Help With Billing
One app many ophthalmologists may find useful is OphthoBilling (currently available at the Apple App Store). OphthoBilling was developed in 2015 by Renelle Lim, MD, during her fellowship training on the Oncology Service at Wills Eye Hospital in Philadelphia. “Traditional coding resources involve a computer or multi-volume book sets,” she says. “I wanted to create something that makes this information more readily available.”
Dr. Lim explains that the OphthoBilling app helps the user select both CPT (procedural) and ICD-10 (diagnosis) codes. “You can type in a keyword, type in the numerical code or just scroll to find the available codes,” she explains. “The app will tell you which codes can be used together and which cannot. OphthoBilling is especially helpful for the physician in the operating room or a surgeon who operates at multiple locations.”
Dr. Lim says the app has a straightforward interface and is very user-friendly. “It takes the guesswork out of billing and should reduce the number of errors and rejections from insurance companies,” she says. “The app can be a valuable tool for both ophthalmologists and billing assistants. It encourages physicians to take a more hands-on approach to billing, and it offers surgeons the opportunity to refine a final list of codes that accurately reflects the procedures performed during surgery, since only the surgeon knows the intricate details of each operation. (See examples, facing page.)
“Once all CPT and ICD-10 codes are entered into a list within the OphthoBilling app, it can be texted, air-printed or e-mailed,” she adds. “The app creates an automatically tabulated list and displays the relative value units, giving the user an indication of reimbursement. Each surgeon can also create customized lists of codes based on the scope of the practice.”
Dr. Lim says the OphthoBilling app is currently available on the App Store for $99.99. You can view an introductory video online at https://www.youtube.com/watch?v=gGffMvjfHWk.
Managing Surgical Data
Anil Shivaram, MD, a cataract and refractive surgeon in Claremont, Calif., is part of a team working with Bausch + Lomb, IBM and Apple to create a multipurpose app that will help cataract surgeons manage surgery-related data in multiple ways. “This app is intended to help optimize outcomes in cataract surgery by capturing and organizing preoperative data and making it available to the surgeon in the OR,” he says. “Even more exciting, it will also capture postoperative data and analyze all of it to help the surgeon refine constants, lens selection and surgical choices.
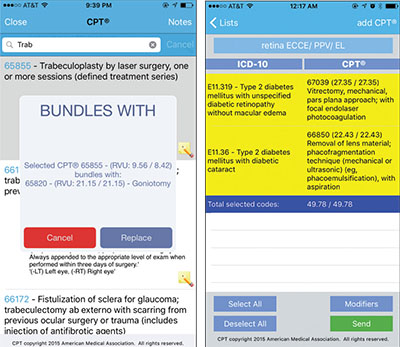 |
| Two examples of the OphthoBilling App in use. Left: The app notifies the user when two codes can be bundled. Here, the user prepares to list trabeculoplasty (CPT 65855) as part of the surgery being coded; the OphthoBilling app alerts the user that goniotomy (CPT 65820)—which was was already in a list of options created by the user—can be bundled with it. The user can choose to replace the original CPT code or simply cancel. Relative Value Units are also displayed. Right: An example of a list created by a user. The sum of the RVUs is listed, and the list title can be customized. |
“Preoperatively, we do a number of tests to collect data such as axial length, keratometry and OCT scans,” Dr. Shivaram notes. “This is often done in a piecemeal way using different manufacturers’ instruments. Collecting, ensuring the accuracy and organizing the data can be messy, and having access to it in the operating room may involve—for some surgeons at least—having a lot of sticky tags or printouts taped to the wall. With this app, the surgeon will be able to simply take a photograph of each printout, onscreen test result or scan. Image recognition software will pull out and organize the numbers while saving images such as scans and topographies. This will reduce transcription errors and pool all of a patient’s data in one place that can be digitally accessed in the OR, via something like a digital tablet. That information can also be easily accessed later if you’re doing the patient’s second eye, for example. The app will show you the result of the first eye’s surgery, to help you decide what you want to do with the second eye.”
Dr. Shivaram acknowledges that optical character recognition could potentially introduce errors, at least compared to a direct digital transfer of data. “We’re conducting a pilot study to determine the level of accuracy of this approach,” he says. “The advantage of having optical character recognition functionality is that there are a variety of machines out there being used by surgeons. This app will allow you to collect the data from any instrument without the need for an additional electronic tool or hookup. The app will also allow the surgeon to make manual changes to the data because sometimes, even with the correct data captured, a surgeon may wish to make adjustments.”
Dr. Shivaram notes that some surgeons take the time to analyze all of their data in order to refine their technique and generate better outcomes. “Since I was a resident I’ve been keeping an Excel spreadsheet tracking every single case I’ve ever done,” he says. “It’s become rather massive. It enables me to see exactly how my choices affect my outcomes with each lens I use, but doing this manually can take a lot of time and effort. If you have an app that integrates all of this data and analyzes it for you, you can optimize your outcomes without having to do the regression analysis on your own.
“For example, at postoperative visits, the data will compare the current measurements to your preoperative prediction,” he continues. “You’ve told it which lens you used, your preferred incision location and so forth. Over time it will refine your constants based on this information and make suggestions to reduce astigmatism and refine your outcomes. That’s a big deal, because many surgeons just use a standard A-constant and never refine it. Customizing those factors based on your individual results could go a long way toward improving your results, but it’s a tall order if you don’t have a meaningful way of accessing and crunching and analyzing the numbers. Given the serious computing power these companies bring to the table, the app can easily do a large, pooled analysis to help determine things like the effective lens position for different lenses and the relative importance of lens thickness or anterior chamber depth.
“At the end of the day, we really want to get LASIK-like outcomes with our cataract surgery,” he notes. “Patients, especially in the age of refractive surgery, are expecting results closer to your target. Using a data-driven process like this pushes us closer to being able to achieve that.”
Dr. Shivaram says the team will be conducting the aforementioned pilot study starting before the end of the year. “The study will test a number of things,” he says. “First, it will see how valid the software’s recommendations are, using a pool of data we’re collecting. For example, is it successfully optimizing each surgeon’s constants? Second, it will compare the efficiency of using the app versus not using it. How much more efficient are you when you have all of this data in one location? Does it save time in the OR? Third, we’ll see whether the app is reducing data input error.
“In the future, we plan to fully utilize the functions of the Apple devices and the security and cognitive computing power of the IBM Cloud services,” he adds. “This app will be the framework on which more ophthalmic services can be deployed. It will take a number of processes that are onerous and time-consuming for the surgeon and make them a lot easier and less error-prone.”
Alexander Faust, an associate partner at Global Business Services—a subsidiary of IBM—who is also working on the project, says IBM is excited to be working with Dr. Shivaram, along with a select group of opinion-leading surgeons and the Bausch + Lomb team. “Our goal,” he says, “is to collaborate with these medical professionals to drive an enhanced quality of patient surgical eye care by delivering a mobile, digital transformation in ophthalmology.”
Andy Chang, senior vice president and general manager, U.S. Surgical, Bausch + Lomb agrees. “Working in collaboration with industry experts IBM and Apple, our goal is to help simplify a cataract surgeon’s ability to achieve target refractive outcomes by providing more intelligent recommendations through the mobile integration of diagnostic data and information,” he says. “Combining the diagnostics in one place and delivering personalized IOL recommendations that fit each individual will ultimately help surgeons make better, more-informed decisions for their patients; it will also increase efficiency by reducing the time needed for data transfer and manual computing, as well as limiting the risk of human error.”
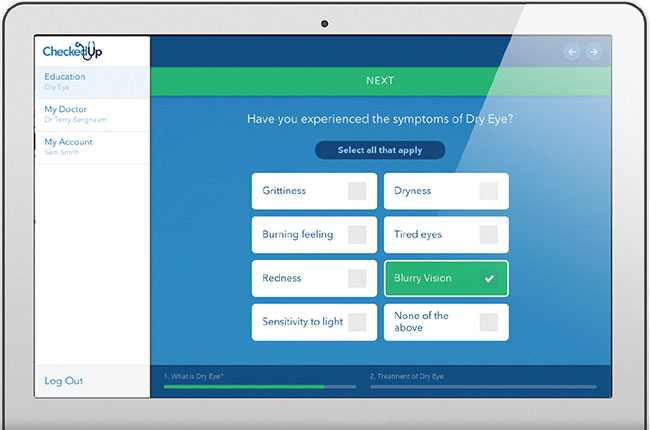 |
| Sample screen from the CheckedUp app, designed to allow patients to access doctor selected content, while eliciting useful information about the patient’s condition that is then forwarded to the practice. New topics, including dry eye, have recently been added. |
A prototype of the app should be completed by the end of the year.
CheckedUp Adds New Content
CheckedUp is a customizable digital platform that allows doctors to give patients access to information about their condition and treatment—before or after seeing the doctor—at home via smartphone, computer or tablet, or in-clinic via kiosks. Originally focused on cataract surgery, the program has recently added multiple new topics and has also increased its functionality.
As before, all content is interactive; the platform provides information to the patient and allows the patient to provide feedback that’s forwarded to the doctor prior to the office visit. The material patients can access can be customized for each surgeon, so patients see exactly what the doctor wants them to see, and the content is constantly being upgraded based on feedback from practices. CheckedUp also includes a follow-up component; it provides data metrics to the practice showing how the program is doing at engaging and educating the patient and how adherent the patient is.
“We’ve recently added a dry-eye platform,” says Richard M. Awdeh, MD, assistant professor of clinical ophthalmology and assistant professor of ophthalmology and pathology at the Bascom Palmer Eye Institute in Miami, creator of the CheckedUp platform. “In addition to answering patient questions, it can help prequalify patients for any premium practice offerings, such as diagnostic tools or types of treatment. CheckedUp also now has educational material for patients diagnosed with many ophthalmic conditions such as glaucoma, macular degeneration or blepharitis, and for patients interested in procedures such as LASIK.”
Dr. Awdeh notes that getting information from the patient outside the office can result in a higher-quality consultation. “The doctor can see which content the patient looked at and the answers the patient gave to the questions before the patient is in the examination room,” he says. “Doctors and other staff members are already informed about the patient’s questions, objectives, concerns, level of education regarding the topic and any symptoms the patient may be experiencing. Meanwhile, being able to access the appropriate information outside the office means patients can refer back to the content at any time, and they’re able to share it with family and friends.” REVIEW
Dr. Shivaram is a consultant for Bausch + Lomb. Dr. Awdeh has a financial interest in CheckedUp.



