Patients with narrow angles can have different presentations, ranging from acute angle-closure attack to anatomical narrow angles without evidence of glaucoma, making management a challenge. In this article, we'll describe our approach to these cases, including a discussion of narrow-angle and angle-closure glaucoma and iridotomy technique tips.
Narrow Angles
The term narrow angle refers to an anatomical condition in which there is irido-trabecular apposition caused by any number of factors. The incidence of narrow-angle glaucoma in the general population is around 1 percent, increasing in Inuit Eskimo and East Asian individuals.
It's important to note that not every narrow angle is occludable. This makes the history and exam vital in diagnosing patients who are at greatest risk for developing angle-closure glaucoma. The risk factors for developing primary angle-closure glaucoma are:
• increasing age;• increasing lens thickness;• female gender;• hyperopia; and• ethnicity (i.e., Inuit Eskimo, East Asian).
There are different mechanisms for acute angle-closure glaucoma, but we will discuss the more common ones: pupillary block and lens-induced glaucoma.
Acute Angle Closure
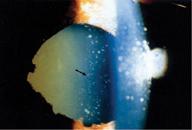
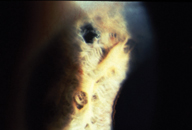
Acute angle-closure glaucoma is characterized by rapid increase in intraocular pressure. A patient suffering from acute angle closure will usually present with severe pain, tearing, photophobia, blurry vision, halos around lights, corneal edema, a fixed mid-dilated pupil and intraocular pressure of 50-70 mmHg.
|
If the clinician isn't able to break the attack and lower the IOP medically, pressure indentation on the cornea with a gonioscopy lens (Zeiss or Posner 4-mirror lens) can be effective in some cases.
If these methods aren't helpful, some physicians advocate making an anterior-chamber paracentesis. This approach doesn't treat the problem permanently, but can lower IOP enough for medications like pilocarpine to be effective, since IOP lowering drugs tend to work better when IOP is below 30 mmHg. However, the danger of creating a paracentesis is that the clinician can flatten the anterior chamber. To avoid this complication, we recommend using a 30-ga. needle on a TB syringe without the plunger. Direct the tip of the needle either to the six or 12 o'clock position to avoid touching the lens. Once in the anterior chamber, the physician can control the amount of aqueous that is released.
If the IOP is lower and the corneal edema improves, the clinician should re-examine the angle gonioscopically to determine if the closure is appositional only or if there is peripheral anterior synechiae (PAS) formation. If the angle is still open (i.e., with, at most, minimal PAS), the surgeon can perform a laser iridotomy. If, however, the narrow-angle reflects a long-standing condition, and there are extensive areas of PAS formation, an iridotomy may not solve the problem. In these cases, the clinician may need to consider glaucoma filtration surgery.
It's also important to evaluate the fellow eye, since it's at risk for developing angle-closure glaucoma. In most cases, the fellow will also have a narrow angle, and it's often prudent to perform a prophylactic peripheral iridotomy in the fellow eye to prevent potential attacks in the future. If the fellow has a deep angle, then the patient should be evaluated for a non-pupillary block mechanism of glaucoma.
An angle-closure attack can also be precipitated by an intumescent cataract. As the cataract gets larger, the angle can markedly narrow, and some surgeons feel that removing the lens may deepen the anterior chamber sufficiently, avoiding peripheral iridotomy. Though lens removal isn't for every patient, there are cases in which the narrow angles have a phacomorphic component in which the lens pushes up on the iris. Cataract surgery can be a viable option in these patients.
Intermittent Angle Closure
There are also patients who have intermittent episodes of angle closure that resolve between attacks. Through the years, these attacks may or may not cause symptoms such as headache, eye pain or occasional halos around lights. Over time, these episodes result in PAS that can cause permanent elevation of IOP (chronic angle-closure glaucoma).
The patient with intermittent angle-closure glaucoma can be a challenge to diagnose because he may have normal IOP between episodes. Since the recurrent symptoms will resolve between attacks, and may not be present during the exam, the physician may need to ask the patient about these symptoms to diagnose intermittent angle closure.
|
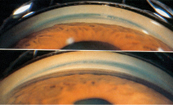
If the patient answers affirmatively regarding the history of any of these triggers, proceed to a Van Herick grading of the peripheral anterior chamber depth at the slit lamp. This is a quick way to gauge the width of the angle that involves bringing the slit beam at an angle of 60 degrees onto the cornea just anterior to the limbus. The clinician estimates the anterior chamber depth between the peripheral iris and the corneal endothelium and compares it to the overall thickness of the cornea. Here's a guide to the Van Herick findings:
• Grade 0 is used to describe peripheral iridocorneal contact.• Grade I is a space between the iris and corneal endothelium of less than one fourth the corneal thickness.• In grade II, the space is between one-fourth and half the thickness of the cornea.• Grade III is considered a non-occludable angle, with the distance being equal to or greater than half the corneal thickness.
If the Van Herick grade shows a narrow space between the iris and the endothelium, one should proceed to gonioscopy. To perform effective gonioscopy in these patients, minimize the amount of light that's both in the room and emitted from your slit lamp, because this illumination can actually cause the pupil to constrict and pull the iris away from the angle. In fact, the physician should seek to simulate the patient's pupil size and angle configuration as it is during the times when it's most prone to an attack. Also, the examiner shouldn't put any indentation pressure on the eye, since this can open the angle. This is especially a concern when using the Zeiss or the Posner 4-mirror lens.
|
An optic disc exam will also rule out glaucomatous optic neuropathy as a result of the intermittent attacks.
• Provocative dilation tests. These tests are occasionally useful. They attempt to incite an angle-closure attack in the office, allowing the clinician to make a definitive diagnosis.
The basic test involves dilating the patient. The caveat with this test is, however, that the time the patient is most likely to develop angle closure isn't in the office when his pupil has dilated fully. Instead, the attack is likely to occur hours later, at home, when the pupil is coming back down.
Another more involved, but possibly more reliable, test involves putting the patient in a prone position in a dark room for 30 minutes, and waiting for the pupil to reach a mid-dilated state. The physician re-examines the angle, taking care not to admit too much light.
Chronic Angle-closure Glaucoma
Patients with chronic angle closure glaucoma have persistent high IOPs between 20 and 30 mmHg. On gonioscopy, the angle is often graded 0-I with concurrent PAS.
Here's a review of gonioscopic findings based on the Schaffer scale:
• Grade 0: The iris is against the trabecular meshwork (definite risk of angle closure).• Slit: The angle between the iris and the trabecular meshwork is less than 10 degrees (significant risk of angle closure).• Grade I: The angle is 10 degrees (moderate risk).• Grade II: The angle is 20 degrees (slight risk).• Grade III: The angle is greater than 20 but less than 45 degrees (low risk).• Grade IV: The angle is 45 degrees (no risk).
An optic disc exam is also vital in the chronic patient to determine the extent of glaucomatous damage.
When performing gonioscopy in patients with chronic narrow angles, the clinician must rule out a plateau iris configuration, an important cause of angle closure in people younger than 40. Plateau iris appears to be due to an abnormal rotation of the ciliary body processes that causes a "double-hump" sign on gonioscopy, in which the anterior ciliary body processes are pushing up and causing the peripheral iris to bow forward. To help identify plateau iris, note if the chamber is deep centrally and shallow peripherally, rather than uniformly shallow as in chronic narrow-angle glaucoma.
The physician can make a definitive diagnosis of plateau iris by performing a peripheral laser iridotomy and then re-evaluating the patient. If the angles are still narrow or occludable and the configuration of the peripheral iris is bowed forward, the patient likely has plateau iris. In such cases, the use of pilocarpine and/or peripheral iridoplasty to push the iris away from the angle is indicated. Younger patients often can't tolerate the ocular discomfort or side effects of pilocarpine. In those cases, peripheral iridoplasty may be a more appropriate option.
For the chronic angle-closure patient, a laser iridotomy will most likely be beneficial. After laser iridotomy, the IOP might be still elevated due to PAS or combined-mechanism glaucoma; in these cases, medical therapy may be indicated.
• Phacomorphic causes. Cataract surgery may be indicated if removing the cataract will improve a patient's vision and alleviate the phacomorphic component of the angle-closure glaucoma. One study advocates performing laser iridectomy in patients with intumescent cataract prior to cataract surgery to prevent an acute angle closure glaucoma attack on the operating table.1 Due to this danger, if the surgeon plans to operate on this type of patient, the patient should be the first case that day, because as the pupil starts constricting it may induce an attack.
The Narrow-angle Glaucoma Suspect
This is the most challenging of patients in the narrow-angle spectrum, because the patient simply presents with narrow anatomical angles, but without optic disc damage or a history of intermittent attacks. The clinician is often asked to determine whether or not the anterior chamber angles are occludable and predisposed to angle-closure attacks.
Though a peripheral laser iridotomy is usually the preferred course of action in other types of narrow-angle patients, the decision may not be as clear cut in a narrow-angle patient without history of angle closure. General laser treatment guidelines based on gonioscopic findings are as follows:
• Between Grade 0 and I, most physicians would advocate a laser iridectomy.• Between I and II, the decision to recommend an iridotomy depends on the patient's tolerance for the small risk of angle closure if no laser treatment is done compared to the risks of undergoing the laser iridotomy.• Above II (an opening wider than 20 degrees), most physicians would simply monitor the angle.
If the patient does a lot of international travel, this could impact the physician's decision to perform a laser iridotomy. The concern is that the patient will not be able to quickly get the medical help that he or she needs. Also, examine the optic disc to ensure that there isn't pre-existing glaucomatous damage from previous attacks.
|
Also, the clinician should monitor the patient for a "creeping angle," a condition that often occurs in African-American patients. In this case, the angle appears relatively normal on the first gonioscopic exam, but then slowly gets narrower over time. Unless the clinician performs repeat gonioscopies at the following exams, he or she may miss this condition.
Finally, though there is a broad spectrum of patients with narrow angles, if one diagnoses this condition early enough, laser iridotomy can truly be "curative." With it, you can give these patients many more years of vision.
Dr. Al-Aswad is an assistant professor of clinical ophthalmology in the glaucoma division at Columbia University's Harkness Eye Institute. Dr. Tsai is an associate professor of ophthalmology and director of the glaucoma division at Harkness.
1. Tomey KF, al-Rajhi AA. Neodymium:YAG laser iridotomy in the initial management of phacomorphic glaucoma. Ophthalmology 1992;99:5:660-5.