The researchers of this observational study wanted to measure the impact of CCT, a possible risk factor for glaucoma damage, and corneal hysteresis, a proposed measure of corneal resistance to deformation, on various indicators of glaucoma damage.
Patients of the Wilmer Glaucoma Service at Johns Hopkins University School of Medicine between December 2003 and August 2004 who underwent measurement of hysteresis on the Reichert Ocular Response Analyzer and measurement of CCT by ultrasonic pachymetry were included in the study. Two glaucoma specialists reviewed the charts to determine highest known intraocular pressure, target IOP, diagnosis, number of years with glaucoma, cup-to-disk ratio, mean defect, pattern standard deviation, glaucoma hemifield test, and presence or absence of visual field progression.
Two hundred thirty patients were included in the study (127 females) mean age of the participants was 65 ±14 years. Of those patients, 194, or 85 percent, had a diagnosis of primary open-angle glaucoma or suspected POAG.
Lower corneal hysteresis value (p=0.03), but not CCT, was associated with visual field progression in multivariable generalized estimating equation models. When axial length was included in the model, hysteresis was not a significant risk factor (p=0.09). A thinner CCT (p=0.02), but not hysteresis, was associated with a higher CDR at the most recent examination. Neither CCT nor hysteresis was associated with MD, PSD, or GHT "outside normal limits," the researchers report. They found that thinner CCT was associated with the state of glaucoma damage as indicated by CDR. Axial length and corneal hysteresis were associated with progressive field worsening, the researchers say.
(Am J Ophthalmol 2006141:868-875)
Congdon NG, Broman AT, Bandeen-Roche K, Grover D, Quigley HA.
Acrysof ReStor Full Range Vision, Fewer Spherical Aberrations
The AcrySof ReStor Intraocular Lens provides a satisfactory full range of vision, with less dependence on glasses and less induced spherical aberrations when compared with the AcrySof SA60AT monofocal IOL, say researchers from a Brazilian study. The researchers say ReStor is associated with a more satisfactory quality of life when compared with the monofocal IOL, but with lower contrast sensitivity.
Forty patients (80 eyes) from the Federal University of São Paulo were enrolled into two groups during this prospective, nonrandomized, clinical trial. Twenty-five patients were assigned to the ReStor group and 15 patients to the monofocal group.
The parameters analyzed by the researchers included distance uncorrected and best-corrected visual acuity, near uncorrected and distance corrected visual acuity, intermediate visual acuity, contrast sensitivity (Pelli-Robson Titmus test), reading speed and wavefront measurement using the LADARWave aberrometer. A quality-of-life questionnaire was also administered.
Distance uncorrected and BCVA in the ReStor group were not statistically different from the monofocal group (p=0.66). Near uncorrected and distance corrected visual acuity were statistically better in the ReStor group than the monofocal group (0.16 ±0.13 vs. 0.62 ±0.09, p<0.001, and 0.14 ±0.12 vs. 0.62 ±0.07, p<0.001, respectively). The ReStor group demonstrated fewer spherical aberrations compared with the monofocal group (p<0.001). Monocular photopic contrast sensitivity was statistically lower in the ReStor group (p<0.001). Stereopsis and reading speed were not statistically different between the groups, the researchers report.
(Am J Ophthalmol 2006141:827-832)
Souza CE, Muccioli C, Soriano ES, Chalita MR, Oliveira F, Freitas LL, Meire LP, Tamaki C, Belfort Jr. R.
Most Patients Are Satisfied Post-Myopic LASIK
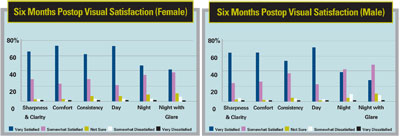
The researcher of a multicenter study says most wavefront-guided LASIK patients were just as satisfied, or more satisfied, with their postop uncorrected visual acuity than with their preoperative BCVA.
The clinical study included subjects recruited from six surgical centers from across the United States. In this retrospective analysis, wavefront-guided LASIK procedures were performed in 274 myopic-astigmatic eyes among the six sites. Comprehensive evaluations of vision and ocular health were conducted preoperatively and for six months postop. Visual acuity and contrast sensitivity were measured, and questionaires were administered. Questionnaire responses were compared with clinical measurements.
The overall distribution shifted toward "more satisfied," according to the researcher. The "very satisfied" population increased by as much as 70 percent in all areas. There was no significant change in frequency of visual symptoms. Patients were more expressive about visual decline than visual improvement, the researcher says. Perception of changes in vision appeared to be related to mesopic contrast sensitivity and mesopic contrast sensitivity under glare. Contact lens wearers were more satisfied with postoperative vision than those who wore glasses. Men were more likely to report visual symptoms and/or complain about night vision, although their changes were the same as those of the women, the researcher says. Residual refractive error was a major predictor for most questionnaire items.
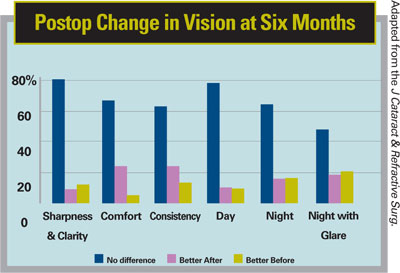
By continuing to minimize postop refractive error through the of nomograms and improved technology, visual complaints such as night glare and halo could be diminished or even eliminated, the researcher, Kuang-mon Ashley Tuan, OD, PhD, FAAO, says.
Some dissatisfaction might be mitigated by being sure patients are educated and have realistic expectations before surgery. Patients need to have a realistic idea of the outcome potential of refractive surgery so that if they experience slight degradation in some areas, disappointment does not outweigh satisfaction with the areas in which their visual performance has improved, she says.
(J Cataract Refract Surg 200632:577-583)
Tuan KmA.