Presentation
An 88-year-old Caucasian male with a history of basal cell carcinoma of the right cheek and right medial canthus was referred to the Wills Eye Oculoplastics Service for evaluation of a lesion near the right lower punctum and right medial canthus.
Medical History
Past medical history included BCC of the right cheek, status-post excision and reconstruction 27 years prior to presentation, with recurrence 19 years ago. The patient also underwent Mohs surgery for BCC of the right medial canthus (RMC) three years prior to presentation and subsequently had a dacryocystorhinostomy with a bicanalicular stent. He developed recurrence at the RMC a year prior to this exam and had excision and reconstruction with a mid-forehead flap and a tarsoconjunctival transposition (Hughes) flap.
Additional past medical history revealed prostate cancer, status-post radiation; papillary thyroid cancer with metastasis to cervical lymph nodes treated with total thyroidectomy; left parotid gland cancer, status-post parotidectomy; hypertension and gastroesophageal reflux disease. Past ocular history included bilateral lower eyelid ectropion repair, cataract surgery in the left eye and advanced glaucoma in the right eye. Social history was significant for being a former smoker with a 10 packyear history. Family history was non-contributory.
Current medications were artificial tears in both eyes, tobramycin ointment in the right eye, levothyroxine, amlodipine, omeprazole, aspirin and a multivitamin.
Examination
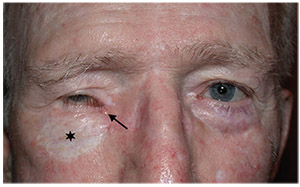 |
| Figure 1. External eye photo showing a small, ulcerated lesion with a pearly base (arrow) at the right medial canthus and a skin graft (star) from a prior basal cell carcinoma. |
External examination revealed a small ulcerated lesion with a pearly base at the right medial canthus (Figure 1). A 40 x 25-mm skin graft inferior to the right lower lid and a right-sided 20 x 25-mm forehead flap were present. Ptosis of the right upper lid was noted, with a margin reflex distance 1 of -2 mm and levator function of 12 mm; MRD1 and LF of the left upper lid were 5 mm and 18 mm, respectively. Visual acuity was count fingers OD and 20/20 OS. A right relative afferent pupillary defect was observed. Motility exam of the right eye demonstrated 100-percent abduction, 5-percent supraduction, 0-percent adduction, and 50-percent infraduction. Motility of the left eye was full. Confrontation visual fields revealed a superior field defect in the right eye and were full in the left eye. Intraocular pressures were normal in both eyes. Slit lamp examination was notable for trace injection and 2+ nuclear sclerosis in the right eye and a posterior chamber intraocular lens in the left eye. Dilated fundus examination revealed a glaucomatous optic nerve but was otherwise normal. Fundus examination of the left eye was normal.
What is your diagnosis? What further workup would you pursue? Click here for the diagnosis.



