreceptor transplantation frontiers. In:



