Here, the manufacturers of the three comprehensive phaco systems available in the United States explain what makes their fluidics systems unique. Surgeons who use each system share their thoughts as well.
Alcon’s Centurion Vision System: Active Fluidics
Alcon’s Centurion Vision System, the follow-up to the Infiniti phaco system, features what the company calls Active Fluidics Technology. Gary Sorensen, head of cataract instrumentation R&D, explains how Active Fluidics works.
“Most fluidics systems are designed to maintain a constant pressure of fluid going into the cassette,” he says. “They’re usually gravity-fed; a bottle of BSS is hung above the patient and gravity provides the input pressure to maintain eye volume during the surgery. In contrast, the Centurion’s Active Fluidics system is designed to maintain the target pressure inside the eye; it does this by having a variable, rather than static, input pressure. To make that possible, the bag of fluid is inserted into the machine and acted upon by pressure plates that are able to change the pressure in the bag very rapidly in response to feedback from sensors in both the irrigation and aspiration paths within the cassette. There’s also a pressure sensor on the bag itself.
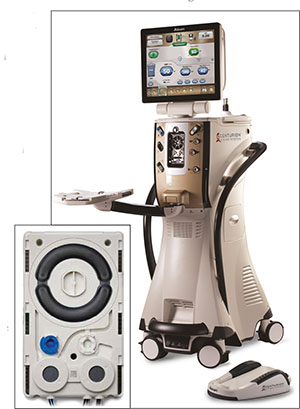 |
| Alcon’s Centurion system maintains a target pressure inside the eye (instead of the fluid pressure going into the cassette). It also features a peristaltic pump that doubles the available flow rate and eliminates the small pulsations usually associated with peristaltic pumps. |
“Another factor that sets the Centurion apart is its nontraditional peristaltic-style pump which, in effect, acts as two pumps pulling in parallel from the same piece of tubing,” he continues. “That has two advantages. First, we can get twice the flow rate achievable with a single pump, more than enough to overcome the resistance of the Centurion’s smaller tubing (which helps to minimize occlusion-break surge). Second, the two pumps are configured to be out of phase with each other, which cancels out the small pulsations that a peristaltic pump always produces. Those small pulses have traditionally been considered one of the downsides of peristaltic pump technology.”
Mr. Sorensen notes another design feature in the Centurion’s fluidics: rotary valves. “Standard valves close off flow by pinching the tube,” he says. “When you do that, it pushes fluid in both directions—one direction being into the eye—so when a valve closes you may see motion in the eye. We now use stopcock-type rotary valves; when open, a rotating gate is aligned with the fluid path so fluid can go by. When you turn it, it stops the flow without causing a change in volume or creating a pulse. This also makes it possible to open or close the valve just a little bit, making the flow proportional. It allows us to do a number of things that would be impossible with the old type of valve.”
In terms of being operator-friendly, Mr. Sorensen says the surgeon can now step through a series of procedures that have default values set up for all the engineering parameters, such as flow and vacuum. “The system can be used very effectively with those default settings, or it can be customized with help from Alcon personnel,” he says. “We try to keep the primary screens simple, like modern cameras; they’re point-and-shoot, but if you want to control every parameter and setting, you can.”
David Lubeck, MD, assistant clinical professor of ophthalmology at the University of Illinois Eye Center, and director of advanced anterior segment surgery at Arbor Centers for Eyecare in Chicago, uses the Centurion system. “The Centurion fluidics control system is so adaptive and adjustable that it allows automation of the process of cataract removal,” he says. “Once a surgeon decides how he or she would like the phaco machine to behave during each phase of the procedure, Centurion can be programmed to create the desired effects. For example, the surgeon can adjust the speed at which the eye pressurizes to prevent sudden overpressurization and reverse pupillary block. As a result, chamber maintenance is so stable that cataract removal can be performed safely at near physiologic intraocular pressures of 25 to 40 mmHg. Our fluid use has been reduced to 35 to 50 ml per procedure. In my experience, surgery with the Centurion system is elegant, making it more comfortable for both surgeon and patient.”
Alan Crandall, MD, clinical professor, senior vice chair of ophthalmology and visual sciences, and director of glaucoma and cataract at the Moran Eye Center, University of Utah, says he appreciates a number of features the Centurion offers, including the Active Fluidics system. “The Active Fluidics system maintains the intraocular pressure, helping to maintain a very stable anterior chamber, which is important not just in routine cases but in floppy iris syndrome and pseudoexfoliation cases,” he says. “In concert with the Intrepid Balanced Tip probe, it becomes a powerful emulsification unit that uses less energy.”
AMO’s Whitestar Signature: Fusion Fluidics
Abbott Medical Optics’ Whitestar Signature System, and its recent upgrade, Whitestar Signature PRO, feature what the company calls Fusion Fluidics, with the CASE (chamber stabilization environment) system. “MK” Raheja, PhD, MBA, global head of cataract R&D for Abbott, explains what makes the Whitestar Signature’s Fusion Fluidics system unique.
“There
 |
 |
| Abbott Medical Optics’ Whitestar Signature System lets the surgeon switch between a peristaltic pump and a venturi pump during surgery (see screen above, left), allowing the surgeon to take advantage of the different capabilities of each pump at different times. |
“Rather than ask the surgeon to choose one of these technologies, we made a conscious decision to design our phaco system to have both capabilities,” he explains. “That’s at the heart of what we call Fusion Fluidics. The surgeon can decide which system to use during the different parts of the surgery, using the foot pedal on the fly to engage either peristaltic or venturi aspiration.” Dr. Raheja notes that having such advanced technology in the system can seem intimidating. “As the system becomes more capable, we’re making sure it remains easy for the surgeon to use,” he says. “If a surgeon wants to alter the settings, he can, but it works beautifully in basic mode.”
Sumit Garg, MD, vice chair of clinical ophthalmology, medical director and associate professor of cataract, corneal and refractive surgery at the Gavin Herbert Eye Institute at the University of California, Irvine, uses the Whitestar Signature System. “I really enjoy operating using dual-pump fluidics,” he says. “By using the strong point of each pump I’m able to be more efficient and I find that I use less phaco energy. Having a dual pump lets me use the peristaltic pump to impale and hold the nucleus during my initial chops; subsequently, I transition to venturi fluidics for fragment removal and irrigation/aspiration. The venturi pump allows me to keep my phaco needle near the center of the eye and use the fluidics to draw the fragments to the tip without having to ‘fish’ for fragments.”
In terms of managing post-occlusion surge, Dr. Raheja says the Signature system senses that an occlusion at the tip has occurred and automatically implements changes to minimize any surge when the occlusion breaks. Dr. Garg agrees that this makes a difference. “The combination of updated sensing and processing along with less-compliant tubing makes for improved chamber stability,” he says.
Bausch + Lomb’s Stellaris: Stable Chamber Fluidics
Bausch + Lomb’s Stellaris Vision Enhancement System features what the company calls Stable Chamber Fluidics, a vacuum-control-based system. (The Stellaris is also available as the Stellaris PC, which is capable of performing vitrectomy surgery in addition to cataract surgery. The Stellaris Elite, featuring more than a dozen new innovations, will be introduced later this year.) Chuck Hess, vice president and general manager of Bausch + Lomb’s U.S. surgical division, explains what makes the Stable Chamber Fluidics system unique.
“The Stellaris’s system allows the surgeon to control vacuum at the tip of the device during phacoemulsification, as well as irrigation and aspiration,” he says. “This is also critical during vitrectomy surgery, which the Stellaris PC can perform.” He notes that post-occlusion surge is more of an issue with a peristaltic-pump-based system. “The Stellaris produces a very stable intraocular environment because the surgeon is able to gauge what’s happening in the eye and use the foot pedal to modulate the vacuum level. If I’m doing phaco and I see an occlusion occurring, I can reduce the vacuum by lifting up on the pedal, effectively preventing the big post-occlusion surge you may see with some systems.”
In terms of managing the system’s complexity, Mr. Hess says the development of B+L’s dual-linear foot pedal technology allows surgeons to manage multiple factors at once—if they wish. “Most surgeons like to have two or three basic modes set up for their machines, such as dense-lens, soft-lens and small-pupil modes. On the other hand, some surgeons also like to have the ability to modulate their parameters on the fly. Dual-linear control allows the surgeon to manage two parameters, such as aspiration and power, with the foot pedal. Your foot can press down on the pedal as if it were an accelerator to control one variable, but you can also move it side to side to control a second variable.”
 |
 |
| Bausch + Lomb’s Stellaris allows the surgeon to control vacuum on the fly, and its dual-linear foot pedal (above, right) lets the surgeon manage two parameters at once, if desired. |
Dr. Singh says he’s impressed by the chamber stability he gets. “The Stellaris decouples vacuum and flow, which leads to lower flow at high vacuum and a decreased likelihood of surge,” he says. “It maintains excellent chamber stability even with vacuum settings of 600 mmHg. We performed a study in which we used an endoscope to video the chamber stability during a standard case, and we saw almost no movement of the iris or shallowing of the chamber.
Dr. Singh adds that he finds the dual-linear foot pedal very useful. “It gives me separate control of phaco, vacuum and irrigation,” he says. “For example, during epinuclear removal pushing down on the foot pedal controls irrigation and aspiration, but if I need a pulse of ultrasound, I can yaw to the right to get that burst. This gives me another level of control.” REVIEW
Dr. Singh is a consultant to Bausch + Lomb; Drs. Lubeck and Crandall are consultants for Alcon; Dr. Garg is a consultant to AMO.



