A 52-year-old man was referred to the Wills Eye Hospital’s Ocular Oncology Service for further evaluation of progressive vision loss in his left eye. He had been diagnosed with a choroidal hemangioma following evaluation elsewhere by both a retinal specialist and ocular oncologist, and had received four injections of the anti-vascular endothelial growth factor drug bevacizumab for overlying subfoveal fluid, with minimal improvement. He was therefore referred for recommendations of how to proceed with treatment.
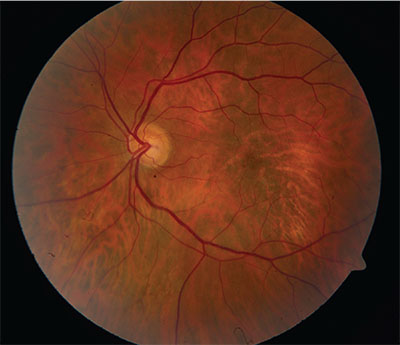 |
| Figure 1. Fundus photograph of the left eye showing an area of central macular RPE alterations and no visible tumor. |
Medical History
The patient’s ocular history was otherwise notable for myopia with astigmatism (-8 D OU). His past medical history included hypertension, hyperlipidemia and migraines, and his medications were verapamil and rosuvastatin calcium. He was allergic only to moxifloxacin. Family history revealed glaucoma and diabetes mellitus. He was a nonsmoker and drank alcohol socially.
Examination
On ophthalmic examination his best corrected visual acuity was 20/20 in the right eye and 20/70 in the left eye. His pupils were equal, round and reactive to light without relative afferent pupillary defect. Extraocular movements and confrontation visual fields were full bilaterally. Intraocular pressures were 14 mmHg by applantion in both eyes. External and anterior segment examinations were unremarkable. A dilated funduscopic examination of the right eye was within normal limits. The left eye showed an elevated macula, suggestive of an underlying tumor, along with related retinal pigment epithelial changes. Despite the elevation, the choroidal vascular tissue appeared of normal color and its architecture was without a visible tumor, suggesting that the mass might be deeper than the choroid (See Figure 1).
Click here to view the Diagnosis & Discussion.



