 |
These are just some of the results from this month’s e-survey on cataract surgery techniques. This month, 927 of the 7,899 surgeons on our electronic mailing list opened the survey (11.7-percent open rate) and, of those, 81 completed the survey. Read on to see how your standards and practices jibe with theirs.
Intraoperative Tweaking
Surgeons may be warming up to the idea of checking their patients’ intraocular lens powers during the cataract procedure via intraoperative aberrometry.
On this year’s survey, 28 percent of the respondents report using intraoperative aberrometry, vs. just 15 percent last year. A lot of them emphasize the technology’s benefits for challenging cases. “Benefits: added comfort of accurate lens selection when it agrees with optical and manual biometry; it’s extremely useful in post-refractive patients and high myopes; and it’s excellent in guiding toric IOL axis,” avers Howard Beach, N.Y., ophthalmologist Brian Collett.
“Shortcomings: Needs clear media and it relies on accurate axial length and keratometry readings.”
Anjali Tannan, MD, of Chicago, concurs with those who see its benefits in certain cases, “It’s great for post-refractive patients,” Dr. Tannan says. “Those are the only patients on whom I use it.”
“Its benefits are that
 |
Though some surgeons are positive regarding intraoperative aberrometry, others are more circumspect. “The accuracy of sphere and axis alignment are good,” says a surgeon from Indiana. “However, the [predicted] power in refractive surgery cases is not as good as anticipated.” A surgeon from Texas doesn’t see a lot of situations where it would be put to use at his practice. “It’s time-consuming, involves cumbersome equipment and the measurements are taken under artificial conditions,” he says. “As for benefits, it can help in decision-making when you’re truly uncertain.” Another Texan quips: “It’s too cumbersome and time-consuming, with little obvious benefit.”
Other Innovations
In addition to intraoperative aberrometry, surgeons weighed in on several new techniques and modalities being applied to cataract surgery.
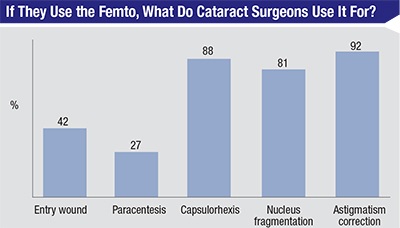
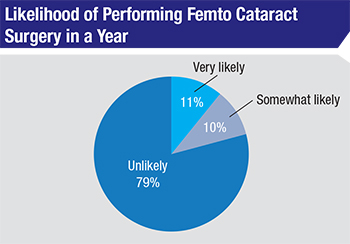
• Femtosecond-assisted cataract surgery. The percentage of surgeons on the survey who say they use the femtosecond laser for at least one step of cataract surgery stayed roughly the same as last year (32 percent vs. 36 percent in 2016). Their usage pattern on the survey has changed, however.
Last year, the entry wound and paracentesis were performed with the femtosecond by 57 percent and 43 percent of respondents, respectively. On the current survey, this has dropped to 42 percent and 27 percent. The percentages of surgeons who use it for the other steps of surgery appear in the graph.
Clint Simpson, MD, of Lansing, Mich., thinks of femtosecond in this way: “My dislikes are the cost to patients, the fact that it slows surgical operation time by 20 to 30 percent, and involves a more challenging cortex removal,” he says. “My likes are the consistent astigmatism correction nomograms and the perfectly centered rhexis. It’s very helpful for traumatic lens cases, dense lens cases and weak zonule cases.” New York’s Dr. Collett sees some benefits, as well. “It’s good for firm cataracts,” he says. “It’s also excellent for AK incisions and astigmatism reduction. It makes a perfect capsulorhexis. However, you can’t use it with central corneal scars.” A surgeon from Virginia also likes femtosecond technology. “It makes taking the cataract out much easier,” he says. “It helps with the critical stage of the capsulorhexis and it’s predictable.”
 |
Other surgeons on the survey, however, aren’t as eager to go down the femtosecond road. “It’s a solution looking for a problem,” opines John Willer, MD, of The Dalles, Ore. A surgeon from Virginia has trouble seeing the benefit. “I’m not sure the results are any better according to surgeons who have used both,” he says. Stewart Gallaway, MD, of Crossville, Tenn., feels similarly, saying, “The accuracy of the corneal relaxing incisions is the only positive. The increased time and cost for little added benefit is the negative.” A surgeon from Texas feels it gives “non-superior visual results and it’s not any safer than manual phacoemulsification cataract extraction; it’s also very costly technology.”
• Managing miosis. For patients whose pupils won’t cooperate, surgeons have some options. The most popular of these on the survey is an intracameral injection of epinephrine/lidocaine, chosen by 54 percent of the respondents. Eleven percent say they use Omidria (phenylephrine and ketorolac injection, Omeros) and 24 percent say they don’t take any additional steps to promote a wide pupil during cataract surgery. Twelve percent choose some other approach to keeping the pupil manageable.
• Sedation. To accomplish preop sedation, the vast majority of the respondents (95 percent) still use intravenous sedation. Three percent say they use Imprimis’ MKO Melt (compounded midazolam, ketamine HCl and ondansetron given sub-lingually). Three percent say they use another kind of method for sedation.
Dealing with Astigmatism
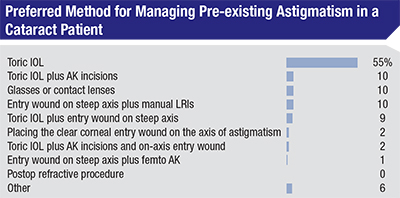
When the surgeons on the survey are faced with a patient with astigmatism, a toric IOL remains the most popular choice, chosen by 55 percent of respondents. Other popular options include combining a toric IOL with AK incisions (10 percent) and placing the entry wound on the steep axis as well as placing manual limbal relaxing incisions (10 percent). The rest of the astigmatism correction results appear in the graph.
 |
A surgeon from Texas says toric lenses provide “proven results, ease of technique, reasonable amount of additional time invested and no deleterious effects on quality of vision.” David Flug, MD, of New York City says, “If your average preop vision is 20/60 or worse, a toric IOL does the job; if your average preop vision is 20/25 you need to get the astigmatism down to less than a half-diopter of cylinder (and you also need to rethink what you’re doing in surgery).” A surgeon from Texas says that placing the entry wound on the steep axis and combining it with a femtosecond AK is his preferred option. “With that, the correction is accomplished easily,” he avers. “For larger degrees of astigmatic correction, a toric lens is necessary. I place the incision on the axis of cylinder to reduce the toric power necessary for correction.” Michigan’s Dr. Simpson says it’s not a one-size-fits all situation, but instead depends on how much astigmatism the surgeon is faced with. “I usually manage 0.5 to 0.75 D with the main incision placed on the steep axis,” he says. “I manage 0.75 to 1.25 D with a temporal incision and paired femto astigmatic keratotomy. I manage anything from 1.5 to 4.5 D with toric IOLs. If the patient has over 4.5 D then I use a toric lens along with femto AK.”
• Postop infection and inflammation prophylaxis. In this arena, the latest movement in some circles is toward dropless (injections) or less-drops (combined drugs in one bottle).
 |
Surgical Pearls
Surgeons also took time to share their tips and techniques for getting the best outcomes with cataract surgery.
Some of the surgeons gave advice on how to be in the proper mindset for surgery. Jonathan B Rubenstein, MD, vice-chairman and Deutsch Professor of Ophthalmology at Rush University Medical Center in Chicago, says, “Have good posture, stay relaxed, and have fun.” A cataract surgeon from California advises his colleages to be “very picky about your ergonomics.” Dr. Willer says to take every case seriously. “Never let your guard down or become complacent,” he admonishes.
Other surgeons provided intraoperative advice. “Dont underestimate the power of verbal anesthesia,” says Dr. Simpson. “Sometimes talking with the patient during the case can be more helpful than any additional IV sedation.” Dr. Collett offers thoughts on incisions. “To make watertight incisions, use a 2.4 mm or smaller keratome, come into the corneal limbus flat in the plane of the iris and then aim slightly up in the corneal stroma but keep the heel of the keratome down,” he says, emphasizing the last point. “You will then enter the chamber with a nice tight, flat and straight cut rather than a V-shaped cut.” Ilan Hartstein, MD, of Los Angeles emphasizes the hydrodissection step. “Hydrodissection should involve rotating the nucleus before trying fracture techniques,” he says, “and holding the cannula down so that fluid egresses from the wound.” Dr. Flug says his best cataract tip doesn’t involve phaco. “My secret weapon is the extracapsular extraction,” he says. “It turns a phaco nightmare/disaster (such as a brunescent lens or loose zonules) into a routine case with great outcomes.”
Finally, a surgeon from New Jersey says that, in the end, it’s better to be good than fast. “Take your time with surgery; it’s not a race,” he says. “An extra minute to provide excellent outcomes is much more important.” REVIEW



