Today, so-called premium IOLs encompass a number of lens types, including toric, aspheric and multifo-cal lenses. [Ed. note: In this article, the term “multifocal” will also refer to extended-depth-of-focus lenses.] It may be tempting—by force of habit, if nothing else—to skip offering these to our glaucoma patients, but glaucoma patients have the same expectations as every other patient. They shouldn’t be slighted because they have glaucoma. Instead, we should be emphasizing that we want to maximize the patient’s vision.
Surgeons who specialize in treating glaucoma tend to be pretty conservative, and most of us have concluded that premium IOLs are not an option for glaucoma patients. That may be true for multifocals, but it’s certainly not true for any of the other intraocular lenses that are thought of as premium options—especially toric lenses. Many glaucoma patients could benefit enormously from having toric lenses implanted, and toric lenses don’t interfere with any aspect of glau-
coma follow-up.
Which Options Make Sense?
When you have a patient sitting in front of you with a cataract and you’re deciding what type of lens to put in, there are three fundamental issues to consider:
1) What are the patient’s visual needs? I ask every patient, “What do you do for a living? What do you do for fun?” For example, I have a patient who is a jeweler. He likes to be able to see very close to his nose without glasses. Knowing that, I left him very nearsighted after surgery, and he was happy as a clam. Had I not asked him what he liked to do, I would have put in a standard lens and he would have been unhappy.
Similarly, some people enjoy doing needlepoint. Some work on the computer all day. Each of those individuals may want to end up with something other than plano at distance after surgery.
2) Does the patient mind wearing glasses? Some people hate wearing glasses while others like them. (Some people say they can’t function without them.) Knowing how the patient feels about this will make a difference in the options you offer the patient.
3) What’s the status of the glaucoma? The status of your patient’s glaucoma should influence the IOL options you offer the patient, as well as your decision about whether or not to combine the cataract surgery with a MIGS procedure. That means it’s important to go into detail regarding the patient’s history.
Generally, the earlier the disease stage, the more options should be considered. If your patient has early ocular hypertension with no visual problems, or is at low risk for visual field loss, then multifocals are an option. On the other hand, multifocals are contraindicated in glaucomatous patients with significant cupping or field loss. If a patient has angle closure but a healthy visual field, taking the cataract out will be curative of the glaucoma. That patient should be eligible for the full complement of options we have to offer. But if your patient has secondary glaucoma from diabetes, you have to be careful, because there are other implications, such as potential cystoid macular edema.
There’s general agreement that a multifocal doesn’t make sense for a glaucoma patient with anything more than early disease, primarily because of issues with follow-up. A multifocal will cause a significant reduction of visual sensitivity during visual field testing, cause wavy artifacts on OCT imaging and make optic nerve examination difficult.1,2 If your glaucoma patient truly wants to be rid of spectacles, I’d suggest pursuing monovision.
However, some surgeons also believe a toric lens isn’t appropriate, primarily because of the extra cost involved. Actually, toric lenses are incredibly valuable; they help people with significant astigmatism achieve great vision, and a toric lens won’t impact any of those follow-up measures.3 (Astigmatic keratotomy is usually effective with less than 1 D of astigmatism; beyond that, a toric IOL should be placed.) I don’t think glaucoma patients with astigmatism should be shorted because they happen to have glaucoma. And yet, when I give a talk to an audience and ask for a show of hands regarding how many offer toric lenses to their glaucoma patients, usually less than half of the doctors in the audience raise their hand.
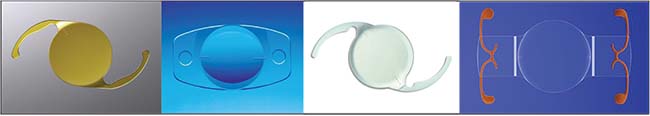 |
| Doctors treating glaucoma have traditionally avoided offering premium intraocular lenses, but monofocal toric lenses such as Alcon’s AcrySof IQ, Staar Surgical’s toric, AMO’s Tecnis toric and Bausch + Lomb’s Trulign toric can be of great benefit to patients with cupping. |
Choosing the Right Lens
These tips will help ensure that you’ll end up with a happy patient, whatever IOL option you end up employing:
• Remember that different premium IOLs have different impacts on contrast sensitivity. While it’s well known that multifocal IOLs can reduce contrast sensitivity—especially refractive, as opposed to diffractive, multifocals—options such as aspheric IOLs can actually improve contrast sensitivity. (Toric and accommodative IOLs have no detectable impact on contrast sensitivity.)
• Remember that cataract surgery by itself can relieve angle-closure glaucoma. Regardless of the type of lens you plan to implant, the best thing you can do for a patient with angle-closure glaucoma is take out the cataract. It’s very curative. In these eyes, the lens is taking up a lot of space inside the eye. Once you get the lens out of there, the iris will fall back into place, relieving the angle closure.
• Avoid using premium IOLs in glaucomatous eyes with weak zonules. This is an important caveat to the benefits of toric lenses in glau-coma patients, depending on the type of glaucoma the patient has. An eye with pseudoexfoliation has inherently weak zonules, which puts any intra-ocular lens at risk of dislocation. This can be a problem with any lens, of course—even a standard lens. But in the case of a toric lens, the axis of astigmatism has to be right on the money. If you get even a little subluxation of the lens, you’re going to get distortion and/or some loss of astigmatic correction.
• Use the best power calculation formula. Myopia is common in glaucoma patients, and some of the newer IOL formulas work better in a highly myopic eye—notably, the Barrett and the Hill RBF.4,5 Many formulas will recommend insufficient power, leaving these patients with postoperative hyperopia. On the other hand, hyperopic eyes often have angle closure. They may have an unpredictable anterior chamber depth, with the consequence that power calculations may also fail to be on target.
• Remember that combined surgery may contraindicate implanting a toric lens. Combining cataract and glaucoma surgery can lead to major astigmatic changes in the cornea. If you’re only performing cataract surgery, most studies suggest that induced astigmatism will pro-bably be less than 0.5 D, so you can incorporate that into your calculations. But when you’re combining surgeries, induced astigmatism is much harder to predict.
For example, if you combine a tra-beculectomy with cataract surgery, you’ll have an open wound away from the cataract wound. That can make the induced astigmatism much more difficult to predict and compensate for. In addition, the combined surgery may increase the possibility of zonules breaking or splitting, leading to unpredictable movement of the lens, throwing off the axis of alignment.
During Surgery …
Potential concerns during surgery include:
• Glaucoma patients are more likely to have pupil problems than patients without glaucoma. They often don’t dilate as well as nonglaucomatous eyes, so you’ll need to be extra careful. Poor visualization caused by an insufficiently dilated pupil can result in capsule tears and other complications. (There are plenty of ways to manage a small pupil, including pharmacological options such as epinephrine/lidocaine and Omidria, and techniques such as stretching or using iris hooks or a Malyugin ring.)
• Weak zonules are an issue in some types of glaucoma. Be prepared to insert capsular tension rings if you run into a problem with the zonules.
• Glaucoma patients are a little more at risk for cystoid macular edema. This is true in part because they’ve usually been on eye drops for a long time. (Prostaglandins in particular seem to be somewhat inflammatory.) There are pros and cons to using nonsteroidals for cataract surgery, but I think that when dealing with patients who are at risk, such as diabetic patients or those who’ve had CME in the past, you should use everything—steroidals and nonsteroidals—to prevent CME. (You should also avoid certain medications, such as prostaglandins, that might tend to cause it.)
• Intraoperative aberrometry may be helpful, especially in certain glaucoma patients. The vast majority of our patients—including most glaucoma patients—will get a good result without the use of intraoperative aberrometry, as long as an appropriate formula is used to calculate the lens power. The question is, what percentage of excellent outcomes is acceptable? Using intraoperative aberrometry will almost certainly improve your score in this department.
In addition, some glaucoma patients will present with problematic eyes that may need this technology to avoid a refractive surprise—such as when a bleb is overhanging the cornea, which can definitely impact the accuracy of your measurements. Also, many glaucoma patients have been using eye drops for years, leading to ocular surface problems that can affect the accuracy of your measurements.
Of course, adding another technology to your armamentarium will involve costs, having to spend a few minutes more in the OR, and the addition of another variable to the procedure. Nevertheless, using intraoperative aberrometry to help improve outcomes is worth considering.
Postoperative Concerns
Whether or not you implant a premium lens, it’s important to manage these issues following cataract surgery in your glaucoma patient:
• Be proactive regarding a post-operative pressure spike. Glaucoma patients are more likely than others to have a postoperative pressure rise within a day or two of cataract surgery, so be prepared to manage this if it occurs. One option is to use an acute pressure-lowering drug like brimonidine or iopidine to keep pressure down; another is to burp the wound to release a little viscoelastic. Either strategy will generally tide the patient over. This is usually a 24-hour phenomenon that soon goes away.
• Don’t confuse a postoperative pressure rise with steroid-induced glaucoma. A number of doctors have referred patients to me one week out of surgery, saying the patient has a steroid-induced glaucoma. In fact, the most common reason for a pressure rise on day one is retained viscoelastic; it has nothing to do with steroid-induced glaucoma. In my experience, you can’t get a steroid-induced glaucoma in a couple of days. It takes two to four weeks for a problem of that nature to develop.
Basically, steroid-induced glaucoma is a diagnosis of exclusion. You have to exclude everything else before you conclude that steroids caused the pressure increase. If in fact the patient does develop steroid-induced glaucoma a month after surgery, the correct response is to stop the steroids and address the pressure increase until the effect wears off.
• Don’t be afraid to stop all medications after cataract surgery to reevaluate the patient’s medication needs. I think many glaucoma patients are being over-treated after they’ve had cataract surgery, using more medications than they actually need. Cataract surgery is a very good pressure-lowering operation, so many patients can reduce or eliminate the drugs they were using before the operation. In essence, cataract surgery is a chance to wipe the slate clean. So it makes sense to start over again and see what the patient really needs. You’ll never know if the patient’s need for drops has been significantly reduced unless you stop the medications and see what happens.
I realize that some of my friends and colleagues don’t agree with this strategy; they believe it puts the patient at risk. However, cataract surgery is very effective at lowering pressure. You’ve done a good surgery; why not let the surgery do its job? It’s very unlikely that your patient will need the same number of medications he was using beforehand.
If I really feel that a patient is at high risk for a pressure rise, I’ll inject a miotic during surgery or give the patient Diamox at the end of surgery to prevent that first day or two of postoperative pressure problems. But once all of that settles down, I’d really like to know how the eye is doing before I start the patient back on glaucoma drops.
Coming of Age
Today, I think premium lenses should be an option we offer to our glaucoma patients—with the ex-ception of multifocals in glaucoma patients with cupping. Just remember that it’s very important to take careful, accurate measurements so you get the right IOL power.
In particular, if you’re a glaucoma surgeon, I urge you to fully correct your patients’ astigmatism. We’ve been ignoring astigmatism forever; now it’s time to address it, whether it’s a low level that you can fix with a femtosecond laser or a higher level that calls for a toric lens. With all of the tools at our disposal, we’re past the point at which we can ignore astigmatism. Correcting astigmatism will be the standard of care in the future, and glaucoma treatment needs to come of age. REVIEW
Dr. Lewis is a cataract surgeon and glaucoma specialist; the former director of the glaucoma service at the University of California, Davis; past president of the American Glaucoma Society; and past president of the American Society of Cataract and Refractive Surgery.
1. Inoue M, Bissen-Miyajima H, Yoshino M, Suzuki T. Wavy horizontal artifacts on optical coherence tomography line-scanning images caused by diffractive multifocal intraocular lenses. J Cataract Refract Surg 2009;35:7:1239–1243.
2. Aychoua N, Junoy Montolio FG, Jansonius NM. Influence of multifocal intraocular lenses on standard automated perimetry test results. JAMA Ophthalmol 2013;131:4:481–485.
3. Brown RH, Zhong L, et al. Toric Intraocular lens outcomes in patients with glaucoma. J Refract Surg 2015;31:6:366-372.
4. Zaldivar R, Shultz MC, Davidorf JM, Holladay JT. Intraocular lens power calculations in patients with extreme myopia. JCRS 2000;26:5:668-74.
5. MacLaren RE, Sagoo MS, Restori M, Allan BD. Biometry accuracy using zero- and negative-powered intraocular lenses. J Cataract Refract Surg 2005;31:2:280-90.



