In ophthalmology, the tools surgeons use to do their jobs are almost as important as the hands that wield them, and technology is often the engine driving new procedures and better outcomes. Along those lines, companies and surgeons have begun working with femtosecond lasers for cataract surgery, in the hope that they're standing on the ground floor of the next innovation. Here's a look at the systems as they stand currently, and what functions and procedures they might hold in store in the near future.
LensAR
The LensAR system recently received Food and Drug Administration approval to create an anterior capsulotomy, but LensAR medical advisor Louis Nichamin, MD, of the
"The research work is progressing nicely in the
 The company is also working on incorporating the creation of limbal relaxing incisions into the system. "We're working on really precise incision creation," says Dr. Nichamin. "In particular, we've been working on LRI algorithms based on computer modeling of the cornea which we believe we'll be able to use to develop extremely accurate astigmatic treatments." He says the development of these incisions will be key to the viability of the device in surgeons' practices. "The accurate astigmatic treatment will be important because that's how we're going to be able to pay for the machine initially—by charging patients for the refractive component. We can't charge Medicare recipients for anything that's currently approved and falls under the rubric of modern cataract surgery; this includes the capsulorhexis, incision and nucleus removal. But we can charge for refractive components such as LRIs and LASIK touch-ups. Refractive services aren't covered by the Centers for Medicare & Medicaid, so patients are able to pay out of pocket for these additional services. So, although there's no question that this machine performs a perfect capsulorhexis, that's a covered component of the standard operation so we can't charge for it, per se."
The company is also working on incorporating the creation of limbal relaxing incisions into the system. "We're working on really precise incision creation," says Dr. Nichamin. "In particular, we've been working on LRI algorithms based on computer modeling of the cornea which we believe we'll be able to use to develop extremely accurate astigmatic treatments." He says the development of these incisions will be key to the viability of the device in surgeons' practices. "The accurate astigmatic treatment will be important because that's how we're going to be able to pay for the machine initially—by charging patients for the refractive component. We can't charge Medicare recipients for anything that's currently approved and falls under the rubric of modern cataract surgery; this includes the capsulorhexis, incision and nucleus removal. But we can charge for refractive components such as LRIs and LASIK touch-ups. Refractive services aren't covered by the Centers for Medicare & Medicaid, so patients are able to pay out of pocket for these additional services. So, although there's no question that this machine performs a perfect capsulorhexis, that's a covered component of the standard operation so we can't charge for it, per se."
The best way to employ a femtosecond system in the cataract surgeon's practice is still being worked out. "It's a new paradigm," says Dr. Nichamin. "I can't say we have a definite answer. I'm leaning toward placing the laser outside the operating room. Patients will pass through a little preoperative area, receive the treatment, and then go into the OR, because after the femtosecond treatment, the eye is essentially still closed. Even though the incisions have been made, we haven't broken them open yet, so to speak.
This can be done in a semi-clean area, with the patient then being moved into the sterile OR. In theory, the shorter the length of time the patient is in the sterile OR, the lower the cost, since that's the most expensive place for someone to be sitting. We're still working out issues of patient flow and logistics, and a lot of cataract surgeons with plans to use a femtosecond laser are thinking along those lines right now." There's even speculation that the femtosecond step of the surgery could be performed by a non-physician member of the staff. "That's being discussed as well," says Dr. Nichamin. "Certainly, at the outset, I plan on doing it myself. In theory it could be performed by a tech with supervision by a physician, but that's still in the theoretical stage."
One of the chief functions of the laser will also be breaking up the nucleus for aspiration. "The algorithms for this continue to be refined," says Dr. Nichamin. "We're continually improving the pattern so less phaco energy is used. There are papers in line to be presented at upcoming meetings showing how we worked through different algorithms."
He says it's premature to detail the algorithms at the moment.
Some surgeons may also wonder how a femtosecond laser would deal with complicated cataract cases, such as those with zonular problems or capsular issues. "One would think the laser would be valuable in those cases," says Dr. Nichamin. "The cases I've accumulated haven't included any of those, though. However, a small pupil is another issue, because you can't laser through the pupil. We'd have to open the pupil in that type of surgical case. But in very dense cataracts, poor red reflexes, weak zonules or cases with difficult capsular qualities, the femtosecond would be useful."
 LenSx/Alcon
LenSx/Alcon
The LenSx/Alcon femtosecond laser has the most approvals of any of the femtosecond cataract laser devices in the
In initial studies of the device's first approved procedure, the anterior capsulorhexis, researchers found the mean diameter and standard deviation of laser-created capsulorhexes to be 5.02 ±0.04 mm. For manually created capsulorhexes, the average diameter in the x-axis was 5.76 ±0.72 mm, in the y-axis it was 6 ±0.81 mm, and overall the mean diameter was 5.88 ±0.73 mm.1
To make its ablations, surgeon Michael Knorz, of
Some surgeons have wondered if the use of a suction ring, common to femtosecond lasers, will deaden the "wow" factor common to postop cataract surgery, since it will leave some eyes red. "It's like LASIK in that it uses a suction ring," says
To break up nuclei, LenSx surgeons have developed two surgical approaches. "First is a divide-and-conquer technique," says Dr. Knorz. "This entails cutting the nucleus into four quadrants, and is designed for hard nuclei of 2+, 3+, 4+. Second, there is a liquefaction approach. This modality uses eight stacked cylinders cut into the nucleus to liquefy it." If there are harder nuclear pieces that resist liquefaction, phaco is used for them.

"What we're concentrating on now is learning how best to integrate it with the phaco," says Dr. Slade. "We're working with different phaco settings, different phaco tips and the Alcon Aqualase technology, the last of which might help us avoid using phaco on larger percentages of cataracts."
The surgeons are also studying the system's ability to create LRIs. "It's going really well," says Dr. Slade. "At first we thought we'd get less correction, but we're getting more. We're doing the incisions on the cornea, not at the limbus, so it looks as if we'll be able to make fairly small cuts." LenSx surgeons have been able to get astigmatic correction in the range of 4 D, but Dr. Slade cautions that this is "early data." In terms of cataract wounds, the laser can create incisions with as many as three incision planes. "Now that we have the basic mechanics of the procedure down," says Dr. Slade, "a lot of our work is concentrating on the astigmatic cuts and optimizing phacoemulsification to the laser and the laser to the phacoemulsification."
OptiMedica's Catalys
Though the Catalys system isn't yet approved in the
 As alluded to by Dr. Culbertson, the system uses OCT technology to image and register the eye's structures and subsequently guide the femtosecond laser pulses. "With precise OCT imaging of the anterior chamber, we can direct the laser where we want it," says Dr. Culbertson. "We can make cuts from 500 microns in the anterior capsule all the way through the nucleus of the lens, and can make a capsulotomy 0.5 mm from the pupil border."
As alluded to by Dr. Culbertson, the system uses OCT technology to image and register the eye's structures and subsequently guide the femtosecond laser pulses. "With precise OCT imaging of the anterior chamber, we can direct the laser where we want it," says Dr. Culbertson. "We can make cuts from 500 microns in the anterior capsule all the way through the nucleus of the lens, and can make a capsulotomy 0.5 mm from the pupil border."
Dr. Culbertson says he and the other OptiMedica researchers have experimented with different types of cuts in the lens for breaking up a cataract. "In cataract surgery in general, the most difficult types of lenses to deal with are very soft or very hard lenses," he says. "With soft cataracts it's hard to get any kind of grip with a chopper to separate the lens into segments or chop it; because it's so soft, it doesn't spread or crack apart very easily. However, with the laser, we can make pie-shaped cuts, separating the lens into four or six segments and then spread the segments apart very easily with the phaco instrument and some variety of spreader.
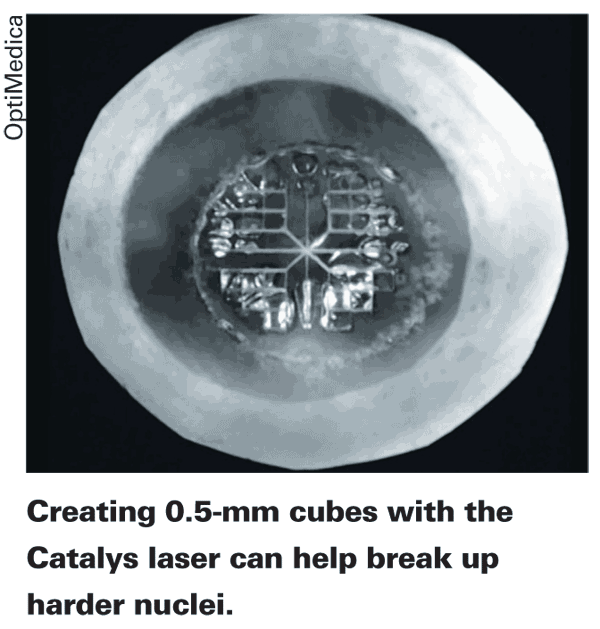
"With a hard lens, we can make the pie-shaped segments with the laser down to within 0.5 mm of the posterior capsule in every case without cutting through the capsule," continues Dr. Culbertson. "And then, without the use of any chopping, we can push the four or six segments apart because they're already cut down to the posterior part of the lens. For harder lenses, we also soften each segment by creating little 0.5-mm cubes of lens material. Then when we spread the segments apart and using a small amount of phaco energy, we can phaco-aspirate them."
In light of all of the progress that's been made with various procedures, Dr. Culbertson says it's now simply a waiting game for FDA approval. "We can't anticipate when we're going to receive approval, but we've tried to go slowly and get it exactly right," he says. "So, as a result, we're seeking approvals for what I believe is a very refined instrument."
1. Nagy Z,
Takacs A, Filkorn T, Sarayba M. Initial clinical evaluation of an intraocular femtosecond laser in cataract surgery. J Refract Surg 2009;25:12:1053.



