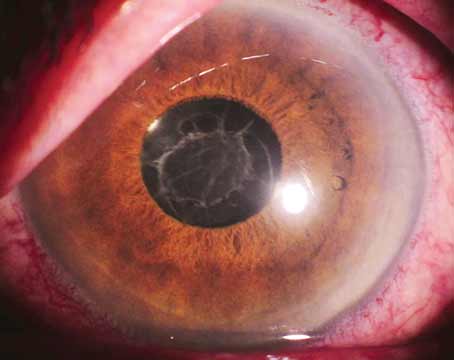
In an effort to remove the microkeratome from the equation, as well as get rid of the need to use alcohol or a blade to remove the epithelium, the Italian company iVIS has developed a laser that is designed and optimized for custom, trans-epithelial ablations. The system can be used for primary refractive surgery cases as well as topographically guided therapeutic treatments for complicated post-refractive surgery eyes. Here's a look at this trans-epithelial system, and how it approaches various procedures.
Going All Laser
The system, called iRES, has a mode called cTEN (custom trans-epithelial, no-touch) that ablates both the epithelium and the stroma in a single procedure.
"To use it, you program a certain epithelial thickness into the laser," explains
Dr. Stojanovic says it's possible to get an exact measurement of the epithelium with the Artemis very-high frequency digital ultrasound unit, but going that route has some drawbacks, as well. "It's expensive and involves an immersion bath," he notes. "This takes time and wouldn't really be practical for virgin-eye cases. However, I have done some cases in which the patient's file had Artemis data in it. Then I could account precisely for the epithelial thickness."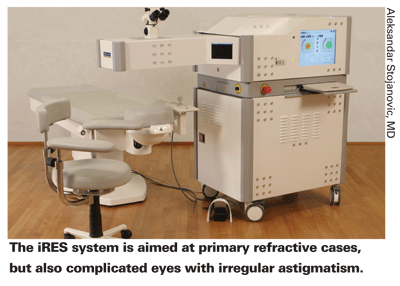
Dr. Stojanovic says performing trans-epithelial ablations helps conserve epithelial tissue in many cases. "You always remove just the right amount of epithelium that you need," he says. "With alcohol or a brush, you always have to remove more to make ample room for the ablation. This removes the exact amount of epithelium you need for the ablation. For instance, if it's an oval shape for a patient with a special need, it will make an oval-shaped ablation removing the amount of epithelium necessary."
Naturally, when a surgeon hears about a surface ablation procedure, fears of haze get stirred up. But Dr. Stojanovic uses mitomycin-C in any case that will require an ablation deeper than 120 µm. Overall, he says the only haze he gets after these procedures is about 0.5 grade (trace) in 10 percent of cases. "And those are usually patients who need deeper ablations or who I know were exposed to considerable UV radiation through sunbathing or fishing postop," he explains.
Mated with the trans-epithelial program is a 1,000-Hz laser that speeds through ablations, most in 25 seconds, including the epithelial removal. "Some might be concerned that this high ablation rate might cause thermal damage," says Dr. Stojanovic. "But the system accounts for this by a function called constant frequency/area tuning. This basically makes the laser deliver a constant pulse rate per square millimeter. This means that if you have a small area to ablate, such as at the end of the ablation when you're doing the final details, instead of delivering the full pulse frequency over that small area, firing many pulses per square millimeter, this laser discards the 'extra' pulses, keeping the number per amount of area the same." To keep treatments on target, the system has a 500-Hz infrared eye tracker and registration based on scleral vessels to account for cyclotorsion.
Treating a Complicated Eye
In addition to primary treatments, the iVIS has been designed to treat the toughest patients: those with induced irregularities and/or aberrations; small optical zones postop; and decentered ablations.
To treat a patient with a decentered ablation, for example, the surgeon first images the eye with a Scheimpflug-based topographer called the Precisio, which was designed to be used in conjunction with the iRES laser for custom treatments. Though Dr. Stojanovic says it provides good images in post-refractive cases, some corneas with extreme irregularities, such as those resulting from a particularly bad corneal injury, would confound it, and would be better off having PTK with a smoothing agent.
After acquiring the topography, the surgeon imports the images into software called CIPTA (Corneal Interactive Programmed Topographic Ablation) to help plan the procedure. "CIPTA will give you many scenarios and possibilities to consider," says Dr. Stojanovic. "But, as usual, with a lot of possibilities comes the need for some experience in choosing the right one. It's not something for the beginner to start using. For example, you can customize the point at which the central ablation will be based and manage all the procedure's possibilities, such as the treatment and transition zones."
The system also has a dynamic pupillometer to help you gauge how small an optical zone you can use to take care of a patient's needs while still conserving corneal tissue. Through an electronic questionnaire, the computer will actually ask about the patient's profession and most frequent activities to get a sense of the conditions he or she usually operates under, and then suggests the optical zone it feels will cover 95 percent of those situations.
An intriguing feature is called the restored morphologic axis function, in which the system tries to determine the appropriate visual axis for someone with a decentered ablation or other complicated eye. "Let's say during a wavefront exam the patient's visual axis is determined incorrectly," posits Dr. Stojanovic. "The axis isn't the actual axis the patient uses in real life, and the resulting procedure causes everything to be tilted toward the wrong position. CIPTA would look at the untreated area and generate the most probable preop axis of the patient, and base the treatment on that."
Finally, to ensure that the transition zone is appropriate, the system has a variable width/constant slope transition zone feature. "Rather than just looking at the optical zone on the wavefront or on the topography and adding a 1-mm transition zone, the CIPTA system looks at the untreated cornea and determines what the height gradient will be between it and the treated zone after the ablation," says Dr. Stojanovic. "It then customizes the transition zone based on the disparity in height for that patient. It can be as wide as 3 mm or as narrow as 0.1 mm, but it doesn't just put down an arbitrary 0.5-mm transition for all corneas, for example. Though I haven't seen much of a difference in outcomes in virgin corneas with this zone adjustment, it's essential on complicated corneas, which often have a large gradient between the treated and untreated cornea."