Nearly 30 percent of
Diabetic retinopathy is the leading cause of new cases of legal blindness among adults 20 to 74 years of age in the
Xinzhi Zhang, MD, PhD, of the Centers for Disease Control and Prevention, and colleagues conducted a study to determine the most recent prevalence and risk factors of diabetic retinopathy in the U.S. population ages 40 years and older. The study included an analysis of data from a nationally representative sample of the National Health and Nutrition Examination Survey 2005 to 2008 and included 1,006 individuals. Diabetes was defined as a self-report of a previous diagnosis of the disease (excluding gestational diabetes mellitus) or glycated hemoglobin A1c of 6.5 percent or greater. Photographs were taken of each eye to determine and classify diabetic retinopathy. Prevalence estimates were weighted to represent the civilian, noninstitutionalized

The researchers found that from 2005 to 2008 the estimated prevalence of diabetic retinopathy and vision-threatening diabetic retinopathy was 28.5 percent and 4.4 percent, respectively, among persons with diabetes ages 40 years and older. Approximately 31.6 percent of men and 25.7 percent of women with diabetes had diabetic retinopathy.
Also, 26.4 percent of non-Hispanic white individuals, 38.8 percent of non-Hispanic black individuals, and 34 percent of Mexican-American individuals with diabetes had diabetic retinopathy. Approximately 3.2 percent of non-Hispanic white individuals, 9.3 percent of non-Hispanic black individuals and 7.3 percent of Mexican-American individuals with diabetes had vision-threatening diabetic retinopathy.
Further analysis indicated that independent risk factors for diabetic retinopathy include male sex (38.1 percent vs. 27.1 percent), higher HbA1c level, longer diabetes duration, use of insulin (47.4 percent vs. 26.7 percent), and higher systolic blood pressure.
"These estimates provide policy makers updated information for use in planning eye-care services and rehabilitation. With the aging of the population and the increasing proportion of the population with diverse racial/ethnic heritage, the number of cases of diabetic retinopathy and vision-threatening diabetic retinopathy will likely increase.
Furthermore, the need for eye care and for culturally appropriate interventions that can reduce disparity and improve access to eye care among diverse populations is also likely to increase," the authors conclude.
BMI in Women Tied to
Maintaining a healthybody weight is important for avoiding many diseases, but a new study from the Massachusetts Eye and Ear Infirmary finds that for primary open-angle glaucoma, the picture may be more complex. A large, prospective MEEI study, conducted over 20-plus years, found that higher body weight (specifically, body mass index) is not associated with higher risk of POAG. In fact, the research shows that in women, higher BMI is significantly linked to reduced risk for normal tension glaucoma. The researchers, led by Louis R. Pasquale, MD, say that clinicians and patients should be cautious about these findings until further research provides substantiation and clarifies the related biological mechanisms.
"Understanding the mechanisms that drive BMI and other body composition factors in relation to POAG might help us solve some mysteries connected with this complex illness," Dr. Pasquale said. "It's reasonable to speculate that hormonally controlled factors released from adipose or lean tissues may alter the risk of NTG in women. Higher BMI in postmenopausal women is linked with higher estrogen levels, which might positively affect estrogen receptors in the optic nerve," he explained.
The study participants were 78,777 women enrolled in the Nurses Health Study (1980 through 2004) and 41,352 men enrolled in the Health Professionals Follow-up Study (1986 through 2004). In women, each unit increase in BMI was associated with a 6 percent reduction in risk for NTG (defined as intraocular pressure equal to or less than 21 mmHg at the time of diagnosis of POAG). Also, in women, having higher BMI during the young adult years was associated with reduced risk of NTG. In men, BMI was not associated with POAG. Because the ethnicity of most participants was European-Caucasian, the study's implications may be limited to similar patient populations.
Dr. Pasquale suggested that if the relationship of POAG to BMI and related body-composition factors can be clarified in future research, new treatments could be developed for patients with POAG, particularly those who have the normal tension variant of the disease.

Tufts Group: Gene Therapy May Delay Some Eye Diseases
Researchers at
"Our work shows that it is possible to attain therapeutic results using non-viral gene delivery methods, specifically, nanoparticles. Nanoparticles, which are small enough to penetrate cells and stable enough to protect DNA, are capable of preventing retinal cell death and preserving vision," said senior author Rajendra Kumar-Singh, PhD, associate professor of ophthalmology at Tufts University School of Medicine and on faculty at the Sackler School.
"The most common approach to gene therapy involves using a virus to deliver DNA to cells," said Dr. Kumar-Singh. "While viruses are very efficient carriers, they can prompt immune responses that may lead to inflammation, cancer or even death. Non-viral methods offer a safer alternative, but until now, efficiency has been a significant barrier."
In a model simulating the progression of human retinal degeneration, the researchers treated mice with nanoparticles carrying a gene for glial cell line-derived neurotrophic factor (GDNF), a protein known to protect the photoreceptor cells in the eye. Retinas treated with the GDNF-carrying nanoparticles showed significantly less photoreceptor cell death than controls. Preservation of these cells resulted in significantly better eyesight in the treatment group seven days after treatment, compared to controls.
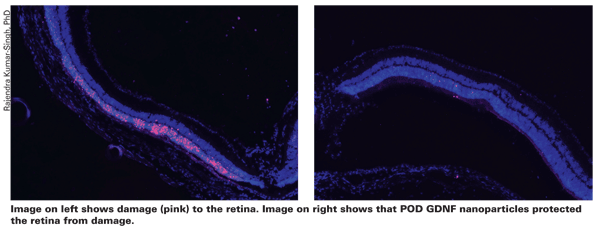
The protection conferred by the GDNF-carrying nanoparticles was temporary, as tests 14 days after treatment showed no difference in eyesight between treated mice and controls.
"The next step in this research is to prolong this protection by adding elements to the DNA that permit its retention in the cell. Bringing forth a more potent and enduring result will move us closer to clinical application of non-viral gene therapy," said Dr. Kumar-Singh.
In a previous study, this same team of researchers developed the gene delivery method used in this research. The researchers showed that a peptide called PEG-POD, which compacts DNA into nanoparticles, delivers genes to the retina more efficiently than other non-viral carriers.
MD Smartphone Adoption Growing Exponentially
A recent survey by the Spy- glass Consulting Group, of
Highlights of the survey include:
• Seventy-eight percent of physicians interviewed were experiencing difficulties accessing and communicating with colleagues in a timely manner. Physicians are busy mobile professionals who are constantly on the go and are not always available when they are needed. Many lack financial incentives to be more accessible because the current fee-for-service reimbursement system encourages physicians to focus on the quantity vs. the quality of health-care delivered. Non-essential phone or e-mail communications with colleagues and patients are seen as non-reimbursable distractions.
• Physicians interviewed report they are overwhelmed by the daily volume of communications received from colleagues, care team members and patients. They lack automated tools to manage voice mail, pager messages, SMS messages and electronic mail. They are forced to continually check separate data silos and manually filter and prioritize communications based upon sender, subject and priority. Critical communications easily fall through the cracks.
• Fifty-six percent of physicians interviewed were concerned about the lack of standardized processes for transitioning care between colleagues. The patient hand-off process used by hospital-based physicians and the patient referral process used by community-based physicians are informal and ad hoc, which can introduce medical errors into the patient-care process.
The report is an outgrowth of a similar study published by Spyglass in November 2006 entitled Trends in Mobile Communications. Content for the current survey was derived from more than 100 in-depth interviews with physicians working in acute care and ambulatory environments nationwide. Physicians interviewed were technically competent and representative of a broad range of medical specialties, organization types and organization sizes. The telephone interviews were conducted over a three-month period starting in March 2010.
For information on the report, Point of Care Communications for Physicians, visit
spyglass-consulting.com. And for more on smartphone use in ophthalmology, see p. 30.



